Data from the Australian Medical Treatment Survey 1990–91, and from BEACH (Bettering the Evaluation and Care of Health), were analysed to detect changes in the management rate of PAD since 1990. Figure 1 shows that management decreased significantly between 1990–91 and 2003–08 for all general practice patients, despite the significant increase in the proportion of older patients in the population over the past 2 decades. This change was more pronounced for patients aged 40 years and over.
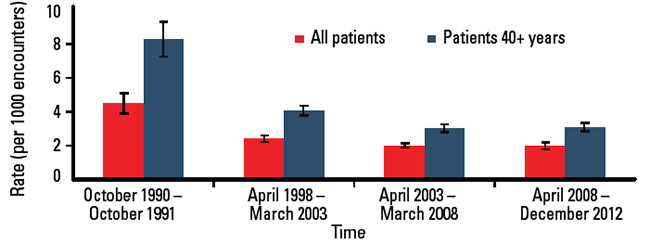
Figure 1. Change in management rate of peripheral arterial disease 1990–2012 (with 95% CI)
Analysis of data from April 2008 to December 2012 showed that the management rate was significantly higher for males than females, and with increased patient age. While the majority of PAD was unspecified (56.3%), intermittent claudication contributed 12.2%, Raynaud disease/phenomenon 11.8%, gangrene 4.4%, and atherosclerosis 4.0%.
Comorbidities most often managed with PAD were hypertension (10.7% of other problems), diabetes (8.0%), lipid disorders (3.9%), and ischaemic heart disease (3.7%). For newly diagnosed PAD (30.8% of total PAD), diabetes was the most common other problem managed at the same encounter (10.0%).
Management per 100 PAD problems included medications (33.5), most commonly antithrombotic agents (9.6), lipid modifying agents (5.0), and opioids (5.0); clinical treatments (22.4), such as advice/education (9.5%) and counselling (9.0); procedural treatments (9.9); referrals (22.3), mainly to vascular surgeons (13.2) and podiatrist/chiropodists (1.7); pathology (23.8), including lipid testing (3.9) and full blood counts (3.7); and imaging (16.6), primarily for Doppler testing (9.7) and ultrasound of the leg (1.9).
The decrease in the management rate of PAD since 1990 has likely resulted from multiple factors. Since 1996, a number of policy changes involving health assessments and care plans for elderly patients, other population sub-groups, diabetes and other chronic diseases, have subsumed the specific management of PAD into other care plans.4 Also, the prevalence of daily and occasional smoking by general practice patients has decreased significantly since 1998, with a corresponding significant increase in the proportion who have never smoked (Table 1).5,6 These factors will have contributed to the reduction and postponement of PAD managed in Australian general practice patients.
Table 1. Smoking status of patients 1998–2012 (95% CI)
| Smoking status | 1998–99 | 2011–12 |
|---|
| Daily |
19.2 (18.4–20.0) |
14.7 (14.0–15.3) |
| Occasional |
6.2 (5.6–6.8) |
2.5 (2.3–2.7) |
| Never smoked |
34.5 (33.3–35.7) |
54.9 (53.9–55.8) |
Competing interests: None.
Provenance and peer review: Commissioned; not peer reviewed.
Acknowledgements
The authors thank the GP participants in BEACH and all members of the BEACH team. Funding contributors to BEACH from April 1998 to March 2012: Australian Government Department of Health and Ageing; AstraZeneca Pty Ltd (Australia); CSL Biotherapies Pty Ltd; Merck Sharp & Dohme (Australia) Pty Ltd; National Prescribing Service; Novartis Pharmaceuticals Australia Pty Ltd; Pfizer Australia Pty Ltd; Abbott Australasia Pty Ltd; Janssen-Cilag Pty Ltd; Sanofi-Aventis Australia Pty Ltd; GlaxoSmithKline Australia Pty Ltd; Bayer Australia Ltd; Wyeth Australia Pty Ltd; and Roche Products Pty Ltd.
BEACH is approved by the Human Research Ethics Committee of the University of Sydney.