Discussion
Figure 1 shows a Monteggia fracture: a displaced fracture of the proximal ulna (short arrow) associated with dislocation of the radial head (long arrow). This case illustrates the principle that where one forearm bone is fractured there is frequently either a second fracture or a joint dislocation, therefore, it is important to always check the adjacent joints. This principle also applies in the axial skeleton. For example, in the mandible and pelvic ring where if one fracture is present, there is often an occult second fracture. The Monteggia fracture requires urgent orthopaedic management. It is important to check that the limb is neurovascularly intact. Table 1 contains a checklist for interpreting extremity X-rays. An undisplaced fracture of the upper extremity is often visible on only one view: the clinician should ensure that there are two views taken in orthogonal planes. Frequently missed fracture sites include scaphoid, triquetrum and proximal forearm.
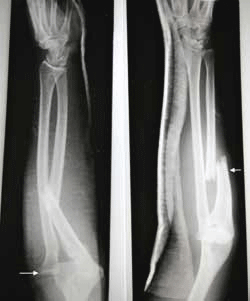
Figure 1. X-ray of the patient's forearm
Table 1. Checklist for interpreting extremity X–rays
- Correct patient?
- Minimum of two views that are orthogonal (ie. at a right angle from one another)?
- Fat pads – are they distorted?
- Cortices – are they intact?
- Margins of image – is another fracture or dislocation present (eg. in a forearm X-ray always check the proximal forearm and carpal bones)?
|
Case study 2
A woman, 30 years of age, has exquisite focal tenderness in the anatomical snuffbox following a fall. Her wrist X-ray is shown in Figure 2.
Discussion
Figure 2 shows an undisplaced, uncomplicated fracture of the scaphoid tubercle. The usual mechanism of injury in the setting of a scaphoid fracture is a fall onto the outstretched hand with an extended and radially deviated wrist. Scaphoid fractures are at high risk of nonunion and avascular necrosis due to limited blood supply.1 Up to a third of patients with clinical suspicion of a fracture of the scaphoid will have a normal initial X-ray.1 Standard management is immobilisation in a thumb abduction cast for 10 days and follow up X-ray, but increasingly advanced imaging is used to avoid overtreatment in adults. Children can usually be treated in immobilisation with follow up plain X-ray imaging. Computed tomography (CT), bone scan and magnetic resonance imaging (MRI) are all equally sensitive but CT is emerging as the preferred option due to greater availability compared to MRI and lower radiation dose compared to nuclear medicine.2 Elite athletes requiring guidance about training should preferably be imaged with MRI. In more severe injuries the scapholunate ligament can be disrupted resulting in scapholunate dissociation. In extreme cases, rupture of both the intrinsic and extrinsic wrist ligaments can occur and this can result in carpal bone dislocation. Figure 3 shows a transscaphoid perilunate dislocation: the antero-posterior (AP) view shows a fracture of the scaphoid waist, and the lateral view shows an anterior dislocation of the lunate (long arrow) from the capitate (short arrows) – this is an othopaedic emergency.
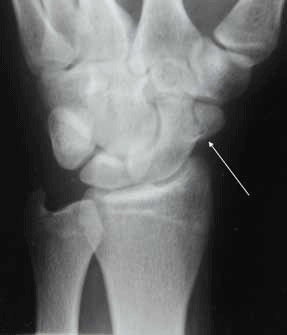
Figure 2. X-ray of the patient's wrist
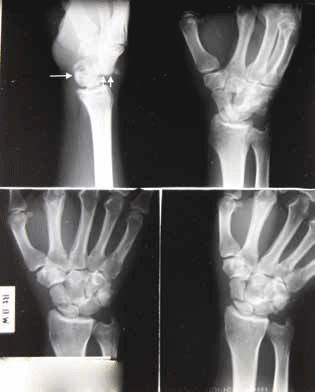
Figure 3. Wrist X-ray in a different patient
Case study 3
A man, 20 years of age, presents following a fall onto his outstretched hand with pain in the elbow and restricted range of motion. His elbow X-ray is shown in Figure 4.
