Case
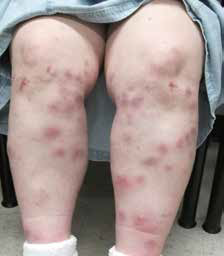 |
Figure 1. Multiple red lumps on the
anterior aspect of the lower limbs |
Ms W, 47 years of age, presented to your clinic with a 2-week history of multiple red lumps on both of her shins. She first noticed areas of redness, which quickly proceeded to lumps that were mildly itchy and tender. Her symptoms persisted throughout the day, with no relieving or exacerbating factors. She denied previous trauma to the lower limbs or allergies to food or medications. She had never smoked and drank alcohol very occasionally. She had no recent history of foreign travel. Her only other active medical condition was depression for which she had been taking the same dose of antidepressants for the past 4 years. She had no other current systemic symptoms. Ms W recalled having similar red lumps 6 years ago but they subsided without any treatment. Four years ago she was investigated for non-specific polyarthritis with a raised C-reactive protein, but no rheumatological diagnosis was made.
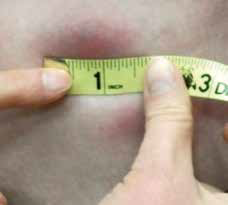 |
Figure 2. The lesions are indurated but
do not blanche upon pressure,
measuring up to 4 cm (1.5 inches)
in diameter
|
On examination, Ms W had a symmetrically distributed rash on the anterior aspect of both shins with multiple erythematous indurated lesions up to 4 cm in diameter (Figure 1). The erythema varied in hue from bright red to purple-brown, and the lesions were not well demarcated. The indurated areas were warm and mildly tender with no blanching or pitting (Figure 2). The overlying skin was intact and there were no signs of desquamation, ulceration or cutaneous oedema. There was no loss of hair and follicular structures were preserved.
Question 1
What is your clinical approach?
Question 2
What are the differential diagnoses?
Question 3
What investigations would you consider and why?
Answer 1
A detailed history and full clinical examination of the patient are necessary to help differentiate the skin eruption and determine the possible underlying causes and triggers. Highlights from the history include a relatively short presentation of 2 weeks, multiplicity of lesions that are erythematous and mildly tender, no recent trauma, external triggers or foreign travel. There was no change of medications, and a previous episode of undiagnosed polyarthritis. Clinical examination revealed a symmetric eruption on the shins with mild tenderness, non-blanching erythema and intact integument.
Answer 2
The list of differential diagnoses includes:
- skin infections
- acute fat necrosis
- necrobiosis lipoidica
- non-accidental injuries
- polyarteritis nodosa
- erythema nodosum.
The erythema and induration suggest an inflammatory condition either due to an infection or autoimmune processes. Common pathogens for painful erythematous skin infections include Staphylococcus aureus and Lancefield Group A Streptococcus pyrogenes. However, S. aureus often presents as pustules and abscesses, and haemolytic Streptococcus infection often leads to cellulitis and possible necrotising fasciitis. The pretibial skin of patients with inflammatory bowel disease and insulin-dependent diabetes is predisposed to necrobiosis lipoidica, but it commonly presents as a solitary, painless plaque with possible ulceration and skin atrophy. Acute fat necrosis is a form of lobar panniculitis, which can result in tender subcutaneous lumps on multiple sites of the body, but is caused by breakdown and death of fatty tissue as a consequence of mechanical or cold injury. Non-accidental injuries can present as multiple bruises of varying sizes and ages but increased warmth and induration at the site of lesions are unusual. Polyarteritis nodosa refers to a syndrome of necrotising vasculitis of small- to medium-size arteries and clinically presents with systemic upset and painful skin nodules (up to 2 cm) that may ulcerate.1 Both polyarteritis nodosa and erythema nodosum can resemble the lesions depicted, although the former commonly results in skin ulceration.
Answer 3
For possible skin infections and other dermatological manifestations of systemic infections, a full blood evaluation (FBE) is recommended. In view of the previous history of polyarthritis, updated indices for possible inflammatory arthritis such as erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), rheumatoid factor, and antinuclear antibodies (ANA) are necessary. A chest X-ray is of value to look for possible tuberculosis, atypical infection (eg mycoplasma) or sarcoidosis. Finally, a deep skin biopsy with a sufficient sample of subcutaneous fat taken from an acute lesion can be considered to enable definitive diagnosis for both granulomatous or pannicular pathologies.
