Anorexia nervosa is often associated with significant psychiatric comorbidities and medical complications.3 Common psychiatric comorbidities are anxiety disorders, obsessive-compulsive disorder, social phobia, depression and subtle cognitive changes.11 Physical complications include adaptations to starvation, such as low body temperature, hypotension and bradycardia, as well as malabsorption, reduced GI motility, diarrhoea, constipation, bone mineral loss, bone marrow suppression, arrhythmias from either electrolyte disturbance or reduced metabolic rate, and multiple skin and hair changes.12 Excessive restrained eating and low weight can result in structural changes including decreased grey matter in the brain that may not normalise with weight recovery.13,14 People who starve themselves in the context of anorexia nervosa often elicit intense negative feelings from others, which can interfere with assessment and effective care of these patients and compromise support from their carers.5–7
General practitioners (GPs) have a critical role in the early recognition and ongoing management of eating disorders.15 The GP also has the potential to reduce the incidence of problematic eating developing into an overt eating disorder as early intervention may limit the progression.16,17 This article provides GPs with some tools to assist with early detection of anorexia nervosa and management of patients and their family through this highly emotive and often daunting problem.
Considering anorexia nervosa in any person who is underweight or has rapid weight loss will assist in early detection, treatment and support of patients and families through the complex range of emotions that may emerge throughout the course of the illness.
Why focus on early detection?
Anorexia nervosa often becomes a self-maintaining disorder after 5 years and it has a cumulative deleterious effect on all areas of the patient’s life, making recovery increasingly difficult.18 Early detection can improve the outcome of treatment and thereby reduce the impact of this disorder on patients and their family.
Most patients who are in the early stages of an eating disorder will be taken, often reluctantly, to their GP by a concerned relative. The relative is often distressed and scared, while the patient will be, at best, ambivalent and withholding, making the consultation a delicate interaction for the GP. Table 1 identifies some of the signs and symptoms that may cause concern.5,16 This can be used as a guide; however, the early presentations to a GP may be for any symptom or sign.
Table 1. Common presentations of patients with or developing
anorexia nervosa
|
Changed attitude to food and cooking
Avoiding meals
Slow eating/picking at food
Eating in secret
Cooking for family not for self
Eating low calorie foods
Changing food choices (eg. vegetarian or vegan diet)
Medical problems
Weight fluctuations with possible denial of diet or deliberate weight loss
Fractures from minimal force
Menstrual irregularities
Gastrointestinal problems (eg. bloating, constipation, generalised abdominal pain, changing bowel habit)
Hypoglycaemia – may present as ‘dizzy spells’
Behavioural and psychological presentations
Raiding the fridge
Social phobia with regard to eating
Excessive work or training
Low mood or mood instability
Poor concentration
Self diagnosis
New food intolerance (eg. lactose intolerance)
Suddenly developing ‘allergies’ to foods
|
Many patients will have a clinically significant eating disorder before meeting the full DSM-V criteria for anorexia nervosa.4 Considering anorexia nervosa in the differential diagnosis of weight loss can facilitate early detection and better prognosis. In this context it is important to consider that for the patient, anorexia nervosa is arguably a life solution to an internal problem and thus they may actively resist any attempt to change their behaviours. Later, as they gain weight, the emotions that starvation served to shield them from can return and this can be a difficult time in treatment as they still lack more adaptive coping mechanisms.
Consistency in management and clear non-negotiable consequences for particular behaviours or starvation-based physical problems act over time to maintain trust. This then becomes crucial for liaison with other services.
Identify the patient
An eating disorder may present at any time during the life span. There are no major differences between treatment of children and adolescents, compared with adults, except that the family is usually more affected in the former cases and are thus more integral to effective care. Non-specialists may not recognise the disorder when it presents, as patients are secretive, and often ashamed by their own behaviour.19 Using a simple screening questionnaire (Table 2) and/or validated screening tools such as SCOFF (Table 3) can help in the recognition of eating disorders in these early consultations and allow earlier interventions.20–22
Table 2. Questions to ask a patient with a suspected eating disorder29
- Have you been deliberately trying to limit the amount of food that you eat to influence your shape or weight (whether or not you have succeeded)?
- Have you gone for long periods of time (8 waking hours or more) without eating anything at all in order to influence your shape or weight?
- Have you tried to exclude from your diet any foods that you like in order to influence your shape or weight (whether or not you have succeeded)?
- Have you tried to follow definite rules regarding your eating (for example, a calorie limit) in order to influence your shape or weight (whether or not you have succeeded)?
- Have you had a definite desire to have an empty stomach with the aim of influencing your shape or weight?
|
Table 3. SCOFF
|
S – Do you make yourself Sick because you feel uncomfortably full?