Discussion
Figure 4 is a lateral elbow view showing elevation of the anterior fat pad (the 'sail' sign – double arrows), and posterior fat pad (single arrow). The elbow fat pads lie in the ventral and dorsal concavities of the distal humerus. The anterior fat pad is normally just visible but when the joint space fills with fluid or blood it becomes elevated like a boat sail. The posterior fat pad is not usually seen. When these fat pads are distorted this reflects an effusion or haemarthrosis and a fracture should be presumed until proven otherwise.
R adial head fractures are the most common injury in adults following a fall on the outstretched hand and are often either occult or difficult to perceive on standard views. They occur as a result of compression of the radial head on the humeral capitellum in elbow flexion. Management of an undisplaced fracture of the radial head centres on pain control with a short period of immobilisation and early restoration of function.
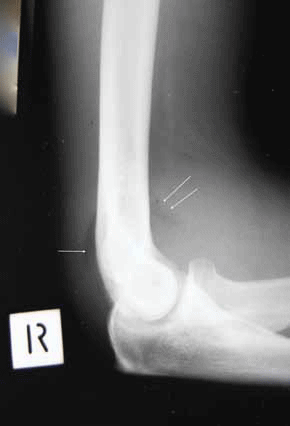
Figure 4. X-ray of the patient's elbow
Fat pads can be seen around the elbow and other joints because they are of a different density to other tissues. Density on plain X-ray reflects the relative attenuation of X-rays as they pass through the patient to reach the detector. Different tissues will result in different attenuation of the X-ray beam: bone attenuates most and is 'white' and soft tissues attenuate relatively less and are grey. Fat is closer in density to air than it is to muscle and therefore appears darker on the image.
Case study 4
A girl, 6 years of age, presents with pain and a deformed, swollen elbow after a fall while performing gymnastics. The neurovascular supply to her upper limb is intact. Her elbow X-ray is shown in Figure 5.
Discussion
Figure 5 shows a supracondylar humeral fracture with elevation of the anterior fat pad (arrowheads). An imaginary line drawn along the anterior cortex of the humerus should bisect the capitellum but in this case the distal fracture fragment is posteriorly angulated (arrow).
The supracondylar fracture is the most common elbow fracture in children and usually occurs due to an extension force. The most serious complication is the Volkmann contracture, which occurs as a result of a forearm compartment syndrome and subsequent muscle and nerve necrosis. Undisplaced supracondylar fractures with normal neurological and vascular supply can be managed in a flexion cast. Orthopaedic intervention is required where there is vascular compromise and for significantly displaced and/or angulated fractures. It is important to always check the neurological and vascular integrity distal to the fracture.
While in adults the weak point around joints is usually the tendons and ligaments, in children it is the growth plate. In supracondylar fractures, the growth plate can sometimes be affected. The Salter-Harris classification describes patterns of growth plate injury and guides management (see Resource). Type 2 is the most common (fracture through the growth plate and the metaphysis, sparing the epiphysis). Orthopaedic management may be required in some cases to ensure normal bone growth and avoid angular deformity.
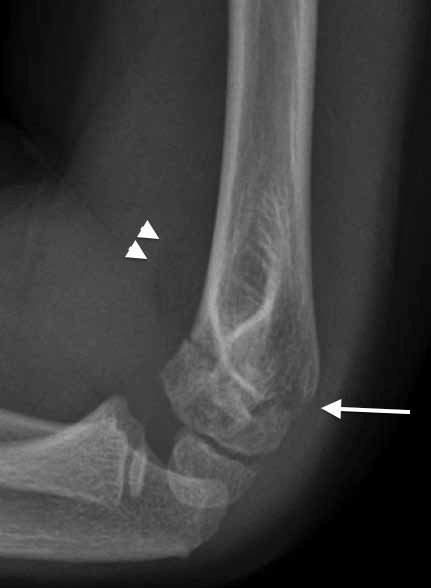
Figure 5. X-ray of the patient's elbow
Case study 5
A man who suffers from epilepsy is brought to the emergency department following a typical seizure. He is drowsy and unable to give a good history. His parents state that he is unable to move his left upper limb. His AP and lateral shoulder X-rays are shown in Figure 6 and Figure 7 respectively.
