Case
A woman aged 88 years was hospitalised with a community-acquired pneumonia and started empirical treatment with amoxicillin/clavulanic acid and azithromycin. Three days later, she developed a pruritic skin eruption consisting of non-follicular pustules on a widespread oedematous erythema. The rash began in the skin folds and spread within a few hours to the trunk and limbs (Figure 1A). Some groups of pustules coalesced to form lakes of pus (Figure 1B).
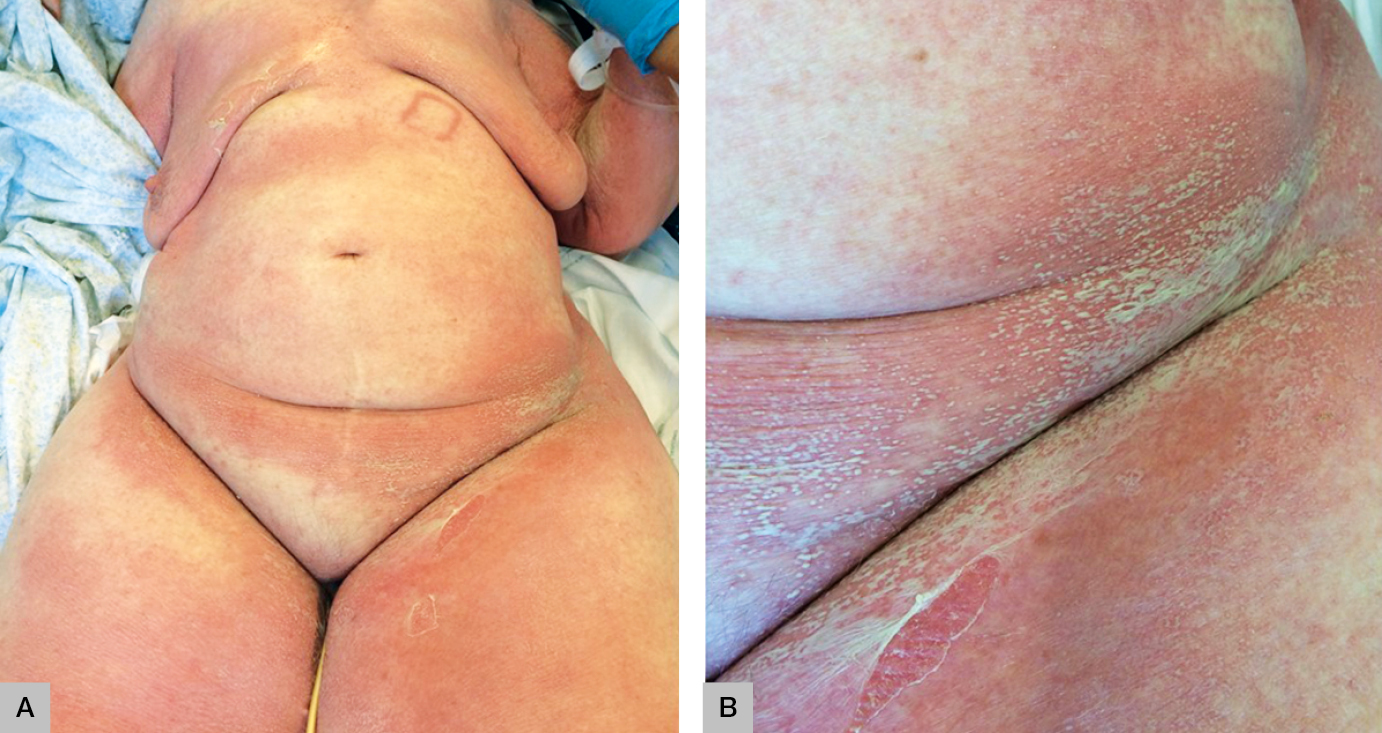 |
| Figure 1. Clinical appearance of the lesions |
The patient’s past medical history included chronic heart failure, dementia and obesity. Her regular medications were bisoprolol, bromazepam, pentoxifylline, triflusal, furosemide and cyamemazine. She had no fever or other symptoms, and had not taken any new drugs in the last months, beyond the above-mentioned ones.
Laboratory analyses revealed leukocytosis (21.1 x 109/L) with neutrophilia (18.9 x 109/L), elevation of aspartate aminotransferase (67 UI/L) and alanine aminotransferase (64 UI/L), and increased C-reactive protein (197.5 mg/L).
Question 1
What is the most likely diagnosis in this patient?
Question 2
What is the aetiology of this condition?
Question 3
How is this condition diagnosed?
Question 4
What differential diagnoses should be considered?
Question 5
What is the recommended management of this condition?
Answer 1
The most likely diagnosis is acute generalised exanthematous pustulosis (AGEP), a severe cutaneous adverse reaction, most often provoked by drugs or acute infections. It is a rare disease, with an incidence of 1–5 patients per million/year.1–4 AGEP can occur at any age and females and males seem to be equally affected.1,3,4
Answer 2
It has been reported that >90% of cases of AGEP are caused by drugs. The drugs conferring the highest risk are antibiotics such as aminopenicillins and macrolides, antifungal agents including azoles and terbinafine, anticonvulsants, antihypertensives (diltiazem) and antimalarial agents.1,3,5 Other triggers identified include acute viral infections (enterovirus, cytomegalovirus, Epstein-Barr virus, hepatitis B virus, parvovirus B19), Escherichia coli, Chlamydia pneumoniae, Mycoplasma pneumoniae, Echinococcus granulosus, dietary supplements, chemotherapy, heavy metal exposure (eg mercury), spider bites, radiation, and psoralens combined with ultraviolet A (PUVA) treatment.1–6
In this case, the most likely causative agents are the antibiotics amoxicillin and azithromycin.
