Case
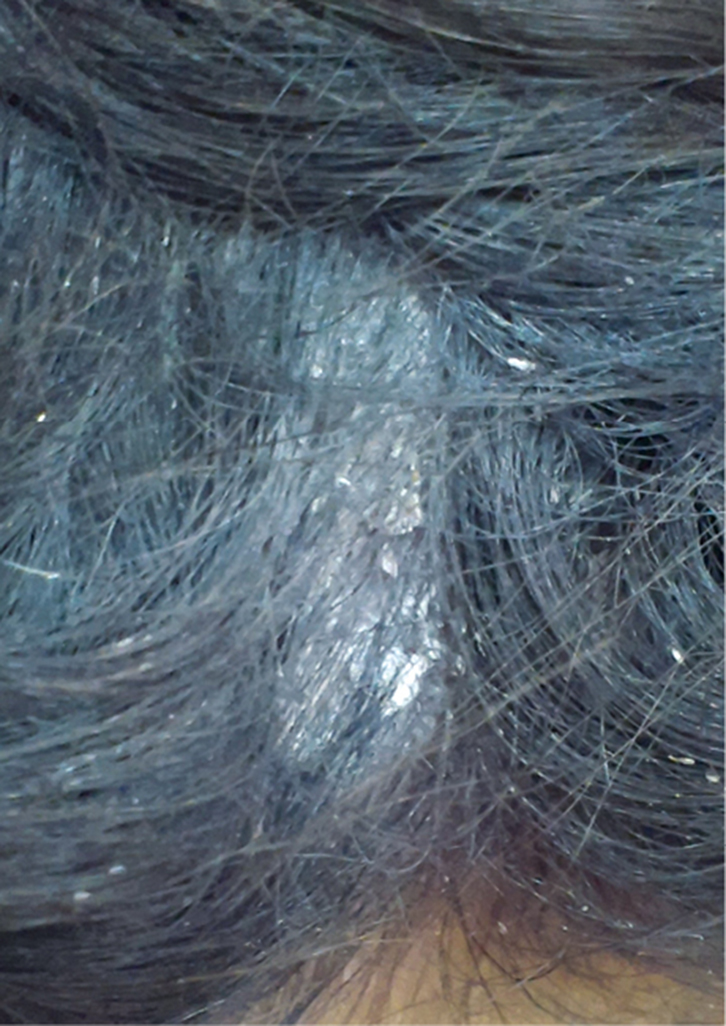 |
| Figure 1. Scaly plaque on the scalp with tufting of hair |
A girl, 8 years of age, was referred from the paediatrics outpatient department with complaints of itching and thick scaling on the occipital scalp for the previous 3 weeks. There were no other cutaneous or systemic complaints. The patient was afebrile and her general physical examination was within normal limits. She had a regular vaccination history, and past and family history were not contributory to the complaint. There was no personal or family history of atopy, allergy or other skin disease. Her body weight was 23 kg.
On examination, a thick, adherent, ‘asbestos-like’, scaly plaque with matted hair was present on the occipital scalp (Figure 1). There was no associated hair loss. The rest of the cutaneous examination, including external genitalia, oral mucous membranes and nails, was within normal limits and did not reveal any evidence of associated mucocutaneous disease.
Question 1
What is the diagnosis?
Question 2
What are the commonly associated diseases/infections?
Question 3
How should the condition be managed?
Answer 1
The diagnosis is pityriasis amiantacea (PA), sometimes also known as tinea or pseudotinea amiantacea. PA is an uncommon but specific reaction pattern to some of the inflammatory conditions of the scalp. The lesions of PA classically consist of thick, adherent, ‘asbestos-like’ (amiantaceus) scaling and plaques. These attach to the underlying scalp and piercing hair shafts and result in matting of the hair. The condition primarily affects young adults, although it may occur at any age.1 As in this case, females are more affected by PA than males.1 Temporary alopecia or hair loss is common, and scarring (cicatricial) alopecia has also been reported.2
Answer 2
In a number of patients, psoriasis,3 seborrheic dermatitis, atopic dermatitis and eczemas are commonly associated with PA. However, the exact aetiopathogenesis of this disease remains unclear. Mucocutaneous examination may be directed specifically to note:
- classic silvery-white scales, oil-drop sign and Auspitz’s sign of psoriasis
- greasy-yellow scale of seborrhoeic dermatitis
- classic flexural involvement with extreme itching and scratching of childhood atopic eczema
- associated head lice infestation of scalp.
Abdel-Hamid et al1 found that 83 of 85 patients with PA had a Staphylococcal infection, which was confirmed by bacterial culture. However, the aetiological role of S. aureus in PA is not defined. In many patients, however, no associated or underlying condition was identified. More recently, case reports have been published on the association of PA with Darier’s disease,4,5 and with tumour necrosis factor (TNF)-α inhibitor therapy for Crohn’s disease,6 tinea capitis7 and pityriasis rosea.8 Scrapings should be taken in suspected cases of tinea infections for a potassium hydroxide (KOH) microscopic examination of fungal elements, as well as for culture/sensitivity as necessary. Untreated tinea capitis as a cause of PA may sometimes lead to cicatricial alopecia. Rarely, scalp biopsy may need to be performed to define an unusual, underlying pathology (eg Darier’s disease) when PA is atypical, recalcitrant or poorly responsive to standard therapy.
Answer 3
At present, there are no specific guidelines for the management of PA. Mid-to-high potency topical corticosteroid preparations (eg mometasone, halobetasol, clobetasol), combined with salicylic acid and tar (sometimes with vegetable or mineral oils) may be left on the scalp overnight, followed by daily shampooing. This usually results in loosening of the scales and their removal. The steroid preparation needs to be applied to scalp for it to be effective. As the scales loosen after the morning shampooing, steroid lotions should be rubbed directly on the scalp.
Associated Staphylococcal1 or fungal7 infections, or other diseases (eg Darier’s disease),4,5 may need appropriate treatment or referral to a dermatologist as well. An antidandruff or tar-based shampoo would be helpful in maintaining remission once the condition is controlled. With appropriate therapy, hair will regrow in areas of associated hair loss, but the scarring from alopecia is usually irreversible.2
Patients need appropriate counselling, as PA usually responds well to treatment but may recur promptly when treatment stops. For our patient, we prescribed a topical lotion containing clobetasol propionate (0.05%) with salicylic acid, (6%) to be applied twice a day, and daily shampooing. She was also advised to apply plain coconut oil liberally on the scalp. A significant improvement was noted at the 2-week follow up after treatment.
Key points
- PA is an uncommon, distinctive reaction pattern of the scalp to some inflammatory conditions resulting in thick, adherent, ‘asbestos-like’ scaling and plaques, and sometimes alopecia.
- The aetiology is unknown. However, some cases are associated with psoriasis, seborrhoeic dermatitis, eczema and, rarely, Darier’s disease, tinea capitis and pityriasis rosea.
- The condition usually responds well to conservative treatment, but recurrences are frequent. Patient need proper counselling on regular follow-up.
Authors
Naveen Kumar Kansal MD, Assistant Professor, Department of Dermatology and Venereology, Government Medical College, Haldwani, Nainital, Uttarakhand, India. kansalnaveen@gmail.com
Saurabh Agarwal MD, Professor and Head, Department of Dermatology and Venereology, Government Medical College, Haldwani, Nainital, Uttarakhand, India.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.