Increasingly, regional training providers (RTPs) employ registrars within their medical education teams, reflecting both registrar interest in teaching and current workforce need. Anecdotally, the roles and responsibilities of a registrar medical educator (RME) differ markedly between training providers. Despite increasing numbers of RMEs, the role is not well defined in the literature or by the profession.
We aimed to explore the experiences and attitudes of all registrars employed as medical educators in RTPs in the Australian General Practice Training (AGPT) program between 2005 and February 2011.
Methods
We conducted a cross-sectional descriptive survey of RMEs in the AGPT program from 2005 to 2011. The survey period was February to March 2011. Participants were contacted either by direct email (via the RME network) or via the directors of training at all 17 RTPs in February 2011. Directors of training were also asked to provide the total number of RMEs in their programs over this time. The survey contained both multiple choice questions and open-ended responses. Responses were collected on an electronic platform. Simple descriptive statistics were calculated where appropriate. Free text responses were tabulated and then coded. These first order codes were then grouped into coherent themes by mutual discussion between the two researchers. All coding and thematic analysis was manual.
Ethics approval was obtained from The Royal Australian College of General Practitioners National Research and Evaluation Ethics Committee. Participation was voluntary.
Results
Characteristics of respondents and role
Sixteen of 17 directors of training responded and reported 44 registrar RMEs over the 6 year period. From our knowledge, the RTP that did not respond had only one RME. This RME was recruited to the study via the RME network. Thirty RMEs (67%) responded to our survey. Most were female (83%) and 53% had commenced training in 2010 or later. Table 1 outlines the characteristics of the respondents. Teaching experience spanned from teaching medical students on the wards to being a school teacher or university lecturer. Time in the role of RME ranged from 0.5 to 2.5 days per week, with 79% of RMEs spending 1 day or less in the role per week. Almost all participants (93%) felt that their prior experience had prepared them well for the role of RME.
Table 1. Characteristics of RMEs in AGPT program (2005–11)
| Characteristic | Percentage |
|---|
| Female |
83% |
| Currently employed as an RME |
50% |
| Degree other than medicine |
47% |
| Teaching experience before RME role |
93% |
Hospital experience before commencing general practice training
2 years
3–4 years
5+ years |
24%
47%
40% |
General practice training experience before RME role
Term 1 (6 months)
Term 2 (12 months)
Term 3 (18+ months) |
24%
45%
31% |
The RME activities and their perceived appropriateness are outlined in Figure 1. All RMEs reported undertaking the full scope of activities of a medical educator, however, the distribution varied considerably depending on the individual. For example, 93% of RMEs identified teaching more junior registrars and all RMEs felt this was an appropriate activity. Only 27% of RMEs were involved in registrar remediation with 67% of RMEs feeling this was an inappropriate activity to be involved in. Interestingly, curriculum planning, policy, resource development and research were highly acceptable to RMEs but many RMEs were not involved in these activities.
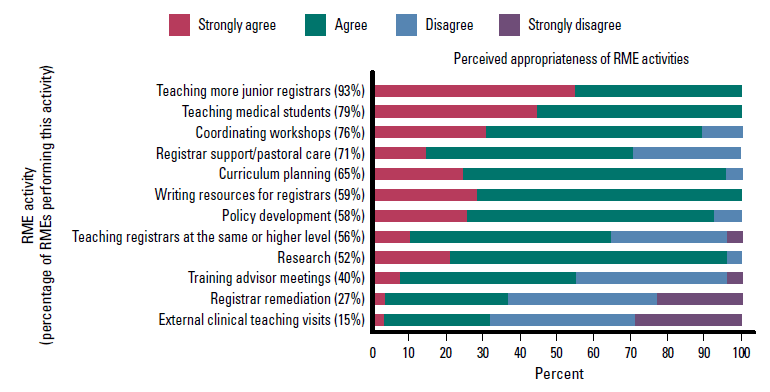
Figure 1. Content and perceived appropriateness of RME activities
Motivation
The overarching reason for starting as an RME was a desire for professional variety. Some saw the role as an opportunity to 'try before you buy', but many were firm about teaching as a career intention. Other motivators included specific skill acquisition and the opportunity to promote general practice and improve the education experience for fellow registrars.
