HPV vaccines that protect against oncogenic HPV types 16 and 18, which are responsible for 70% of cervical cancers, have been available in Australia since 2007.9 Preliminary investigations analysing the effect of the HPV vaccine are promising, although longitudinal population studies are needed to further investigate and validate the effectiveness of the vaccine.9 HPV vaccination does not replace cervical screening because 30% of cervical cancer incidences are caused by other oncogenic HPV types that are not protected by the vaccine.10 In Australia, all women are advised to continue having regular Pap smears whether or not they have been HPV vaccinated.11 The National Cervical Screening Program (NCSP) has adopted an organised approach to cervical screening, which has halved cervical cancer mortality12 (Figure 1).
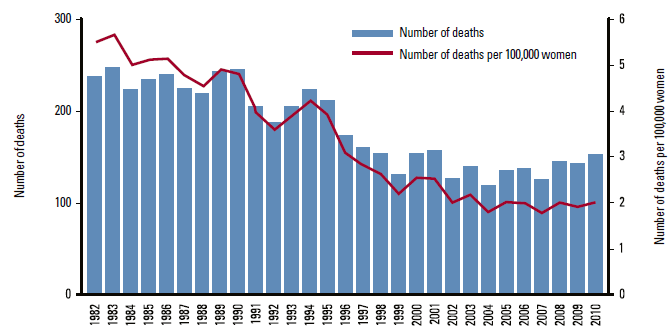
Figure 1. Cervical cancer mortality, women aged 20–69, 1982–201012
Despite Australia’s two-pronged approach to preventing cervical cancer, 771 women were diagnosed in 2009 and in 2010, 232 women died from this largely preventable disease.12 These incidence and mortality outcomes highlight the importance of women having routine (2-yearly) Pap smears, which can prevent up to 90% of the most common type of cervical cancer.13
Women’s participation
In the general practice setting, about 1.7 per 100 encounters will be for a Pap smear.14 Consequently, general practitioners (GPs) play an important part in providing information and services for women. GPs are well placed to encourage women to participate in cervical screening, including those with known cervical cancer risk factors, such as a history of multiple sexual partners, young age at first sexual intercourse, current tobacco use and immunosuppression (eg. HIV-positive).15–18
The continued success of the NCSP relies on sustaining a high rate of participation of eligible women (ie. those aged 20–69 years and with an intact cervix who have commenced sexual activity). In 2010–2011, 57.2% of eligible women participated in the NCSP at the recommended (2-yearly) interval, a significant decline from 63.4% in 1998–199912 (Figure 2). The Practice Incentives Program (PIP) for cervical screening offers financial incentives to encourage GPs to perform Pap smears on under-screened women aged 20–69 years.
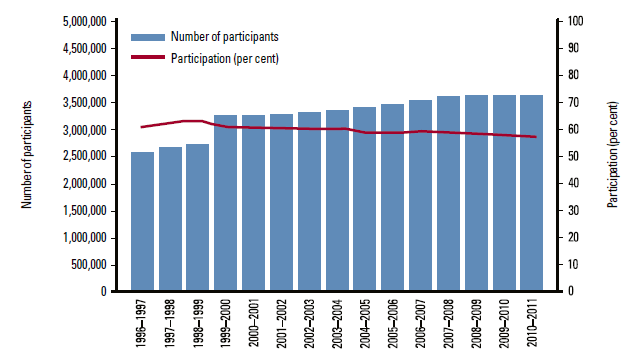
Figure 2. Australian participation in cervical screening, women aged 20–69, 1996–1997 to 2010–201112
Potential barriers
Unfortunately, the benefits of participation in cervical screening are not fully realised or shared equally by all women.19 The reasons for women not participating in cervical screening and the impact of not participating are complex and multifaceted and, therefore, difficult to quantify.20–23 Previous studies report that a lower uptake of cervical screening by vulnerable populations (ie. women from an ethnic background or low socioeconomic status) may be associated with cultural beliefs, language barriers, lack of information regarding cervical screening benefits and prohibition by male partners.22,24–29 Women often prefer a female practitioner to perform their Pap smear. This is particularly relevant for Aboriginal and Torres Strait Islander and culturally and linguistically diverse women.31
Different barriers exist at different stages of life. Studies have reported that menopausal and/or post-menopausal women may not realise that participation in cervical screening is required after the reproductive years.26,27 Younger women (<25 years) have reported different barriers to participating in cervical screening including:
- being too busy to book an appointment27
- finding it difficult to book in for screening through the GP appointment systems28
- believing they are covered by the HPV vaccine and no longer need to have regular (2-yearly) Pap smears.29
A GP’s approach to performing a Pap smear is critical in assisting women to overcome potential feelings of emotional unpleasantness, vulnerability, anxiety and fear.24,25
In 2011, the Western Australia Cervical Cancer Prevention Program (WACCPP) conducted a pilot study investigating women’s attitudes, knowledge and understanding of cervical cancer prevention.25 Participants included women aged 18–69 years (53% of participants were aged 31–54 years), living in the WA metropolitan area, with varying levels of education (Year 10 or lower, 23%; university qualification, 34%) and employment situations (full-time, 35% and home duties, 22%), who had ever been sexually active and had not had a hysterectomy. Thirty women were interviewed to investigate factors that contribute to reluctance or motivation to participate in cervical screening. Of particular relevance to GPs, the study found that participants request GPs to validate their emotions and to recognise that their feelings are not merely perception but are reality. If such acknowledgement occurs, it will support GPs in assisting their patients to make an empowered decision to have a Pap smear, rather than the patient simply following directions.25
