Overall in general practice presentations, acute and overuse mid-foot conditions may not be encountered frequently. Unfamiliarity arising from infrequent presentations adds to management difficulties in the primary care setting. However, there is a clustering of diagnoses occurring in the mid-foot region, including navicular bone stress, Lisfranc ligament disruption and tibialis posterior dysfunction, that require sound management. Delay in diagnosis has a potentially adverse impact on outcome.1 The aim of this article is to provide some guidance in recognising and managing red flag conditions in this region. Recent trends in imaging and medical management will be outlined.2
Anatomy
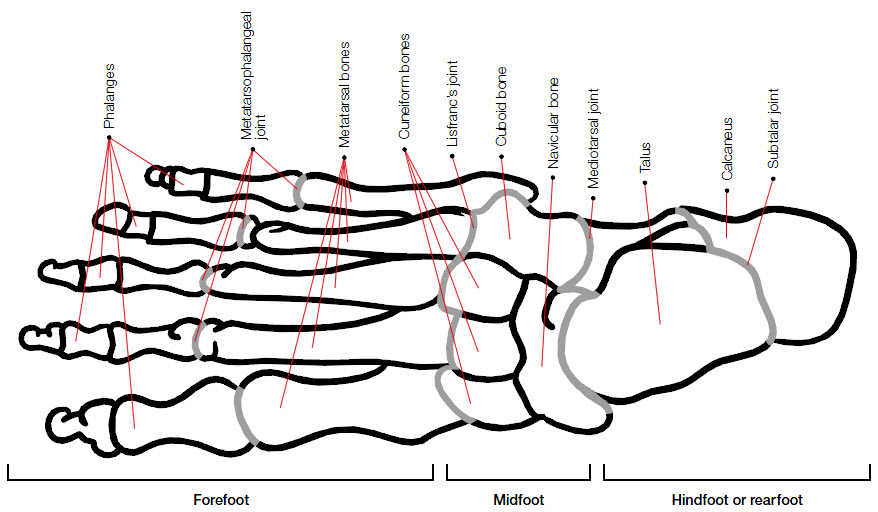 |
| Figure 1. Bony anatomy of the foot – relationship of mid-foot bones to metatarsals and proximal tarsal bones |
Anatomically, the mid-foot is the region distal to the talus and calcaneus, and proximal to metatarsal bases (Figure 1).1 However, from a differential diagnosis assessment perspective, it is necessary to consider conditions of significance occurring at the margins of the more strictly applied anatomical boundaries. The main players include the navicular bone and the three cuneiform bones medially and the cuboid laterally, the proximal tarsal and the distal tarso-metatarsal joints, the ligaments, including the central (anterior cruciate ligament equivalent) first tarso-metatarsal ligament3 and medial spring ligament, tibialis anterior and posterior and peroneal tendons. Structures immediately adjacent include the bases of the metatarsals. Joint, bone and tendon insertion pathology, especially in the immature skeleton apophyses in these tissues, need to be included in the diagnostic mix of pain in the mid-foot region.
Together, these anatomical structures contribute to the integrity of the longitudinal and transverse arches of the foot, which are critical for shock absorption at foot strike (foot landing in supination), energy store in stance and propulsion at heel lift-off. Complex rotations and flexion-extensions fulfil these roles.
Clinical assessment
As in all areas of general practice, the approach to clinical assessment involves review in terms of what is likely in this person, at this age, in this region, doing this activity, and what must not be missed (red flags).
History in acute injury requires clarifying precise details of mechanism and subsequent functional deficit in terms of the ability to weight-bear, and swelling and bruising. In gradual-onset conditions, activity and loadings, progression and current functional limitations, and previous treatment are important.
