Management of ingrown toenail
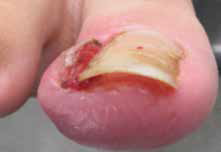 |
Figure 1. Typical ingrown toenail presentation
The dashed line indicates the section of the nail plate to be removed for conservative treatment |
Often the medial or lateral nail edge of an incurved toenail may press into the nail sulcus without actual skin penetration, which leads to the formation of a painful hyperkeratotic lesion. Should the nail plate penetrate through the thin skin of the nail sulcus, infection and hypergranulation tissue will ensue and the toenail is then best described as ingrown (Figure 1).8 Either condition may become symptomatic and require definitive surgical management. The authors suggest that, ideally, all presentations of ingrown toenail should be managed conservatively in the first instance.
Conservative treatment
Careful trimming of the affected distal nail corner is the preferred conservative management of an incurved toenail followed by application of a suitable antiseptic dressing. Referral to a podiatrist to carefully trim the nail edge and debride any hyperkeratotic lesion may be necessary. Traditional conservative treatments have included the use of astringent soaks such as hypertonic solution of Epsom salts or the application of 25% silver nitrate solution may be beneficial but are rarely used today. Encouraging patients to carefully trim their toenails to avoid creating sharp spicules and to place small inserts of cotton wool beneath the nail corners to protect the skin of the nail fold may also be helpful.9
Patients presenting with an ingrown toenail that has penetrated the nail sulcus usually require a partial avulsion of the offending border of toenail to allow for drainage and the excision of any hypergranulation tissue.10 Local anaesthesia should first be attained via a digital ring block injection of the hallux proximal to the area of erythema with plain local anaesthetic solution. Using small sterile nail nippers, the distal corner section of the involved nail edge is removed taking care not to leave any sharp projections. Care must be exercised not to extend the nail excision more proximal than necessary to avoid the nail matrix area. Hypergranulation tissue should be excised if present. Application of a haemostatic dressing such as Gelatamp may also be necessary. Oral antibiotics are sometimes required but are usually not necessary, providing the offending nail section and any hypergranulation tissue are removed. Home care then consists of soaking twice daily in Epsom salt or saline solution and using a topical antiseptic dressing until healed.
Surgical procedure – Winograd technique
If conservative care proves unsatisfactory or if the patient presents with a recurrent ingrown toenail then surgical treatment is indicated. Sharp nail resection and phenol-ablation techniques have been reported in the literature as safe and effective methods for treating ingrown toenails.11–14 The Winograd technique is perhaps the most commonly performed sharp procedure11 and is often used when a hypertrophied nailfold is in need of excision. Winograd, a US podiatrist first described the technique in 1929.15 A large case series analysis published by Güler et al11 in 2014, which followed 239 patients who underwent a Winograd procedure for ingrown toenails, reported that 96.3% (n = 230) were satisfied with the procedure and 231 patients (96.6%) were satisfied with the cosmetic result.11 Another recent analysis performed by Kayalar et al12 of 224 patients who underwent the Winograd procedure found a high success rate of 91.2% (n = 202), with revisional surgery only required in 7.1%
(n = 16) at a minimum 10-month follow-up.12
The local anaesthetic preferred for the procedure is either bupivacaine 0.5% or ropivacaine 0.75% plain. Instruments and materials required are:
- nonstick antiseptic gauze (eg Bactigras paraffin-wax gauze)
- 4.0 non-absorbable suture
- suture forceps
- scalpel handle
- English anvil nail splitter
- small curette
- straight haemostat
- #15 blade
- sterile saline
- digit tourniquet (eg Tourni-cot ring)
- The procedure is illustrated in Figure 2 and outlined below:
- Prepare the toe using alcohol skin wipes and inject 3–4 ml of bupivcaine 0.5% or ropivacaine 0.75% plain as digital ring block.
- Use standard sterile technique after applying a suitable alcoholic chlorhexidine or povidone-iodine liquid solution to prepare the foot.
- Use a digit tourniquet to exsanguinate the toe.
- Use the nail splitter to split 2–3 mm of the affected side of the nail longitudinally (Figure 2A)
- Make two skin incisions:
- The first is made deeply through the split nail to include the nail bed extending proximally to include the dorsal skin over the nail matrix (Figure 2B)
- The final incision is to excise the lateral nailfold, connecting the proximal and distal ends of the initial incision (Figure 2C, D).
