Case
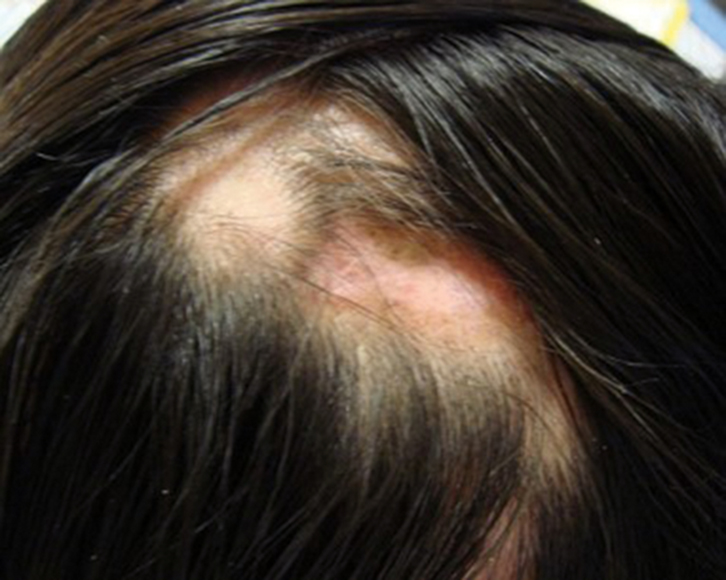 |
| Figure 1. Scalp lesions with scarring alopecia 44 x 35 mm |
A woman, 30 years of age, presented with patchy hair loss on her head. It started 1 year ago when she developed an itchy, slightly painful, red scaling rash on her scalp 1 month after she dyed her hair. She had been treated with antifungal and other treatments unknown to her by several primary care doctors. However, the lesion worsened, and new lesions appeared. She was referred to a dermatologist. Aside from the devastating psychological effects from the disfigurement and the effect on her occupation as a cosmetics sales promoter, she had no other symptoms. There was no significant past or family history. She did not smoke, but her husband smoked heavily in the house.
An examination of the scalp revealed focal coin-shaped, scaly, erythematous lesions, some of which had coalesced (Figure 1). Closer examination revealed shiny, central hypopigmentation and absence of hair follicles, and some thickened areas of hyperpigmention peripherally. Where there were no lesions, her hair was black, thick, straight and long. At the periphery of the lesions, her hair became sparse and thin. A full examination of her face, neck, body and nails revealed no other skin lesions.
Question 1
What differential diagnoses should be considered?
Question 2
What investigations would be helpful in making a definitive diagnosis?
Answer 1
On the basis of the clinical features, including nummular-shaped lesions with central permanent scarring alopecia due to total loss of hair follicles, and peripheral hyperpigmented adherent thick scales, the most likely diagnosis is discoid lupus erythematosus (DLE).1–4 DLE is the most common form of chronic cutaneous lupus erythematosus and is usually localised on the face (eg cheeks, nose and ears). It is termed ‘generalised’ if found on the neck, upper back and dorsum of hands. On the scalp, it causes dilatation and plugging of hair follicles with adherent scales. This leads to destruction of hair follicles and permanent balding. Initial manifestation of DLE can be difficult to recognise. Early referral to a dermatologist is recommended if in doubt, or if there is disease progression and treatment failure.
Alopecia areata can cause patchy hair loss but does not cause scaling or scarring. It is characterised by ‘exclamation mark’ hair.
Differential diagnoses for cicatricial (scarring) alopecia include trauma, burn, tinea capitis, lichen planus, scalp psoriasis and sarcoidosis. The history of hair dyeing 1 year ago might suggest a chemical burn, but this should not have progressed and no new lesions should have appeared.
Tinea capitis is associated with scaling, and severe lesions (kerion) can scar, but it usually affects children, individuals who are immunocompromised and those in contact with animals.
Lichen planus lesions are erythematous and hyperkeratinised. They can cause temporary or permanent scarring alopecia but have characteristic white, lacy patterns on the buccal mucosa and nail changes.
