GP supervisors are well placed to contribute to increasing high-quality primary care research for several reasons. Good teachers promote intellectual rigour in their discipline and contribute to the body of knowledge in which they teach.8 On a pragmatic level, they work intensively for at least 6 months with registrars in training practices, and can thus influence their registrars’ attitudes towards and experience of research. Furthermore, GP supervisors are experienced and respected GPs who can contribute to research at a local level. Evidence to guide clinical management and teaching is more likely to be generated if GPs take an active role in promoting research that answers questions that matter to GPs and their patients.9,10 Research undertaken in primary care settings can increase the applicability and the translation of knowledge to practice.11
Previous research indicates GP supervisors have positive attitudes towards research, and are interested in increased research involvement.7 This paper reports on an initiative, undertaken in a partnership between a regional training provider (RTP) and two medical schools in western Sydney; it aimed to explore this further and develop strategies to increase the research capacity of GP supervisors.
GP supervisor research capacity building consultation
Supervisors were invited to attend optional 90-minute workshops within two training days in 2010 and 2011. Members of the project team, comprising representatives of the two medical schools, acted as facilitators. A total of 31 GP supervisors participated, representing 32% of supervisors working with the RTP. Two facilitators gave a 20-minute presentation on medical school research activities, the importance of general practice research and the principles of EBM. GPs then divided into small, facilitated groups of 4–6 and discussed questions such as ‘What are your training needs/research interests?’ and ‘What would you need to increase your research involvement?’. The groups presented key points back to the larger group for further discussion, which was recorded through handwritten notes.
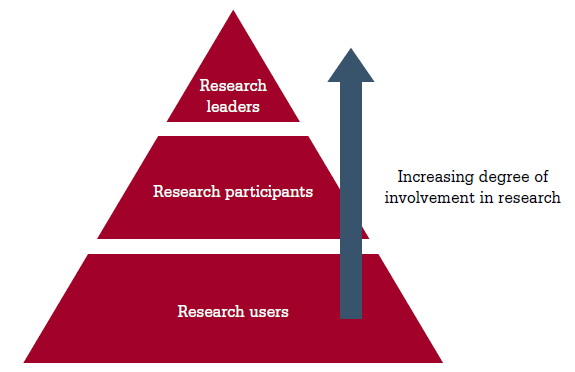
Figure 1. Glasziou’s triangle: levels of GP research engagement
Reproduced with permission from the Royal Australian College of General Practitioners from Del Mar C. Publishing research in Australian Family Physician. Aust Fam Physician 2001;30:1094–95.
Subsequent to the workshop, the facilitator notes were categorised and analysed using Glasziou’s triangle of the levels of research engagement12 (Figure 1) in a framework approach.13 Glasziou’s model highlights GPs’ different levels of research interest and skills, from the large base of GPs who are translators of research into practice, or ‘research users’, through to the smaller group of GPs who engage in research as participants or leaders. The needs, motivations and barriers to GPs increasing their use of research findings and research engagement, and enabling strategies that could be put in place by the universities and the RTP, were considered within this framework (Table 1). Capacity building strategies to meet supervisors’ expressed needs were further developed through project team discussions. The results were presented back to and discussed with supervisors in a series of four supervisor regional training meetings to check that the understanding of their needs was correct and the proposed strategies were appropriate.
Table 1. GP supervisor views on increasing their EBM and research skills
| Needs | Motivations | Barriers | Enabling strategies |
|---|
| Research users |
Increased confidence and time efficiency in accessing evidence |
Using EBM as part of quality clinical practice
Effective teaching |
Time pressures of clinical practice
Lack of familiarity with suitable resources |
Increased use of synthesised evidence-based summaries
Training, including EB journal clubs |
| Research participants and potential leaders |
Increased research skills
Increased opportunities and support to participate in research |
Promotion of research which is important to primary care
Professional development
Personal clinical interest areas |
Time constraints
Low awareness of evidence gaps
Inadequate research skills, including literature searching and critical appraisal |
Increased access to and awareness of literature evidence to identify evidence gaps
- Training, including EB journal clubs
- University affiliation (including library access to increase access to full text journals)
- Collaborative mechanisms at a local level to collect Supervisor views on research priorities
Increased research skills
- Research skills training
- Researcher fellowships with academic supervision
Increased support to enable research participation
- Inter-practice collaboration, including data sharing & supported networking (PBRNs)
- Infrastructure, including up-skilled practice staff, visiting and centralised research support (university, RTP or Medicare Local)
|
GP supervisors’ views on their research capacity and needs
As summarised in Table 1, supervisors reported varying degrees of interest in research, and subsequently different needs, motivators and barriers to using and participating in research. For all supervisors, the time pressures of general practice were agreed to be the primary barrier to becoming more active research users and participants, and a central consideration to research capacity building strategies. There was consensus that RTPs had a role in developing GP supervisor research capacity. Affiliation with a university was seen as an attractive opportunity by some.
