Although general practice is often the most important first point-of-contact with the healthcare system for refugee families,5 a South Australian study interviewing 12 general practitioners with experience in refugee health suggests that GPs are under-resourced at a personal and a structural level to provide effective initial care for refugees.4–6
Refugees have complex and diverse healthcare needs, and it is recognised that general practice would benefit from education, training and support of those staff involved in refugee care.1,7 Underlying these practical issues, limited research has been published in the area of physician attitudes toward refugees and asylum seekers. Begg and Gill8 have published one such study, however, their research is based on 17 GPs across greater Birmingham (United Kingdom) without incorporating regional GPs.
The purpose of this study was to explore the level of contact a cross-section of regional and rural GPs had with community based people from a refugee background, how comfortable they were working with these patients, the impact that dealing with refugees had on their practice, and the supports needed in order to effectively help the refugee population.
Methods
A short, one page questionnaire on refugee health was first distributed to 107 participants (aged 25–65 years) at a CoastCityCountry General Practice Training (CCCGPT) GP supervisor training weekend in March 2012. CCCGPT is an organisation within the Australian General Practice Training (AGPT) system for the postgraduate specialty education of GPs. The sample was chosen because it provided a convenient sample of GP supervisors who are responsible for the training of general practice registrars and could be expected to exert some influence on behaviour within the practice. The training weekend allowed a rapid sampling of supervisors across southern New South Wales and the Australian Capital Territory, and from a range of practice settings including coastal, suburban, remote and rural.
A comparison was then undertaken with registrars. Questionnaires were distributed to 46 registrars (aged 25–30 years) at a registrar education day in August 2012. The questionnaire was identical to that distributed to the supervisors, with a further question about supervisors.
Statistical analysis
Data were analysed using SPSS (Version 20, SPSS Inc., Chicago, USA). Percentages were calculated for all questions. Differences in responses between groups were analysed using Pearson’s chi-square tests (c2) at p<0.05 significance level. Due to small cell numbers in some instances, some categories were combined. If participants could choose, for example to the question: ‘Have you found that working with refugees disrupts your practice schedule?’ ‘very disruptive’, ‘disruptive’ or ‘not disruptive’, responses were grouped into positive and negative categories, ie. very disruptive and disruptive were combined into one category and not disruptive at all was a separate category. Any question that still had low cell numbers was analysed using Fisher’s exact test. Bivariate correlations (Spearman’s rho) were also calculated for those questions relating to attitude and support/education perceptions of participants.
Results
Responses were obtained for 56 supervisors and 20 registrars. A demographic summary of registrar and supervisor respondants is presented in Table 1. Athough fewer supervisors were international medical graduates (IMGs), the difference was not significant. However, there was a significant gender difference between supervisors and registrars (p=0.04). Only 20% of the registrars who responded to the questionnaire were male, whereas the gender split was almost 50:50 in the supervisor group.
Table 1. Demographics of survey participants
| Response n (%) |
|---|
| Registrars | Supervisors | Total |
|---|
| Gender |
Female |
16 (80) |
29 (53.7) |
45 (60.8) |
| Male |
4 (20) |
25 (46.3) |
29 (39.2) |
| Australian graduate |
No |
8 (40) |
15 (27.3) |
23 (30.7) |
| Yes |
12 (60) |
40 (72.7) |
52 (69.3) |
| Country where medical qualifications were conferred |
Australia |
12 (60) |
40 (71.4) |
52 (68.4) |
| Asia |
7 (35) |
4 (7.2) |
11 (14.4) |
| UK |
0 |
4 (7.2) |
4 (5.2) |
| Other |
0 |
7 (12.6) |
7 (9.1) |
| How often do you see refugee patients in your practice? |
Daily |
0 |
1 (1.8) |
1 (1.3) |
| Weekly |
3 (15) |
4 (7.1) |
7 (9.2) |
| Monthly |
2 (10) |
7 (12.5) |
9 (11.8) |
| Infrequently |
14 (70) |
25 (44.6) |
39 (51.3) |
| Never |
1 (5) |
19 (33.9) |
20 (26.3) |
Overall, 20–25% of both groups saw refugees at least once a month. However, more than one-third of supervisors had never treated a refugee patient, while only one registrar (5%) had never seen a refugee patient in their practice. Practitioner attitudes toward refugee patients are presented in Table 2. There were no significant differences between supervisors and registrars in their perceptions of refugee patients disrupting their practice, with more than 70% reporting that refugee patients were not disruptive at all. Interestingly, more than 60% of the respondants in both groups reported that refugee patients actually enhanced their practice. Almost 62% of supervisors and 77% of registrars reported that treating refugees enhanced or considerably enhanced their practice. When participants were asked about the benefits of being involved with refugee health, the overwhelming message was the underlying altruism in the work. Many responses related to the satisfaction gained in helping and serving the community and how involvement in refugee health helps to broaden one’s understanding, experience and scope of practice.
