Case
A previously well Lebanese woman aged 28 years, who wears a headscarf, presented to her general practitioner with a three-month history of an abruptly appearing, painful papule on the antihelix of her left ear. She denied any preceding trauma and had no personal or family history of skin cancer. She had type 3 skin on the Fitzpatrick scale. The lesion was a 4 mm papule with a central keratin plug (Figure 1) that was ‘exquisitely’ tender on palpation. Examination of lymph nodes in the neck was normal.
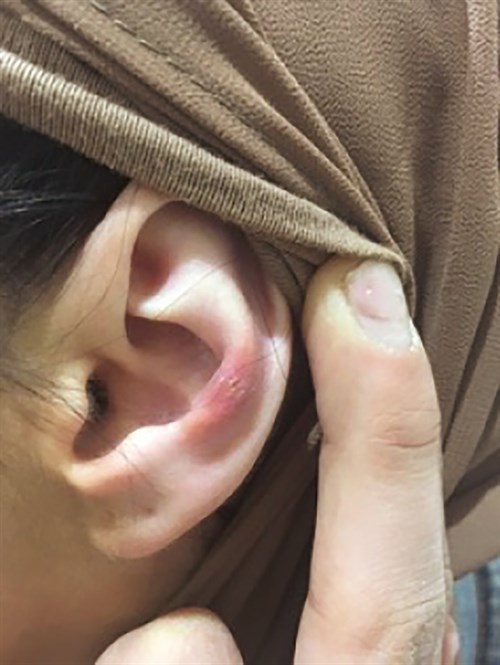
Figure 1. Inflamed papule on the antihelix of the left ear
Question 1
What are the important diagnoses to consider? How would you distinguish between these?
Question 2
How would you confirm the diagnosis?
Question 3
What is thought to be the cause of the diagnosed condition?
Question 4
What is the natural history of the diagnosed condition?
Question 5
What are the treatment options?
Answer 1
Diagnoses to consider are actinic keratosis, squamous cell carcinoma (SCC), basal cell carcinoma (BCC) and chondrodermatitis nodularis helicis (CDNH). The most important differential diagnosis to exclude is non-melanoma skin cancer, particularly SCC. In this case, SCC was considered unlikely because the patient was young and had very minimal exposure to ultraviolet light. The most useful discriminators are pain and tenderness, which are prominent in CDNH and usually absent in SCC and BCC. It is important to note that these features do not exclude malignancy but rather support a diagnosis of CDNH. Non-melanoma skin cancers are also typically accompanied by co-existent and/or a history of same lesions.
Answer 2
Diagnosis of CDNH is usually clinical, based on the rapid appearance of a site-specific nodular lesion, which may be centrally scaled, crusted or ulcerated, and with associated pain and tenderness. Characteristically, pain is initiated by pressure or changes in temperature lasting minutes to hours. A biopsy may be indicated in cases of uncertainty or failed response to treatment.
Answer 3
CDNH is believed to be caused by prolonged and excessive pressure (eg call centre headset or traditional head dress) on an anatomically predisposed area with relatively little subcutaneous protection and poor blood supply. Trauma, cold and actinic damage may provide the inciting event.1
CDNH may occasionally be associated with underlying inflammatory conditions, including autoimmune thyroiditis, systemic lupus erythematosus, dermatomyositis and scleroderma. These associations may be more frequent in cases involving younger females.2 Ordering of tests to investigate these causes should be clinically indicated. There is also a possible hereditary influence.3
Answer 4
Initially, growth of the lesion is rapid over a few months and then reaches a plateau, persisting for several months or even years. It rarely resolves spontaneously and will usually require some form of active treatment.4
Answer 5
Treatment options consist of general measures, and medical and surgical therapies. All patients should be advised to avoid excessive sun and cold exposure.
First-line therapy is local decompression. Patients should be instructed to sleep on the unaffected side and a doughnut-shaped pillow or foam padding may be useful. Any ongoing physical trauma to the ear (eg phone) should be minimised or, ideally, avoided altogether.
Conservative measures could be trialled for several weeks before proceeding to more invasive therapies.5
Intralesional corticosteroids (ie triamcinolone acetonide 10 mg/mL) may provide rapid symptom relief and even resolution in some cases; however, repeat treatments may be necessary.6 Cryotherapy can be attempted in the office setting. Topical nitroglycerin 2% has also been used with some success.7
For recalcitrant cases, where specific efforts to relieve pressure are unsuccessful, surgical approaches are almost always needed. Surgical options include curettage, electrocauterisation, carbon dioxide laser and excision.8 Surgical success relies on removal of the focus of damaged cartilage with relief of pressure. Surgery has a failure rate of 10–30%.9
Case continued
The patient was advised to loosen her headscarf and minimise use where possible. She also purchased a doughnut pillow to assist with sleeping. She was advised to return for review in two months.
She returned two months later with no improvement and was referred to a skin specialist. A 2 mm punch biopsy was consistent with CDNH. She received an intralesional corticosteroid injection and her condition resolved completely within four weeks.
Key points
- CDRH is caused by prolonged and excessive pressure on an anatomically predisposed area.
- Diagnosis is usually clinical and within the scope of general practice.
- SCC must be confidently excluded and this may require biopsy.
- Spontaneous resolution is rare so most cases will require some form of active treatment.
Author
Thomas Jonathan Stewart BBioMedSc (Hons), MBBS, General Practice Registrar, Kogarah, NSW. thomas_stewart@live.com
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.