A brief history of the Chapter of Military Medicine
The Chapter of Military Medicine was established in 2000 following the signing of a charter by the, then RACGP President, Dr Margaret Kilmartin and the, then Surgeon General of the Australian Defence Force (ADF), Major General John Hearn.
In his introduction to the charter Major General Hearn wrote:
'The clinical skills and preventive outreach of all medical practitioners within the Australian Defence Force have as their core, state-of-the-art skills of best-practice general medicine.
'The basic terms of reference for all doctors who serve in uniform within the Australian Defence Force is the maintenance of positive health at the individual level both in peacetime training and during operational service. The individual doctor responsible for the care of service personnel is subject to great demands and carries significant responsibilities.
'Every Regimental Medical Officer, every member of the RAN Medical Branch, every Air Force doctor–officer who cares for the servicemen and women of their battalion, regiment, ship or squadron, is required to be the most skilled of general practitioners. In addition, they need to practise state-of the-art travel medicine, preventive medicine and health, sports medicine, tropical medicine and emergency trauma response – all to discharge their normal professional duties.
'The Military Medicine Chapter will promote such best-practice medicine, in such settings on land, sea and air.'
The Chapter fell under the auspices of the National Faculty of Specific Interests (now RACGP Specific Interests) in 2010.
In recent years, the members of the Chapter have concentrated their efforts in the establishment of a post-Fellowship specialty recognition for RACGP members working in the ADF, the framework of which is currently being piloted.
Meet the Chair, Dr Andrew Ramage
 Dr Ramage is an Australian trained ADF Medical Officer. He has particular interests in military medicine, veteran’s health, military family member’s health, sports and exercise medicine, occupational medicine, musculoskeletal rehabilitation and general practice.
Dr Ramage is an Australian trained ADF Medical Officer. He has particular interests in military medicine, veteran’s health, military family member’s health, sports and exercise medicine, occupational medicine, musculoskeletal rehabilitation and general practice.
Dr Ramage holds a BAppSc(Hons) in Human Movement Studies from Queensland University of Technology and worked as an exercise physiologist for seven years before starting officer training at Royal Military College, Duntroon. He completed his Bachelor of Medicine, Bachelor of Surgery and a Master of Public Health at the University of Qeensland and is currently completing a Master of Sports Medicine there.
Dr Ramage was elected as Chair of RACGP Specific Interests Chapter of Military Medicine in December 2018. He shares a few words with us:
I was honoured to be elected as the Chair of the Chapter of Military Medicine and would like to thank the previous Chair, Dr Glen Pascoe, for his efforts and achievements while in the role. The Chapter has had some significant achievements since its inception, including the RACGP Standards for Garrison Health Facilities and, more recently, progression of the post-Fellowship specialty in military medicine.
Military Medicine is a complex mix of primary care, population health, occupational medicine, aviation and underwater medicine, emergency medicine and mental health. It is also characterised by exposure to unique challenges of location, resources and personnel management that can sometimes make simple clinical decisions very complicated. For serving Medical Officers, command, leadership, management, clinical governance, health support, aeromedical evacuation and disaster response planning also fall into our remit as GPs. These skills and experiences gained are a direct benefit of military service as a GP and are invaluable skills and experience for military registrars that most civilian registrars will never have the opportunity to acquire.
It is important to note that the role of the GP in military medicine extends beyond that of uniformed GPs and registrars. Civilian GPs working in Garrison Health and Recruiting facilities provide valuable services that help to ensure the maintenance of entry standards and the conservation of the human element of combat power for the ADF.
Special acknowledgement also needs to be made of the GPs who provide healthcare to the families of serving ADF members, reservists and veterans. While not directly involved in the ADF, understanding the unique stressors, support services and benefits available to ADF families, Reservists and Veterans is important for these GPs to feel confident that they are facilitating the best care possible. The Chapter has an important role in communicating the considerations and entitlements when working with these special populations.
I would also like to extend thanks to those GPs who are providing supervision, education and training to ADF Registrars. The demands of military service on Registrars often see them deployed or sent on military training activities at short notice. This can be disruptive to practices and training. Civilian GP supervisors and practices are critical in the training of ADF Medical Officers and, by extension, the health capability of the ADF. I am extremely grateful to the practice managers, owners and GP supervisors who continue to support ADF Registrars in their training and development.
Finally, I hope to continue to expand the understanding of military medicine within the RACGP, ADF and wider medical community. This will require active participation from as many members of the Chapter as possible. I encourage you to become actively involved in the Chapter by participating in meetings, conducting and publishing research, contributing articles to AJGP, presenting at conferences and participating in working groups and Chapter meetings to progress the understanding of the breadth and depth of military medicine.
Recent research in military medicine
Medical contributions of Royal Navy physicians
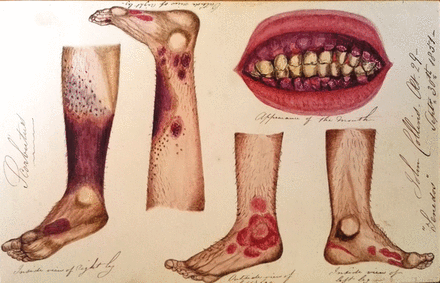
This article reviews the contributions that Royal Navy physicians have made to medicine over the centuries.1 They have detailed some of the better known, as well as some almost forgotten, but still remarkable, achievements. Royal Naval ships' companies that are isolated by hundreds of miles of sea with contacts to the outside world tightly regulated, provided perfect environments to study the epidemiology of disease.
