In marked contrast to the trajectories of non-malignant diseases, the burden of disease and the time course of disseminated cancer are relatively predictable. This makes care planning for these patients relatively straightforward. Comprehensive care is made more possible by the fact that specialist palliative care is largely built around the care of people with cancer,4 so GP-based coordinated care is possible.
Palliative Care Australia service planning documents assume a hierarchy of need5 (Figure 1). Many patients have uncomplicated problems at the end of life, well within the skill of most GPs. Some will require advice from a palliative care team only. A small proportion of patients will have such complex needs that they require the full suite of services offered by specialist teams. At all levels, specialist care should link with the patient’s GP (Figure 2). The presence of a GP actively involved in care increases the likelihood of dying at home, compared with low GP involvement.6 Low continuity of care increases the likelihood of visits to the emergency department in the last 6 months of life by 2–4 times.7
This article focuses on the process of care and presents evidence supporting GP involvement in end-of-life care. In particular, it discusses care planning, advance health directives and the care of carers. Finally, it discusses barriers to good care, and resources to assist in providing high-quality end-of-life clinical care.
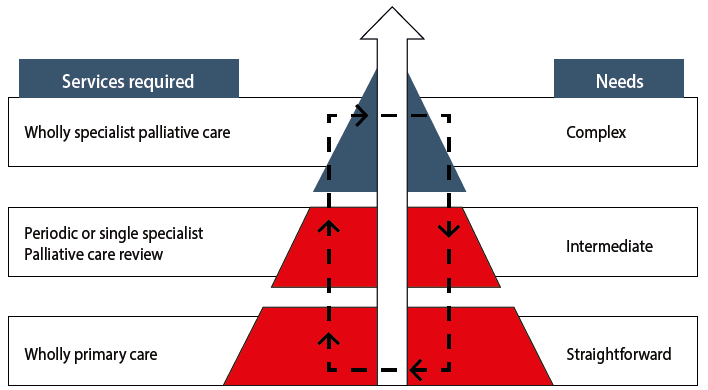
Figure 1. Needs-based palliative care model. Adapted with permission from Palliative Care Australia from A guide to palliative care service development: a population-based approach, 2005.5
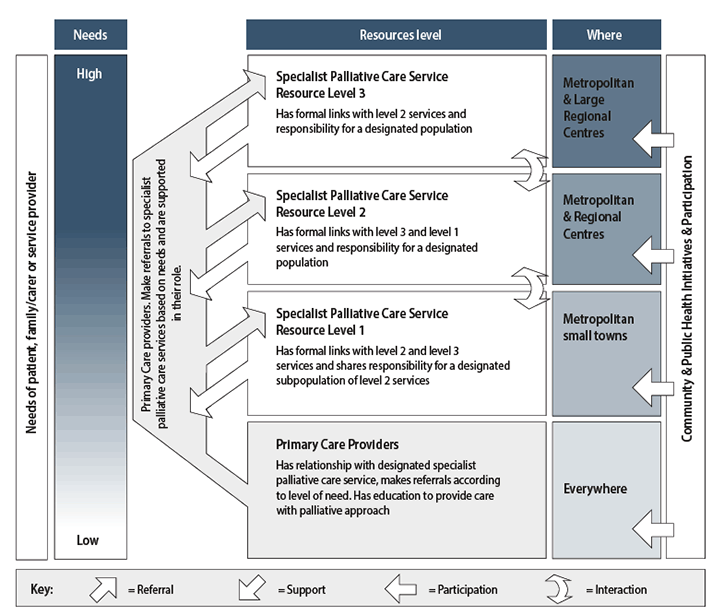
Figure 2. Framework for palliative care planning. Reproduced with permission from Palliative Care Australia from A guide to palliative care service development: a population-based approach, 2005.5
Advance care planning and clinical care planning
At the heart of good end-of-life care is advance care planning. This planning is defined as the opportunity for people to think, discuss and plan for the medical treatment they would prefer if they became too ill in the future to express their wishes.8,9 Advance care planning usually involves completing a legally binding document called an advance health directive (AHD) or living will, which seeks to capture the patient’s intentions for their future healthcare. A randomised controlled trial (RCT) of advance care planning versus normal care (in a specialist hospital)10 showed that developing an AHD leads to the patients wishes being known and followed. Furthermore, it leads to more satisfied bereaved carers, who experience less anxiety and depression.