C – Do you worry you have lost Control over how much you eat?
O – Have you recently lost more than One stone (6.35 kg) in a 3-month period?
F – Do you believe yourself to be Fat when others say you are too thin?
F – Would you say Food dominates your life?
If the patients answer ‘Yes’ to 2 or more then there is a high index of suspicion that they have an eating disorder and warrant a more detailed assessment.22
SCOFF has been validated across various languages.19
|
| Reproduced with permission from the BMJ Group from Morgan JF, Reid F, Lacey JH. The SCOFF questionnaire: assessment of a new screening tool for eating disorders BMJ 1999;319:1467–68. |
The screening questions also assist in opening up an ongoing non-judgmental discussion about food and weight, which can be the beginning of establishing a therapeutic relationship. The GP can use them again at various intervals to monitor changes in either the disordered eating or compensatory behaviours. For example, at times a patient may use excessive exercise to compensate for any increase in food intake but as they become weaker they restrict more food groups.
Once there is an index of suspicion that a patient has an eating disorder, a systematic approach to the medical assessment is required to determine the severity of malnutrition, screen for other causes of weight loss, and establish who delivers treatment and the setting of care. This is crucial to ensure that there is a coordinated approach to care from the outset.
On initial assessment, a full physical examination should be conducted with feedback to the patient about the results. On subsequent visits, monitoring weight, temperature, blood pressure and heart rate are the basic requirements. Figure 1 is a summary of the core physical examination and investigations that should be performed on all patients with a suspected eating disorder. The feedback of results of various investigations and physical trends can assist the GP engage the patient in a dialogue about their illness and how the body is responding to malnutrition.
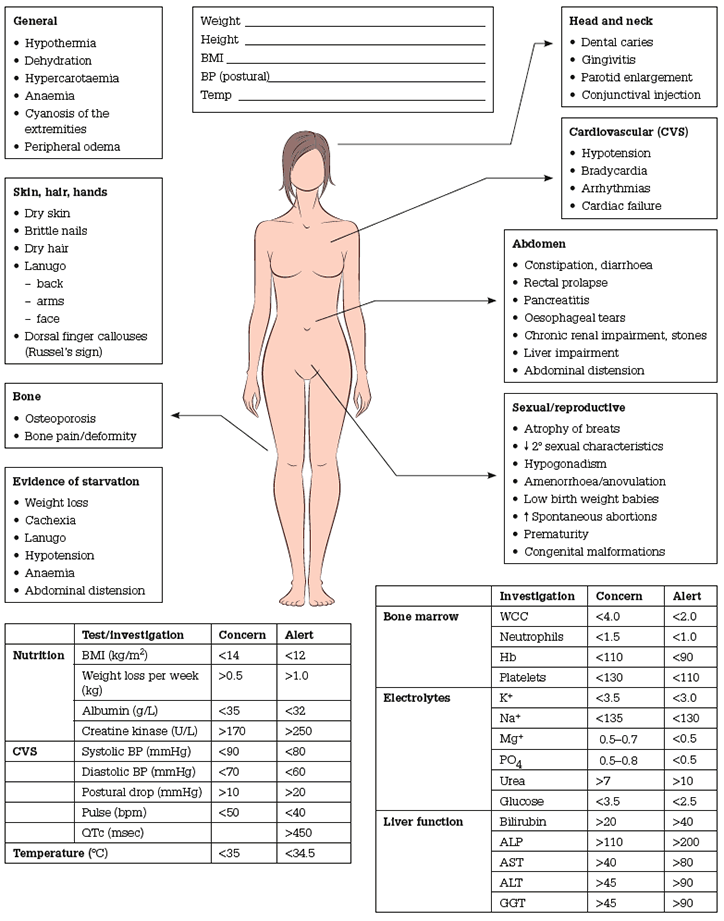
Figure 1. Body image Eating disorder Treatment and Recovery Service (BETRS). Eating Disorder alert sheet developed by the team, 2010
The psychological minefield
Presented with an anxious relative, who is concerned that their child may be starving themselves, and a reluctant patient, the GP may initially be at a loss. The relative often presents a mixture of emotions – guilt, anger, frustration and helplessness.
