The oral glucose tolerance test (OGTT) is currently the gold standard for the diagnosis of diabetes. The recommended preparation for and administration of the OGTT are important to ensure that test results are not affected. Interpretation is based on venous plasma glucose results before and 2 hours after a 75 g oral glucose load.
When should an OGTT be ordered?
The Royal Australian College of General Practitioners (RACGP) recommends an OGTT when the results of fasting or random blood glucose are equivocal (Figure 1): fasting 5.5–6.9; random 5.5–11.0 mmol/L.1 An OGTT is unnecessary if fasting or random blood glucose values are clearly in the nondiabetic or diabetic range: fasting or random <5.5; fasting ≥7.0 or random ≥11.1 mmol/L respectively. Diagnosis should be based on laboratory results, not results from a benchtop glucose meter.
The Australasian Diabetes in Pregnancy Society recommends a 50 or 75 g glucose challenge at 26–28 weeks in all pregnant women. An OGTT should be performed if the test result is abnormal: 1 hour values after a 50 or 75 g glucose challenge exceeding 7.8 or 8.0 mmol/L respectively.
If a woman has had gestational diabetes, a repeat OGTT is recommended at 6–8 weeks and 12 weeks after delivery. If the results are normal, repeat testing is recommended between 1 and 3 years depending on the clinical circumstances.1
There is a recent Australian recommendation to screen all women with polycystic ovarian syndrome for type 2 diabetes using an OGTT.2
It is also recommended that after a diagnosis of prediabetes (impaired fasting glucose or impaired glucose tolerance), the OGTT should be repeated after a year, and then subsequently based on the individual situation.3
What do I tell my patient?
The OGTT results can be affected by carbohydrate intake and duration of fasting preceding the test, the time of day the test is performed and carbohydrate intake or activity during the test.4–6 During the 3 days preceding the OGTT, 150 g of carbohydrate should be eaten (approximately ten 40 g slices of bread per day). The person being tested should then fast overnight except for water (eg. from 22:00 hours) and should not smoke or consume caffeine containing drinks, such as coffee. The OGTT is usually scheduled in the morning (eg. 09:00 }1 hour) and lasts for 2 hours. The test is preceded by venesection before the glucose load and followed by a second venesection 2 hours after the consumption of a drink containing 75 g of glucose. In children, a glucose load of 1.75 g/kg of body weight up to 75 g is used. (Some laboratories also perform a third venesection at 1 hour, although the result of this test does not contribute to the interpretation of the OGTT.) During the test no carbohydrate should be consumed and the person should remain seated throughout the 2 hours of the test. After the test is completed, the patient's usual lifestyle can be resumed. Both blood samples should be kept in fluoride-containing collection tubes.
There is a Medicare Benefits Schedule item for an OGTT, but patients should check with the pathology provider about any out-of-pocket costs.
How does the test work?
Blood glucose values reflect the balance between carbohydrate absorbed from the gut, hepatic glucose output/uptake and peripheral glucose uptake (largely muscle). Assuming the person is fasting beforehand and rests during the test, blood glucose values reflect the hepatic glucose output before the test (the fasting value) and the combination of the glucose load and any hepatic glucose output during the test (the 2 hour value). The fasting and 2 hour blood glucose values associated with the onset of the specific microvascular complications of diabetes (retinopathy, nephropathy and neuropathy) and macrovascular complications (atherosclerotic vascular disease) have been identified and these values are used as the diagnostic levels for the absence of diabetes and the presence of diabetes or prediabetes.
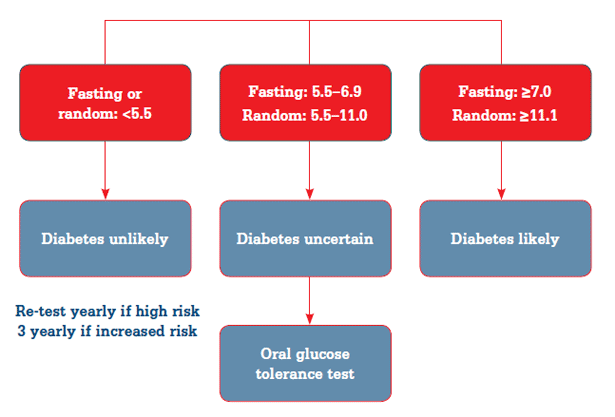
Figure 1. The RACGP recommendations for when to perform an OGTT1
What do the results mean?
