In 1971, when the Aboriginal Medical Service (AMS) Redfern opened its doors, Medicare did not exist and the only option for most Aboriginal and Torres Strait Islander families living in inner Sydney was to attend an emergency department or rely on the goodwill of local general practitioners. Many Aboriginal and Torres Strait Islander people experienced racism in the health system and wider community, and poverty was a major barrier to attending general practice or purchasing medicines.
The AMS Redfern
The AMS Redfern was the first community controlled health service in Australia and was founded in 1971 by Aboriginal and Torres Strait Islander community activists (Figure 1). Initially a 'shopfront' volunteer service on Regent street in Redfern, it was staffed by non-Indigenous doctors, nurses, nuns and students. Naomi Mayers, the current Chief Executive Officer, joined as secretary in 1972, Shirley Smith, affectionately known as Mum Shirl, was the first field officer and the late Professor Fred Hollows was instrumental in signing up medical students, doctors and volunteers.

Figure 1. Community activists involved in setting up AMS Redfern
Within a year of opening, AMS Redfern had become so popular it was unable to meet the demand for its services. Federal government funding was made available the following year and since then, AMS Redfern has grown into a multidisciplinary health service, consisting of a wide range of clinics and services including medical, dental, public health and outreach services (Figure 2). This community controlled model of health is now widely adopted, with over 150 Aboriginal community controlled health services (ACCHSs) in urban, regional and remote Australia.6
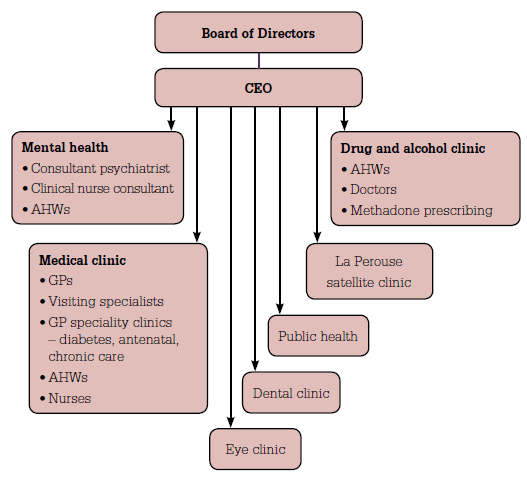
Figure 2. Structure of the AMS Redfern
The AMS Redfern has always been a free service for all Aboriginal and Torres Strait Islander patients and follows the principles of holistic healthcare, designed to care for the wellbeing of the whole community7 (Table 1). While the majority of patients are local, many come from rural and remote communities and visit the service when in Sydney to get their chronic health issues addressed.
Table 1. Principles of holistic healthcare as applied to Aboriginal and Torres Strait Islander health7 and adopted by NACCHO, 2006
|
'Health does not just mean the physical wellbeing of the individual but refers to the social, emotional and cultural wellbeing of the whole community. This is a whole of life view and includes the cyclical concept of life-death-life. Healthcare services should strive to achieve the state where every individual can achieve their full potential as a human being and thus bring about the total wellbeing of their community'
|
The AMS Redfern recognises that the education of health professionals is an integral nonpart of Indigenous healthcare. The first Aboriginal health workers (AHWs) course commenced in 1984 (developed by Sister Dulcie Flower) and a postgraduate program for training in mental healthcare followed. Aboriginal health worker training has since been moved to tertiary settings, but many of the original class continue to work at Redfern and subsequent graduates are employed in Indigenous medical and mainstream health services throughout New South Wales.
The AMS Redfern has also been a teaching practice for over 20 years. In the past 7 years the service has hosted 18 general practice registrars, of whom seven have remained in Aboriginal medical service employment on completion of their terms. With such a huge demand for training, the AMS Redfern also has a large number of short term placements for both medical and nursing students from the University of Sydney.
Over many years, AMS Redfern has developed and fostered links with local hospitals and specialists (Table 2), who have continued the tradition of the shopfront volunteers by providing their services onsite. Others have facilitated access for AMS Redfern patients in their rooms by a commitment to bulkbilling and by providing urgent services at the request of AMS Redfern GPs.
