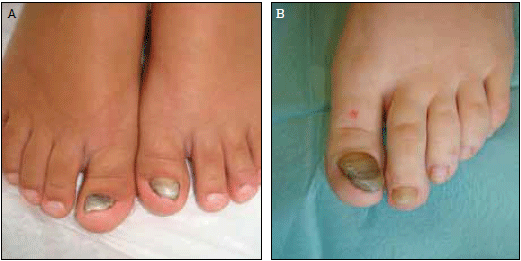
Figure 1 and 2. Clinical appearance of the patients' great toenails
Question 1
What is the diagnosis?
Question 2
How would you diagnose this disease?
Question 3
What differential diagnoses would you consider?
Question 4
What are the main complications of this condition?
Question 5
What is the expected clinical course of the disease?
Question 6
What is the management strategy?
Answer 1
Based on the clinical appearance, the presence of nail deformity since birth or early childhood and the absence of response to previous treatments, the diagnosis of congenital malalignment of the great toenails (CMGTN) is likely. Congenital malalignment of the great toenails is not uncommon and is probably inherited with an autosomal dominant gene of variable expression.1 It is possibly caused by an abnormality in the ligament that connects the nail matrix to the periosteum of the distal phalanx.
The defining characteristic of this condition is the lateral deviation of the long axis of the nail plate with respect to the long axis of the distal phalanx of the hallux.1–3 The severity of the malalignment may vary. A medial deviation of the great toenail plate has been described, although it seems a rare event. The disorder may involve one or both feet and is typically present at birth. While it usually involves the great toenails, other toenails or fingernails are rarely affected.2
Answer 2
The clinical appearance of the great toenails, together with knowledge that the condition was present at birth, usually establishes the diagnosis.2 In addition to lateral deviation of the long axis of the nail plate, other typical findings encompass:
- congenital or early acquired hypertrophy of the lateral nail folds
- shortening or thickening of the nail plate
- greyish to brown discoloration of the nail and, if persisting into adulthood, development of a greenish hue
- transverse ridging in the form of a single or multiple nail ridges that give the nail the appearance of an 'oyster shell'
- triangular shape
- onycholysis (separation from the nail bed), especially in adult patients
- transverse overcurvature
- slower growth rate of the nail plate.1,2
A culture is required to rule out onychomycosis. While the diagnosis is clinical, an X‐ray of the toes with a technique that displays an overlap of the nail plate and the bone structures of the terminal phalanx of the hallux can further help to determine the malalignment.2
Answer 3
It is important to recognise CMGTN as several nail disorders can occur concurrently with and/or clinically mimic it.3 The list of possible differential diagnoses is long and, depending on the particular clinical picture, includes: onychomycosis, eczema, psoriasis, paronychia congenita, Hallopeau acrodermatitis, Darier disease, dyskeratosis congenita, acrodermatitis enteropathica, neuropathies, connective tissue diseases, tumours involving the nail region and congenital conditions that are also associated with increased risk of developing ingrown toenails, such as congenital ingrown toenails of the hallux, inherited overcurvature of the nails and congenital hypertrophy of the nail folds of the hallux.2 Congenital malalignment of the great toenails should also be differentiated from traumatic and iatrogenic (eg. a consequence of surgical intervention or wide lateral nail biopsy) malalignment of the nail plate.
Answer 4
In addition to aesthetics, the most important complication of CMGTN is ingrown toenail (onychocryptosis), ie. embedding of the malaligned nail plate into the lateral nail fold with accompanying inflammation, bacterial or candidal paronychia, dermatophytic or candidal onychomycosis, significant onycholysis and progressive onychogryphosis (hypertrophy and curving) that interferes with footwear and may cause inflammation and pain.1–4
Answer 5
In approximately 50% of patients, especially those with mild disease, satisfactory spontaneous improvement during childhood may occur, which leads to an almost normal appearance. In these cases, realignment is almost complete before the age of 10 years, with most spontaneously realigning by the age of 6 years.1,2,4 In others, the malformation may persist into adulthood to such a degree that it substantially restricts the everyday activities of the patient.2
Answer 6
Management of CMGTN depends on accurate assessment of the degree of malalignment, the associated changes and their course.2 As a result of possible spontaneous improvement, surgery may be delayed and regular follow up with photographic documentation of the course of the deviation is recommended to allow for such improvement. If there is no improvement by the age of 2 years, surgery should be considered.2,4 In practice, management of CMGTN varies according to severity and can include:
- if the deviation is mild (and therefore with the potential for gradual spontaneous resolution), treatment should be conservative. As the nail hardens with age it may overcome the slight distal embedding2,4
- if the deviation is moderate and the lateral horn of the matrix is bulging, phenolisation (destruction of the nail bed by use of concentrated phenol) of the latter is the best option. The nail will remain malaligned but the painful bulge will disappear2,4
- if the deviation is moderate to severe, and the child is aged less than 2 years, surgical correction is essential to prevent permanent nail dystrophy and complications. This consists of a realignment of the whole nail apparatus (nail rotation) and produces good results. When performed at a later age, improvement is more functional than cosmetic, which allows patients to wear almost any type of footwear. The surgical result is a short, narrow and thin nail that does not adhere to the epithelialised nail bed. However, this is more cosmetically acceptable and patients may use acrylic nails.2,4
Summary
Although CMGTN is a common condition it is often misdiagnosed, most commonly as onychomycosis, and treated with oral antifungals without any benefit. Physicians should be aware of this diagnosis, especially in patients with isolated unilateral or bilateral toenail deformity present from birth.
Conflict of interest: none declared.