The relationship between personal advance care planning and clinical care planning is shown in Figure 3. In addition to recording the wishes of the patient, it is also important to consider the nature and clinical course of the cancer and to do a comprehensive review of the whole person’s needs from many perspectives. This makes it possible to anticipate problems and prepare for them.11 This process can also assist people who are ill to consider their wishes across a much broader spectrum that is not limited to whether they want resuscitation or other life-sustaining processes. Each element of care planning supports the other.
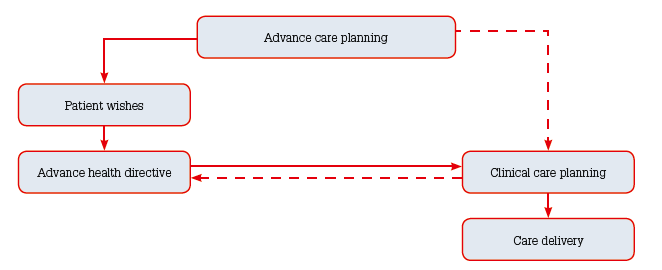
Figure 3. Conceptual map of advance care planning
Facilitating care planning within primary care is well developed in the UK and Europe.11,12 In the UK, the Gold Standards Framework program of end-of-life care11 developed by Thomas offers a conceptual framework to end-of-life care (Table 1). By considering all of the elements of the PEPSI COLA framework, a GP can be reasonably confident of anticipating and preparing for most potential problems.
Multidisciplinary teamwork
The complexity and intensity of the problems at the end of life, and the short time frames inevitably lead to a team forming around the patient. It is essential that the team has a coordinator, and this role often falls to the GP. However, this is not inevitable – it could be a palliative care or domiciliary nurse that bears this responsibility.
Involvement of a palliative care team is important and effective. Temel’s landmark study13 in a USA oncology service showed the early addition of palliative care to specialist oncology in disseminated lung cancer improved quality of life, reduced service utilisation and, most significantly, improved survival.
Further, coordination between specialist palliative care and the GP also confers patient benefit. Two RCTs of a single case conference (and subsequent care planning) between GPs and specialist palliative care teams showed improved quality of life in the last month of life,14 persistent improvements in functional ability of patients14 and a 30% reduction in hospital admissions,15 compared with normal care.
How well are we doing?
In spite of clear evidence that GP involvement in end-of-life care is beneficial to patients and carers, there is also evidence that about 25% of GPs do not accept this role and are particularly reluctant to do home visits and out-of-hours calls.16,17 Other reasons for this were having family or personal commitments, and a sense of inadequate knowledge or support. One-third of this group stated they had no interest in end-of-life care.17 More disturbingly still, the demographics of those who did not do palliative care were similar to the demographics of the emerging GP workforce17 (Table 2). This problem is compounded by an increasingly ageing population,18 where more patients will die of cancer and more palliative care will be required.
There is also a problem in recognising when patients are approaching the end of life. Doctors routinely overestimate patient prognosis19 and, as a result, are likely to undertake palliative care planning too late. Even with cancer, this leads to people being considered as approaching the end of life far later than is ideal and to late referrals to palliative care.20
The self-perceived role of GPs in advanced cancer care is also dependent on location.21 Urban GPs are not sure where they fit, particularly where some oncology services refer directly to specialist palliative care services. What is expected of them? Who brings the GP into this picture? The role is much clearer in regional and rural settings, and much more accepted: the GP may often be the only medical resource available. Involving younger GPs in end-of-life care is a very important task. The more GPs perform palliative care, the more comfortable they become with it.22 Not starting early will lead to more difficulty in engaging in end-of-life care later.
Table 1. The PEPSI COLA structure for palliative care clinical planning11
| Domain |
Issues to consider |
| Physical |
Symptom control
Medication – regular and as needed
Compliance/stopping non-essentials
Complementary therapies |
| Emotional |
Understanding expectations
Depression and adjustment
Fears/security
Relationships |
| Personal |
Spiritual/religious needs
Inner journey
Quality of life
Patient/carer agenda |
| Social Support |
Benefits/financial
Care for carers
Practical support |
| Information/ communication |
Within team
Between professionals
To and from patient
To and from carers |
| Control |
Choice, dignity
Treatment options/management plan
Advance directive
Place of death |
| Out of hours/ emergency |
Continuity
Provision of out-of-hours care to
patients/carers
Carer support
Medical support
Drugs and equipment |
| Late |
End-of-life/terminal care
Stopped non-urgent treatment
Patient and family aware
Comfort measures/spiritual care
Rattle, agitation |
| Afterwards |
Bereavement follow-up/others informed
Family support
Assessment/audit
Support team |
Solutions
Advance care planning
Scott et al23 offer suggestions for GPs to facilitate having the difficult but necessary conversations about end-of-life care. These include computer-generated prompts, mailouts to eligible patients, incorporating advance care planning discussions into regular health checks and chronic disease management plans, and training practice nurses to participate in advance care planning case management. The Personally Controlled eHealth Record24 contains provision for recording the contact details of the substitute decision maker, as well as for storage of medical documents such as the AHD. This will make the AHD available to all healthcare providers.
