Case 1
Nadia Khallil
Nadia, 78 years of age, has spilt hot tea on her right thigh. She has run cold water over her leg for 20 minutes. You determine she has a superficial dermal burn on 2% of her total body surface area.
Question 1
Which of the following is suggestive of a superficial dermal burn:
- white, waxy skin that is very painful to touch
- skin that blanches to pressure but has sluggish capillary refill
- skin that is very painful to touch and blanches to pressure
- skin that is red and dry, and somewhat painful to touch
- rapid formation of blisters on the skin with decreased sensation.
Question 2
In addition to providing analgesia, how will you manage the wound today:
- dressing with silver sulfadiazine cream and gauze
- dressing with nonadherent occlusive dressing and 5 days of oral antibiotics
- dressing with topical antibiotic and nonadherent occlusive dressing
- dressing with paraffin gauze alone
- dressing with hydrogels and nonadherent occlusive dressing.
Question 3
Nadia returns in 48 hours for review. The wound looks clean and dry. There are two 5 mm intact blisters present. The area is still painful. How will you manage the wound:
- sterile debridement of blisters followed by paraffin gauze dressing
- sterile debridement of blisters followed by hydrocolloid dressing
- leave the blisters intact and dress with silver sulfadiazine cream and gauze
- leave the blisters intact and dress with hydrogels and occlusive dressing
- leave the blisters intact and dress with occlusive dressing alone.
Question 4
Nadia returns 7 days later. She reports that her right thigh appears more swollen than the left although she has been careful to continue her usual activities. On inspection, the wound looks clean and dry, though still not healed. What is the most appropriate management:
- swab the wound and commence the appropriate oral antibiotics
- swelling from burn: encourage strict bed rest until it subsides
- swelling from burn: apply supportive tubular bandages to reduce swelling
- commence broad-spectrum oral antibiotics to cover for infection
- change to silver based dressings and apply tubular bandages.
Case 2
Ezra Tafua
You are one of two team doctors at an U-19 rugby match in a rural town. There is a sudden commotion on the field. You note that Ezra, 17 years of age, is on the ground and his teammate, Paul, has started chest compressions. Your colleague has run to get the emergency medical pack.
Question 5
How can you ensure that Ezra has the best basic life support until your colleague returns:
- pause CPR so that you can rapidly assess Ezra's pulse and breathing
- take over CPR, as doctors perform more effective compressions
- encourage Paul to pause CPR to deliver two breaths
- encourage Paul to continue chest compressions without pausing
- encourage Paul to continue CPR at a rate 30 compressions: one breath.
Question 6
Your colleague arrives with the semi-automatic defibrillator and medical pack and informs you that the ambulance is 30 minutes away. The defibrillator trace shows pulseless electrical activity. What will you do next:
- resume CPR immediately for 2 minutes
- deliver 1 mg of IM adrenaline rapidly in the next 2 minutes
- pause CPR so that you can obtain IV access in the next 2 minutes
- deliver atropine 0.2 mg IM rapidly in the next 2 minutes
- reset the defibrillator to obtain another trace in the next 2 minutes.
Question 7
Four minutes after the above event, the defibrillator records ventricular fibrillation and Ezra is defibrillated twice. IV access has been obtained. What will you do next:
- continue CPR for 2 minutes with a new team member
- deliver 1 mg of IV adrenaline rapidly with 100 mL fluid push
- C. deliver 300 mg of IV amiodarone with 100 mL fluid push
- halt CPR to assess Ezra's pulse and breathing
- insert LMA to assist effective ventilation.
Question 8
Six minutes after Ezra collapsed, resuscitation is ceased as Ezra has been restored to spontaneous circulation and ventilation. He received three defibrillations in total. Which of the following is NOT in keeping with best management practices:
- aim for a normal BSL of 4.0–6.0
- cool Ezra with bags of cold saline
- deliver 300 mg of IV amiodarone with 100 mL fluid push if not given earlier
- commence thrombolysis protocol
- give oxygen to Ezra via face mask.