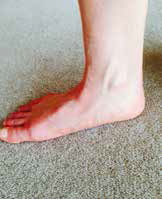
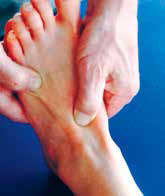
Examination involves review of foot type biomechanically by observing foot posture on standing. The range of mid-foot mobility provides a feel for stiffness or hypermobility. From a patho-anatomical diagnostic basis, careful systematic palpation, clarifying the site of tenderness is key to assessment of the likely pain generator. For traumatic presentations and severe swelling, it is important to assess neurovascular structures and the possibility of compartment syndrome.1 The key features to examine include mid-foot posture for pronation (Figure 2), mid-foot motion and stability (Figures 3, 4) and palpation of the navicular (Figure 5).
 |
 |
 |
 |
| Figure 2. Mid-foot posture pronation |
Figure 3. Assessment of mid-foot motion – stabilising rear – foot and rotating forefoot |
Figure 4. Assessment of mid-foot mobility, standing and walking posture, and ability to and quality of hop |
Figure 5. Palpation of ‘N’ spot for navicular |
Imaging modalities
As a general rule, the clustering of small bones in this area can make the interpretation of plain X-ray more challenging; when considering conditions being screened for with imaging, there is a lower threshold for using further imaging modalities in mid-foot assessment.
Plain X-ray needs to be included in all trauma and overuse presentations.2 Ultrasonography in the absence of plain X-ray often misses important diagnostic clues. The traditional path of further imaging has been bone scans as a screen for bone stress and degeneration within mid-foot joints, further clarified in presence of increased isotope uptake with computed tomography (CT) scan.2 However, magnetic resonance imaging (MRI), if available, is the preferred modality, possibly supported by CT scans to further investigate bone pathology.2
Important conditions to consider
A number of important conditions in the mid-foot are due to chronic overuse rather than acute injury. These are detailed by age and location in Table 1.
Table 1. Chronic overuse conditions by age and region
|
|
Age
|
Medial
|
Central
|
Lateral
|
|---|
|
Younger child
|
|
|
- Traction apophysitis at base of fifth metatarsal
|
|
Young adult
|
- Accessory navicular
- Peroneus longus enthesopathy
|
- Navicular stress fracture
- Stress fracture at base of second metatarsal*
|
- Stress fracture at base of fifth metatarsal*
Accessory cuboid
|
|
Older adult
|
- Insertional osis – tibialis posterior and anterior
- Peroneus longus
|
|
|
|
*Bones adjacent to mid-foot to be considered in diagnostic assessment
|
Childhood
Medial
Accessory navicular
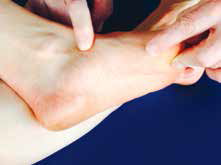 |
| Figure 6. Medial tubercle of navicular |
As an anatomical variant, the medial process of the navicular can develop as a separate ossification centre (Figure 6). The medial fragment is attached to the remainder of the navicular by a fibrous union forming a synostosis that becomes increasingly stronger with skeletal maturity. In active young children this immature anatomy potentially leads to a locally tender prominence of the medial navicular tubercle from traction at insertion of the tibialis posterior.
Management of 'accessory navicular' includes an explanation that it usually improves over weeks to months, similarly to Osgood Schlatter Syndrome. Activity loads need be adjusted according to pain level (offloading cross training). Simple analgesics and regular ice are required. Podiatry review may be useful in optimising mid-foot support. Further offloading with fracture boots, such as Cam walkers, or crutches is rarely required.
Central
Kohler’s osteochondrosis
This is an uncommon condition presenting in early childhood (4–9 years) as medial dorsal mid-foot pain, possible limp and local tenderness. The natural history is full improvement over months with attempted activity modification in interim.
Lateral
Traction apophysitis at the base of the 5th metatarsal
Pain in the lateral mid-foot, and swelling and tenderness at base of the 5th metatarsal can be quite troublesome in active children (10–13 years) and overload the maturing apophysis at this site. Improvement generally occurs with modified loads and only occasionally is there a need for more restrictive offloading using a Cam walker.
