Case
A girl, three years of age, with neurofibromatosis type 1 (NF1) presented with two lesions for review. Both lesions had been present since birth and were not causing any concern. The lesion on her scalp (Figure 1) was absent of hair and the one on her left upper back (Figure 2) was more noticeable after a bath.
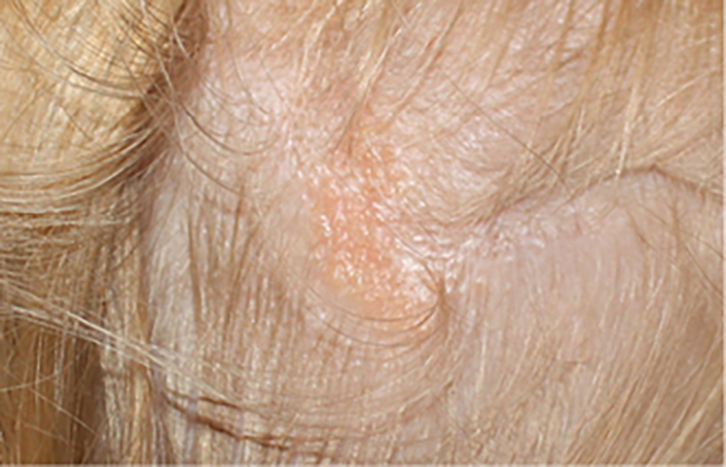
Figure 1. Waxy pink plaque on the scalp with absence of hair
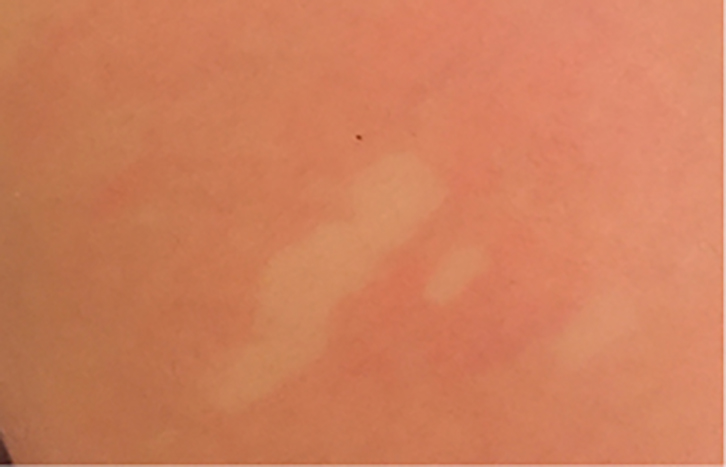
Figure 2. Pale macules with surrounding erythema brought on by rubbing the area
Question 1
What is the lesion shown in Figure 1?
Question 2
What are the possible complications of the lesion shown in Figure 1?
Question 3
What is the management of the lesion shown in Figure 1?
Question 4
What is the lesion shown in Figure 2?
Question 5
How is the lesion shown in Figure 2 diagnosed and what is its pathophysiology?
Question 6
Is there an association between the lesion shown in Figure 2 and NF1?
Question 7
What is the management of the lesion shown in Figure 2?
Answer 1
The lesion shown in Figure 1 is a sebaceous naevus or nevus sebaceous of Jadassohn.1,2 It is an uncommon, benign, congenital hamartoma of the skin that comprises a combination of skin structures including hyperplastic epidermis, sebaceous glands, immature hair follicles and apocrine glands.1,2 In infants and children, they present as pale, waxy, hairless plaques with a yellow–tan verrucous top and are usually diagnosed by clinical appearance alone.1,2 In adolescence, under hormonal influences, they become more pronounced and verrucal in appearance.1,2 Most lesions (95%) are located on the face or scalp,3 and the size ranges from one to several centimetres.2 Rarely, they form part of a syndrome called sebaceous naevus syndrome, which involves disorders of the eye, brain and skeleton.1,2
Answer 2
Both benign and malignant skin lesions can arise in sebaceous naevi. The most common benign lesions include syringocystadenoma papilliferum and trichoblastoma.1 Malignant growths are uncommon (5–22% of cases) and basal cell carcinoma (BCC) is by far the most common of these.2–4 Squamous cell carcinoma (SCC), sebaceous carcinoma and adnexal carcinoma can also occur.1 Most of these malignancies occur in adulthood, although rare cases of malignant growth in childhood have been reported.2,4,5
Answer 3
Management of sebaceous naevi is controversial. Some studies suggest early excision and others advocate long-term monitoring with excision, as necessary, for malignant growth.1,2,5,6 Long-term monitoring can be problematic as malignant lesions arising in sebaceous naevi may not present with their usual diagnostic features, making diagnosis difficult.3 A sensible approach is to monitor for any changes during childhood, when the risk of malignant transformation is low, and consider performing full thickness excision just prior to adolescence, when the risk increases.7 The lesion may also be excised to reduce the nuisance value with grooming or to remove the hairless area for cosmetic reasons. At any stage, if any changes occur within a sebaceous naevus (eg rapid growth, irritation, ulceration), it should be reviewed by a dermatologist and biopsied or removed by full-thickness excision.1,3
Answer 4
The lesion shown in Figure 2 is a naevus anaemicus.
