Severe obesity (BMI >35 kg/m2, WHO Class II and III) with comorbid T2DM is associated with a compounding array of stressors including additional obesity-related comorbidity, lower socioeconomic status, education and employment opportunities, higher levels of unemployment, dependence on disability pensions and depression.5 These issues are exacerbated with increasing levels of BMI and are greatest in those with a BMI >45 kg/m2. The term ‘severe complex obesity’ is now often used to indicate the plethora of issues encountered in these higher BMI groups.6 In general practice, this will require a chronic disease management approach as obesity, T2DM and other obesity-related conditions are treatable but not curable.
There is consistent evidence that health service providers, including general practitioners (GPs), have pejorative attitudes, beliefs and behaviours towards patients who are severely obese.7 Indeed, a large US survey found medical practitioners were one of the primary sources of weight bias reported by obese people.8 Obesity bias is systemic in Western communities from an early age, affects all areas of society and is most readily seen influencing employment, education and healthcare.9 There is some evidence that this weight bias in healthcare settings acts as a barrier to engagement with health practitioners for people who are overweight or obese.10,11 In those with comorbid obesity and T2DM, this weight-based bias may be confounded by a diabetes-related stigma,12 making positive and sustained healthcare engagement even more difficult.
The Diabetes MILES (Management and Impact for Long-term Empowerment and Success) – Australia survey dataset offers an opportunity to explore whether people with T2DM and severe obesity report less access to, and lower quality of, diabetes care than those who are not severely obese.
Methods
A brief summary of the study design and methods is provided here, as detailed description is published elsewhere.13 Diabetes MILES – Australia received ethical approval from the Deakin University Human Research Ethics Committee (reference number 2011-046).
The survey focused on the topics of emotional wellbeing, self-management, healthcare and support in relation to diabetes using a series of validated questionnaires and study-specific items. The survey was available in hard copy and online. Hard copy survey booklets were posted to 15,000 randomly selected National Diabetes Services Scheme (NDSS) registrants with type 1 or 2 diabetes, aged 18–70 years. The online survey was advertised nationally.
Participants
In total, 3338 eligible respondents took part in the survey, using hardcopy or online formats; 59% of the sample had T2DM (49% women; age 59 ± 9 years, 37% insulin-treated). The rest had type 1 diabetes. This paper focuses on the subset of participants with T2DM and comorbid severe obesity, defined as a BMI of ≥35 kg/m2 (n = 530, or 30% of the T2DM cohort). For this case-controlled analysis, each severely obese participant was matched to one control participant with T2DM and BMI <35 kg/m2 on the basis of age, gender, duration of diabetes and use of insulin (Table 1). A total of 1795 participants with T2DM had valid data for age, gender, height, weight (for calculation of BMI) and diabetes duration. Each control participant was used once only. This matching allowed for confounding differences between the groups to be minimised.