Interpretation is based on the fasting and 2 hour plasma glucose values after the 75 g glucose load (mmol/L, Table 1). Prediabetes is diagnosed if the fasting or the 2 hour (} fasting) values are in the prediabetes range: impaired fasting glucose (IFG) and impaired glucose tolerance (IGT) respectively. Diabetes is diagnosed if the fasting and/or 2 hour values exceed 7.0 or 11.1 mmol/L in the presence of symptoms typical of diabetes. In the absence of symptoms a second abnormal blood test on a separate day is required.
When the OGTT is performed during pregnancy (eg. at 26–28 weeks following a positive oral glucose challenge) the criteria for overt diabetes is the same but the criteria for gestational diabetes are different: fasting 5.5–6.9 and 2 hour 8.0–11.0 mmol/L.1
Table 1. Interpretation of OGTT
| |
Fasting |
2 hour |
Implications |
| No diabetes |
≤6. |
<7.8 |
No excess micro- nor macro-vascular risk |
| Prediabetes |
6.1–6.9 |
7.8–11.0 |
Excess macro- but not micro-vascular risk |
| Diabetes |
≥7.0 |
≥11.1 |
Excess macro- and micro-vascular risk |
What won't the results tell you?
The OGTT results will not indicate whether the preparation for and administration of the test was correctly carried out. The OGTT assesses glucose tolerance at the time of the test. Results will only give a qualitative idea of the 24 average blood glucose and HbA1c (ie. normal, high, very high) and will not differentiate between type 1 and type 2 diabetes. Nor will they predict response to hypoglycaemic therapy or the current or future risk of diabetes complications.
What if the OGTT is unreliable?
Repeating the OGTT because results are potentially incorrect may be considered in at least two circumstances:
- marginally abnormal results and potential for incorrect preparation for and/or administration of the test (eg. as suggested from patient recall of the test)
- marginally abnormal results and major implications of abnormality for the person's future life (eg. loss of job; difficulties obtaining insurance).
Results of the OGTT are variable within the same individual with co-efficients of variation (CV: standard deviation ÷ average value as %) of approximately 8% and 20% for fasting and 2 hour values respectively.7 This means that in 20% of repeat tests compared to the original values, fasting values will be at least 13% higher or 13% lower and 2 hour values will be at least 33% higher or 33% lower. The sensitivity of the test to incorrect preparation or administration and the high intra-individual variability make the gold standard for diabetes diagnosis less than perfectly reliable.
Future directions in diabetes diagnosis
The American Diabetes Association recommends HbA1c as well as venous plasma glucose levels to diagnose type 2 diabetes with diagnostic values of HbA1c ≥6.5%. Authorities are considering accepting and implementing this recommendation during Australia in 2012–13.
The criteria for the diagnosis of gestational diabetes are currently under review following recommendations by an international committee that recommends criteria based on the fasting 5.1–6.9, 1 hour >10 and 2 hour values 8.5–11.0 mmol/L.8 These criteria have been adopted by the American Diabetes Association9 and some Australian hospitals.
The following case study illustrates the interpretation of OGTT results.
Case study – Peter
- 53 years of age; body mass index (BMI) 29.4 kg/m2; mother with type 2 diabetes
- Reason for OGTT: high risk of type 2 diabetes (age, familial hypercholesterolaemia, overweight) and fasting glucose level 5.8 mmol/L
- OGTT results: fasting 6.6, 2 hours 7.6 mmol/L.
Interpretation: Prediabetes. Highly likely to develop type 2 diabetes and to have other components of the metabolic syndrome (hypertension, dyslipidaemia, increased risk of atherosclerotic disease).
Conflict of interest: none declared.