Answer 5
Naevus anaemicus is diagnosed clinically.8 It presents as an asymptomatic pale macule and is roughly round, oval or linear in shape.8 The main patch may be surrounded by satellite macules and is usually located on the trunk.8,9 It is present from birth; however, it may not be noted until the individual is much older.8
Naevus anaemicus is caused by a localised vascular hypersensitivity to catecholamines that results in permanent vascoconstriction and pallor.8,9 Putting a warm compress over the area or scratching it will not induce vasodilation signified by erythema.8,9 Diascopy, which involves putting a glass slide over the lesion and blanching the surrounding skin, reveals no border between the lesion and normal skin.8,9 The diagnosis is normally made from history and examination alone. However, if the skin were biopsied, it would reveal normal skin and melanocytes.8
Answer 6
In one study, 8.8–51% of children with NF1 were found to have naevus anaemicus.10 Before the age of two years, 50% of children with sporadic NF1 present with only one of the seven criteria for NF1 (Box 1), making the diagnosis of NF1 difficult during this time.11 As naevus anaemicus is present since birth, it may be a possible indicator of NF1 in young infants with only one criteria of NF1 present,10,11 but further research is required to substantiate this.
Box 1. Diagnostic criteria forneurofibromatosis type 1 (NF1)11,12
|
A diagnosis of NF1 is established by the presence of at least two of the following criteria:
- six or more café au lait macules >5 mm (prepubertal) and >15 mm (postpubertal)
- two neurofibromas or one plexiform neurofibroma
- axillary or inguinal freckling
- Optic glioma
- two or more Lisch nodules (iris hamartomas)
- a characteristic bone lesion (pseudoarthrosis or sphenoid dysplasia)
- a first-degree relative with NF1.
|
Answer 7
Management of naevus anaemicus involves reassurance and cosmetic measures as needed.1
Key learning points
- Malignant lesions may form in sebaceous naevi and close monitoring is recommended. Sebaceous naevi may be excised at the onset of puberty or they may be observed and full-thickness excision performed if any changes occur.
- Naevus anaemicus is a benign condition involving a localised abnormal vascular response to catecholamines that results in permanent vasoconstriction in the dermis. Diascopy results in loss of the border between the lesion and normal skin.
Author
Christie Beveridge FRACGP, BMed, DipChildHealth, General Practitioner, 76 Prince Medical and Orange Dermatology, Orange, NSW. cbeveridge@ausdoctors.net
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.
Acknowledgements
The author thanks Dr Michelle Y McRae MBBS (Hons), FACD, BEng (Hon1), Dermatologist at Orange Dermatology for reviewing the article.
References
- Ngan V. Sebaceous naevus. Hamilton: DermNet NZ, 2014. Available at www.dermnetnz.org/lesions/sebaceous-naevus.html [Accessed 21 March 2016].
- Wright TS. Nevus sebaceous and nevus sebaceous syndrome. Massachusetts: UpToDate, 2015. Available at www.uptodate.com/contents/nevus-sebaceous-and-nevus-sebaceous-syndrome?source=search_result&search=sebaceou+nevus&selectedTitle=1%7E147 [Accessed 21 March 2016]
- Amin K, Orkar S. Basal cell carcinoma arising in a sebaceous naevus. J Surg Case Rep 2015;2015(4):1–3.
- Dunkin CS, Abouzeid M, Sarangapani K. Malignant transformation in congenital sebaceous naevi in childhood. J R Coll Surg Edinb 2001;46(5):303–06.
- Rosen H, Schmidt B, Lam HP, Meara JG, Labow BI. Management of nevus sebaceous and the risk of basal cell carcinoma: An 18-year review. Pediatr Dermatol 2009;26(6):676–81.
- Santibanez-Gallerani A, Marshall D, Duarte AM, Melnick SJ, Thaller S. Should nevus sebaceous of Jadassohn in children be excied? A study of 757 cases, and literature review. J Craniofac Surg 2003;14(5):658–60.
- Idriss MH, Elston DM. Secondary neoplasms associated with nevus sebaceous of Jadassohn: A study of 707 cases. J Am Acad Dermatol 2014;70(2):332–37.
- Oakley A. Naevus anaemicus. Hamilton: DermNet NZ, 2016. Available at www.dermnetnz.org/vascular/naevus-anaemicus.html [Accessed 9 March 2016].
- Pielop JA. Vascular lesions in the newborn. Massachusetts: UpToDate, 2016. Available at www.uptodate.com/contents/vascular-lesions-in-the-newborn?source=search_result&search=vascular+lesions+in+the+newborn&selectedTitle=1%7E150 [Accessed 9 March 2016].
- Hernandez-Martin A, Garcia-Martinez FJ, Duat A, Lopez-Martin I, Noguera-Morel L, Torrelo A. Nevus anemicus: A distinctive cutaneous finding in neurofibromatosis type 1. Pediatr Dermatol 2015;32(3):342–47.
- Ferrari F, Masurel A, Olivier-Faivre L, Vabres P. Juvenile xanthogranuloma and nevus anemicus in the diagnosis of neurofibromatosis type 1. JAMA Dermatol 2014;150(1):42–46.
- Korf BR. Neurofibromatosis type 1 (NF1): Pathogenesis, clinical features, and diagnosis. Massachusetts: UpToDate, 2015. Available at www.uptodate.com/contents/neurofibromatosis-type-1-nf1-pathogenesis-clinical-features-and-diagnosis?source=search_result&search=NF1&selectedTitle=1%7E77 [Accessed 9 March 2016].
|