Table 1. Characteristics of survey respondents* by WHO BMI category^
|
BMI category (kg/m2)
|
|
|
Total
|
<25
|
25–29.99
|
30–34.99
|
35–39.99
|
≥40
|
|
Total respondents (n)
|
1795
|
220
|
520
|
525
|
288
|
242
|
|
Percentage of total (%)
|
100
|
12.2
|
28.9
|
29.2
|
16.0
|
13.5
|
|
Males (%)
|
51.6
|
55.5
|
62.3
|
52.8
|
45.8
|
29.3
|
|
Age (mean ± SD)
|
58.4 ± 8.9
|
58.7 ± 8.7
|
60.2 ± 7.6
|
58.6 ± 8.4
|
56.7 ± 9.7
|
56.0 ± 8.7
|
|
Diabetes duration (years) (median ± IQR)
|
8 (3–12)
|
6 (3–11)
|
8 (3–12)
|
9 (4–13)
|
8.5 (4–12)
|
8 (4–13)
|
|
Age at T2DM onset (years) (mean ± SD)
|
49.4 ± 9.7
|
50.8 ± 9.5
|
51.4 ± 9.2
|
49.2 ± 9.6
|
47.4 ± 9.7
|
46.6 ± 9.8
|
|
Treatment:
oral diabetes agents (%)
insulin (%)
|
73.9
36.7
|
60.5
21.4
|
71.9
30.6
|
74.7
40.4
|
78.8
45.1
|
82.6
45.9
|
|
*Participants with T2DM who provided data regarding gender, age, height and weight (n = 1795)
^World Health Organization classifications
|
Data extracted for this analysis
Socio-demographic characteristics were extracted from the database, including marital-relationship status, living situation, education, household income and employment, as previously described.5 Experiences with, and support provided by, the respondents’ diabetes healthcare team were measured using the Resources and Support for diabetes Self-Management (RSSM) questionnaire.13,14 Participants were asked about which healthcare professionals they had accessed in the past 12 months and their access to healthcare services generally, and to rate the quality of their consultations with the healthcare professional whom they relied on most for their diabetes care (using items adapted from the Australian Longitudinal Study of Women’s Health Survey).15
Statistical methods
The analysis involved comparing cases with controls and an examination of increasingly severe obesity by stratifying the severely obese group into Class II (BMI 35–39.99 kg/m2), Class IIIa (BMI 40–44.99 kg/m2), and Class IIIb (BMI >45 kg/m2) to assess relative associations with increasing BMI.
Cases and controls were compared using Chi-square tests for proportions, Student’s t-tests for normally distributed outcomes (mean ± SD) or Mann-Whitney U tests otherwise (median ± IQR). Controls and those in the three levels of severe obesity were compared using one-way analysis of variance, Kruskal-Wallis tests for non-parametric continuous variables, and linear association for proportions. SPSS statistical software 19 (SPSS Inc, Chicago, Il) was used for all analyses and a two-sided P value of 0.05 was considered to be statistically significant.
Results
The characteristics of the 1795 participants who reported having T2DM and reported their height and weight (enabling BMI to be calculated) are shown in Table 1. The mean BMI for this cohort was 32.5 ± 7.9 kg/m2. Men (51.6%) were more highly represented in the overweight category but women comprised the majority in the Class II (BMI ≥35 kg/m2) and, in particular, Class III (BMI ≥40 kg/m2) categories (Table 1).
The 530 participants with a BMI ≥35 kg/m2 (cases) were successfully matched with 530 control participants (BMI <35 kg/m2), as shown in Table 2, which also details the demographic, socioeconomic, clinical characteristics and comorbidities of the cases and controls (including stratification by BMI). As described previously, increasing levels of obesity were associated with lower income, greater likelihood of financial assistance with unemployment and disability pension benefits (Table 2).5
Table 2. The demographic, socioeconomic and clinical characteristics for controls and cases stratified
by BMI subgroup
| |
Matched controls |
Cases |
Subgroups of cases |
P value between groups* |
P value linear association# |
| Class II |
Class IIIa |
Class IIIb |
| |
BMI <35 |
BMI ≥35 |
BMI 35–39.99 |
BMI 40–44.99 |
BMI ≥45 |
|
|
| Number of respondents |
530 |
530 |
288 |
133 |
109 |
|
|
| BMI (kg/m2, median) |
28.2 |
41.6 |
37.1 |
42.0 |
49.1 |
|
|
| Demographics |
| Age (years) |
56.6 ± 9.6
Median 58 |
56.4 ± 9.6
Median 58 |
56.7 ± 9.5 |
57.3 ± 9.4 |
54.4 ± 9.8 |
NA |
NA |
| Men (%) |
38.3 |
38.3 |
46 |
33.1 |
24.8 |
NA |
NA |
| Unemployed (%) |
8.6 |
9.0 |
7.6 |
4.6 |
18.4 |
0.80 |
0.002 |
| Disability pension (%) |
14.9 |
21.4 |
16.5 |
25.8 |
28.7 |
0.008 |
<0.001 |
| Private health insurance (hosp) (%) |
60.4 |
49.6 |
54.5 |
44.0 |
43.3 |
0.001 |
<0.001 |
| Household income:
|
41.0%
18.2% |
50.6%
13.2% |
44.7%
18.7% |
59.0%
11.5% |
56.3%
2.9% |
0.003
0.05 |
0.001
<0.001 |
| Diabetes characteristics |
| Duration of diabetes (years) |
8.8 ± 6.6Median 8 |
9.2 ± 7.1Median 8 |
9.2 ± 7.0 |
10 ± 7.5 |
8.4 ± 6.9 |
NA |
NA |
Primary therapy:
- insulin
- Oral hypoglycemic agents
|
45.7%
37.4% |
45.8%
42% |
45.3%
40.4% |
45.5%
47.0% |
47.7%
40.2% |
NA
0.001 |
NA
0.006 |
| Diet and exercise |
16.3% |
10.1% |
12.3% |
5.3% |
10.3% |
0.004 |
0.01 |
|
*NA, not applicable as these were the variables used to match the cases and controls. Cases and controls were matched for age, sex, duration of diabetes, and use of insulin therapy. #P-values were obtained using linear associations between values for matched controls and the three case subgroups.