Case continued
Blood was taken from Ms W and results for FBE, ESR and rheumatoid factor were all within the reference intervals but CRP was raised (55 mg/L, normal <8 mg/L). The chest X-ray showed prominence of hilar lymph nodes and reticulate opacities in both lungs, highly suggestive of sarcoidosis. Biopsy was deferred as discussed later.
Question 4
What is the final diagnosis?
Question 5
How would you manage this condition?
Answer 4
The final diagnosis was erythema nodosum secondary to sarcoidosis. The annual incidence of erythema nodosum is 1–5 in 100,000, affecting mostly females (M:F ratio of 1:4 to 1:6) with age predisposition from 15–40.1–3 Clinically, the classical picture of erythema nodosum is an acute eruption of single or multiple erythematous nodules on the extensor surfaces of the lower limbs and, to a lesser extent, the upper limbs and torso. The erythema is poorly demarcated and does not blanch on pressure. The nodules measure 1–10 cm in diameter and usually involute within 2–3 weeks of onset, taking on a characteristic green-yellow hue that can be indistinguishable from old bruises.1 Erythema nodosum lesions retain the integrity of overlying skin and rarely, if ever, ulcerate.1,2 Systemic symptoms can occur prior to eruption of erythema nodosum, which may include fever, malaise, weight loss, arthralgia or non-specific arthritis.3 These symptoms may also be due to the underlying diseases that trigger erythema nodosum (see below).
Pathology and aetiology of erythema nodosum
Erythema nodosum is a hypersensitive inflammatory response of subcutaneous fatty tissues to certain antigenic triggers. Classified as septal panniculitis, erythema nodosum is one of the commonest forms of panniculitis.4 Histologically, there are multiple areas of neutrophilic and eosinophilic infiltration around the blood capillaries and thickening of the septa in the adipose tissues.1,4 The formation of macrophage clusters around blood vessels or interlobular septa, known as Miescher’s radial granuloma, is a diagnostic marker for erythema nodosum.5 The exact pathogenesis of erythema nodosum is still unknown. The original hypothesis of circulating immune complexes6 proposed in the 1970s was refuted in the 1980s.7 Other theories include mediation via leucocyte activation and reactive oxygen intermediates;8 increased TNF-production (in sarcoidosis-associated erythema nodosum)9,10 and hypersensitivity to oestrogens and progesterone (in pregnancy-induced erythema nodosum).11 There are numerous triggers for erythema nodosum (Table 1), although 55% of cases are idiopathic.1,4
Table 1. Treatments for chronic skin ulcers
|
|
Causes of erythema nodosum
|
Occurrence (%)
|
|---|
|
Idiopathic
|
55
|
|
Bacterial infections (eg TB, Yersinia, chlamydia, Mycoplasma and Salmonella)
Viral infections (eg EBV, HSV, HBV, HCV, HIV)
Fungal infections
Parasitic infections (amoeba, giardia)
|
20
|
|
Sarcoidosis
|
13
|
|
Adverse drug reactions (eg, oral contraceptives, sulphur drugs, halide drugs)
|
6
|
|
Pregnancy
|
3
|
|
Inflammatory bowel disease (Crohn’s disease and ulcerative colitis)
|
2
|
|
EBV, Epstein-Barr virus; HBV, hepatitis B virus; HCV, hepatitis C virus; HIV, human immunodeficiency virus; HSV, Herpes simplex virus; TB, tuberculosis
|
|---|
Answer 5
Erythema nodosum per se is self-limiting and symptomatic treatment is sufficient. If there is an identifiable cause or trigger, it should be addressed to expedite recovery. For pain relief and resolution of lesions, non-steroidal anti-inflammatory drugs (NSAIDs) (eg ibuprofen 400 mg three times a day orally) and a pair of support stockings are beneficial.11 Bed rest and leg elevation also help. Studies have mentioned other therapeutic options, such as potassium iodide,2,11 dapsone,11 hydroxyquinone11 and colchicine,2,11 with varying efficacies. Corticosteroids are seldom used systemically. Intralesional triamcinolone injection had been reported to be beneficial but further evidence is needed to ascertain their efficacy.12 Finally, where available in other countries, biological treatment with anti-TNF agents is supported by recent Italian studies.13,14 Prognosis for erythema nodosum is generally good except for idiopathic cases. In a 10-year longitudinal study of 100 patients with erythema nodosum, it was found that patients with idiopathic erythema nodosum have a much higher annual relapse rate (62%) as compared with erythema nodosum with an identified cause (1%).3,15
Case conclusion
|
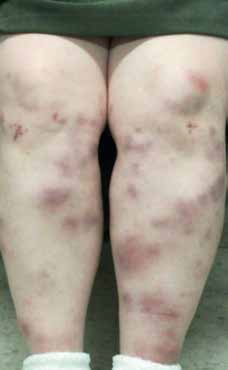
Ms W was instructed to take a regular dose of NSAIDs with web bandaging of her lower limbs and most of her symptoms subsided within 1 week. The eruption evolved to a green-brown colour, reminiscent of old bruises (Figure 3). In view of the clinical progress and the suspected underlying sarcoidosis, skin biopsy was deferred and the patient was referred to a rheumatologist and pulmonologist for further assessment. A computed tomography scan of the chest, and blood tests for serum angiotensin converting enzyme level and serology for Yersinia and mycoplasma were arranged while waiting for the specialist appointments.