- Excise the nail section, bed and matrix tissue in total (Figure 2E) and the gently curette to remove any remaining matrix tissue (Figure 2F).
- Flush with normal saline.
- Close the wound with simple interrupted sutures (Figure 2F, H).
- Remove the tourniquet and allow the toe to bleed for a minute or two with local pressure to control the reactive hyperaemia often encountered after release of the tourniquet.
- Dress the toe with a suitable antiseptic dressing, sterile gauze and crepe bandage.
The patient should be advised of the following the post-operative protocol:
- Rest and elevate the foot.
- Use oral analgesics as needed.
- Keep the dressing dry until post-operative review.
- Advise of increasing pain/discomfort (infection).
- The suture will be removed in 5–7 days.
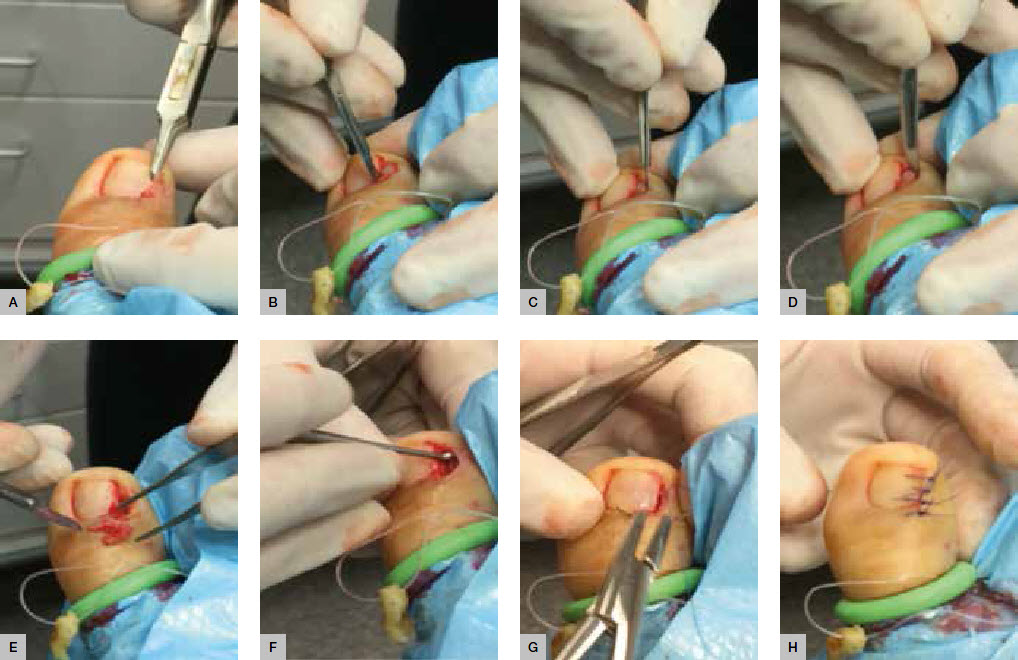 |
| Figure 2. Sequential illustration of Winograd technique |
Surgical procedure – phenol matrixectomy
Phenol matrixectomy is an alternative procedure often favoured by podiatrists and was first described by Boll, a US podiatrist, in 194516 and popularised by Bell, a UK podiatrist, in 1977.17 The procedure differs from the Winograd technique in that the nail matrix is destroyed via chemical ablation rather than being surgically excised. Phenol BP is caustic to tissues and, although the optimum application time has not been accurately determined, a histological study on fresh cadaveric specimens suggested at least 60 seconds is necessary for the phenol to penetrate matrix tissue.18 Phenol matrixectomy has been reported to offer certain advantages over the more traditional surgical approach, including lower levels of post-operative pain and infection, and has comparable success rates.19 A recently published randomised controlled trial of 123 patients with ingrown toenails concluded that the phenolic ablation technique produced less recurrence and spicule formation than the sharps nail resection (n =117 at 12 months follow-up) and no significant difference in post-operative infection rates.13 Another large retrospective case study of 197 phenolic ablations performed reported a 98.5% (n = 194) success rate at mean follow-up of 36 months with no severe complications observed.14
The local anaesthetic preferred for this procedure is lignocaine 1–2% plain. Instruments and materials required are the same as those listed above for the Winograd technique plus:
- Betadine ointment
- Beaver handle with #62 Beaver blade
- sterile cotton-tipped applicators
- liquefied phenol BP.