Young adult
Medial
Accessory navicular
Older patients (14–24 years) may present with localised pain, medial navicular prominence or tenderness medially. Diagnosis can be confirmed on plain X-ray or with MRI if uncertainty persists. Although the underlying anatomy will have been present long term, there must have been occasional instances of overload, placing stress on the synostosis between the two navicular fragments and causing pain. Management is to offload in the short term, support the medial mid-foot (podiatry input) and use analgesics and anti-inflammatory medication. Occasionally, corticosteroid injection into the synostosis under ultrasonography guidance may be required. Surgical excision of the accessory ossicle is rarely warranted.
Central
Navicular bone stress
A case illustrating management is presented at the end of this article.
Bone stress to the cuboid and to each of the three cuneiform bones is uncommon. These structures present with local pain and tenderness, and MRI can be useful in diagnosis. Management requires off-loading with crutches and possibly Cam Walker.
Bone stress at the base of the second metatarsal
A classical ballet dancer may develop bone stress at the base of the second metatarsal. This is an uncommon injury that is associated with ‘dance en pointe’ and presents with mid-foot pain and tenderness. It is another red flag in general practice presentations. MRI is required for diagnosis and to exclude the possibility of tarso-metatarsal synovitis occurring at this site. Referral is appropriate.
Lateral
Accessory cuboid-os peroneum
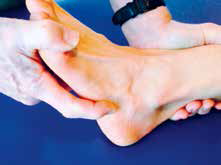 |
| Figure 7. Site of the cuboid/peroneus longus tendon immediately proximal to base of fifth metatarsal |
The peroneus longus and brevis tendons pass posterior to the lateral ankle and along the lateral rear foot. The peroneus brevis inserts into the base of the fifth metatarsal and the peroneus longus courses into the plantar mid-foot, wrapping around the lateral cuboid (Figure 7). At this point there may be an ossicle within the tendon. Friction and traction can lead to pain and local tenderness.
The ossicle will be readily apparent on plain X-ray. Management includes modified loading, anti-inflammatory measures, podiatry review and, in more refractory cases, referral for consideration of corticosteroid injection.
Bone stress at the base of the fifth metatarsal
Bone stress in the metaphyseal–diaphyseal junction at the base of fifth metatarsal is an important differential diagnosis in lateral mid-foot pain in young running athletes, although metaphyseal–diaphyseal junction is not anatomically part of the mid-foot. It is a stress fracture that can readily become a completed fracture or can go on to delayed/non-union2 and recurrence. It is often apparent on plain X-ray, which should be primary imaging.2 It requires orthopaedic referral for management (surgical versus conservative care) advice as it can, like the navicular bone, have an uncertain outcome.2
Older adults
Tendon pathology
Tibialis posterior insertional tendon pathology (enthesopathy) is not an uncommon foot presentation in general practice and can be a major source of pain and disability in the older adults (mid 40s and older).
Tibialis anterior
This is a common site of low shin soreness and crepitus in a regular walker. As the muscle becomes tendon in the anterior lower leg, the tendon courses anterior to the ankle to insert into the more medial mid-foot rather than the more intuitive dorsal mid-foot.
Tibialis anterior enthesopathy presents as pain, local swelling and tenderness in the dorsal and medial mid-foot. Tendon rupture tends to occur more at the level of the ankle synovial sheath and extensor retinaculum, but soreness in this medial mid-foot insertion can be persistent and frustrating. Appropriate management include modified loading with alternate aerobic activity, anti-inflammatory measures, podiatry review and referral for more persistent cases. Footwear can often have a significant impact on the progression of tibialis anterior enthesopathy, and friction and compression from shoes can exacerbate any symptoms. The removal of these forms of stress, as well as isometric exercises, can quickly improve pain.