Case 3
Benjamin Withers
Benjamin, aged 18 months, is brought to you for urgent review. Ellen, his mother, is worried because he ingested crushed peanuts 30 minutes ago for the first time, and was then noted to have a rash. You examine him rapidly and note that Benjamin is alert and well perfused, with a normal ENT and respiratory examination. The rash is erythematous, covering the flexures of the elbows and the knees. Benjamin had several episodes of bronchiolitis last year.
Question 9
What is the most likely diagnosis:
- peanut allergy
- asthma
- eczema
- anaphylaxis
- postviral rash.
Question 10
Two weeks later Benjamin is again brought to you for urgent review. Ellen is worried because he has become progressively pale and floppy, with swollen lips, noisy breathing and an urticarial rash over the trunk in the past 30 minutes. Benjamin was discovered in the laundry. What is your first management step:
- give adrenaline 1:1000 at a dose of 0.01 mg/kg to the lateral thigh
- give adrenaline 1:1000 at a dose of 0.5 mg to the lateral thigh
- give adrenaline 1:10 000 at a dose of 0.01 mg/kg to the lateral thigh
- give adrenaline via nebuliser mask and oxygen pump
- commence CPR at a rate of 30 compressions: 2 breaths.
Question 11
Benjamin is still pale and floppy, although his breathing is no longer noisy. He is normotensive and bradycardic, and you note his tongue is swollen. It has been 7 minutes since he first presented. You have obtained IV access. What will you do next:
- IM adrenaline to the lateral thigh
- IM antihistamine to the lateral thigh
- IV N/saline bolus 20 mL/kg stat
- IV atropine at 0.01 mg/kg stat
- IV adrenaline infusion.
Question 12
Benjamin is transferred to a tertiary hospital for stabilisation and observation. He makes an excellent recovery and returns home within the week. When would you consider prescription of an adrenaline autoinjector:
- conclusive serial mast cell tryptase measurements
- identification of trigger with the help of a clinical immunologist
- it should be routinely prescribed after an anaphylactic event
- confirmation by raised IgE levels and positive skin prick testing
- in cases where there is risk of accidental exposure to the trigger.
Case 4
Clarence Wong
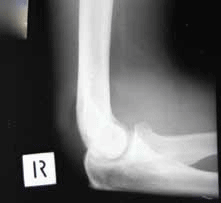
Clarence, 19 years of age, presents following a high impact fall onto both outstretched hands while mountain-biking. He complains of pain and restricted movement in the right elbow. You request plain films of the elbow.
Question 13
Which of the following is NOT part of a structured interpretation of X-rays of the extremities:
- ensure imaging is of the correct patient
- ensure at least one view is well-exposed
- check fat pads around joints
- check all cortical lines
- check margins of image for occult fractures.
Question 14
Is the X-ray shown normal:
- yes: the anterior and posterior fat pads are present, and cortices intact
- yes: but an orthogonal view is required to confirm this
- no: there is cortical disruption to the radial head
- no: there is elevation of the anterior and posterior fat pads
- yes: the anterior and posterior fat pad elevation is an anatomical variation.
Question 15
How will you manage the painful right elbow:
- immobilise in backslab and sling; urgent orthopaedic review required
- immobilise in backslab and sling for a few days and then review
- encourage immediate mobilisation, using analgesics for pain relief
- compression bandaging to reduce fat pads; using analgesics for pain relief
- immobilise in backslab and sling; request CT elbow if still painful in a week.
Questions 16
Clarence returns 10 days later with tenderness in the left anatomical snuffbox, slowly worsening after the mountain-biking accident. X-ray of the wrist indicates a healing undisplaced fracture of the scaphoid tubercle. Which of the following is true:
- a CT wrist is also indicated to assess for ligament injury
- place the left hand in a thumb abduction cast for 10 days
- two simultaneous fracture sites raises suspicion of osteoporosis
- orthopaedic review is indicated to assess for ligament injury
- scaphoid fractures are at high risk of nonunion and avascular necrosis.