No sutures are needed. The procedure is illustrated in Figure 3 and outlined below:
- Prepare the toe using alcohol skin wipes and inject 3–4 ml of lignocaine 1–2% plain as digital ring block.
- Use standard sterile technique after preparing the foot.
- Use a digit tourniquet to exsanguinate the toe.
- Use a nail splitter to split 2–3 mm of the affected side of nail longitudinally (Figure 3A) and complete to the proximal edge with the #62 Beaver blade (Figure 3B).
- Perform avulsion of the nail by grasping the sectioned nail with a haemostat and using a gentle distraction technique to rotate it towards the midline of the nail plate and ease the nail free of the nail bed (Figure 3C, D).
- Gently curette the surgical site to remove any remaining matrix tissue.
- Apply liquid phenol BP directly to the site of the germinal nail matrix using small cotton wool applicator tips or the corner of gauze soaked phenol in 3 x 20-second applications (Figure 3E). Application of phenol should be carefully confined to the immediate surgical area, avoiding excess phenol contact with surrounding skin as this may result in unnecessary tissue injury. It is important to ensure that the nail sulcus and matrix area are dried immediately before applying phenol as the chemical is quickly neutralised by body fluid.
- Flush the site using chlorhexidine solution (Figure 3F).
- Remove the tourniquet and use local pressure to control any bleeding, which is normally minimal if any.
- Dress the toe with Betadine ointment, sterile gauze and crepe bandage.
Advise the patient of the following post-operative protocol:
- Postoperative analgesics are rarely required.
- Keep the toe dry overnight.
- Clean the site daily after showering using Epsom salts dissolved in water and to re-dress with Betadine ointment and a simple toe dressing until fully healed (2–3 weeks).
- Monitor for signs of increasing pain/discomfort (infection).
- The wound will be reviewed at 1 week post-operative to evaluate healing, at which time the wound should be debrided of any material inhibiting free drainage of the healing tissue.
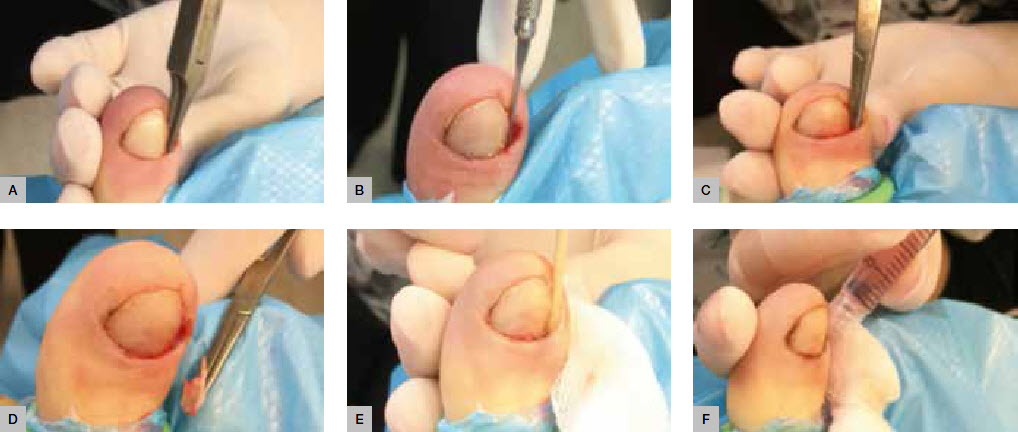 |
| Figure 3. Sequential illustration of phenol-ablation technique |
Conclusion
An ingrown toenail is a painful condition routinely managed by podiatrists and general medical practitioners alike. The surgical techniques available include the Winograd and phenol-ablation procedures. The choice of technique is largely dependent on practitioner experience and preference.
Competing interests: None.
Provenance and peer review: Commissioned, externally peer reviewed.