Tibialis posterior
The tibialis posterior tendon passes postero-medial to the ankle to its insertion on the medial tubercle of the navicular and is a critical contributor to the integrity of the medial foot and longitudinal arch. Overload of this complex leads to mid-stance excess pronation of the medial ankle and mid-foot, and to a self-perpetuating tissue failure and medial ankle and mid-foot collapse (tibialis posterior dysfunction). For both tendons, ultrasonography is used for diagnosis, although standing, weight-bearing X-ray is indicated to assess the degree of talar subluxation.
Tibialis posterior tenosynovitis can cause postero-medial ankle pain and swelling, but tibialis posterior enthesopathy presents in patients with more severe pronation with medial mid-foot pain and swelling in the region of the medial navicular. A clue to rupture of the tendon is failure of the rear foot, viewed from behind, to invert in comparison with other side. This condition can cause severe morbidity in the elderly and requires sound care.
Anti-inflammatory agents are important, but a more formal podiatry review of mid-foot posture and mobility, and footwear is critical to arrest the medial mid-foot collapse that otherwise will perseverate the process. Often the biomechanics of the foot are influenced by other variables such as ankle joint dorsiflexion range of motion. Improvement of this, as well as controlling how the foot is moving with the use of an orthoses, can be effective in treating pain. Reconstructive surgery, may be required for refractory pain and collapse. Although such surgery is a major procedure, it can be life-changing by restoring function and independence, and alleviating pain.
Central foot
Synovitis/steoarthritis mid-foot
Progressive degeneration from early symptomatic chondrosis and synovitis to established osteoarthritis can occur at talo-navicula joint and tarso-metatarsal joints, especially the first, and presents with local pain and tenderness, bony osteophyte prominence and irritable loss of mid-foot motion on clinical testing compared to opposite foot.
Plain X-ray may be diagnostic, although CT scans or MRI may be required.
Podiatry review of foot mechanics and footwear are critical to support the mid-foot and maximise weight-loading through the foot away from irritable joints. More protracted extreme disability may require surgery.
Trauma
Fractures
Fractures in the mid-foot are uncommon and are usually caused by high-velocity motor vehicle or crush injuries. Inability to weight-bear, marked swelling and bruising warrant assessment with X-ray, CT scans and orthopaedic review.
Fracture sprains1
Ankle and foot sprains are common presentations in general practice but often there is uncertainty as to the degree and duration of offloading support required.
Higher-grade ankle and mid-foot sprains can be associated with bony avulsion flake fractures at the site of ligament attachment. Examples include flake fractures of the cuboid at the calcaneo-cuboid ligament, avulsion of the calcaneus anterior process at the calcaneo-navicular ligament, forced plantar flexion incident at the dorsal talo-navicular ligament (dorsum of talus head) and avulsion at the base of the fifth metatarsal, which can occur by clipping a heel on step or stepping from the gutter. The clue is pain more distal to the ankle, where the patient points to their most painful site, and exquisite focal tenderness at this point. The fractures are visible on plain X-ray. As for a ligament injury, these fractures can be treated in a supportive manner with weight-bearing between crutches or using a Cam walker, guided by pain and adopting RICE
(rest, ice, compression, elevation) modalities, physiotherapy care and graded activity progress guided by comfort and confidence and tape support. While more aggressive off-loading1 with plaster or Cam-walker immobilisation is more intuitive, this may produce morbidity and hence physiotherapy review to supervise strengthening and load resumption and manual therapy is critical to prevent joint stiffness, osteopenia and weakness.
Ligament strains
Lisfranc ligament disruption3
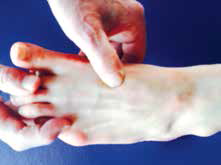 |
| Figure 8. Site of the Lisfranc ligament – base of the first and second metatarsals |
This condition is a red flag presentation in general practice. The Lisfranc ligament complex stabilises the medial cuneiform-second metatarsal joint and so stabilises the peak of the longitudinal and transverse arches of the mid-foot. It is integral to mid-foot structure and function. Surface anatomy is illustrated in Figure 8.
