Osteoporotic fractures are very common, with a fracture occurring every 3 seconds and a vertebral fracture every 22 seconds worldwide.1 Osteoporosis currently affects 10% of the Australian population, with $1.9 billion being spent in 2007 on direct costs associated with this disease.2
Unfortunately, it appears that many individuals are not being appropriately diagnosed or treated for osteoporosis in Australian general practice, as the majority of individuals considered to be high risk (having at least one previous osteoporotic fracture) are neither identified nor treated.3 A study of over 8800 postmenopausal Australian women showed that almost one-third had an osteoporotic fracture, yet more than 80% of these women had neither been investigated nor treated to reduce their risk of a further fracture.4 These women carry a considerable risk of long term morbidity and mortality for osteoporotic fractures.
Morbidity and mortality
Peripheral, vertebral and hip fractures associated with osteoporosis can happen as a result of minimal trauma to weakened bones. These fractures often have a wide range of effects on patients, both physically and psychologically, including short term pain and morbidity, and long term loss of height, bone deformities, chronic pain, disability and death. Hip fractures in particular are the most serious consequence of osteoporosis, with 24% estimated to die within 12 months,5 and an increased risk of death for at least another 4 years.6
Guidelines
There are a number of guidelines regarding risk calculation for osteoporosis, however, these often differ substantially on their recommendations. Fortunately, they all generally agree that there are a number of ‘important’ risk factors for osteoporosis, such as age, previous vertebral fracture, and low trauma fracture.
This study applied guidelines from The Royal Australian College of General Practitioners (RACGP),7 as these are widely used by general practitioners in Australia.
The RACGP guideline recommends BMD scanning for any person with a minimal trauma fracture or vertebral fracture confirmed on spinal X-ray (Figure 1), or the presence of major risk factors, including age >60 years, low body weight, and being a cigarette smoker (Table 1).
Table 1. Major risk factors for osteoporosis7
| Age (over 60 years) |
One or more vertebral or low trauma fracture |
| Prolonged glucocorticoid therapy (>7.5 mg prednislone or equivalent >3 months) |
Excess alcohol intake (2–4 standard drinks per day for men, 1–2 standard drinks per day for women, over 5 days per week) |
| Male or female hypogonadism |
Primary hyperparathyroidism or thyroxine excess |
| Chronic liver or renal disease |
Rheumatoid arthritis |
| Malabsorption |
Low BMI (<20) |
| Family history of hip fracture |
Immobilisation |
| Current smoker |
Glucocorticoid secretion |
| More than one fall in the past year |
|
| Source Clinical guideline for the prevention and treatment of osteoporosis in postmenopausal women and older men. The RACGP, 2010 |
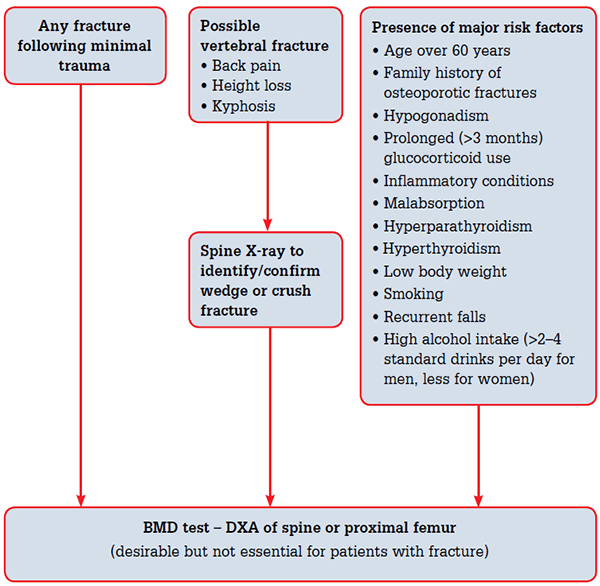
Figure 1. The RAGCP recommendations for bone mineral density scanning7
Reproduced with permission Clinical guideline for the prevention and treatment of osteoporosis in postmenopausal women and older men. The RACGP, 2010
The aim of this study was to audit 10 GPs for their identification of patients with risk factors for osteoporosis, plus appropriate screening, treatment and follow up care.
Method
Selection and description of participants
The medical records of 10 GPs from a rural medical centre in New South Wales for the period 1 January 2000 through to 20 March 2012 were audited. Both men and women aged >60 years with at least one additional osteoporotic risk factor were evaluated for their screening and treatment status, ie. the population requiring DXA screening and at clear risk of osteoporotic complications.
In total, there were 7347 active (three or more visits in 2 years) and long term (over 2 years) patients in the practice database, with 1589 aged >60 years.
Information collected included whether a DXA scan had been performed, the result (normal, osteopenia or osteoporosis), and the nature of treatment types (Figure 2). Each patient’s notes were examined and those with extenuating circumstances such as ‘patient refused DXA scan’ or ‘patient refused treatment’ were excluded.