Answer 3
The diagnosis of AGEP is always based on a detailed history and a thorough clinical examination.1 AGEP is a self-limiting disease, characterised by acute onset of numerous small (<5 mm), non-follicular, sterile pustules on a widespread oedematous and erythematous base. It usually begins in the intertriginous areas or on the face and rapidly spreads to the trunk and limbs. The interval between administration of the drug and onset of the eruption is usually 2–3 days for antibiotics and longer (1–3 weeks) for all other drug triggers.1,4 The rash is usually accompanied by fever (>38°C), increased blood neutrophil counts (>7 x 109/L) and typical histopathological changes such as subcorneal and/or intraepidermal pustules, marked oedema of the papillary dermis, perivascular neutrophilic infiltrate, eosinophils and/or apoptotic keratinocytes.7,8 The pustules resolve spontaneously within 15 days and are usually followed by a typical post-pustular pinpoint desquamation lasting a few days.1–3,8 About 50% of patients experience atypical skin symptoms, including purpuric lesions, Stevens-Johnson-syndrome-like ‘atypical targets’, vesicles and blisters.1,4,8 The mucous membranes may be involved in 20% of patients and lymphadenopathy has been reported in some cases. Apart from a slight reduction in creatinine clearance and mild elevation of aminotransferases, internal organ involvement is uncommon.2,3,8
When the clinical presentation is unclear, a lesional biopsy should be performed to establish a definitive diagnosis.6 Patch testing may contribute to identify the causative agent.1,4
Answer 4
Early diagnosis of AGEP and differentiation from other pustular eruptions are essential to avoid unnecessary and eventually dangerous drug therapy.8 The main differential diagnoses of AGEP are listed in Table 1.
Table 1. Conditions to consider in the differential diagnosis of AGEP1-3,6
|
|
Disease
|
Clues for diagnosis
|
|---|
|
Pustular psoriasis (von Zumbusch type)
|
Familiar and/or individual psoriasis history; confluent annular or polycyclic erythematous patches with pinhead-sized pustules at the periphery and a central area of desquamation.
|
|
Subcorneal pustular dermatosis (Sneddon-Wilkinson disease)
|
Pustules arising on normal skin or slightly erythematous base coalescing in annular or serpiginous patterns; presence of livedo reticularis; neurological symptoms can appear some years later.
|
|
Bullous impetigo
|
Small vesicles and pustules developing into bullae, containing clear yellow or turbid fluid without surrounding erythema, arising on a normal-appearing skin.
|
|
Drug rash with eosinophilia and systemic symptoms (DRESS)
|
Generalised maculopapular eruption on face, upper trunk, upper extremities; oedema of the face; eruption may become purpuric on legs.
|
|
Stevens-Johnson syndrome and Toxic epidermal necrolysis (TEN)
|
Flat, irregular, atypical target lesions or diffuse purpuric macules that frequently have necrotic centre (particularly in TEN) and tend to coalesce over time; predominant involvement of trunk and face; life-threatening condition.
|
|
Erythema multiforme
|
Erythematous iris-shaped papular and vesiculobullous lesions typically involving the extremities and the mucous membranes.
|
|
Acute febrile neutrophilic dermatosis (Sweet’s syndrome)
|
Abrupt onset of painful erythematous lesions (plaques, papules, nodules) in the face, neck and extremities associated with fever, arthralgia and peripheral leucocytosis.
|
|
Pemphigus
|
An autoimmune disease of the skin and mucous membranes
- Pemphigus vulgaris: extensive skin blisters and erosions with mucosal involvement
- Pemphigus foliaceus: scaly and crusted superficial erosions of the skin but not the mucous membranes.
|
Answer 5
When the cause of the eruption is a pharmacological agent, its cessation is the most important action. Supportive measures include the use of moist dressings with drying and disinfecting solutions (pustular phase), and the application of emollients (post-pustular desquamation phase). Corticosteroid treatment is usually unnecessary, but some authors support the use of topical corticosteroids for symptomatic relief and the use of a brief course of systemic corticosteroid in severe disease.2 Oral antihistamines and analgesics may also be considered.
The overall prognosis is good although the mortality rate is up to 5%. This occurs mostly in elderly patients who have significant comorbidities.
Case continued
The patient stopped amoxicillin/clavulanic acid and azithromycin treatment and started oral prednisolone (50 mg/day in tapering doses for 3 weeks). For the pneumonia, other antibiotics (levofloxacin and vancomycin) were prescribed. Thirty days later, she presented with only a pinpoint desquamation. Laboratory analyses were normal and she was discharged to go home. During hospitalisation, the patient’s daughter informed the treating clinicians that her mother was allergic to penicillin, which suggests that the skin rash in this patient was caused by amoxicillin.
Key points
When a patient is suspected to have experienced a drug-related skin eruption:
- Take a careful medication history, including any drug the patient is currently taking or has recently been exposed to, its chronological relationship with the rash onset and previous history of drug sensitivity. Consider not only prescription drugs but also over-the-counter medicines (herbal or homoeopathic medications), contrast media or vaccines.
- Perform a detailed clinical examination to determine what type of rash it is and whether it appears to be a drug eruption.
- Stop the suspected drug. In most cases, drug eruptions are reversible and disappear when the offending drug is withdrawn.
- Drug-induced rashes should be documented in the patient’s health record and explained to the patient or relatives, so that their recurrence can be avoided.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.