Research users – translators of research into practice
The majority of supervisors were interested in more actively using research evidence to guide clinical management and teaching. Their key need was improved ability to access evidence efficiently, given the time pressures of general practice. Other expressed needs were awareness of the evidence-based resources that their registrars and students were taught to use and an improved understanding of research methodologies.
Research participants and leaders
Some supervisors had experience as research participants and others felt that, given appropriate opportunities and support, they would be interested in increasing their research participation. No supervisors considered themselves to be research leaders, but they were interested in contributing to the research agenda in their region through identifying research areas that would inform practice and improve patient outcomes. However, it was evident in the group discussions that supervisors would initially need support to search the literature for answers to their questions – lack of time and literature searching skills meant they were not fully aware of evidence gaps.
This group was also interested in research methodology training, particularly focussing on research they could undertake using existing practice data, potentially in collaboration with other practices. Systems to support practice-based research were considered crucial to allow GPs to participate in research without undue time and paperwork burden. Collaboration of practices through research networks was attractive if supported with adequate infrastructure, including support staff at the university, RTP or Medicare Local level.
Increasing capacity: next steps
Despite the interest of GP supervisors in developing their research skills and activity, they identified important barriers to this. Different enabling strategies are required according to whether supervisors want to increase their role in using research evidence to guide practice and teaching or to increase their participation in research.
For those supervisors who are mainly research users, training in how to access research evidence in a timely manner may assist. An underused source of support is point-of–care, evidence-based summaries, which provide electronic access to pre-appraised and synthesised research evidence.14 This can be used during consultations or teaching sessions without pre-planning or requiring critical appraisal of research evidence, which may be impractical for the time-poor, less research-focussed GP. There is evidence that synthesised summaries increase the ability of GPs to answer questions to inform clinical decisions more quickly compared to their usual on line resources.15 Such summaries include Dynamed16 and others that are available on subscription or through university libraries.
Evidence-based (EB) journal clubs are another strategy to increase GP research users’ confidence and skills in identifying and critically appraising research evidence to inform practice.17 GPs choose a question from their clinical practice, seek and appraise the evidence, and then consider how it may apply in their setting.18 In addition to promoting the incorporation of research evidence into teaching and practice, EB journal clubs may help bridge the gap between GP supervisors’ desire to contribute to the research agenda and their lack of awareness of up-to-date research in their areas of interest. Important primary care questions for which there is little evidence to guide practice may be generated and promote research useful to GPs and their patients.
For those keen to increase their research participation or move towards leading research, more support and attractive opportunities are required. Supervisors, already linked through their RTP and regularly attending events which build collegiality, could collaborate as a practice-based research network (PBRN) given support by RTPs and universities. Described as the laboratories of primary care research, PBRNs are groups of primary care practices devoted to the healthcare of patients and to the investigation of questions related to community-based practice and improvement of the quality of primary care.19 PBRNs may allow GP training practices to contribute to research that informs their clinical care, enhances their discipline and involves the registrars and students they are training. However adequate in-practice and centralised support, including research staff who performed most of the time-consuming research activities, is needed to make this viable. Research fellowships, supported through funded, protected time and university-based academic supervision, may be attractive to supervisors who want to increase their research knowledge and skills.
GP supervisors whose views were collected in this consultation may have been more interested in research given their attendance at the optional workshops. However the reported needs, motivations, barriers and potential enablers are likely to be common to many supervisors with a similar level of interest across diverse RTPs. This project builds on previous evidence that GP supervisors are interested in increasing their research skills and involvement, and proposes some strategies RTPs and other relevant organisations could use to enhance supervisor research capacity.
Conclusion
Given their central role in training of GP registrars and their experience and existing regional links, GP supervisors are well placed to take a more active role in research, both as translators of research into practice and as active participants or leaders in primary care research. Increased skills in accessing research evidence efficiently and supported involvement in research would enhance busy GP supervisors’ ability to incorporate EBM and research supervision into their teaching and to model engagement with research to their registrars and students. This would require in-practice and centralised regional support that could be facilitated by RTPs, universities and Medicare Locals, and would allow interested training practices to participate in research as collaborative networks.
Competing interests: None.
Ethics approval: This project was determined as exempt from Ethics Review by the Ethics Committee of the University of Western Sydney.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgements
The authors would like to thank the regional training providers and GP supervisors who informed this paper.