Case study 2
Mr RC, 84 years of age, presented to the emergency department with a painful, red right eye of 24 hours duration associated with decreased vision. He had received an intravitreal injection of ranibizumab, an antivascular endothelial growth factor (VEGF), 3 days earlier for the treatment of wet age related macular degeneration (AMD). He had received four ranibizumab injections over the previous 6 months. His vision had stabilised at 6/18 in the right eye with the injections prior to the acute deterioration. On examination right visual acuity was reduced to nil perception of light. There was significant periorbital swelling and chemosis of the conjunctiva (conjunctival swelling). Slit lamp examination demonstrated evidence of severe intra-ocular infection with a secondary corneal perforation (Figure 3). The patient was admitted to hospital and treated with intravenous antibiotics. Due to the corneal perforation and severe infection, the eye was deemed nonsalvageable and required removal of intra-ocular contents.
Discussion
Endophthalmitis refers to inflammation of two or more adjacent coats of the eye, and is most commonly secondary to microbial infection. Infective endophthalmitis may be exogenous (eg. following surgery or trauma) or endogenous (spread haematologically from a distant site, often in an immunocompromised patient). Acute infective exogenous endophthalmitis is an ophthalmic emergency that requires immediate assessment and treatment within hours of presentation. There is often a guarded visual prognosis.
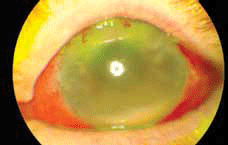
Figure 1. Inferior hypopyon (pus in the anterior chamber). The cornea is hazy from inflammation. There is conjunctival injection and subconjunctival haemorrhage following the intravitreal antibiotic injections
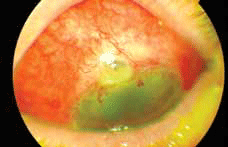
Figure 2. Infected trabeculectomy bleb at the superior limbus. Note the avascular cystic elevated area with white infiltrate
It is important that primary care physicians are aware of this sight-threatening intra-ocular infection and are able to distinguish it from less serious pathology. Immediate injection of intravitreal antibiotics by an ophthalmologist is crucial in influencing the long term visual outcome. A history of recent eye surgery, intravitreal injection, trauma or previous glaucoma surgery should be sought, and if present should raise the index of suspicion. While it is common practice for surgeons to provide contact numbers and emergency department details for patients when they are in the postoperative phase of their care, as trabeculectomy surgery carries with it a lifelong risk of endophthalmitis a patient may well present to their general practitioner months or years later thinking this is as an unrelated event. Signs and symptoms of acute infective exogenous endophthalmitis are shown in Table 1.
Table 1. Common symptoms and signs of acute infective exogenous endophthalmitis
| Symptoms | Signs |
|---|
- Visual blurring or loss
- Pain
- Purulent discharge
|
- Decreased visual acuity
- Decreased red reflex
- Eyelid oedema
- Conjunctival injection and chemosis
- Anterior chamber cells
- Hypopyon (pus in anterior chamber)
- Vitreous cells
|
Most cases of endophthalmitis are bacterial, although viral and fungal cases also occur. Common causative organisms include coagulase negative staphylococci (70%), Staphylococcus aureus (9.9%), Streptococcus species (9.0%), and Gram negative organisms (5.9%).1
The mainstay of endophthalmitis treatment is immediate vitreous sampling for microbiological analysis, followed by intravitreal injection of broad spectrum antibiotics. The method of intravitreal injection is demonstrated in Figure 4. Vitrectomy surgery or repeat intravitreal antibiotics may be necessary in severe cases.
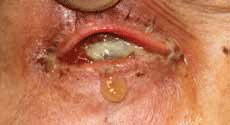
Figure 3. Severe intra-ocular infection and corneal perforation following intravitreal ranibizumab injection
Exogenous endophthalmitis following cataract surgery is the most common cause of acute endophthalmitis in Australia, and usually presents within a few days of the initial operation. The cases presented in this article highlight two other important, but less well known, causes of acute exogenous endophthalmitis.
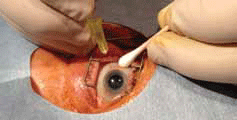
Figure 4. Method of intravitreal injection. A speculum is inserted. Most commonly performed with topical (+/- subconjunctival) anaesthetic
A trabeculectomy is a glaucoma surgical procedure that aims to lower intra-ocular pressure through the creation of a fistula that allows aqueous fluid to drain from the anterior chamber to the sub-Tenon's space. In successful surgery, an elevated area known as a 'bleb' is formed, usually under the upper eyelid, which contains fluid drained from the anterior chamber.
In recent years there has been more frequent use of intra-operative antimetabolites such as mitomycin-C and 5-fluorouracil during glaucoma surgery to reduce unwanted scar formation and bleb failure. As a consequence there is an increased risk of bleb leaks months to years after the initial surgery.2 This may result in a bleb infection ('blebitis') or endophthalmitis. It has been estimated the incidence of late postoperative bleb related infections after trabeculectomy is 0.4% to 6.9%.3
The use of intravitreal injections for the treatment of ocular conditions is becoming increasingly common. The introduction of anti-VEGF treatment such as ranibizumab has revolutionised the treatment of neovascular (wet) AMD. The risk of intra-ocular infection with intravitreal injection is small, with an estimated risk around 0.05%.4 Nevertheless, prompt recognition and treatment is crucial for the long term visual prognosis.
Summary
- Endophthalmitis is a potentially sight threatening intra-ocular infection.
- Prompt empirical intravitreal antibiotics are imperative.
- Previous eye surgery is a red flag in the assessment of a patient with a painful red eye. Ask specifically for a history of intravitreal injections or glaucoma surgery – blinding infection can occur years after the initial operation.
- GPs should be familiar with the signs and symptoms of acute infective endophthalmitis, and refer these patients immediately for specialist review and management.
Conflict of interest: none declared.