Table 2. Practitioner attitudes toward refugee patients treated in their practice
| Response n (%) |
|---|
| Registrars | Supervisors | Total |
|---|
| Does working with refugees disrupt your practice schedule? |
Very disruptive |
0 |
1 (2.9) |
1 (1.9) |
| Disruptive |
5 (27.8) |
5 (14.3) |
10 (18.9) |
| Not at all disruptive |
13 (72.2) |
29 (82.9) |
42 (79.2) |
| Does working with refugees enhance your practice? |
Considerably enhances |
1 (5.9) |
2 (5.9) |
3 (5.9) |
| Enhances |
12 (70.6) |
19 (55.9) |
31 (60.8) |
| Not at all enhances |
4 (23.5) |
13 (38.2) |
17 (33.3) |
Confidence levels in dealing with refugees were similar between supervisor and registrar groups (Table 3). Almost two-thirds of both groups were either confident or very confident in their management of refugees and their medical issues, however, this dropped to 40–50% when it came to management of psychological issues. Participants who indicated that they were not at all confident commonly listed that they had minimal, if any, experience with refugees.
Table 3. Confidence of GP supervisors and registrars managing the medical and psychological issues of refugee presentations
| Response n (%) |
|---|
| Registrars | Supervisors | Total |
|---|
| Medical issues |
Very confident |
1 (5.9) |
2 (4.7) |
3 (5.0) |
| Confident |
10 (58.8) |
26 (60.5) |
36 (60.0) |
| Not at all confident |
6 (35.3) |
15 (34.9) |
21 (35.0) |
| Psychological issues |
Very confident |
0 |
2 (4.5) |
2 (3.3) |
| Confident |
7 (43.8) |
20 (45.5) |
27 (45.0) |
| Not at all confident |
9 (56.2) |
22 (50.0) |
31 (51.7) |
As a group, IMGs were significantly less confident in dealing with the medical issues (p=0.02) refugees present with, yet there was no significant difference between IMGs and Australian graduates in their confidence in dealing with psychological issues. Interestingly, women from this study were significantly more likely to report that they do not feel confident in treating both medical (p=0.04) and psychological (p<0.01) issues of refugee patients.
When practitioners were queried about their satisfication with the support services available to assist them in treating refugees in their practice, more than 70% of both groups were either happy or very happy with the available services. Despite this level of satisfaction, almost 80% of registrars and 50% of supervisors would like more support in this area (Figure 1). Registrars were significantly more interested in obtaining additional support (p=0.04), however, there was no significant difference between requests for further education. More than 70% of both groups wanted more education to assist with treating refugee patients.
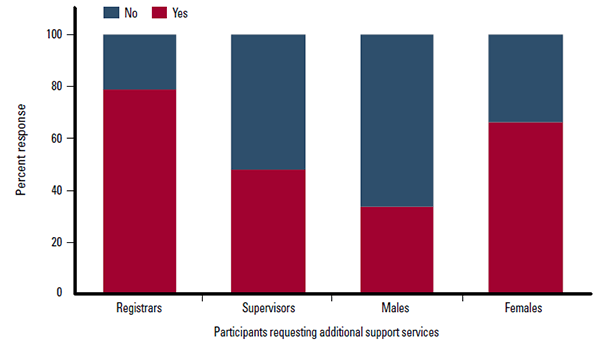
Figure 1. Proportion of participants requesting additional support services to assist in treating refugees (Differences between genders [chi-square=5.206, p=0.02] and training level [chi-square=4.071, p=0.04] are significant)
Females were more likely to request increased support services (p=0.02), while there was no gender difference in requests for further education. The more often supervisors and registrars saw refugees, the more likely they were to highlight the need for further education in the area (r=0.322). In addition, those respondents who reported that seeing refugees enhanced their practice were more likely to request further support (r=0.448) and education (r=0.377).