|
More than 70% of participants reported that the healthcare professional they rely on most for diabetes care is their general practitioner (GP) and this did not differ between controls and cases (Figure 1). The remaining participants nominated diabetes specialists (endocrinologist), nurse educators and dieticians. Responses did not vary by BMI category. The proportion of participants accessing professional healthcare for their diabetes and the type of practitioners accessed is shown in Table 3. Ninety-three percent of the severely obese and control participants visited a GP in the past 12 months. Severely obese participants reported similar utilisation of medical specialist services and were more likely than controls to have had appointments with diabetes educators and dieticians (Table 3).
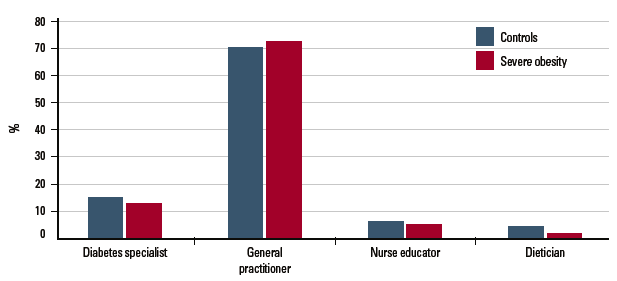
Figure 1. Which health professional do you rely on most for your diabetes care? No other professionals were nominated by more than 1% of either group. Others included other medical specialists, pharmacists, community nurses and alternative medical practitioners.
Table 3. BMI classification and the help received from healthcare professionals
|
BMI <35
|
BMI ≥35
|
BMI 35– 39.99
|
BMI 40–44.99
|
BMI ≥45
|
P value case versus control
|
P value controls and subgroups
|
| |
530 |
530 |
288 |
133 |
109 |
|
|
| |
Matched Controls |
Cases |
Subgroups of cases |
|
|
|
Class II
|
Class III a
|
Class III b
|
|
Median BMI (kg/m2)
|
28.2
|
41.6
|
37.1
|
42.0
|
49.1
|
|
|
|
Proportion accessing help in the past 12 months
|
|
Professional
|
| Diabetes specialist (eg. endocrinologist) (%) |
34.7 |
33.0 |
30.0 |
37.6 |
33.9 |
0.6 |
0.50 |
| Other medical specialist (eg. cardiologist) (%) |
13.8 |
15.3 |
15.3 |
16.5 |
13.8 |
0.5 |
0.83 |
| General practitioner (%) |
93 |
93 |
93.1 |
93.2 |
92.7 |
1.0 |
0.99 |
| Diabetes educator (%) |
42 |
50 |
50 |
56.4 |
49.5 |
0.01 |
0.08 |
| Dietician/nutritionist (%) |
29 |
36 |
32.6 |
40.6 |
39.6 |
0.018 |
0.03 |
| Resources and support for self-management14 |
| In the past 3 months how often someone on your diabetes care team (1–5: never, rarely, sometimes, usually, always): |
- ask about what’s important to you...?