The patient is usually ambivalent about change, not fully connected to their emotions and masking the intensity of their fear, anger, sadness and/or low self-esteem. If the GP is not aware of this pool of emotions, this first tentative contact can lead to the patient being even more reluctant to consider there is a problem with their eating and not engage with treatment.8,9
Patients with an eating disorder tend to use various psychological strategies to make their day-to-day existence tolerable. These include, denial of any problems, projecting unwanted feelings onto others and avoidance. Once the patient is significantly underweight the cognitive changes of starvation exacerbate avoidance of unwanted emotions and thus starvation becomes both a precipitating and maintaining factor.11
At the core of the psychological component of anorexia nervosa, the patient has low self-esteem and impaired self-worth that has become linked to appraisals of their weight and shape.7,9,23,24 Being aware that some of these defences might be active during the consultation can help the GP be mindful not to react if the patient suddenly becomes angry or frustrated. Maintaining positive regard for patients and their family members may be all that can be done to begin a therapeutic alliance, which will be critical in keeping the anorexic patient engaged in treatment and limiting the burden on the carer.8,25,26
Many caregivers worry they have caused the illness and carry guilt, which can lead to anger that may be directed towards the patient, the GP or the specialist service.8 By allowing carers to vent their frustration and feelings of guilt, and providing psychoeducation, the GP can help reduce this distress.5,7,8,26 Using a stance taken from motivational interviewing, the GP can help guide the patient towards change in a collaborative manner.24,27 It is important to remind patients that the eating disorder exists for a reason and part of their recovery includes finding alternative coping strategies and will take time. Help them see the pros and cons of change in relation to simple achievable goals and be curious with them about how they can promote change.7,24,27 Questions that could be asked include, ‘What was happening when you were able to follow a meal plan?’, and, ‘How did this feel?’.
Another common response to anorexia nervosa is fear and mistrust.6,7 The patient has often covered up their disordered eating prior to diagnosis and, when in treatment, may be compelled to continue anorexic behaviours to compensate for any observed eating. The shame associated with this may often cause adamant denials of compensatory behaviours even when there is clear evidence to the contrary.23,28 The GP’s best approach is to allow for all compensatory behaviours and discuss risk management rather than pursuing revelations of disordered behaviour.
Does this mean the GP should be vigilant in asking about behaviours if they are not volunteered or require some other sort of strategy? If the therapeutic relationship begins with a screen then this can be used regularly to ‘check in’ with the patient or their carers about various behaviours including compensatory exercise, purging or deliberate self-harm, all of which may occur during the course of this illness with the same patient.
Treatment
The treatment of anorexia nervosa uses a stepped approach which for most is community- rather than hospital-based.1,3,15,18,29 All patients with anorexia nervosa should have a dietitian, a psychologist/psychiatrist for psychological treatment and ongoing contact with their GP.3,18,29 If the patient engages with these practitioners, is able to maintain their development in relation to career and interpersonal relationships, and begins to restore their weight, then treatment may stay at this level.
Often patients need referral to the local area mental health service (AMHS) or a specialist treatment program (see Resources for websites). The latter is to allow for more ongoing support to weight restore while giving psychological treatment, psychoeducation about the illness and a greater understanding of why they found this behaviour a solution to their problems.18,30 There is a paucity of publicly funded specialist programs across Australia but local AMHSs can assist the GP to access what is available for their patient and liaise with tertiary referral centres in the public or private area to provide direction of treatment.
In terms of treatments specifically for anorexia nervosa, a Cochrane review found that family-based therapy (FBT), also known as the Maudsley Method, for people under 18 years is more effective than ‘treatment as usual’.31 It has been shown recently that FBT is better accepted by adolescents and parents, and reduces the stigma and helplessness experienced during the treatment of this illness.32 FBT as an early intervention may help reduce the cycle of shame, guilt and recriminations that can occur between the patient and their family.7,23,26,32
Hospitalisation can be critical for short-term medical rescue, intensive treatment of the whole illness, respite for the family and outpatient treating team or a combination of these. Hospital treatment should be considered if there is immediate danger to life secondary to physical deterioration; suicide risk; no adequate outpatient treatment available or the patient has failed to progress despite appropriate outpatient treatment. Admissions that arise out of anxiety and highly expressed emotions tend to be unproductive for the patient, GP and the family. A patient with anorexia nervosa can be kept alive by enforced treatment but it is difficult for them to enter into any meaningful recovery until they are willing to engage with biological and psychological treatment.1
Using Figure 1 as a guide, the GP can decide when to refer their patient to the local emergency department for assessment and possible admission. The family and care providers can feel very nihilistic at times but there is always room for hope. Longitudinal outcome studies indicate that even a person with severe enduring anorexia nervosa can recover.28 However, there may be many chronic medical and psychosocial problems remaining that require extensive rehabilitation.
Regardless of whether the person has an inpatient admission or completes an outpatient program, the GP continues to coordinate treatment and is often the patient’s most consistent care provider. The aim of management should be to assist the patient to maintain a maximum tolerable weight, deal with psychological distress without resorting to weight loss and focus on improving their quality of life.