Psoriatic lesions are red, scaly, hyperkeratinised and itchy. Scalp psoriasis can progress to alopecia, but it is associated with arthritis, plaques elsewhere, nail changes of pitting, and subungual hyperkeratosis. Scalp lesions in psoriasis usually involve the hairline. Scalp sarcoidosis can also mimic DLE.5
Answer 2
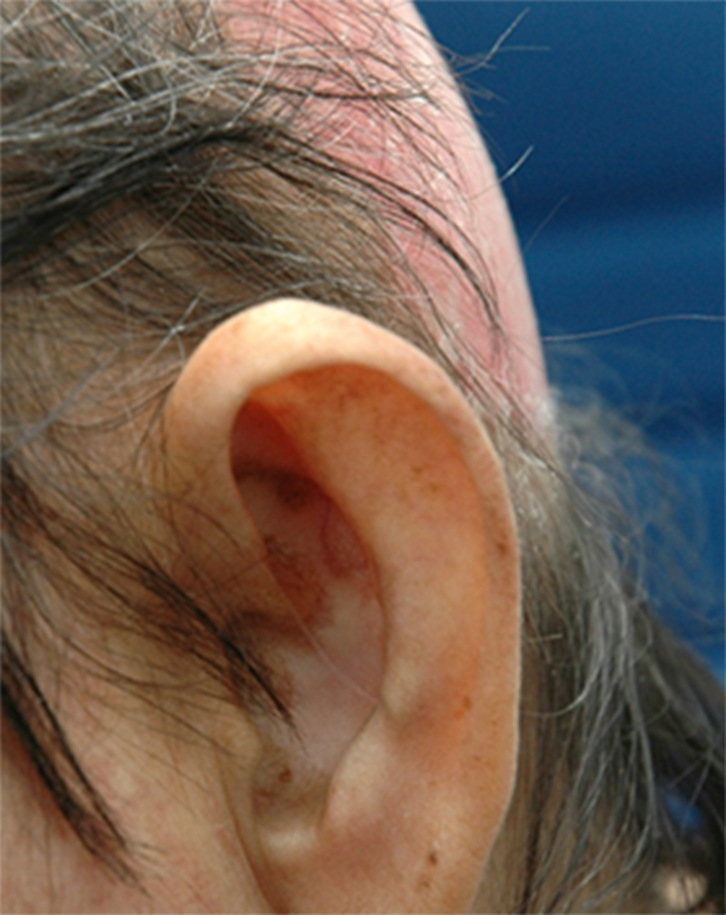 |
| Figure 2. Scarring alopecia with post-inflammatory dyspigmentation in advanced DLE |
Microscopy and culture of skin scraping and hair are required to exclude dermatophyte infections.
Scalp biopsy is necessary for the diagnosis in the early stages, when the lesions are indeterminate. Histological findings include thickening of the basement membrane, hyperkeratosis, follicular plugging, and perivascular and perifollicular lymphocytic infiltration. Early diagnosis and treatment is important to prevent disfiguring alopecia, dyspigmentation and loss of self-esteem (Figure 2).6
Case continued
Microscopy and culture results were negative for fungus. A biopsy was not performed as the dermatologist was able to clinically diagnose limited DLE.
Question 3
What further investigations must be done once a diagnosis of DLE is confirmed?
Question 4
What is the most important preventive strategy in managing DLE?
Question 5
How would you manage her scalp lesions?
Question 6
What other preventive measures are appropriate for this patient?
Answer 3
DLE is an autoimmune, connective tissue disorder that can arise alone or as part of the disease spectrum of systemic lupus erythematosus (SLE).7 It was previously reported that 5–10% of DLE can progress to SLE within 3 years, but it is now understood to be an estimated 16.7%.7
Hence, on diagnosis of DLE, full screening for SLE should be conducted.8 Referral to a rheumatologist may also be necessary. Screening includes a thorough history for photosensitivity, joint pain, renal problems, fits and psychosis. A physical examination should look for signs of malar rash, oral ulcer, jaundice, pallor, serositis and arthritis. Investigations should include full blood examination, renal and liver function tests, urinalysis, inflammatory markers (erythrocyte sedimentation rate, C-reactive protein, antinuclear antibody/extractable nuclear antigen antibodies, double-stranded DNA and complement levels. The patient should be educated on the importance of periodic annual screening for SLE and to seek early consultation if symptoms are suggestive of SLE.