|
2.6 |
2.4 |
2.4 |
2.3 |
2.3 |
|
|
- set goals to take care of your diabetes?
|
3.5 |
3.6 |
3.5 |
3.7 |
3.6 |
|
|
- teach you how to deal with problems?
|
2.7 |
2.6 |
2.6 |
2.7 |
2.3 |
|
|
- get the information you needed?
|
3.3 |
3.1 |
3.1 |
3.2 |
2.9 |
|
|
- contact you between appointments
|
1.7 |
1.6 |
1.7 |
1.6 |
1.6 |
|
|
| How many programs are in your community now? |
2.9 |
2.8 |
2.9 |
2.7 |
2.7 |
|
|
| Mean score for items (mean (SD)) |
2.8 (1.0)
|
2.7 (1.0)
|
2.7 (1.0)
|
2.8 (1.1)
|
2.6 (1.0)
|
0.29*
|
0.75*
|
| How would you rate the following (mean (SD) median); 1–5: poor, fair, good, very good, excellent): |
- access to medical specialists if you need them?
|
3.5 (1.1) 4 |
3.3 (1.1) 3 |
3.3 (1.2) 3 |
3.3 (1.2) 3 |
3.3 (1.2) 3 |
0.007 |
0.06 |
- access to hospital if you need it?
|
3.6 (1.1) 4 |
3.5 (1.2) 4 |
3.5 (1.1) 4 |
3.5 (1.2) 4 |
3.5 (1.1) 4 |
0.18 |
0.67 |
- access to after-hours medical care?
|
2.9 (1.3) 3 |
2.8 (1.2) 3 |
2.8 (1.2) 3 |
2.8 (1.3) 3 |
2.8 (1.2) 3 |
0.11 |
0.41 |
- access to GP who bulk bills?
|
3.3 (1.5) 4 |
3.3 (1.5) 4 |
3.3 (1.5) 3 |
3.3 (1.6) 4 |
3.2 (1.5) 3 |
0.87 |
0.75 |
- ease of seeing GP of choice?
|
3.6 (1.2) 4 |
3.6 (1.2) 4 |
3.6 (1.3) 4 |
3.7 (1.2) 4 |
3.6 (1.3) 4 |
0.69 |
0.82 |
- access to psychologist if you want?
|
3.0 (1.2) 3 |
3.0 (1.2) 3 |
2.9 (1.2) 3 |
3.1 (1.2) 3 |
2.9 (1.1) 3 |
0.77 |
0.66 |
- access to dieticians if you want?
|
3.3 (1.1) 3 |
3.2 (1.1) 3 |
3.3 (1.1) 3 |
3.2 (1.2) 3 |
3.1 (1.1) 3 |
0.11 |
0.38 |
Thinking about the health professional(s) you rely on most, how would you rate the following? (mean (SD) median);
1–5 (poor, fair, good, very good, excellent) |
| The amount of time they spend with you? |
3.6 (1.0) 4 |
3.5 (1.1) 4 |
3.5 (1.1) 4 |
3.5 (1.1) 3 |
3.7 (1.0) 4 |
0.97# |
0.54# |
| Their explanation of your problem and treatment? |
3.7 (1.0) 4 |
3.6 (1.1) 4 |
3.7 (1.1) 4 |
3.5 (1.2) 4 |
3.7 (1.0) 4 |
0.55# |
0.66# |
| Their interest in how you feel about the tests, treatment or advice given? |
3.6 (1.0) 4 |
3.6 (1.1) 4 |
3.6 (1.1) 4 |
3.5 (1.2) 3.5 |
3.7 (1.0) 4 |
0.88# |
0.75# |
| Your opportunity to ask all of the questions that you want? |
3.8 (1.0) 4 |
3.8 (1.1) 4 |
3.8 (1.1) 4 |
3.6 (1.1) 4 |
3.8 (1.0) 4 |
0.88# |
0.20# |
| Their technical skills, (thoroughness, carefulness, competence)? |
3.9 (1.0) 4 |
3.8 (1.1) 4 |
3.9 (1.0) 4 |
3.7 (1.1) 4 |
3.9 (1.0) 4 |
0.89# |
0.45# |
| Their personal manner (courtesy, respect, sensitivity, friendliness)? |
4.4 (1.0) 4 |
4.0 (1.0) 4 |
4.0 (1.0) 4 |
4.1 (0.9) 4 |
4.0 (1.1) 4 |
0.64# |
0.91# |
*Parametric, Independent Student t-test or one-way ANOVA Tukey post hoc analysis as appropriate
#Non-parametric, Mann-Whitney U or Kruskal-Wallis as appropriate |
In respect of rating aspects of their interactions with the healthcare professional they relied on most, there were no differences between cases and controls, or across BMI categories. The time with the practitioner, their personal manner, level of skill and interest were all comparable (Table 3).
