 |
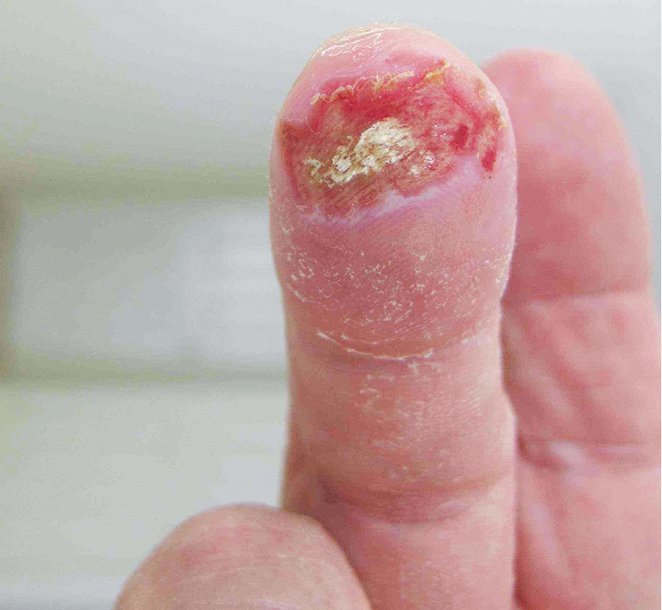
| Figure 1. Ulcerated lesion to the right middle fingertip |
Case
A man aged 71 years presented to a suburban general practice complaining of sores on his hands that had appeared 48 hours earlier. He noticed them while washing his hands after spending the day tiling with ready-made cement. He did not wear gloves. Initially, the wounds were painless but had become increasingly painful, red and throbbing over the preceding 24 hours. On examination, there was an ulcerated lesion on the tip of the right middle finger (Figure 1) and smaller lesions on his left index finger and thumb. There was poor sensation in the centre of the large ulcer, and pain and tenderness in the surrounding area. The skin elsewhere on his hands was peeling.
Question 1
What is the most likely diagnosis? What differential diagnoses should be considered?
Question 2
What is the typical clinical course of a cement burn?
Question 3
How does cement cause skin damage?
Question 4
What treatment is appropriate?
Question 5
What preventive measures should be taken?
Answer 1
The most likely diagnosis is a chemical burn caused by exposure to the tiling cement. Cement burns are under-reported as a cause of chemical burns.1 They are not thermal burns but a severe form of acute irritant contact dermatitis due to the alkalinity of cement, which removes surface lipids from the skin.2–4 Approximately half of these burns occur during do-it-yourself projects, while the remainder occur at work.3
The differential diagnosis includes allergic contact dermatitis (ACD) to the chromium or cobalt found in cement.5,6 ACD is due to a type IV (cell-mediated) hypersensitivity. It is more likely to present with itch rather than pain and ulceration, and is less likely to be localised. Repeated exposure is required for sensitisation to occur; therefore, it is more common among occupational cement workers5 and less likely in this case. Irritant contact dermatitis is usually due to repetitive trauma to the skin, either physical trauma such as the use of sandpaper, or chemical irritants such as soap and those found in cement. ACD can sometimes be difficult to distinguish clinically from irritant contact dermatitis, especially if the itch is mild. Patch testing is required to confirm the presence or absence of true sensitisation.
Connective tissue diseases such as scleroderma, lupus and vasculitis may also cause digital ulcers, but these are painful from the onset and present with other associated features. Other differentials include physical trauma and self-harm.
Answer 2
Cement burns have an insidious onset and symptoms appear 15 minutes to 48 hours after contact.4,7 Most commonly, patients complain of a burning sensation, possibly associated with pain, erythema, oedema and the development of vesicles. If not promptly managed, this can progress to ulceration, erosions and necrosis. Depending on the severity and location, long-term sequelae may include hypertrophic scar formation, hypersensitivity and contractures.4
As cement is commonly laid while kneeling, the majority of cement burns occur in the lower limbs.3,4,8 Although rarer, reports do exist of severe injuries to the hands.3,9,10 This case highlights the importance of being vigilant about making the diagnosis even in the upper limbs.
Answer 3
Irritant contact dermatitis ranges from slight scaling of the stratum corneum, redness and wheal formation to burns with ulcers and necrosis.11,12 The addition of sand and gravel to cement causes skin abrasions that facilitate penetration of cement into the skin. The calcium oxide in cement reacts with water to form calcium hydroxide, a highly alkaline substance (pH 12–13), which then causes liquefactive necrosis and ulceration of the skin.13
ACD results from repeated exposure to the chromate and cobalt found in most commercial cements.5 The hexavalent chromate and cobalt ions penetrate the horny layer of the skin and generate a type IV sensitisation reaction.
Ultimately, the severity and type of injury depends on the alkalinity and abrasiveness of the cement, the duration and repetitiveness of exposure, skin integrity before contact and the safety precautions taken.13,14
Answer 4
First aid involves removal of all contaminated clothing and equipment. Aggressive irrigation with water or saline should be performed immediately to remove any particulate matter causing ongoing skin damage. This should be followed by cold compresses, rest, elevation, analgesia and wound dressing.7 Referral to a burns unit should be considered for cement burns.
The existing literature suggests that approximately two-thirds of cement-related burns are full thickness and 33–85% may require surgical debridement.4,8,13 Of those not requiring surgery, conservative treatment with regular dressings and monitoring of healing is adequate. This was the approach taken with our patient. We applied 1% silver sulfadiazine cream and protective dressings for a period of 3 weeks. During the last 2 weeks, the patient replaced the dressing every 2 days. After the fourth week the wound had healed with no scarring.
Answer 5
Warnings about the possibility of cement burns are listed on most cement packages. Nonetheless, studies suggest that 50–100% of patients who present with cement burns are unaware of the dangers.3,14,15 The incidence appears to be increasing, possibly because of the increase in do-it-yourself projects.3 Recognising the risks associated with wet cement and using appropriate safety gear, including long pants, gloves and covered shoes, are the most effective methods of prevention.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.