Answer 4
Sun protection is the most important preventive strategy as sunlight (ultraviolet (UV) A and B) can induce and exacerbate DLE lesions.9,10 Squamous cell carcinoma, as a result of chronic inflammation and absence of melanin in hypopigmented lesions, is a rare complication.11
The patient should be advised to avoid sunbathing, outdoor work and exposure to sunlight during the peak hours. If sun exposure is inevitable, she should apply sufficient amounts (2 mg/cm2 or about half a teaspoon for the face and neck) of sunscreen lotion with SPF of >50, 30 minutes before exposure and use sun-protective clothing and headwear.12 She should avoid tanning salons and prolonged exposure to fluorescent lights with high UV irradiation.10 She should be taught to recognise early malignant skin change.
Answer 5
In the management of DLE, we aim to reduce disease activity and prevent scarring alopecia.10,12 On the basis of the criteria set by the Oxford Centre for Evidence-based Medicine,13 there are no studies with Level 1 evidence for cutaneous lupus erythematosus treatment. From clinical experience, potent topical preparations from Class 1 or 2 corticosteroid are effective for limited DLE lesions. If these fail, intralesional corticosteroids can be used, but limited to small areas. Oral systemic steroid medicines are usually not necessary except in severe DLE because of significant side effects and the large dosage required. Other useful topical preparations that do not cause skin atrophy are calcineurin inhibitors (eg tacrolimus, pimecrolimus).
For extensive lesions, with or without systemic involvement, antimalarial treatment (eg hydroxychloroquine, chloroquine, quinacrine) remain the primary therapy,8,10,12,14 and may delay the onset of SLE.15 Hydroxychloroquine causes less severe effects on the retina, compared with chloroquine, and remains the first line antimalarial drug of choice.16 Patients on antimalarial treatment should undergo baseline and periodic retinal screening using newer, more objective screening tests.17
Vitamin A-derived oral retinoids are effective alternatives to antimalarial treatment, but are best avoided because of higher side effects and teratogenicity for women in child-bearing ages, unless covered by effective contraception during use and up to 3 months after treatment has ceased.8
Treatment of recalcitrant lesions include immunosuppressants (eg methotrexate, mycophenolate mofetil, azathioprine) and immunomodulators (eg dapsone).
Dyspigmentation and scarring can be camouflaged with cover cosmetics and use of hats, scarves and wigs.
Answer 6
She should be screened and monitored periodically for vitamin D levels. If there is a deficiency, vitamin D supplements (400 IU/day) can be prescribed to counteract the lack of sun exposure.10
Smoking exacerbates DLE,10 but there is controversy regarding its effects and whether it affects the response to treatment with antimalarials.18,19 Nevertheless, she should be advised to avoid secondary smoke exposure. Her husband should be strongly counselled to stop smoking for their health.
Key points
- DLE appears as red scaly patches, leaving post-inflammatory dyspigmentation and scarring.
- DLE may involve hair follicles and lesions elsewhere (eg cheeks, nose, ears, neck, upper back, hands).
- Non-reversible scarring alopecia will develop if hair follicles are destroyed.
- An estimated 16.7% may go on to develop SLE. Screening for SLE annually and looking for new symptoms is recommended.
- Sun protection is the most important preventive strategy as sunlight can induce and exacerbate lesions.
- Management is aimed at reducing disease activity, and this can be done with topical or intralesional corticosteroids.
- Monitor vitamin D levels for deficiency and prescribe supplements if necessary.
- Advise on the importance of smoking cessation.
Authors
Siew Kim Kwa MBBS Malaya, MSc Medical Demography (Univ of London), FAFPM (Academy of Medicine of Malaysia), FRACGP, Professor and Head, Department of Family Medicine, International Medical University, Seremban, Malaysia. kwaskim2@yahoo.co.uk
Esha Das Gupta FRCP (Lond), FRCP (Ire), Head of Division of Medicine, and Professor, Department of Internal Medicine, International Medical University, Seremban, Malaysia
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.
Resources
Useful websites: