Case
A man in his early 20s presented with perianal lesions. Two general practitioners (GPs) had previously diagnosed haemorrhoids and provided treatment advice. However, the patient described worsening symptoms over six months and was now struggling to walk or sit comfortably. He was otherwise well. His sexual partners were male. Sexually transmissible infection (STI) screening 16 months earlier was unremarkable. He had no regular medications or allergies.
On examination, there were multiple tender, flesh-coloured perianal papules/plaques up to 15 mm in diameter (Figure 1). Other skin areas, mucous membranes and hair were unremarkable.
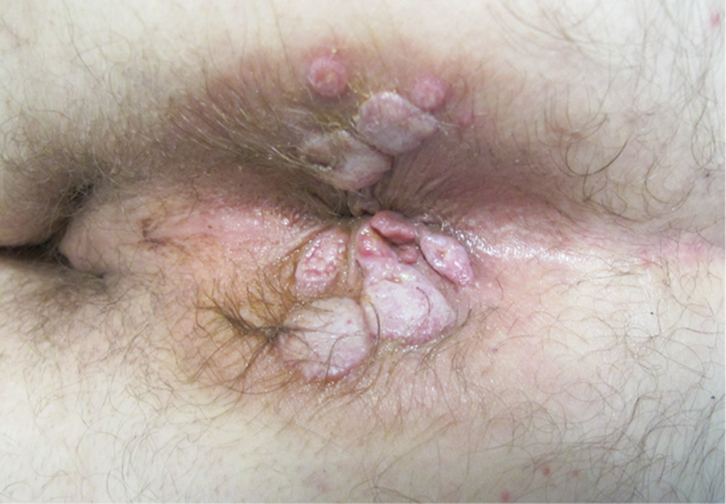 |
Figure 1. Perianal lesions
These had been increasing in number/size over months and the patient had been applying witchhazel ointment |
Question 1
What STI screening is appropriate for men who have sex with men (MSM)?
Question 2
What are the main differential diagnoses in this case?
Question 3
What investigations are appropriate?
Answer 1
The Australian STI management guidelines1 (www.sti.guidelines.org.au) and STIGMA guidelines2 recommendations for MSM are:
- gonorrhoea nucleic acid amplification testing (NAAT) of the throat and rectum
- chlamydia NAAT of urine, throat and rectum
- serology for human immunodeficiency virus (HIV), syphilis and, if immunity has not been previously demonstrated, hepatitis A and B
- serology for hepatitis C if the patient is HIV-positive or has a history of injecting drug use.
STI screening should be conducted three-monthly to yearly, depending on the risk.1,2
Answer 2
The lesions are most consistent with condylomata lata (secondary syphilis), with a differential of condylomata accuminata (warts).3 Broad differentials for perianal lumps are shown in Table 1.
Table 1. Common and important causes of perianal lumps1,9
Viral infections
- Condylomata accuminata (warts: human papilloma virus)
- Molluscum contagiosum
- Herpes simplex virus (HSV)
|
Bacterial infections
- Condymomata lata (syphilis)
- Perianal abscess (multiple causes including gonorrhoea)
- Folliculitis (multiple causes)
|
Other
- Haemorrhoids
- Fibroepithelial polyps
- Perianal neoplasia (anal intraepithelial neoplasia [AIN]/squamous cell carcinoma [SCC])
|
Answer 3
Testing should include syphilis serology and a swab from the lesions for syphilis NAAT (flocked swab). NAAT may be positive before positive serology develops. A suspicion of syphilis with negative serology should prompt re-testing in two weeks1 or consideration of treatment with same-day rapid plasma reagin (RPR).
Warts are generally diagnosed clinically but can be confirmed histologically. Anogenital ulcers or fissures may be swabbed for herpes simplex virus (HSV) NAAT.1
As the patient has a probable STI, he should also be offered chlamydia, gonorrhoea, HIV, and hepatitis A and B testing as per Answer 1.
Case continued
Treatment for secondary syphilis was offered presumptively and the patient’s symptoms improved dramatically post-treatment. Baseline syphilis serology on the day of treatment was positive, with an RPR of 64. Perianal swab for syphilis NAAT was also positive.
Question 4
What is the appropriate treatment for syphilis? What specific warnings need to be given regarding that treatment?
Question 5
What follow-up does this patient need?
Answer 4
The recommended treatment for syphilis is long-acting parenteral benzathine penicillin. For infections within two years, a single 1.8 g intramuscular (IM) dose is recommended, but for infections longer than two years, or where the duration is uncertain, 1.8 g IM weekly for three weeks is recommended.1 In patients with a penicillin allergy, oral doxycycline 100 mg twice daily for 14 days (infections under two years) or 28 days (infections longer than two years) may be given, but it is less efficacious than benzathine penicillin.1
Tertiary syphilis and neurosyphilis require intravenous therapy,4 so it is important to exclude these and refer if suspected.1 Sexual health clinics can assist with the interpretation of serology, treatment decisions and treatment provision. To find your nearest service, see Table 2.
Benzathine penicillin syphilis treatment can cause a Jarisch−Herxheimer (JH) reaction1, a flu-like syndrome, within hours of treatment. This is self-limiting, typically lasting under 24 hours.5 It can be managed with simple anagesia (eg paracetamol) and rest.1
Table 2. State-based resources
| Australian Capital Territory |
|
| Canberra Sexual Health Centre |
02 6244 2184 |
| New South Wales |
|
| NSW Sexual Health Infolink |
1800 451 624 |
| PEP Hotline |
1800 737 669 |
| Northern Territory |
|
| Clinic 34 Darwin |
08 8999 2678 |
| Queensland |
|
| Healthline |
134 325 84 |
| South Australia |
|
| Clinic 275 Royal Adelaide Hospital |
08 9222 5075 |
| PEP Hotline |
1800 022 226 |
| Tasmania |
|
| Tasmanian Sexual Health Service |
1800 675 859 |
| PEP Hotline |
1800 889 887 |
| Victoria |
|
| Melbourne Sexual Health Centre clinician advice line |
1800 009 903 |
| PEP Hotline |
1800 889 887 |
| Western Australia |
|
| WA Sexual Health Helpline |
08 9772 6178 or 1800 198 205 (country callers) |
| PEP Line |
1300 767 161 |
Answer 5
The patient should not have any sex for seven days post-treatment and not have sex with recent sexual contacts until they have been tested and treated.1 Contact tracing for secondary syphilis covers the past six months (three months for primary syphilis),6 but given this patient’s symptom duration, a nine-month timeframe is more realistic. If he opts to contact partners himself, he should be followed up after a few weeks to see if he has been successful and to offer him support. Helpful contact-tracing resources for patients include Let Them Know
(www.letthemknow.org.au) and The Drama Downunder (www.thedramadownunder.info/introduction). The local public health department will need to be notified.
RPR or venereal disease research laboratory (VDRL) should be collected on the day of treatment, and at three, six and, if necessary, 12 months, to monitor response (a four-fold drop in titre is expected).1 The patient should be warned that his syphilis serology will remain positive for the rest of his life, and only RPR/VDRL will be useful for screening from now on. In addition to the management of his syphilis and STI screening, this patient needs:
- education about harm reduction strategies,1 including use of condoms, post-exposure prophylaxis (PEP)7 and pre-exposure prophylaxis (PrEP)8 for HIV
- to consider PEP7 if his last condomless anal sex was within 72 hours. PEP is available from sexual health centres or emergency departments. To find the nearest provider, see Table 2 or check online resources (eg www.getpep.info/where.html).
- to be offered hepatitis A, hepatitis B and/or HPV immunisation, depending on his vaccination status and serology.1
Key points
- Secondary syphilis can cause lesions that closely resemble warts.
- A sexual history is part of assessment of anogenital lesions.
- Treatment for syphilis depends on the duration of infection.
- Diagnosis with one STI should prompt testing for others. The Australian STI management guidelines provide free online recommendations for testing and treatment.
- Sexual health centres can help with interpretation of syphilis testing and provide treatment.
Authors
Miranda Sherley BSc (Hons), PhD, MBBS, FRACGP, Registrar, Canberra Sexual Health Centre, Canberra Hospital, Canberra, ACT. Miranda.Sherley@act.gov.au
Sarah Martin BA (Hons), BMed (Hons), DCJ, DipForensMed, FAChSHM, Director, Canberra Sexual Health Centre, Canberra Hospital, Canberra, ACT
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.