Summary
Erythema nodosum is a benign skin condition that typically resolves in 6–8 weeks without any treatment. The morphology of erythema nodosum lesions may mimic a number of other skin conditions, and a detailed history and clinical examination with appropriate investigations are essential to differentiate erythema nodosum from other more sinister diagnoses (eg polyarteritis nodosa or non-accidental injuries). Identification of possible triggers is also important for diagnosis and management of erythema nodosum.
|
 |
|
Figure 3. Patient reviewed at day 4,
taking non-steroidal anti-inflammatory
drugs for symptomatic relief. Note the
deepening hue of the rash to
purplebrown, similar to organising
bruises
|
|
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.
References
- Cox NH, Jorizzo JL, Bourke JF, Savage COS. Vasculitis, neutrophilic dermatosis and related disorders. In: Burns T, Breathnach S, Cox N, Griffiths C, editors. Rook’s Textbook of Dermatology. 8th edn. Oxford: Wiley-Blackwell, 2010;doi: 10.1002/9781444317633.ch50.
- Gilchrist H, Patterson JW. Erythema nodosum and erythema induratum (nodular vasculitis): diagnosis and management. Dermatol Ther 2010;23:320–27.
- Mert A, Kumbasar H, Ozaras R, et al. Erythema nodosum: an evaluation of 100 cases. Clin Exp Rheumatol 2007;25:563–70.
- Schwartz RA, Nervi SJ. Erythema nodosum: a sign of systemic disease. Am Fam Physician 2007;75:695–700.
- Sanchez Yus E, Sanz Vico MD, de Diego V. Miescher’s radial granuloma. A characteristic marker of erythema nodosum. Am J Dermatopathol 1989;11:434–42.
- Jones JV, Cumming RH, Asplin CM. Evidence for circulating immune complexes in erythema nodosum and early sarcoidosis. Ann N Y Acad Sci 1976;278:212–19.
- Nunnery E, Persellin RH, Pope RM. Lack of circulating immune complexes in uncomplicated erythema nodosum. J Rheumatol 1983;10:991–94.
- Kunz M, Beutel S, Brocker E. Leucocyte activation in erythema nodosum. Clin Exp Dermatol 1999;24:396–401.
- Labunski S, Posern G, Ludwig S, Kundt G, Brocker EB, Kunz M. Tumour necrosis factor-alpha promoter polymorphism in erythema nodosum. Acta Derm Venereol 2001;81:18–21.
- McDougal KE, Fallin MD, Moller DR, et al. Variation in the lymphotoxin-alpha/tumor necrosis factor locus modifies risk of erythema nodosum in sarcoidosis. J Invest Dermatol 2009;129:1921–26.
- Acosta KA, Haver MC, Kelly B. Etiology and therapeutic management of erythema nodosum during pregnancy: an update. Am J Clin Dermatol 2013;14:215–22.
- Requena L, Yus ES. Erythema nodosum. Dermatol Clin 2008;26:425–38.
- Passarini B, Infusino SD. Erythema nodosum. G Ital Dermatol Venereol 2013;148:413–17.
- Zippi M, Pica R, De Nitto D, Paoluzi P. Biological therapy for dermatological manifestations of inflammatory bowel disease. World J Clin Cases 2013;1:74–78.
- Mert A, Ozaras R, Tabak F, Pekmezci S, Demirkesen C, Ozturk R. Erythema nodosum: an experience of 10 years. Scand J Infect Dis 2004;36:424–27.