Liaising with other specialists
Recovery can take years and more often than not be punctuated with lapses, relapses and comorbid psychiatric problems. Assisting the patient and carers cope with anxiety and uncertainty while involving specialist services (Table 4) is a key role of the GP.15,33 Clinicians managing a patient with significant anorexia nervosa have to balance the need to keep the patient alive with the need to engage the patient in long-term treatment.
Table 4. The multidisciplinary team to assisting in the management of patients with anorexia nervosa
|
The dietician assists with realistic meal plans and advise patients and their family on how to re-introduce foods in a safe manner.
The psychiatrist or psychologist assists in cognitive therapy for the constant thoughts and behaviours that rule the disordered approach to food.
The area mental health services in Australia are learning to manage patients with anorexia nervosa and can coordinate care from suburban, regional and remote areas. They can also assist the GP to care for the patient and the family and/or carers.
|
There is no evidence that restoring a patient’s weight to normal against their will improves the long-term outcome of the illness. Indeed there is reason to believe that weight restoration without the active participation of the patient will lead to intense anxiety that is relieved on discharge from hospital by a return to self-induced weight loss, thus positively reinforcing both the association of weight gain with distress and self-induced weight loss with relief.
The people around the patient with anorexia nervosa often have an understandable yet simplistic view of helping their loved one, including ‘make them eat’, yet are unable to do so, leading to a mixture of powerlessness, helplessness and frustration. It is often intolerable to feel this way towards someone one loves, so these emotions are projected towards the doctor and this can make interactions distressing, anxiety-provoking and result in the GP feeling overwhelmed, anxious and at times angry.6,8,10,15,25,26,33 If recognised by the clinician as projection then they are dealt with more easily.
Conclusion
People affected by eating disorders, particularly anorexia nervosa, may deny having a problem, minimise their symptoms and resist treatment yet engage partially with their GP. Thus the GP is integral to keeping the patient in healthcare by establishing a strong therapeutic relationship based on trust and an ability to withstand the strong emotions that are elicited.
Resources
- International/national organisations:
- Families Empowered and SupportingTreatment of Eating Disorders (FEAST) is an international organisation of and for parents and caregivers, infor@feast-ed.org, http://feast-ed.org/FEAST
- Australian New Zealand Academy for Eating Disorders (ANZAED) Disorders, www.anzaed.org.au
- Royal Australian and New Zealand College of Psychiatrists (RANZCP) guidelines, www.ranzcp.org/Files/Resources/Publications/CPG/Clinician/CPG_Clinician_Full_Anorexia-pdf.aspx
- The National Eating Disorders Collaboration resources (prepared for the Commonwealth Department of Health and Ageing, www.nedc.com.au
- Victorian Centre of Excellence in Eating Disorders (CEED), The Royal Melbourne Hospital – Royal Park Campus, email: ceed@mh.org.au
- Headspace, www.headspace.org.au
- New South Wales, The Butterfly Foundation, supportline: 1800 33 4673, e-mail: support@thebutterflyfoundation.org.au, www.thebutterflyfoundation.org.au
- InsideOut is Australia’s national institute for research and clinical excellence in eating disorders, https://insideoutinstitute.org.au/
- Eating Disorders Victoria (EDV) is a non-profit organisation that aims to support those affected by eating disorders and to better inform the community about disordered eating, www.eatingdisorders.org.au
- Eating Disorders Association Inc Queensland is a non-discriminatory, non-profit organisation funded by the Mental Health Branch of Disability Services Queensland, to provide information, support and referral services for the state of Queensland, Australia, www.eda.org.au
- Isis The Eating Issues Centre works with people aged over 17 years with serious eating issues such as anorexia nervosa, bulimia and compulsive eating, www.isis.org.au
- Women’s Health Works is a non-profit community organisation in Western Australia that provides a range of education, information and support services to women, including self help groups for people experiencing an eating disorder, www.womenshealthworks.org.au
- ARAFMI Mental Health Carers & Friends Association Incorporated is a non-profit community-based organisation in Western Australia that provides information and support for families and friends of people with mental health issues, including family support counselling, support group program advocacy, respite and community education.
- Eating Disorders Association of South Australia (EDASA) is a non-government, not-for-profit incorporated association providing practical advice, empathic support and guidance for those affected by eating disorders in South Australia, www.eatingdisorderssa.org.au/
- Centacare: PACE supports individuals living with panic anxiety, obsessive compulsive and eating disorders and those that support them. Services include telephone support, face to face counselling and referral pathways, www.centacare.org.au/OurServices/HealthWellbeing/PACE.aspx#
- ARAFMI Tasmania, www.arafmitas.org.au
- Top End Mental Health Services (TEMHS), Northern Territory, www.health.nt.gov.au
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.