Stroke is highly preventable in AF with the use of appropriate thromboprophylaxis.6 However, large treatment gaps are prevalent. Therefore, early identification of unknown AF and appropriate evidence-based management7 could lead to a significant reduction in the overall stroke burden and substantial savings to the healthcare system.8 Our recent systematic review found the incidence of unknown AF on a single screen of those aged ≥65 years was 1.4% in both clinic and community screening settings.8
International guidelines recommend opportunistic screening for AF in the clinic by pulse palpation in people ≥65 years to reduce the burden of disease attributable to AF.8–10 Given the high proportion of elderly people who visit their general practitioner (GP) each year, general practices are ideally placed to screen for AF. Each year 81% of adults visit their GP at least once,11 and people aged ≥65 years accounted for 30.5% of all GP encounters in 2012–2013.12 Frequency of attendance increases dramatically with age such that 26% of people aged ≥75 years who had seen a GP had done so 12 or more times in 12 months.11 An AF screening program in UK general practices identified previously unknown AF in 1.6% of screened patients using a pulse check and electrocardiograph (ECG).13
Unfortunately, a pulse check is not routinely performed in all patients and it may be less sensitive than ECG for AF. One of the major barriers to routine ECG screening, however, is the time and inconvenience associated with obtaining 12-lead ECG readings. An innovative iPhone ECG (iECG) device has recently been developed to support rapid collection and recording of a single-lead ECG rhythm using a simple snap-on sensor for the iPhone (Figure 1). Recently, we reported a pharmacy-based screening program using this device and found unrecognised AF in 1.5% of participants, all of whom had CHA2DS2-VASc scores ≥2.14 Importantly, screening in general practice offers the advantage of immediate verification and action by the GP. In this study we sought to determine whether it was feasible for practice nurses and receptionists to use the iECG device to systematically screen patients ≥65 years for AF prior to their GP consultation.
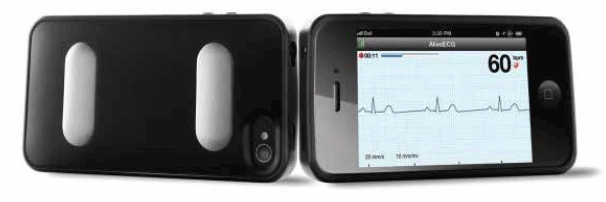
Figure 1. The iECG
Methods
The iECG device used was the AliveCor Heart Monitor for iPhone. This device has been previously validated15 and has Class IIa Therapeutic Goods Administration approval. Three general practices in greater Sydney were recruited to the study. Receptionists or practice nurses and GPs at each site were trained to operate the iECG.
For periods between May and October 2013, patients ≥65 years routinely attending the practice for a GP consultation were invited to participate by either the receptionist or nurse and provide informed consent. Patients with a severe co-existing medical condition or insufficient English proficiency to provide informed consent were excluded. The receptionist or nurse asked the patient to hold the iECG for 30 seconds (Figure 2) and entered the patient’s name into the application. An iECG record was wirelessly transmitted to a secure server, processed to remove noise and interpreted by a validated automated algorithm that states whether AF was detected. This information was then immediately accessible by the GP via a third-party secure website during the patient’s consultation (Figure 3). The iECG trace could be downloaded as a PDF and imported into the patient’s medical file. Any further treatment or testing was entirely at the GP’s discretion. There was no charge to patients for screening (nor any specific Medicare rebate), although usual consultation fees applied. It is possible that discussion of the iECG with the patient extended the duration of the consultation, but these data were not collected and consultation fees were determined by the GP. Practices were not paid for participation in the study.
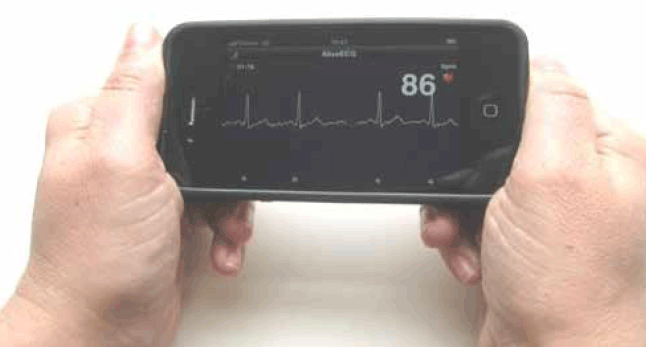
Figure 2. Taking an iECG reading
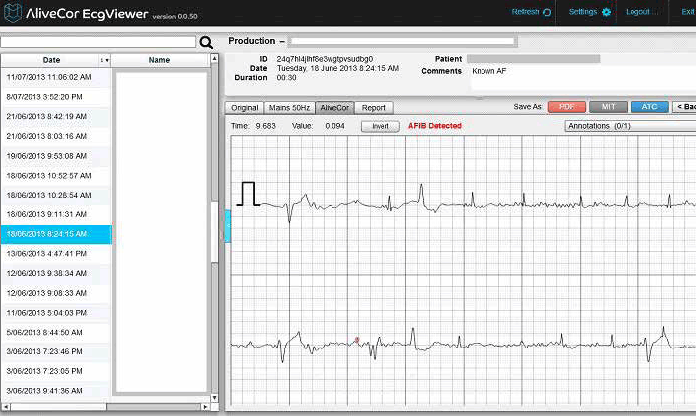
Figure 3. An ECG on a secure website
A detailed process evaluation was undertaken to inform the optimal AF screening model and to understand the barriers and enablers to uptake of screening. Semi-structured interviews were conducted with patients, receptionists, practice nurses and GPs. Face-to-face interviews were conducted, audio-recorded, transcribed and analysed thematically. Analysis explored views on benefits, disadvantages and acceptability of the screening device; the utility of the screening intervention; and the effects it had on the patient consultation. Data were contemporaneously analysed while interviews were being conducted and interviews were completed when thematic saturation was reached. The research team discussed the analysis to achieve final consensus on the principal themes.