Discussion
Figure 6 and 7 show a posterior shoulder dislocation. In the AP view the distance between humeral head and glenoid is widened (double arrowhead) and the humeral head is shaped like a 'tennis racquet' due to internal rotation by the more powerful teres major and subscapularis. Irregularity of the medial aspect of the humeral head indicates an impaction fracture (the reverse Hill-Sachs lesion). In the lateral view, the humeral head marked by a ring lies posterior and inferior the marked 'Y' intersection of coracoid (posterior), acromion (anterior) and scapula body (inferior tail).
Evaluating shoulder joint alignment is easier when a structured approach is used. On the lateral view look for the 'Y' formed by the coracoid process anteriorly, the anterior acromion posteriorly and the body or blade of the scapula inferiorly. At least part of the humeral head must overlie the point of intersection of these structures but does not need to be perfectly centred on it.
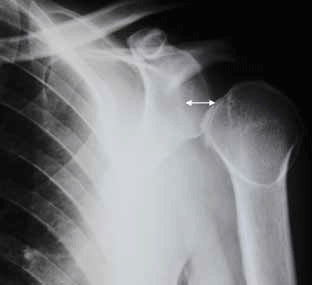
Figure 6. AP view of the patient's shoulder
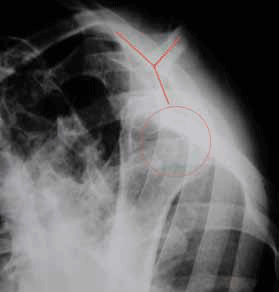
Figure 7. Lateral view of the patient's shoulder
The more common anterior dislocation (Figure 8) can be diagnosed on the AP projection. In this image the dislocated humeral head (asterisk) overlies the inferior aspect of the glenoid (white oval). There may be a compression fracture of the postero-superior humeral head (the Hill-Sachs fracture) and/or a fracture of the inferior margin of the glenoid (the bony Bankart fracture). These are often visible on postreduction views, which are an essential part of the management of shoulder dislocation.
Patients with anterior instability associated with repeated dislocations require orthopaedic review.
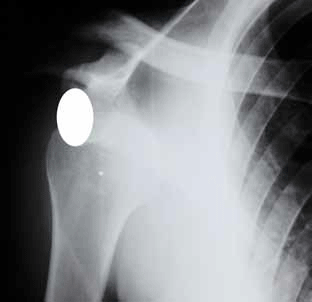
Figure 8. Shoulder X-ray in a different patient
Case study 6
A woman, 45 years of age, has severe shoulder pain without a history of recent injury. She awoke unable to move her arm and has markedly restricted abduction but relatively normal external rotation. Her shoulder X-ray is shown in Figure 9.
Discussion
Figure 9 shows calcific tendinosis, with two small calcifications visible in the rotator cuff superior to the humeral head. The larger calcification lies in supraspinatus. Calcific tendinosis is a common cause of nontraumatic shoulder pain. It occurs as part of a spectrum of rotator cuff lesions, which are thought to occur as a result of repetitive microtrauma of the cuff against the bony arch. An injection of local anaesthetic and steroid into the overlying subacromial-subdeltoid bursa, either by palpation or under ultrasound guidance, may be helpful to alleviate acute pain. Rarely, surgical removal of calcific tissue is required.
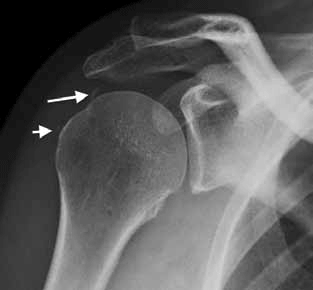
Figure 9. X-ray of the patient's shoulder
Case study 7
You are called by the local hospital nursing staff to clear the cervical spine of a middle aged man who has fallen from a ladder. He had a brief loss of consciousness after hitting his head and appears to be intoxicated. He also has an obviously fractured forearm. You decide to order a cervical spine plain X-ray series. His lateral cervical spine X-ray is shown in Figure 10.
