Question 1
What is the most likely diagnosis?
Question 2
What differential diagnoses would you consider?
Answer 1
The patient developed facial subcutaneous emphysema as a result of her dental procedure. Subcutaneous emphysema refers to the collection of air beneath the subcutaneous tissue. It is more commonly seen in facial bone fractures, infection by gas-producing organisms, tracheostomies and anterior neck dissections.1 Subcutaneous emphysema is a known, but rare, complication of dental procedures, especially extraction of the third molar.2–4 This is caused by the use of air-driven surgical instruments such as high-speed surgical drills and compressed-air syringes. It has been proposed that the use of these tools can push compressed air into the space between tissues, especially if there is a break in the mucosa;1 this probably accounts for the unusual sensation experienced by the patient during the procedure. The earliest documentation of this complication dates back to 1900 when an infantry bugler developed facial swelling when blowing his bugle after having a tooth extracted.5
Answer 2
Differential diagnoses of hemifacial swelling with periorbital oedema in this patient include:
- an allergic reaction precipitated by either the local anesthesia or latex in the dentist’s gloves
- angioedema
- facial haematoma
- cellulitis
- surgical emphysema secondary to fracture of the facial sinuses.
The first four differentials do not produce the classical crackling sounds or crepitus of subcutaneous emphysema when pressure is applied to that area.
Case study continued
The patient was referred to a dental surgeon. Further imaging was deemed not necessary as the emphysematous area was localised to the patient’s face and had not progressed downwards from the angle of her jaw. Furthermore, there were no respiratory symptoms.
The patient was discharged with a course of antibiotics (a penicillin and a nitroimidazole, eg. metronidazole) to prevent odontogenic infections. Dual antibiotic treatment was given because the patient was deemed to be at an elevated risk of bacterial transfer into the surrounding bone and tissue due to the extensive surgical manipulation and prolonged operation time. A formal hearing assessment done 3 days later was normal. The facial swelling and crepitus spontaneously resolved over a period of 6 days.
Question 3
What possible complications might arise?
Question 4
What imaging methods can be used to confirm the diagnosis?
Question 5
What are the treatment options for this condition?

Figure 1. Left hemifacial swelling with fullness over the left nasolabial fold
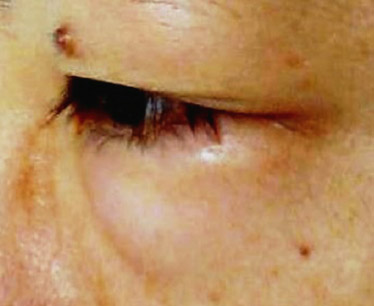
Figure 2. Left periorbital oedema
Answer 3
Cases of periobital oedema and surgical emphysema as a complication of a dental procedure have been well documented.1,4,6–9 Interestingly, periorbital oedema in one of the cases documented was not due to surgical emphysema as it did not have the characteristic crepitus. Instead, it was suggested that normal saline might have been forced upwards via the muscosal break at the treatment site on the patient’s upper jaw by pressurised air from the drill.9 Although the emphysema is usually limited to the subcutaneous spaces of the head and neck, it is possible for the air to track along the fascial planes of the neck, causing para- and retropharyngeal emphysema.10 Pneumomediastinum and pneumothorax have also been documented following a seemingly simple procedure such as extraction of the lower molar.2 As air in the free spaces may be contaminated by oral bacteria, there is also risk of infection to these areas.1,6 Other possible complications include transient hearing disturbances and retinal artery and optic nerve damage.9
Answer 4
Although surgical emphysema is usually a clinical diagnosis, imaging may be used to determine the extent of the air tracking and assist in the management. Plain anterioposterior and lateral neck films will show lucency where air is present. A chest radiograph also rules out possible complications such as pneumothorax, pneumomediastinum or pneumopericardium. A computed tomography (CT) study of her face and neck will help to differentiate it from fluid collections or masses.
Answer 5
Management depends on the severity and extent of the subcutaneous emphysema. Most cases will start resolving spontaneously after 2–3 days. Complete resolution usually takes 7–10 days.11 Prophylactic antibiotic should be given to the patient as there is a risk of introducing oral bacteria into the air spaces either via direct transfer or through contaminated air or fluids.1,6 It is prudent that patients with neck or mediastinal involvement be admitted for observation of potential respiratory distress or cardiovascular compromise. Surgical decompression is usually reserved for dangerous space emphysema10 and should not be routinely done as it is unlikely to be effective and may even aggravate or promote the spread of the emphysema.3
Key points
- Periorbital oedema and subcutaneous emphysema can occur as uncommon complications following dental procedure.
- Symptoms may develop hours after the procedure when the patient is at home and hence the patient may present to a family physician.
- Severe cases can have dire consequences if there is a failure to diagnose and manage them appropriately.
Competing interest: None.
Provenance and peer review: Not commissioned, externally peer reviewed.
Acknowedgements
The author wishes to acknowledge the Director General of Health Malaysia for his permission to publish, and the CRC Sibu, Sarawak for their assistance with this manuscript.