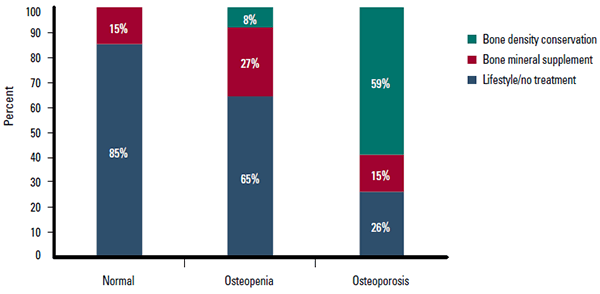
Figure 2. Osteoporosis status vs treatment type
Technical information
Information was extracted from the practice database using the Best Practice software and the clinical audit tool (PENCAT) developed by Pen Computer Systems.8 Simple frequency analysis was used to highlight the differences in the patients’ gender, age, and risk factors in relation to the management (screening, treatment and follow up care) of osteoporosis.
Results
There were 402 subjects: 185 men (46%) and 217 women (54%), aged 60–95 years (71.5 +/– 8.6 [mean +/– standard deviation]). The most common risk factors were glucocorticoid use (195), high alcohol intake (143), previous fracture (62), and smoking (42). Low frequencies were recorded for excessive thyroxine dosage (18), rheumatoid arthritis (10), low body mass index (BMI) (8), malabsorption (3), and primary hyperparathyroidism (2). The prevalence of individual risk factors is outlined in Figure 3.
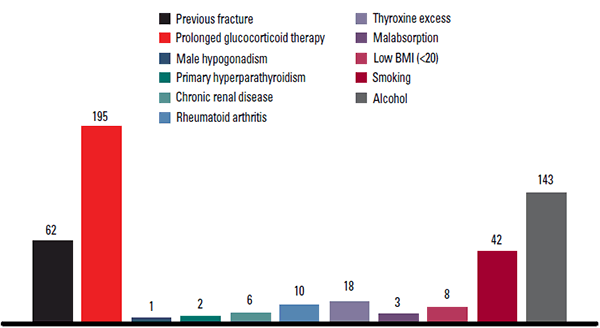
Figure 3. Prevalence of individual risk factors
Risk factors vs scanning
In addition to age, patients had a total number of risk factors ranging between one and six. Men had on average 1.7 risk factors, and women 2.8. The largest group was individuals with two risk factors (172) representing 43% of the total group (Table 2). This group also had the most even distribution of men (53%) to women (47%). From the 172 individuals in this group only 50 (29%) had been screened for osteoporosis; however, as the risk factors increased, the number of DXA screening rate also increased. For example, patients with three risk factors had a screening rate of 49%, four risk factors at 51.7%, and at five risk factors the screening rate was 67%. Interestingly, all the patients with one risk factor (77) were male and only 12 (16%) of these patients had previously been scanned for BMD. Additionally, eight (67%) of these individuals that were scanned showed low BMD. Women accounted for 137 (90%) of the 153 individuals with multiple (3–6) risk factors and 77 (56%) of these individuals were screened for osteoporosis.
Table 2. Risk factors vs DXA scan
| Risk | Total | Percentage | Male | Female | Had DXA | Percentage |
|---|
| One risk factor |
77 |
19.0% |
77 |
0 |
12 |
16% |
| Two risk factors |
172 |
43.0% |
92 |
80 |
50 |
29% |
| Three risk factors |
120 |
30.0% |
14 |
106 |
59 |
49% |
| Four risk factors |
29 |
7.0% |
2 |
27 |
15 |
52% |
| Five risk factors |
3 |
0.75% |
0 |
3 |
2 |
67% |
| Six risk factors |
1 |
0.25% |
0 |
1 |
1 |
100% |
| Total |
402 |
100% |
185 |
217 |
139 |
(Avg) 35% |
According to the guidelines,7 any individual with low trauma fracture or vertebral fracture should receive a DXA scan. Only 25% of the individuals in this cohort with a fracture alone received a DXA scan. This figure rose as risk factors were added to individuals with fractures. For example, 44% were scanned with a fracture plus one risk factor, 60% for fracture plus two risk factors, and 79% for fracture plus three risk factors (Table 3).
Table 3. Fracture + risk factors vs DXA scan
| Fracture + risks | Total | Percentage | Male | Female | Had DXA | Percentage |
|---|
| Fracture alone |
4 |
6.45% |
4 |
0 |
1 |
25% |
| One risk factor |
18 |
29.03% |
8 |
10 |
8 |
44% |
| Two risk factors |
25 |
40.32% |
4 |
21 |
15 |
60% |
| Three risk factors |
14 |
22.58% |
0 |
14 |
11 |
79% |
| Four risk factors |
1 |
1.61% |
0 |
1 |
0 |
0% |
| Total |
62 |
100% |
16 |
46 |
45 |
(Avg) 73% |
Regarding the risk factors alone, the screening rates were relatively high for: previous fracture (56%), low BMI (63%), primary hyperparathyroidism (100%), and rheumatoid arthritis (50%). Low screening rates were shown for smokers (21%) and those with a high alcohol intake (15%).