Breaking down the barriers
Communication
Talking through concerns and addressing why the patient may feel uncomfortable and/or be avoiding cervical screening will promote the patient’s commitment to overcoming perceived barriers and improve their adoption of preventive health behaviours. The WACCPP pilot study reported that 66% (n = 368) of participants knew ‘not much/nothing’ about cervical cancer.25 Allowing adequate time with patients to provide them with information about the benefits and limitations of the Pap smear will break down the barriers to patients accessing a screening service.30
Before performing the Pap smear, the consultation should include advice on the implications of positive and negative test findings, and a plan for communication of the test result.31 In particular, a process whereby normal Pap smear results are provided over the phone has been shown to be helpful.30,32–34
Recall and reminder systems have mutual benefits for patients and GPs35–37 by providing individual support to patients, promoting adherence to screening recommendations and improving continuity of care. Computerised patient record management software packages are available for use in practices and may assist GPs in having timely recall and reminder practice systems. Practices could use this software to identify patients who are due for screening, as well as those who are under-screening, and invite those patients to have a Pap smear. Australian cervical cytology registries complement general practice reminder services by providing a ‘safety net’ through contacting healthcare providers and the patient should they be overdue for their next cervical screening test.
Opportunistic screening
It is imperative that GPs opportunistically encourage women’s participation in cervical screening. This is particularly important for women who are under-screened (have not had a Pap smear in the past 4 years) and can be achieved by identifying patients due for screening and encouraging eligible patients to have a Pap smear. Other strategies include educating patients about the screening pathway, when it is appropriate to commence and finish cervical screening, and offering a Pap smear during the consultation. Because of time constraints, these strategies may not always be feasible in the general practice setting. However, informing patients that they are due for their Pap smear and offering to make another appointment will serve to highlight the importance of cervical screening and encourage participation.
Delivery of screening services
Service delivery is critical, as communication alone will not result in sustained behaviour change. One of the most important strategies to ensure women’s participation in cervical screening is providing accessible and acceptable screening services.33,35–40 This can be achieved by offering patients a variety of clinic times (including facilitating booking appointments through email), offering bulk-billing for Pap smears and, where possible, providing access to female Pap smear providers (eg. employing a female nurse/midwife who can perform cervical screening services). In this way, general practices can contribute to a reduction in social inequalities and improve access to cervical screening services.30,41
Promoting access to cervical screening can also be achieved by providing information about where patients can find practitioners whom they consider acceptable to perform the screening. It is important to have an awareness of:
- the Medicare Local
- local women’s health centres
- Aboriginal medical services
- healthcare services for women with disabilities
- healthcare services for migrant and refugee women.
A patient who attends a different practitioner for Pap smears instead of her usual GP should be encouraged to have a copy of her cervical screening test result forwarded to her usual GP. This will assist in:
- supporting the patient with follow-up care if an abnormality is detected
- reminding the patient to re-screen at the appropriate interval.
Alternatively, with the patient’s permission, the appropriate state or territory Cervical Cytology Registry can be contacted (13 15 56) to request the patient’s most recent cervical test result.
Conclusion
GPs play a critical part in educating women on the benefits of the HPV vaccine and participating in routine cervical screening. Providing comprehensive education to women provides the GP with an opportunity to espouse a life course approach to cervical cancer prevention. Implementation of key strategies in general practice, such as provision of accessible services, recall systems and opportunistic screening, will ensure GPs continue to contribute to the success of the NCSP.
Key points
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.