Discussion
Figure 10 shows a lateral view of the cervical spine with a type 2 dens fracture (single vertical arrow), associated disrupted spinolaminar line (dotted arrow line) and posteriorly displaced anterior atlanto-axial joint (thin arrows).
The first task in a possible cervical spine injury is to decide whether or not to order imaging. The National Emergency X Radiography Utilization Study (NEXUS) was established to reduce unnecessary imaging in cervical trauma. It identified clinical criteria (Table 2), which, if associated with normal range of motion of at least 45 degrees to the right and left, indicate a very low probability of clinically significant injury to the cervical spine.3,4 Conversely, if any of the NEXUS criteria are present (in this case the patient is intoxicated and has a distracting injury), the patient must be adequately imaged to exclude cervical spine trauma.
Computed tomography is generally replacing plain X-ray imaging due to the higher incidence of missed injuries on X-ray, but GPs may be called to interpret 5-view plain radiography of the cervical spine at a site where CT is unavailable.5 A standard plain X-ray series includes lateral, odontoid peg, AP and oblique views taken with the patient immobilised.
When interpreting cervical spine X-rays, the first step is to look at the lateral view to establish that all seven cervical vertebrae have been included. Without this you can miss C7–T1 fracture dislocation, so a 'swimmer's' view and/or CT is required. Then look at the alignment of the anterior vertebral body line, posterior vertebral body line and spinolaminar line on the lateral view (the dotted line on Figure 10). These lines must be smooth/unbroken. In this case interruption of the spinolaminar line is the first clue to the diagnosis.
The normal precervical soft tissue space measures less than 7 mm at C2 and less than 2 cm at C7. Any widening of these spaces should alert you to the possibility of occult injury. The cervical spine series also includes a 'peg' view of C1/2 and AP view from skull base to C7. Check the base of the odontoid peg and that the lateral masses of C1 are in exact alignment with C2. Also the distance between the peg and C1 masses should be equal. On the AP view check spinous process alignment.
Remember that the major cause of 'missed' fractures is inadequate imaging rather than perceptual error. Any abnormality on plain X-ray should initiate further imaging with CT. If CT is normal but there is persistent midline tenderness, further imaging with MRI is appropriate to exclude disc and ligamentous injuries, which are more likely in patients with advanced spondylosis.5
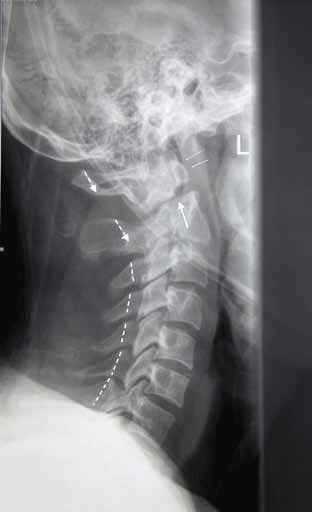
Figure 10. Lateral view of the patient's cervical spine
Table 2. Indications for imaging in cervical spine trauma (NEXUS criteria)4
- Midline cervical tenderness on palpation
- Focal neurological deficit (parasthesia, central cord syndrome, radiculopathy)
- Intoxication (alcohol, narcotic analgesic, other drugs)
- Painful distracting injury (long bone fracture, considerable burns, visceral injury)
- Altered mental status, ie. Glasgow Coma Scale (GCS) score <15
|
Case study 8
An elderly man presents after being found in a collapsed state at home. He is short of breath. Examination reveals fever and complete absence of breath sounds in the left hemithorax. His chest X-ray is shown in Figure 11.
Discussion
The AP chest X-ray in Figure 11 shows 'white out' of the left hemithorax due to a large pleural effusion. The dotted line shows the position of the trachea, which is deviated away from the opacity indicating a space occupying process. The differential diagnosis includes effusion, empyema, consolidation or mass. It is important to use a systematic approach when interpreting a chest X-ray. This can help avoid missing important clues to the diagnosis (Table 3).