Finally, regarding age groups, those aged 60–69 years had a scan rate between 20% and 27%. The scan rate then peaked at between 49% and 50% for those aged 70–79 years, and then dropped to between 25% and 30% for those aged 80–95 years.
Management
Of the 402 patients in this data set, 139 (35%) had DXA scans, of which 36 (26%) showed a normal scan, 64 (46%) showed osteopenia, and 39 (28%) showed osteoporosis. Of those with a normal scan, five (14%) patients were prescribed calcium supplements. Within the osteopenia group, five (8%) individuals were receiving bone density conservation therapy, 18 (28%) were receiving bone mineral supplements, and 42 (66%) were either being treated with lifestyle changes or not receiving any treatment. Finally, of the osteoporosis patients, 23 (59%) were receiving bone density conservation therapy, only six (15%) were receiving bone mineral supplements, and 10 (26%) were receiving no treatment at all (Figure 2).
Follow up care
Of the 402 patients, 132 had DXA scan(s) in the period from 2000 to 2012, of which 36 patients (26%) were reported normal and 101 patients (74%) showed low BMD.
The RAGCP guidelines recommend that all patients with risk factors for osteoporosis be scanned by DXA, not only for diagnosis, but also for baseline and follow up care.
In this study, the last DXA scan was recorded in order to assess the ongoing management of patients with a recorded diagnosis of osteopenia or osteoporosis. It is recommended that patients be scanned at least every 2 years after a diagnosis, however, the data show that although 53 (52%) of the patients had their last DXA scan between 2010 and 2012, a further 48 (48%) have not had any follow up scanning beyond 2 years.
Discussion
This study found that only 1 in 3 patients were correctly identified as having one or more major risk factors and subsequently considered for a DXA scan.
There were a number of interesting patterns that emerged from this study regarding who was screened and who was missed. First, the total number of risk factors for each individual, correlated to their chance of receiving a DXA scan. For example, patients with one risk factor had a 16% chance of receiving a scan while those with four risk factors had a 52% chance. If one of these risk factors included a low trauma or vertebral fracture, this figure again rose sharply, and those with four risk factors including a fracture, were scanned at 79%. This highlights that general practitioners understand the importance of fractures above other risk factors; however, this still leaves a large percentage of patients with multiple risk factors for osteoporosis (including some with fractures) undiagnosed and without treatment.
Women were also more likely to be screened at 46% compared with a low of 21% for men. This is not surprising, as although the RAGCP guidelines treat men and women equally, a number of other guidelines, such as The World Health Organization Fracture Risk Assessment Tool (FRAX®),9 regard women more at risk than men.
Age was an important factor impacting the decision to order DXA scans. Low screening rates were recorded for those aged less than 70 years or more than 80 years, peaking in-between.
This study also measured appropriate management. Those with known osteopenia should be treated with lifestyle changes, bone mineral supplements, and possibly bone density conservation therapy (Table 4). However, 66% were not receiving any form of treatment (not including lifestyle changes) and only 28% were receiving bone mineral supplements, such as calcium and vitamin D. Additionally, of the patients with known osteoporosis, only 59% were receiving bone density conservation therapy (the mainstay of treatment), and 15% were receiving bone mineral supplements only. This has left 26% of known osteoporosis patients receiving no treatment at all. These figures broadly suggest that either the primary care management of osteoporosis is not adequate or some other factor is interfering with these results.
Table 4. Treatment of osteopenia and osteoporosis7
| Osteopenia | Osteoporosis |
|---|
Consider preventive anti-osteoporotic therapy
- Calcium and vitamin D supplements when dietary intake is inadequate, and, depending on the degree of osteopenia/osteoporosis:
- Bisphosphonates
- Hormone therapy
- Strontium ranelate (women only)
|
Initiate anti-osteoporotic therapy
- Calcium and vitamin D supplements when dietary intake is inadequate
- Bisphosphonates
- Hormone therapy
- Parathyroid hormone (teriparatide)
- Selective oestrogen receptor modulators (SERMs)
- Strontium ranelate (women only)
|
|
Source Clinical guideline for the prevention and treatment of osteoporosis in postmenopausal women and older men. The RACGP, 2010
|
Limitations
The accuracy of the recorded clinical data underpinning this study is unknown. For example, lifestyle changes may have been recommended and not recorded, or a DXA scan considered and then not acted upon especially if there were issues accessing Medicare funding for the scan.
Recommendations
General practitioners are the healthcare hubs of our communities, including for prevention of diseases such as osteoporosis. The low level of concordance with the guidelines suggests that in this general practice community, passive screening for osteoporosis has been less than effective. Active surveillance, such as the PENCAT tool used in this study, would offer an alternative approach. Further studies could then evaluate whether incorporating this into the usual practice audit process leads to improved patient outcomes.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.