'A sense of whether this was an area of medicine I wanted to pursue.'
'I see it as a stepping stone to ongoing medical education as part of my long term career plan.'
Experience
Registrar medical educators were overwhelmingly positive about their experiences, with 100% of registrars surveyed responding 'strongly agree' or 'agree' to the statement 'overall, I enjoyed my experience as an RME'. All were active participants in medical educator professional development. Participants identified both positive and challenging aspects of their roles. Flexibility, variety, networking opportunities and skills development were strongly identified positive themes. Other positive aspects included interaction with registrars and RTP staff, and the promotion of general practice.
'I contributed to the change in our education program which I now believe is one of the best offered.'
'Junior registrars seemed very grateful to have someone still on the program involved in their training.' The challenging aspects of the role were identified under the themes of time pressures, role definition, managing conflicts of interest, supervision and support. Most RMEs (73%) identified that the role involved dealing with conflicts of interest.
'[It was difficult] sorting out what the role involves.'
'Making a clear line between usual [discussion between registrars] … versus knowledge gained confidentially at work.'
A minor theme identified was credibility with fellow registrars and RTP staff. Many RMEs were surprised that this was not more of an issue.
'The RME needs to be very publicly backed by the RTP.'
'They seemed very responsive … I seemed more aware to the fact that I am a registrar than they did.'
The future
All respondents felt that their time as an RME was useful to future career planning. Most respondents (93%) planned to work in medical education in the future. Many respondents (67%) supported the assertion that all RTPs should have an RME, though some respondents countered that this role should only be available if there was an actively interested candidate.
'We are facing a tsunami of new grads/junior doctors and they will require ongoing education. The greater [the] number of doctors with both clinical experience and educational experience to help [with] training, the better.'
Discussion
The role of RME is increasingly popular within the AGPT program. Our study found that registrars become RMEs for many reasons, with prominent themes being intentional career development and diversity within their current work. Registrar medical educators find the job satisfying and enjoyable and most plan to continue working in the field. The RMEs work over the breadth of medical education activities.
This research is the first attempt to describe this emerging role within the AGPT. With a 68% response rate it provides a good insight into the characteristics and experiences of those who have been RMEs. One limitation is our inability to compare respondents to nonrespondents. Due to the emergent nature of the role, there is no register of these former RMEs or any way to track them. The survey methodology ensured good descriptive data but did not provide any opportunity for deeper explorations of the RME experience.
The role of the RME – or similar – has not been well described before. While peer-topeer teaching is recognised as an essential activity across the professional lifespan, it generally occurs on an informal basis.4 In the United States, one study identified that nearly a quarter of a family medicine trainee's teaching comes from a peer.5 The role of RME is a way to formalise this process in the AGPT program, providing an important connection between medical school problem based learning and the professional conversations between consultant GPs. Registrar medical educators can demonstrate to their peers that teaching is not only achievable and enjoyable but also a way to consolidate their own clinical knowledge and skills.6
Together with assisting in the delivery of the AGPT program, RMEs also provide RTPs with arguably work-ready medical educators on completion of training. The General Practice Education and Training Board has also recognised registrars as teachers within their submission to the Health and Hospital Reform Commission, stating that it should be a recognised role: clearly defined, educationally supported and properly remunerated.7
Conclusion
Registrars employed as medical educators within their RTPs are an increasing part of the general practice medical education workforce. This emerging role is of benefit to the individual, the learner and to the program more broadly. Further research and evaluation has the potential to shape the successful implementation of the RME role within the AGPT program. Particularly important are the perspectives of the RTPs and the learners themselves in this research. Conflict of interest: none declared.
Acknowledgements
This research was made possible by the in-kind support of General Practice Registrars Australia. The authors would also like to thank the participants and acknowledge the mentorship they received during their academic posts in the Australian General Practice Training program.