Support for providing patient care
Most specialist palliative care services are more than happy to support GPs caring for patients. They will usually take phone calls from GPs to discuss clinical problems. GP–specialist case conferences improve patient outcomes.14,15 While GPs can initiate a case conference, it is more likely that the initiation will come from specialists or aged care facilities. They will attract a rebate even if conducted by distance technology and this may make them more feasible. There is a wide array of online resources aimed at providing general and clinical information. Some of these are presented in Table 3.
Accessibility
A key part of providing palliative care is to be available. Issues of personal safety are legitimate and concern some doctors. However, this service does not have to be made available to all – it can be applied to well known patients only. If this is not feasible, offering patients and their carers a telephone contact number is enormously reassuring. Given the small number of palliative care patients a GP sees annually,25 the number of calls is very small and patients almost never abuse this privilege. If neither of these options is possible, it is important that patients know what the practice after hours arrangements are, and that a written health summary including an up-to-date medicines list, is at the home to assist locum services provide appropriate care. Consider informing the locum services of the patient’s palliative status – they may hold a register.
Carers
A good way of introducing GPs into palliative care is to care for the carers. Their needs are very substantial26 and often overlooked because they are not the ill person. The Needs Assessment Tool for Carers (NAT-C)27 is a self-completed checklist for carers, which allows them to identity their own major concerns and is available online (Table 3). This can guide such a consultation. NAT-C improves outcomes for carers, particularly those with anxiety or depression.
Table 2. Characteristics of GPs willing to and unwilling to treat palliative care patients17
|
Performs palliative care |
|
Yes (74.8% of total) |
No (25.2% of total) |
P value |
| Female (%) |
38.7 |
52.2 |
0.052 |
| Mean age (years) |
52.1 |
48.0 |
0.004 |
|
Years in general practice
|
22.7
|
18.2
|
0.001
|
|
>40 hours per week (%)
|
48.7
|
25.8
|
0.001
|
|
Overseas medical degree (%)
|
25.3
|
40.3
|
0.019
|
|
Employment status – employee
(vs practice owner or associate) (%)
|
13.2
|
50.8
|
0.001
|
Table 3. Useful resources for GPs when providing palliative care
| Clinical resources |
Therapeutic Guidelines: Palliative Care. 3rd edn.
www.tg.org.au |
National consensus-based palliative care guidelines
|
|
|
EviQ. Cancer Treatments online.
Cancer Institute of NSW. www.eviq.org.au/
GP pain help. (PDA device app)
Australian College of Rural and Remote Medicine
https://itunes.apple.com/au/app/gp-pain-help/id722694198?mt=8
|
Web-based resources in palliative care and primary care. Includes an opioid conversion page
Comprehensive assistance in managing severe pain. Includes an opioid conversion function
|
|
|
Flinders University. Caresearch. GP Hub.
www.caresearch.com.au/caresearch/tabid/901/Default.aspx
|
National palliative care information hub. Has a dedicated hub for GPs, with comprehensive information on clinical palliative care
|
|
Advance care planning
|
Advance Care Planning Australia
http://advancecareplanning.org.au/
|
National web page for advance care planning that provides state-by-state information on legally binding advance care documents, as well as information and a how-to process for the community
|
|
Care for carers
|
University of Queensland. Needs assessment tool – carers.
www.caresearch.com.au/caresearch/tabid/1643/Default.aspx
|
Self completed form for carers to systematically identify care needs. For use in guiding GP consultations about caring for people with advanced cancer
|
Conclusion
Quality general practice necessarily includes quality end-of-life care, regardless of the type of illness involved. Caring for cancer patients has distinct advantages over other forms of cancer in that planning is possible. Planned care improves outcomes for patients and should be the norm in modern general practice.
Competing interests: None.
Provenance and peer review: Commissioned, externally peer reviewed.