The resources and support for self-management that participants reported receiving from their diabetes healthcare team were no different between cases and controls, or across the BMI categories (Table 3). Severely obese participants reported generally the same level of utilisation and access to health services as controls for GP services, hospital access, psychologists and dieticians, but less access to medical specialists if they were needed (Table 3).
Discussion
Findings from this analysis of the Diabetes MILES cohort indicate that severely obese and non-severely obese Australian adults with T2DM report the same levels of access to and satisfaction with diabetes-related healthcare.
An important finding of this analysis was that most patients, whether severely obese or not, tend to rely on their GP for their diabetes management over and above any other healthcare professional. Given that almost 30% of the survey participants with T2DM were also severely obese, a combination that we have previously described as having compounding socioeconomic, medical and psychosocial stressors,5,16 the GP is therefore in a pivotal position to assess these issues and provide the guidance and support needed for improved health outcomes.
It is reassuring that severely obese Australians with T2DM report similarly good access, support and satisfaction with their primary health practitioner as the control participants in this study, given the previously reported level of bias, stigmatisation and pejorative attitudes that medical practitioners can show individuals who are obese.7 It is important to consider, however, that these perceptions may not reflect actual equity of access and service. This is suggested in the small but significant difference between cases and controls in their rating of accessibility to specialist medical care if needed (Table 3). The slightly lower rating on this item by severely obese patients could have been brought about by a cost barrier, due to lower levels of private health insurance, and this would be worth exploring further. Examination of actual access of health services, for example via Medicare claims analysis, would also strengthen this analysis.
The results of the present analysis differ from our previous findings from focus groups conducted with severely obese women, which found that younger women (<35 years) were more likely than those aged >35 years to report health provider discrimination,11 and also of other researchers who have assessed physicians’ reported pejorative attitudes to managing obesity in primary care.17 Differences in research design may be the reason for the differing results and certainly highlight the need to continue to investigate the issues of healthcare providers’ attitudes to and management of obese patients.
Adults with T2DM and severe obesity report equity of access to, and satisfaction with, almost all aspects of diabetes care in Australia, compared with those in a non-severely obese range. The finding that the most of the patients listed their GP as their principal diabetes care-provider highlights the need for GPs to understand that they are integral to diabetes care and that management of severe obesity must be considered as a part of optimal diabetes care.2 In addition, adequate resources should be directed to GPs in line with their role as principal providers.
Competing interests: Jessica Browne: National Diabetes Services Scheme Strategis Development Grant - funded the Diabetes MILES Australia 2011 survey; Unrestricted educational grant from Sanofi Aventis – supported development of the Diabetes MILES website; Payment to institution by Roche Diagnostics Australia. Jane Speight: Unrestricted educational grant from Sanofi Aventis – supported development of the Diabetes MILES website; Payment to institution by Roche Diagnostics Australia and Novo Nordisk. John Dixon: Research grant Royal Australian College of General Practitioners, Payment from Nestle Australia, Metagenics Inc., Allergan Inc., and iNova Pharmaceuticals. Kay Jones: Research grant Royal Australian College of General Practitioners.
Provenance and peer review: Not commissioned, externally peer reviewed.