Case
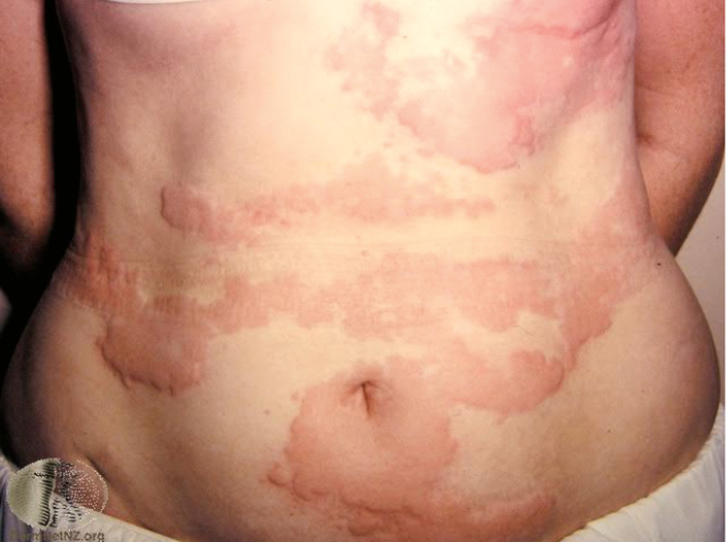 |
Figure 1. Urticarial rash
Image courtesy of DermNet NZ. Published online at www.dermnetnz.org |
A woman, 50 years of age, presents to her general practitioner (GP) with a relapsing rash, assessed as hives and welts. Her symptoms began a few months ago, but intensified in the past four weeks. The rash occurred anywhere on her body (Figure 1) without an identifying trigger, occasionally causing swelling around her lips and eyes. It was worse at night and where her clothing was tight. It lasted for around six to 12 hours and troubled her most days of the week. Her medications included occasional ibuprofen for tension-type headaches.
Relevant past history included a spider bite three months ago, which healed with no apparent complications. Twelve months ago her youngest daughter died of breast cancer, aged 23 years. Since her daughter’s death, she lost 5 kg and became increasingly withdrawn. Her affect appears depressed and anxious on her visit to you today.
Question 1
What are the differential diagnoses?
Question 2
What further tests would you perform?
Answer 1
Differential diagnoses include:1,2
- one of the physical urticarias (a subset of chronic urticaria caused by physical stimuli)
- chronic spontaneous urticaria
- recurrent erythema multiforme (lesions that leave residual pigmentation and desquamation)3
- mast cell activation disorders (lesions that occur with light touch)
- urticarial vasculitis (hives that are painful but not pruritic)
- subacute cutaneous lupus erythematosus
- bullous pemphigoid (an autoimmune, blistering skin disease).
Answer 2
Skin prick tests are not indicated as urticaria without atypical features, occurring on a near-daily basis for weeks at a time, is rarely an allergic condition.
A systematic review of 6462 patients with chronic urticaria concluded that there is no relationship between the number of laboratory tests performed and the identification of an underlying medical condition. The authors advised that only a full blood examination (FBE) and erythrocyte sedimentation rate (ESR) are necessary for patients with a suggestive clinical history.4
A 3–4 mm punch biopsy of a new lesion is warranted if urticarial vasculitis or the rarely occurring mastocytosis, a subclass of systemic mast cell activation disorders, is suspected.
Case continued
FBE and ESR were found to be normal. A recent thyroid-stimulating hormone (TSH) test was also found to be normal. Screening for systemic lupus erythematosus (SLE) and punch biopsy was not considered necessary.
Question 3
What is the diagnosis?
Question 4
What is known about the aetiology of this condition?
Question 5
How would you counsel this patient on the natural history of her condition? What aggravating factors should she be aware of?
Question 6
What would you consider for the treatment of her condition?
Question 7
Would you refer this patient to a specialist?
Answer 3
The diagnosis for this patient is chronic spontaneous urticaria (CSU), previously known as chronic idiopathic urticaria. This condition is defined by the presence of urticaria (hives) on most days of the week for six weeks or longer. About 40% of patients have episodes of facial angioedema.5
Answer 4
In 80–90% of cases, no external allergic cause can be identified.6 The relationship between insect bites and CSU is contentious and unproven.
Answer 5
Reassurance and education are paramount. CSU is a self-limited, non-allergic condition. Symptoms spontaneously resolve in a year for half of all patients.7 Although 30% of patients experience symptoms lasting five or more years, reassurance can be given that most people respond to medications and lifestyle modifications. Certain factors exacerbate CSU in some people and the following should be considered:
- Symptoms can present at pressure areas on the skin. Loose-fitting clothing is recommended. Other physical stimuli include high temperatures and humidity. Air-conditioning may bring relief.
- Non-steroidal anti-inflammatory medications are thought to worsen symptoms in 25–50% of patients.8
- Patients who suffer from CSU may have a higher sensitivity to histamine-rich or histamine-producing food (such as wine and fermented sauces).9
- There is a strong association of severe symptoms with comorbid stress and depression.10
Answer 6
The following are possible treatments for CSU:
- Histamine H1 receptor antagonists (antihistamines) – may provide some control of symptoms and, given the low toxicity of non-sedating formulations, increasing the dosage up to fourfold has been recommended11,12
- glucocorticoids – rarely justified except as a short-term ‘rescue’ medication
- leukotriene modifiers (eg monteleukast, 10 mg once daily) – useful as add-on therapy or monotherapy
- novel approaches – cyclosporine, hydroxychloroquine, dapsone, methotrexate, sulfasalazine, intravenous immune globulin and omalizumab.13
Answer 7
The role of stress and depression is undervalued in the initiation and maintenance of CIU. Nearly half of all CIU patients suffer from a comorbid mental illness and social isolation.14 In this case study, referral to a clinical psychologist or psychiatrist is important. Referral to a dermatologist may be indicated if an underlying disorder such as urticarial vasculitis is suspected, or if symptoms are not controlled without corticosteroids.
Key points
- CIU is predominantly a clinical diagnosis.
- It is a non-allergic condition defined by the presence of urticaria (hives) on most days of the week for six weeks or longer.
- About 40% of patients with CIU have episodes of facial angioedema.
- Lifestyle modification, stress management and H1 antihistamines form the basis of treatment.
- Comorbid mental illness is common and should be screened for in all presentations.
Author
Kirsten Due BPsych, MBBS, FRACGP, FACRRM, DipPalMed (RACP), General Practioner, Barrier Reef Medical Centre, Cairns North, QLD. katieandluther@gmail.com
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.