In 1747, James Lind organised one of the earliest clinical trials, demonstrating that scurvy (pictured left) could be treated by lemon juice. A century later, Alexander Bryson proved the value of careful epidemiological data collection and observation of infectious diseases encountered on the West Africa station. In the twentieth century, Royal Navy physicians were at the cutting edge of vaccine research and antibiotic production. Nuclear submarines placed naval physicians at the forefront of nuclear medicine and environmental safety.
1. Houlberg K, Wickenden J, Freshwater D. Five centuries of medical contributions from the Royal Navy. Clin Med (Lond). 2019;19(1):22-25. doi:10.7861/clinmedicine.19-1-22.
Reduction in combat deaths in Afghanistan and Iraq
This analysis of all US military casualties, from October 2001 to December 2017, found that survival among the most critically injured casualties increased three-fold during the course of the conflicts. 2
Three key interventions – tourniquets, blood transfusions, and prehospital transport within 60 minutes – were associated with 44% of mortality reduction. Across 16 years of conflict, military trauma system advancements, namely, improvements in methods to control bleeding, replace blood, and reduce time to treatment, may be associated with increased survival of battle casualties.
2. Howard JT, Kotwal RS, Turner CA, et al. Use of combat casualty care data to assess the US military trauma system during the Afghanistan and Iraq conflicts, 2001–2017. JAMA Surg 2019. doi:10.1001/jamasurg.2019.0151.
A military medicine hisory of syphilis and gonorrhoea
The purpose of this historical article is to demonstrate the scale of gonorrhoea and syphilis infections in the Australian Army's overseas campaigns during the twentieth century.3
It refers to the Australian Army’s major overseas deployments; from the Boer War at the beginning of the century to the war in Vietnam, which ended in 1975. It investigates the measures taken by the staff of the Army Medical Service to prevent the sexually transmitted diseases (STDs) and to treat those who contracted STDs.
3. Howie-Willis, I. The Australian Army’s two ‘traditional’ diseases: gonorrhea and syphilis — A military-medical history during the twentieth century. J Mil Veterans Health 2019;27(1):11–22.
Managing solidiers at risk of suicide
This paper describes a collaborative effort between line-unit leaders, medical personnel and installation services to synchronise suicide risk identification and communication between these disparate entities.4
It describes the process of implementing a suicide risk assessment and management policy at one installation in the Pacific Northwest. This policy was subsequently adopted as the standard of care for the US Army.
4. Hoyt T, Repke DM. Development and implementation of US Army guidelines for managing soldiers at risk of suicide. Mil Med 2019;184(Supplement_1):426–431. doi:10.1093/milmed/usy284.
Australasian Conference on Traumatic Stress (ACOTS2019)
Trauma, recovery and growth: Advances in research and practice

While trauma may have a severe, negative impact on an individual’s life, trajectories that promote recovery and growth are possible. This conference will explore research and clinical advancements in the field of traumatic stress studies that continue to transform the understanding of treatment and recovery for those affected by trauma and its aftermath.
Research into the science of post-traumatic growth further demonstrates that trauma can bring a deeper response to personal transformation.
ACOTS2019 will launch a dedicated clinical training stream that will provide clinicians and practitioners working with those affected by traumatic stress a unique training opportunity to refresh their skills in core evidence-based, trauma-focused treatments, and be exposed to some of the latest treatment innovations in the field.
ACOTS2019 conference is a collaboration between the Australasian Society for Traumatic Stress Studies (ASTSS) and Phoenix Australia – Centre for Posttraumatic Mental Health.
The conference will be held on Thursday and Friday 13–14 September in Sydney, NSW at ICC Sydney, Darling Harbour with pre-conference workshops on Tuesday 12 September 2019.
Registration is now open.
Australian Military Medicine Association 2019 Conference
After the war: Repatriation, recovery and public health
The 2019 Australian Military Medicine Association (AMMA) Conference will be held in Adelaide on Friday to Sunday 4–6 October 2019.
The AMMA Scientific Committee are seeking standard (20-minute) and short (five-minute) oral presentations, and poster presentations.
Topics sought include, but are not restricted to:
• aero medical evacuation
• ethics
• veteran's health (including PTSD and rehabilitation)
• operational health support
• bioterrorism
• trauma.
Abstracts of no longer than 600 words must be submitted by Friday 31 May 2019 through the AMMA submission portal.
Chapter of Military Medicine on shareGP

RACGP Specific Interests Chapter of Military Medicine has its own
closed shareGP group.
shareGP is the RACGP's online space for members to share collaborative content including blogs, papers or research, search and connect with peers;
All members of the RACGP with an interest in military medicine are welcome to join. Once you have requested to join, an administrator will approve your membership within 48 hours.
You will need your RACGP password to log in. If you are unsure of your password, it can be reset on the RACGP login page.