Case 1 Arya
Arya, 4 years of age, sustained a deep laceration on her thigh after striking it on a tree branch. The wound is 5 cm long, gapes slightly, and will require some form of wound closure.
Question 1
When considering preparation for the wound cleaning and closure procedure for Arya, which one of the following is CORRECT?
- You should avoid explaining what you are going to do to her.
- She will probably need procedural sedation if she is not able to cooperate.
- Distraction techniques are generally unhelpful.
- It is best if you keep all instruments where she can see them.
- Her parents should be asked to leave the room as they are likely to add to her distress.
Question 2
Which one of the following is CORRECT regarding pain control for Arya before wound cleaning and closure?
- You should consider using a topical anaesthetic on her wound as this approach is supported by strong evidence.
- ALA (Laceraine), a combination of amethocaine, bupivacaine and adrenaline, may be injected into the skin surrounding her wound.
- EMLA (eutectic mixture of local anaesthetics) can be applied directly to her wound.
- If using ALA, her parents should be informed it has not been approved for use by the Therapeutic Goods Administration.
- You may safely use as much ALA as needed to anaesthetise Arya’s wound.
Question 3
In order to minimise Ayra’s discomfort on injection of local anaesthetic, which one of the following approaches is best?
- Mix the lignocaine with sodium bicarbonate solution to increase the pH.
- Use a large bore needle.
- Cool the lignocaine solution in the fridge prior to use.
- Inject the anaesthetic rapidly.
- Inject through the intact skin adjacent to the wound.
Question 4
Which one of the following will result in the best cosmetic outcome?
- Avoiding scrubbing of Arya’s wound to remove dirt and gravel
- Using absorbable rather than non-absorbable sutures
- Using tissue glue rather than sutures
- Using a series of small strips of adhesive tapes rather than sutures
- Covering the scar for a minimum of 3 months with protective tape
Case 2 Tyrone
Tyrone is a nursing home resident aged 84 years. You are asked to see him to review a wound he has developed on his left lower leg over the past few weeks. You suspect he may have an arterial ulcer.
Question 5
Which one of the following is typical of arterial ulcers?
- They are usually irregular in shape.
- They have a purple discolouration of the peri-skin.
- They most commonly occur below the ankle.
- Skin changes may include atrophy blanche.
- The degree of pain is related to the size of the ulcer.
Question 6
Which one of the following treatments might Tyrone require for his ulcer?
- Avoiding long periods standing
- A graduated compression stocking applied from toe–knee
- Amputation
- Cessation of calcium channel blockers
- Elevation of his legs when possible
Question 7
Several weeks later Tyrone develops a skin tear on his shin after bumping it on a chair. Which one of the following is CORRECT regarding skin tears?
- Skin tears are the third most common wound type in the elderly after venous and arterial ulcers.
- Applying moisturising lotion twice daily may significantly reduce skin tear incidence.
- The ageing process leads to increased blood supply to the skin and difficulty controlling bleeding from skin tears.
- Treatment involves replacing the flap and holding it in place with adhesive strips applied with maximal tension.
- Compression bandages should be avoided after dressing the wound.
Question 8
Which one of the following is an appropriate strategy to address factors that may affect the healing of Tyrone’s wounds?
- Reducing his dietary arginine intake
- Avoiding wound surface drying
- Cooling the affected areas to <36°C
- Cleansing the wounds regularly with antiseptic
- Commencing Tyrone on a course of a non-steroidal anti-inflammatory drug
Case 3 Chantelle
Chantelle is 78 years of age and has a history of heart failure. She attends your clinic for management of an ulcer above her right medial malleolus. Chantelle is very stoic, lives at home alone and has good cognition. However, you are aware that her diet is nutritionally poor, as she is unable to drive (her late husband used to drive for her) and she refuses meals on wheels. About 30% of the ulcer comprises necrotic tissue and about 60% lacks evidence of epidermal reconstruction. It has a smelly exudate and previous swabs confirm colonisation with Staphylococcus aureus. She experiences significant itch around the wound. Her ankle brachial index (ABI) is 1.3.
Question 9
Which one of the following is CORRECT regarding assessment of Chantelle’s wound?
- The TIME acronym can be used to develop an individualised management plan for her.
- Photographs of the wound are of limited use in this situation.
- Her ABI excludes arterial occlusion.
- Testing of sensation around her feet should be performed using a 20-gauge cannula.
- The distal location suggests it may be an atypical ulcer.
Question 10
What is Chantelle’s TIME-H score?
- 3 (certain healing)
- 6 (certain healing)
- 8 (uncertain healing)
- 11 (uncertain healing)
- 13 (difficult healing)
Question 11
Which one of the following is the correct management of Chantelle’s ulcer?
- Debridement should be performed as infrequently as possible to allow tissue regeneration
- Application of 3-layered bandaging would be beneficial if it is a venous ulcer but would increase overall bandage costs.
- Chantelle should be asked regularly about pain, as increasing pain in a chronic wound is a reliable indicator of infection.
- Silver-based dressings should be used to manage her malodorous exudate.
- Topical steroids should not be used to control the itch around the wound.
Question 12
You are deciding which dressing to use for Chantelle’s ulcer. Which one of the following is the correct regarding your dressing options?
- Alginate dressings are useful for dry wounds with covering fibrin and necrotic tissue.
- Hydrofibre dressings are useful for non-infective wounds.
- Hydrocolloid dressings are useful for wounds in the terminal stage of the clearing process.
- Cadexomer iodine dressings are useful for wounds with malodorous exudates.
- Foam dressings are useful for infective wounds.
Case 4 Eddard
Eddard is a fisherman aged 38 years and recently returned to Australia after working off the coast of Sri Lanka for 8 months. He has become worried about a lesion on his left leg over the past couple of weeks.
Question 13
Which one of the following features would suggest that Eddard has a simple bacterial tropical ulcer?
- The lesion occurred at a site of previously intact skin.
- He is feeling weak and lethargic.
- The lesion is spreading very slowly.
- He has not had any fevers.
- The lesion is not painful.
Eddard explains that the lesion is not painful and he feels well. He tells you it actually started as a small bump a couple of months ago and has been growing slowly. The ulcer in the middle developed 2 weeks ago, which is when he began to worry about it. On examination, his lesion has the appearance in Figure 1.
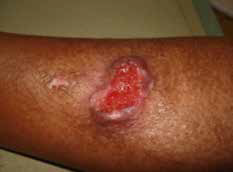
Figure 1.
Question 14.
Which one of the following is the most likely diagnosis?
- Acutaneous leishmaniasis
- Tuberculosis
- Chromocycosis
- Mycetoma
- Lupus vulgeris
While examining Eddard, you also notice his left hand has some lesions on it (Figure 2).
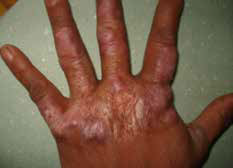
Figure 2.
Question 15.
Which one of the following is the most likely causative organism?
- Mycobacterium ulcerans
- Sporothrix schenckii
- Cladosporium carrionii
- Mycobacterium marinum
- Pseudallescheria boydii
Question 16.
Which one of the following would be appropriate treatment for the lesions on Eddard’s hand (Figure 2)?
- Oral terbinafine
- Streptomycin injections
- Oral clarithromycin
- Oral itraconazole
- Potassium iodide solution topically