Pulmonary infiltrates may be caused by:
- fluid, ie. effusion/empyema, pulmonary oedema, aspiration
- pus, ie. pneumonia, abscess
- cells, ie. carcinoma, metastasis, other neoplasm
- blood, ie. pulmonary haemorrhage.
'Fluffy' infiltrates suggest alveolar origin. If the mediastinum is shifted toward the opacity, this indicates volume loss (collapse).
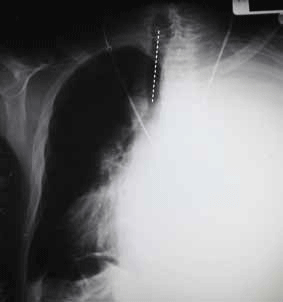
Figure 11. The patient's AP chest X-ray
Careful assessment of the cardiac silhouette will enable you to localise the site of collapse or consolidation. Figure 12 illustrates the common patterns of collapse on a chest X-ray. Persistent collapse or consolidation should raise suspicion of an obstructing lesion and requires further investigation with CT.
Table 3. Checklist for chest X-ray interpretation
Quality
- Name
- Rotation
- Side marker
Diaphragm
- Elevation
- Tenting
- Free/displaced air
Heart
- Size less than half thorax on a postero-anterior film
- Silhouette
|
Hila
Cardiophrenic angles
Lungs
- Infiltrates
- Air bronchograms
- Masses
- Vascularity
|
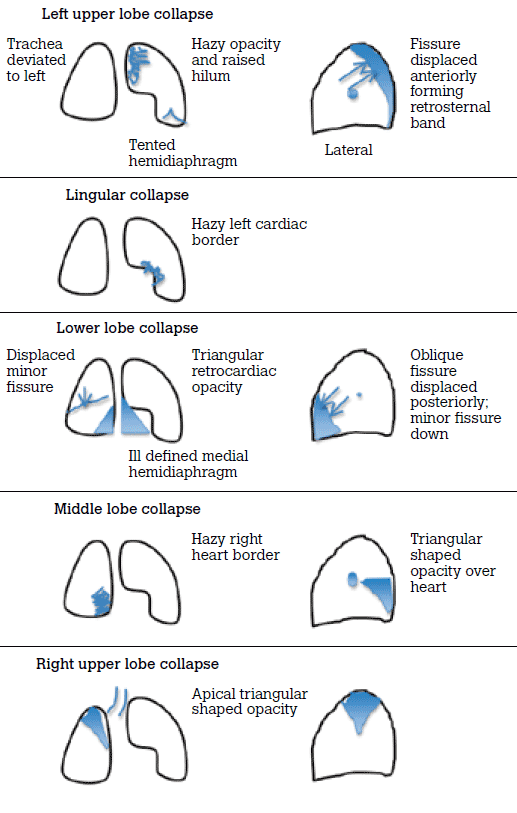
Figure 12. Patterns of collapse on a chest X-ray
Case study 9
A middle aged woman arrives at the surgery accompanied by her husband, who appears anxious. She has a past history of Crohn's disease and has had abdominal surgery on multiple occasions in the past. She has acute severe abdominal pain and is vomiting while in the waiting room. Her abdominal X-rays are shown in Figure 13 and Figure 14.
Discussion
The patient's abdominal X-rays show a small bowel obstruction. On the supine X-ray an arrow indicates the valvulae conniventes and multiple dilated loops (>3 cm diameter) are present (Figure 13). The erect X-ray shows multiple long air-fluid levels (arrows). Note the erect X-ray includes the hemidiaphragms and absence of free gas excludes a pneumoperitoneum (Figure 14).
