Travel advice and vaccination for general practice patients before their travel was investigated in a sub-study of the Bettering the Evaluation And Care of Health (BEACH) program in May and June 2012. Patients were asked if they had travelled overseas in the past 2 years, the main reason for their most recent trip, the country where they spent most of their time, and whether they stayed overnight in a rural area. The patients were also asked whether travel advice was sought prior to travel, and from whom, for each of: rabies, typhoid, Japanese encephalitis, meningococcal encephalitis, cholera, hepatitis A and hepatitis B. If advice or vaccination was not sought prior to travel, reason/s were requested.
Of 2955 respondents, 690 (23%, 95% CI: 19.8–26.3) had travelled overseas in the previous 2 years. Patients travelled mainly for leisure, to visit family and friends, or for business. On these journeys, 66.1% (n = 448) of respondents travelled to countries or regions where they were at risk of exposure to one or more transmissible diseases (Figure 1). The regions most commonly visited were Maritime South-East Asia, North America, the United Kingdom/Ireland (UK) and Mainland South-East Asia (Figure 1). The individual countries most commonly visited were the UK (12.8% of respondents), the United States (12.7%), New Zealand (12.5%), Indonesia (10.8%; Bali 7.1%; other Indonesia 3.7%) and Thailand (9.1%). Where patients had reported staying overnight in a rural area at their travel destination (n = 133 patients), this most commonly occurred in the UK (23.3%), New Zealand (17.3%), Italy (9.2%) and Thailand (8.3%) (results not shown).
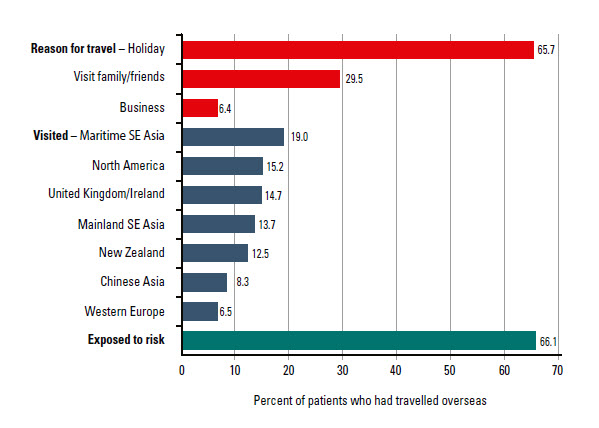 |
Figure 1. Reasons for travel, destinations and exposure risk for GP patients
Note: missing data removed |
Of 670 travelling respondents, 36.1% had sought travel advice prior to their trip: 29.9% (n = 200) from a GP; 3.7% (n = 25) from a travel clinic and 1.5% (n = 10) from the internet. Of the two-thirds of patients who had travelled to destinations with known risk of exposure, the most common diseases for which they had exposure risk were hepatitis B (for 64.2% of patients), typhoid (60.5%), hepatitis A (55.9%) and rabies (50.1%). Of 423 patients travelling to a country with risk of disease exposure, only 42.7% sought travel advice before their journey (Figure 2). The first column in Figure 2 shows the proportions of patients who travelled to regions with known risk of exposure to each nominated disease. Column 2 shows the proportions of travellers (from column 1) who: were vaccinated against that risk prior to travel; had discussed the risk prior to travel; and who did not discuss the risk prior to travel. The proportions of patients vaccinated against each risk varied from 50.9% for hepatitis A and 44.6% for typhoid to 3.2% for rabies and 1.5% for Japanese encephalitis. There was significant variance among the patients’ apparent perceptions of disease risk. For example, of the patients travelling to a region with exposure to hepatitis A, just over half were vaccinated prior to travel, whereas only 1.5% of patients at risk of exposure to Japanese encephalitis were vaccinated before travelling, and three-quarters had not even discussed the risk beforehand.
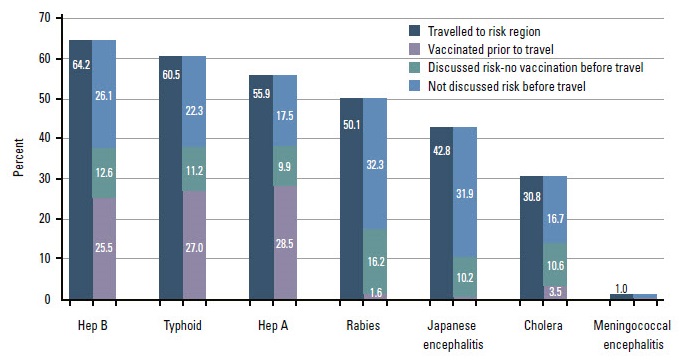 |
Figure 2. Exposure risk in visited regions and vaccination/advice prior to travel
Note: missing data removed |
Of 345 patients not vaccinated prior to travel, reasons were reported for 110. The most common were: patient refusal (31.8%); the GP did not think it was needed (22.7%); the patient did not inform the GP of their travel plans (13.6%); the patient informed the GP but too late for vaccination (7.3%); the patient did not realise they were at risk of infection in the country of destination (2.7%). Only two patients reported cost as the reason for not vaccinating.
GPs are an excellent source of advice and prophylaxis for patients intending to travel abroad. Public health media campaigns to increase awareness may encourage patients to discuss travel plans with their GP well in advance of their departure to ensure appropriate vaccination within the necessary time period.
Competing interests: None.
Provenance and peer review: Commissioned, not peer reviewed.
Acknowledgements
The authors thank the GP participants in the BEACH program and all members of the BEACH team. Financial contributors to BEACH 2012–2013: Australian Government Department of Health and Ageing; Australian Government Department of Veterans’ Affairs; AstraZeneca Pty Ltd (Australia); bioCSL Pty Ltd; Merck, Sharp and Dohme (Australia) Pty Ltd; National Prescribing Service Ltd; Novartis Pharmaceuticals Australia Pty Ltd; Pfizer Australia Pty Ltd. This SAND sub-study was undertaken in collaboration with bioCSL Pty Ltd. BEACH and SAND sub-studies are approved by the Human Research Ethics Committee of the University of Sydney.