Pathophysiology
Dental infections arise when the hard outer coating of the tooth, the enamel, is compromised and the inner dentin is exposed, which exposes microtubules to the pulp chamber. These microtubules form a direct path for bacteria to invade from the oral cavity into the vascularised pulp, resulting in pulpitis and causing acute pain. At this stage the inflammation is contained within the tooth structure. If not treated by a dentist, the infection may spread into and destroy the local alveolar bone and form a small periapical abscess. Subsequent erosion of the cortical plate in the jaw allows bacteria to spread along tissue planes into potential spaces of the face and neck, depending on the specific tooth or teeth involved and the site of erosion.8,9
Most dental infections will decompress through the gingiva or mucosa into the buccal space but deep extension is more likely when the mandibular molars are involved, as their root structures lie close to the cervical fascia. Extension from these teeth can be laterally into the submasseteric space or medially into the submandibular space. Further progression along these planes will lead to the submental and sublingual spaces and ultimately result in airway compromise by entering the parapharyngeal spaces and mediastinum.10,11
Maxillary teeth generally do not cause such problems but, instead, infection may extend infraorbitally causing peri-orbital cellulitis and, in severe cases, enter the cavernous sinus, causing cavernous sinus thrombosis and visual loss. Additionally, infection from maxillary teeth can spread into the cranial vault and cause encephalitis or meningitis.9
Assessment
Assessment of patients with a presumed dental infection is no different from that required for other conditions. Following a primary survey to assess airway, breathing and circulation the clinician should take a detailed history, perform a physical examination and order relevant investigations.
Symptoms of early dental infections include localised pain, facial swelling, halitosis and general malaise. There is often a long history of dental pain and the patient may have had prior dental treatment such as root canal therapy.12 As the infection progresses, the patient may complain of the much more serious features of trismus, dysphagia, dyspnea, inability to protrude the tongue or swallow saliva, hoarse voice and stridor. The patient may lean forward in an effort to open their own airway.
The most important feature on examination is the patency of the airway. If there is any doubt, the patient should be placed in an environment, such as an emergency department, where an unstable airway can be appropriately managed and the oral and maxillofacial unit should be informed.
The face should be examined for swelling and induration. If present, the extent of these features and whether they have crossed the lower border of the mandible should be determined. Ask the patient to open their mouth as wide as they can and measure the distance between the medial incisors: a distance of <20–30 mm means that it will be difficult to intubate the patient and nasal intubation or a surgical airway may be required. Ask the patient if they can protrude their tongue and swallow, as the inability to do so may be due to an infection in the sublingual space that is raising the floor of the mouth and posteriorly displacing the tongue.10
The oral cavity should be examined using a light source, looking for buccal swelling or a visible punctum. Each tooth should be examined individually for appearance, mobility and percussion tenderness. It is useful to understand the different numbering systems for teeth when referring to dentists or oral and maxillofacial surgeons. The most common system involves two numbers: the first number denotes the quadrant, 1 being the upper right and progressing clockwise to 4 as the lower right; the second number, 1–8, denotes medial to lateral (Table 1).
The examination should include other causes of the presenting complaint as it may not be dental in origin; for example, tonsillar and salivary gland infections may cause lower facial swelling and dysphagia, and acute sinusitis or ear infections can cause upper facial swelling.
Table 1. Schematic representation of tooth numbering system used in Australia
| Upper right | Upper left |
|---|
| 18 |
17 |
16 |
15 |
14 |
13 |
12 |
11 |
21 |
22 |
23 |
24 |
25 |
26 |
27 |
28 |
| 48 |
47 |
46 |
45 |
44 |
43 |
42 |
41 |
31 |
32 |
33 |
34 |
35 |
36 |
37 |
38 |
| Lower right | Lower left |
|---|
Investigations
Relevant investigations include simple blood tests, such as a full blood count and electrolytes, and an orthopantomogram (OPG) to assess the dentition (Figure 1). If the patient has generalised symptoms, blood cultures should be taken. Blood tests such as C-reactive protein do not often change the patient’s management.
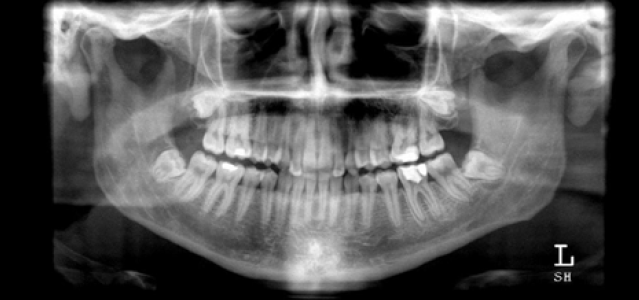
Figure 1. Orthopantomogram
A contrast computed tomography (CT) scan of the neck and lower face should only be performed if the patient’s presentation warrants it, for example, to identify a deep space infection.8 If the patient is not stable enough for a CT or the assessment does not warrant a CT, an OPG may be sufficient. If there is doubt as to the type of imaging required, it is prudent to consult the oral and maxillofacial team.
Management
The severity of the infection will dictate whether the patient can be managed as an outpatient under the care of a dentist, or if they will require referral to a hospital emergency department.
If the patient has airway compromise, significant facial swelling or trismus, is systemically unwell or has significant medical comorbidities, they will require admission for incision and drainage of the abscess, extraction of unrestorable teeth and possible placement of external drains.
If the patient does not require admission they should be referred to a dental practitioner for prompt evaluation and consideration of tooth-saving techniques or buccal incision, drainage and extraction of unrestorable teeth. Many patients and clinicians assume that antibiotics alone are definitive treatment. This is not the case. Definitive treatment can be administered only by the dental practitioner.
If the patient cannot attend the dentist that day, it is advisable to commence antibiotics and ensure the referral is completed as soon as possible. Dental infections are often caused by the normal oral flora and are polymicrobial, including a mixture of anaerobic and aerobic bacteria. The antibiotic chosen must target these groups of organisms and, for outpatients, a combination of a penicillin and beta-lactamase inhibitor or metronidazole provides appropriate cover.13,14
A widely believed myth is that a course of antibiotics is necessary before extraction of an infected tooth to prevent seeding into the cervicofacial spaces. Waiting for the infection to settle before extracting the tooth can result in life-threatening consequences as the infection spreads along the tissue planes. Teeth can be extracted in the presence of an acute infection; indeed, extraction of the offending tooth is often curative. It is a pitfall to assume that a course of antibiotics will definitively treat an established infection and this attitude often leads to prolonged morbidity and the potential for the infection to progress into a life-threatening condition.12,15
An appointment with a dentist should be organised for the patient as this increases compliance. This should be carefully recorded in the patient’s record. Unfortunately, for many patients, Medicare does not cover dental services unless the patient holds a healthcare card.
Conclusion
Practitioners who are likely to treat patients with dental infections should understand the pathophysiology, management and complications of such infections. It is important for practitioners and patients to understand that antibiotics alone are insufficient. Definitive management, whether surgical or dental, is the gold standard and is best provided as soon as possible to prevent serious illness or death. To provide antibiotic treatment alone without proper referral to a dental practitioner in the first presentation is indefensible should the patient’s condition subsequently seriously deteriorate. Furthermore, it is recommended that medical schools incorporate fundamental dental education as part of their curriculum.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.