Rupture of the ligament leads to separation of the first and second metatarsals, leading to instability, and is the basis for imaging diagnostic abnormalities. Injury follows a high-grade strain event such as hyperextension of the mid-foot when a footballer is run down from behind and the forefoot is dragged into hyperflexion, or walking by down stairs, clipping the toe and collapsing over the forefoot, leading to marked acute or ongoing disability and local tenderness in region of the base of the second metatarsal.
These injuries can be diagnosed by imaging with plain X-ray, including comparison of weight-bearing views looking for flake fractures and any obvious widening of the gap between the medial cuneiform and second metatarsals. If plain film does not give a clear diagnosis, further imaging may be required (eg CT scans for separation and avulsion, or MRI for ligament disruption).3
Management includes the use of crutches or a Cam walker to reduce loading, pending review by an orthopaedic foot and ankle surgeon3 for decision on the treatment required (surgical or non-surgical), subject to the degree of instability shown on imaging.
Case
Navicular bone stress
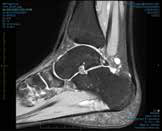
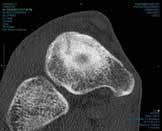
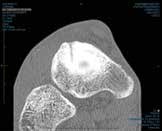
An Australian Rules footballer, aged 23 years, with a past history of navicular stress fracture, which was managed with screw fixation, presented with increasing dorsal mid-foot soreness in the other foot. At examination, there was pain with hopping, pointing to the dorsal mid-foot – the ‘N’ spot –and the site of bone stress.2 MRI confirmed navicular bone oedema (Figure 9) and a CT scan showed a fracture line in the mid-dorsal navicular in the sagittal plane (Figure 10).
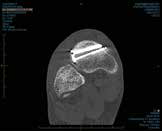
The fracture was managed non-surgically with a 6-week period of non-weight-bearing using a Cam walker, followed by weeks of partial and 2 weeks of full weight-bearing. Subsequent surveillance imaging by CT showed fracture healing (Figure 11). A program of graded walking, running and skill progression preceded a return to full training 15 weeks after the injury. However dorsal rear foot pain recurred within 2 months of return to play and imaging showed recurrence of the stress fracture, which was treated with percutaneous screw fixation (Figure 12).
Subsequently, a delayed and full return to competition was achieved.
This case highlights the difficulties and controversies in managing injuries to this bone,2 and the importance of suspicion in active young adults with local ‘N spot tenderness’ as a red flag, organising adequate imaging and obtaining guidance from an orthopaedic foot and ankle surgeon to plan management.
 |
 |
 |
 |
| Figure 9. MRI sagittal scan showing Figure 12. Post-operative CT scan the high signal in navicular |
Figure 10. CT scan showing the dorsal mid-navicular fracture line |
Figure 11. CT scan 2 months after return to play |
Figure 12. Post-operative CT scan |
Summary
With the exception of tibialis posterior dysfunction in the elderly, mid-foot pain may not be a common presentation in general practice. It is important, therefore, to have a scheme for assessment and an awareness of the possible causes, particularly the red flags of navicular stress fracture and Lisfranc ligament disruption, as delayed care can result in poor outcomes.
Competing interests: None.
Provenance and peer review: Commissioned, externally peer reviewed.
Resources
- Kitaoka HB, Lundberg A, Luo ZP, An KN. Kinematics of the normal arch of the foot and ankle under physiologic loading. Foot Ankle Int 1995:16:492–99.
- Haytmanek CT Jr, Clanton TO. Ligamentous Lisfranc Injuries in the Athlete. Oper Tech Sports Med 2014;22:313–20.
- Gross CE, Nunley JA. Medial-sided stress fractures: medial malleolus and navicular stress fractures. Oper Tech Sports Med 2014;22:296–304.