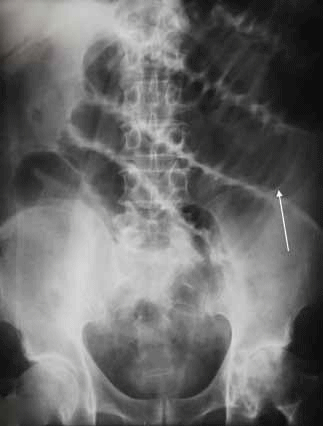
Figure 13. The patient's supine abdominal X-ray
Features of small bowel obstruction (SBO) include dilated small bowel loops and air fluid levels. The small bowel is centrally located and has valvulae conniventes (radiodense lines crossing the width of the loop representing mucosal folds). Small bowel loops over 3 cm in diameter suggest an SBO. This may be associated with reduced or absent colonic gas. Air fluid levels represent the interface between air and fluid in the bowel lumen. They are seen on the erect AP view or alternatively on lateral decubitus view if the patient is unable to stand; 3–4 air fluid levels in the distal small bowel are frequently seen in normal patients. More than this suggests an SBO. Length of air fluid level is no longer considered a reliable sign as it is variable in mechanical obstruction: a complete gasless obstruction and short air fluid levels arranged in a partial ring (the 'string of pearls' sign) are equally pathological. Dilated small bowel does not always indicate a mechanical obstruction: ileus can be caused by inflammation of underlying organs (eg. in acute pancreatitis).
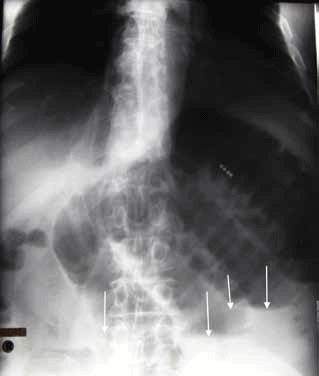
Figure 14. The patient's erect abdominal X-ray
The most common causes of SBO are adhesions (look for surgical clips), hernias (check physical examination and inguinal regions), tumour and strictures from Crohn disease. Remember to check under diaphragm on the erect film for a pneumoperitoneum.
Case study 10
Your local nursing home requests a visit to assess an elderly resident who has an obviously distended abdomen and a history of chronic constipation. The patient's supine abdominal X-ray is shown in Figure 15.
Discussion
Figure 15 is a supine abdominal X-ray showing large bowel obstruction secondary to sigmoid volvulus. The dotted line demarcates the wall of the grossly distended sigmoid colon extending superiorly from the pelvis in contrast to caecal volvulus, which arises from the right flank. Remember to exclude perforation either with an erect chest X-ray or lateral decubitus view where free air will rise superior to bowel.
Large bowel haustra are formed by the external muscle layer and do not cross the lumen. In chronic constipation, the colon can become so dilated that it fills the central as well as the peripheral abdomen, often obscuring small bowel. The small bowel may also be dilated if the ileo-caecal valve is incompetent.
Common causes of dilated large bowel are pseudo-obstruction, sigmoid volvulus and obstructing carcinoma. In pseudo-obstruction gas is visible in the rectum. In sigmoid volvulus, as in this case, the 'football' shaped sigmoid extends from the pelvis into the upper abdomen and there is no rectal gas. A caecal diameter of greater than 11 cm or small bowel dilatation should initiate urgent surgical referral as it indicates complete obstruction and the risk of perforation is high.
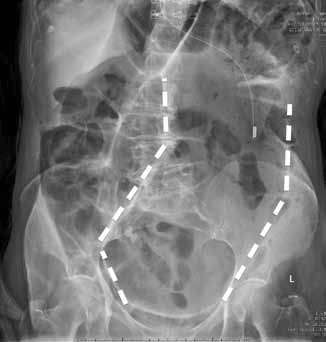
Figure 15. The patient's supine abdominal X-ray
Resource
Information on musculoskeletal injury in children, including the Salter-Harris classifications of growth plate injuries is outlined in the Trauma Manual from the Royal Children's Hospital Melbourne. Available at www.rch.org.au/paed_trauma/ manual.cfm?doc_id=12602#8.
Conflict of interest: none declared.
Acknowledgement
This article is based on the cases presented by Dr Damien Cleeve to many hundreds of rural and regional doctors and students in his successful Survival radiology for GPs tutorial.