Discussion
Participants in this study differed from the general practice workforce as a whole, as there was a higher percentage of Australian graduates.9,10 Almost 73% of supervisors surveyed in this study were Australian graduates, and 84% had spent at least 10 years in general practice. However, the proportion of IMG registrars matched the reported rural profile of 41%, and it was found that these IMGs were significantly less confident in dealing with medical issues of refugee presentations. Mindful that in 2008, 62% of all rural pathway registrars were either trained overseas or were international students graduating from an Australian university,10 the need for additional support services in regional areas is highlighted. This is especially important when one considers the Australian Government policy to settle increasing numbers of refugees in regional and rural Australia.11
Surprisingly, there were no differences between the two groups in their confidence level in treating refugees. It was expected that registrars would be less confident due to less experience. However, this confidence may not equate with knowledge, as several of those who indicated that they were confident, also indicated they were confident they could access help and advice if they needed it. Almost 50% of participants who reported having little or no experience with refugees reported that they were confident in dealing with the unique issues facing refugee patients. Some confidence levels could be explained by tertiary institutions now teaching more about cross-cultural care. Another explanation could be that the high level of confidence was a false perception born out of lack of real experience. In this study, females were significantly more likely to report lack of confidence in treating both medical and psychological issues of refugee patients. Further research is needed to define reasons for these differences.
Both supervisors and registrars were less confident when it came to psychological versus medical issues. Comments such as: ‘transcultural psychological/social/relational/spiritual issues and concerns are amazingly complex’; ‘mental health clearly related to cultural issues’; and ‘can only begin to understand their prior experiences, language and cultural barriers impact on this’, indicate the awareness of the participants about barriers relating to refugee health.
Language and cultural barriers were the most common issues raised by participants. The importance of these social barriers12,13 and systemic barriers14 in influencing access to healthcare has been reported previously. Table 4 lists selected comments about both social and systemic barriers to refugee health, as reported by supervisors and registrars. Surprisingly, only one participant commented on time as a barrier in refugee health. There were several comments relating to funding and lack of access to Medicare funded specialist services within rural and regional areas.
Table 4. Selected comments about barriers to refugee health and potential solutions as reported by GP supervisors and general practice registrars
| Social | Systemic | Potential solutions |
|---|
| ‘Can only begin to understand their prior experiences; language and cultural barriers impact on this’ |
‘Lack of Medicare funded specialist services with ease in rural and regional areas, ie. GPs may bulk-bill but more difficult to have dentists and other specialist, imaging etc. participate’ |
‘Refugees (should) have a card like a DVA gold card that allows streamlined access to health services allowing GPs to concentrate on medical and social needs rather than financial and bureaucratic red tape’ |
| ‘Unfamiliarity with medical illness and psychological problems encountered’ |
‘Lots of red tape when they don’t have Medicare cards etc’ |
‘A refugee liaison person (GP community nurse or other) as a resource person with whom the GP could liaise to seek direction on difficult refugee issues’ |
| ‘Inexperience’ |
‘No cash for medicines’ |
‘Freedom to book longer consultations’ |
| ‘Cultural barriers’, ‘cultural differences’, ‘cultural knowledge’ |
‘Big ticket items claimed by initial assessor not their GP without sharing of results – pathology’ |
‘Approach mainstream practices to see refugees on a regular basis and help in organising transport, payment, interpreters, ongoing social links’ |
| ‘Language’ |
‘We don’t have enough GPs’ |
‘Cross-cultural awareness training’ |
When participants were asked about solutions that would be helpful for managing barriers in refugee health, education and cross-cultural awareness training were common responses (Table 4). One participant suggested that ‘refugees [should] have a card like a Department of Veterans’ Affairs gold card that allows streamlined access to health services, allowing GPs to concentrate on medical and social needs rather than financial and bureaucratic red tape’.
Despite the majority of registrars reporting that they were happy with the support services available, 80% indicated a strong desire for more support in this area. This was significantly higher than for the supervisor group where <50% wanted more support. Regarding education, 88% of registrars and 68% of supervisors desired more educational support. Comments indicating there was no need for additional support tended to be made by participants who did not have any contact with refugees. Those participants advocating for additional support responded that there was a need to ‘find out more about what services are available’ or that the services needed to be ‘more accessible’.
There are some limitations to this study. There is potential for bias in the study, as it only addresses supervisors involved with CCCGPT, thus, the results may not be applicable to other areas or to other GPs. In addition, participants responding to the questionnaire could have a personal interest in this area. However, within these similarly recruited groups, significant differences still remain.
Conclusions
There are significant challenges for general practice in ensuring good cross-cultural care. This study found a desire for more support and more education in relation to refugee healthcare. This is particularly important for IMGs, as IMGs make up a large proportion of GPs in rural Australia, and the IMGs in this study were significantly less confident than their Australian counterparts in dealing with the medical issues of refugee patients.
Reasons for the disparity between the levels of reported confidence in treating refugees and concrete knowledge needs to be further explored, as does the relative lack of confidence reported among female GPs.
An unexpected finding from this research was that there is a strong sense that there are benefits in dealing with refugee health. Further studies would be helpful in exploring this finding.
Competing interests: None.
Ethics approval: University of Notre Dame Australia Human Research Ethics Committee.
Provenance and peer review: Not commissioned; externally peer reviewed.