Table 2. Organisations collaborating with AMS Redfern
Prince of Wales Hospital
- Ear, nose and throat and ophthalmology registrar clinic at AMS Redfern
Hearing Australia
- Audiology/hearing aid clinic at AMS Redfern
International Centre for Eye Education
- Optometry clinic at AMS Redfern
Royal Prince Alfred Hospital (Sydney Local Health District)
- Visiting specialist clinics at AMS Redfern including psychiatrist/clinical nurse consultant, liver and drug and alcohol, gynaecologist/obstetrician and cardiologist/ interventional cardiology
- Antenatal shared care
- Visiting podiatrist clinic at AMS Redfern
St Vincent's Hospital
- Visiting orthopaedic surgeon and physiotherapist at AMS Redfern
Sydney University Medical Faculty
- Medical student placements
University of Technology Sydney Nursing Faculty
- Nursing student placements
GP Synergy
- General practice registrar terms and short term placements
- Workshops on Aboriginal health
BreastScreen NSW
|
The services
At AMS Redfern, nurses and AHWs work alongside GPs to provide coordinated care, particularly in critical target areas, including:
- cervical screening. Reports suggest that 20–64% of Aboriginal and Torres Strait Islander women have never had cervical screening.8 In addition, the mortality rate from cervical cancer among Aboriginal and Torres Strait Islander women is estimated to be 4–5 times that of the national average.9 At AMS Redfern, a women's health nurse conducts Pap smears, maintains a recall system and coordinates follow up care with a visiting female gynaecologist who conducts colposcopies on site
- type 2 diabetes. Type 2 diabetes is approximately five times more common in Aboriginal and Torres Strait Islander people compared to the rest of the Australian population.10 This illness and its cardiac complications are particularly prevalent in Indigenous patients over 50 years of age attending AMS Redfern (Table 3). The service has established a multidisciplinary clinic with all patients reviewed first by a diabetes educator and GP and then onsite referrals for the eye clinic and podiatrist. An AHW assists in organising appointments, follow up, transport and basic monitoring for the patients. The service has a close working relationship with the Royal Prince Alfred Hospital (RPA) diabetes clinic, which expedites endocrine review of poorly controlled patients
- Mental health. Twenty-seven percent of Aboriginal and Torres Strait Islander adults have been reported as experiencing high or very high levels of psychological distress.10 This is double that experienced in the non Indigenous community. The AMS Redfern's mental health program is coordinated by a senior AHW with postgraduate training in mental health, and has both male and female visiting psychiatrists, a clinical nurse consultant and a psychologist. Having multidisciplinary services onsite facilitates genuine shared care and appropriate continuity from the hospital to the community
- Drugs and alcohol. A separate drug and alcohol unit was established in 1999, staffed by AHWs, AMS Redfern GPs and clinical nurse consultants with mental health and drug and alcohol training. The unit provides education, counselling, narcotic replacement pharmacotherapy and assistance with rehabilitation. In partnership with the RPA, an onsite liver clinic now runs fortnightly where patients can be assessed for hepatitis C treatment.
Table 3. Number of patients aged over 50 years with type 2 diabetes and cardiovascular disease attending AMS Redfern in 2012
| Diagnosis | Number of patients | Percentage of patients aged over 50 years |
|---|
| Type 2 diabetes |
312 |
28% |
| Cardiovascular disease |
486 |
43.6% |
| Type 2 diabetes and cardiovascular disease |
249 |
22.4% |
| Total patients aged over 50 years |
1114 |
100% |
The AMS Redfern has a proud history of creative health promotion programs including the World Health Organization awarded 'U Me & HIV' videos, the Koori Line Dance Troupe, the youth surfing program, the Elders pottery group, the men's group and walking groups (Figure 3). Programs supporting healthy lifestyle such as smoking cessation and fruit and vegetable boxes for needy families are all part of the AMS Redfern's extended service.

Figure 3. Health promotion program poster
Recognising the gap in urban Aboriginal research, the service is currently involved in a retrospective cohort study of all cause and cause specific mortality among Aboriginal and Torres Strait Islander patients attending the service from 1971 to 2008. The service is also a partner in the Kanyini vascular collaboration11 (www.kvc.org.au), which is testing whether improved outcomes for heart disease can be achieved by using a polypill rather than multiple dose tailored medications.
Improving access in mainstream general practice
While some Aboriginal and Torres Strait Islander patients prefer to attend ACCHSs, many visit mainstream general practices. The following strategies to improve access to primary care services in this population apply to any primary care setting. Mainstream general practices may like to consider and adapt some of these strategies to better meet the needs of Indigenous patients in their community.
- Sensitively ask all patients about Aboriginal and Torres Strait Islander status and record this on all patients records12
- Regularly update contact details – Aboriginal and Torres Strait Islander patients may move frequently and travel regularly between the bush and the city. While most patients have mobile telephones, the numbers may also change frequently
- Employ Aboriginal staff – this helps to make the practice culturally welcoming and helps close the employment gap
- Develop a referral list of specialists prepared to bulk-bill Aboriginal patients and negotiate a similar arrangement with pathology and radiology
- Be opportunistic in screening – nonfasting blood results can be better than no blood results
- If you have a sufficient number of Aboriginal and Torres Strait Islander patients, invite specialists to run clinics at your practice at appropriate intervals
- Undertake cultural awareness training and register for the Indigenous Practice Incentive Program – as well as annual health checks, your patients will also be eligible for the pharmaceutical co-payment measure, reducing their out-of-pocket expenses on Pharmaceutical Benefits Scheme medicines (see Resources).
Resources
Conflict of interest: none declared.
Acknowledgements
We would like to thank Dr Naomi Mayers and Dr Kate Burgess for assistance with the historical information referred to in this article.