Ethics approval
The study was approved by the University of Sydney Human Research Ethics Committee (HREC2013/135). The trial is registered with the Australian and New Zealand Clinical Trials Registry (ACTRN12613000429752).
Results
In total, 88 patients (51% male; age range 42–99, mean age 74.8 ± 8.8 years) were screened across the three general practices. Of these patients, 17 (19%) were in AF at the time of the screening. No cases of previously unknown AF were identified. Fourteen semi-structured interviews were conducted across all three practices, including two receptionists, one nurse, three GPs and eight patients. Interview duration ranged from 5–40 minutes. Figure 4 shows the relevant barriers and enablers to screening for each group.
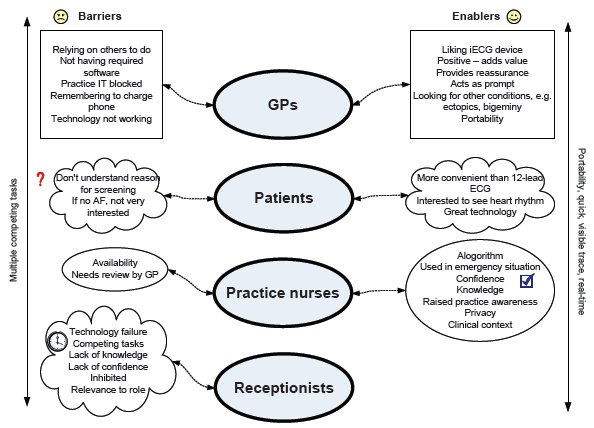
Figure 4. Qualitative themes
GPs: iECG a valuable tool
GPs overwhelmingly liked the portability and instantaneous results of the iECG, and that it acts as a prompt.
‘I think it’s fantastic. It helps us to concentrate for a moment on cardiovascular health’ (GP1)
‘It’s the awareness you need to look for AF in the GP setting…an opportunistic check’ (GP2)
Interestingly, despite the automated algorithm for predicting AF, GPs tended to rely on their own interpretation and were often able to see other detail in the trace. GPs noted that possible uses of the iECG were broader than AF screening, and a negative result (for AF) provided reassurance.
‘It’s actually helped us to pick up other people with other minor abnormalities’ (GP1)
‘The reassurance aspect of it was great’ (GP3)
Receptionists’ reluctance
Receptionists expressed ease with using the iECG device but were often reluctant to ask patients and generally felt inhibited.
‘I’d always get a little bit nervous about asking people’ (Receptionist 2)
Despite receiving training, they were also uncertain about explaining the screening and were unmotivated to learn.
‘We found either we give patients basically no information and just tell them the doctor wants that or you have to try and explain it in a way that they can understand and then they get confused and we get confused, and they just end up doing the test’ (Receptionist 1)
Receptionists were unsure how to respond to patients' questions and generally felt this duty was not part of their role. They did not see the relevance of screening for stroke prevention.
‘Patients would say, “Is this my heart rate?” and I would say, “I don’t really know”’ (Receptionist 2)
Receptionists also had multiple competing tasks, often quite urgent (eg. phone ringing). The study paperwork and consent forms meant the screening process took longer, which would have made it even more difficult for receptionists at busy times.
‘When we were really busy, it was impossible even with 3 receptionists’ (Receptionist 1)
Practice nurses’ confidence
While receptionists were reluctant, practice nurses were very confident with screening patients and explaining the process.
‘It gave you a chance to speak with the patient and ensure they understood … Patients were very eager, actually’ (Nurse)
‘[the nurse] opportunistically spoke to them about the study, educated them about the importance of it and then subsequently did the tracing and ... then called me down to have a look at it, so that I found it worked really well’ (GP2)
Nurses also performed the screening in a treatment room, which was more private and clinically focused than the waiting room.
Patients were attracted to the technology but not engaged in the clinical objective
Patients generally were impressed with seeing their heartbeat on the iECG.
‘It’s fascinating … well I did look at the screen as it was moving and it was quite interesting to wonder what it was actually saying’ (Patient 1)
‘It’s an impressive little gadget’ (Patient 2)
However, patients generally had a poor understanding of AF and the aim of the screening. This is likely to be related to how thoroughly it was explained to them prior to the screening.
‘What aspect of the screening process did you find useful? Well I don’t know what I did’ (Patient 3)
Once patients found out they did not have AF, they disengaged with the screening process. Many patients had other more pressing health concerns and were more focused on these.
‘I said, “Oh God, me old heart’s not going to close down" but he didn’t think there was anything wrong’ (Patient 4)
Discussion
Of the two models explored, a practice nurse model showed considerably more potential than a receptionist model. Enablers for practice nurses included confidence, independence, ease of training and an understanding of the relevance of screening. Drawing on Michie’s behaviour change theory,16 which suggests that intervention functions should target deficiencies in capability, opportunity and/or motivation, such a device seems to be promoting improved screening opportunities through its ease of use. The fact that the device was easy to use enhanced nurse motivation, which in turn improved knowledge and self-efficacy.16 Ideally, workflow can be improved in future by automatic importation of the ECG recording and the rhythm diagnosis into the patient’s electronic medical file. The extent to which such a model may be successful is highly influenced by the practice environment, particularly practice size and patient population serviced, the motivation and availability of staff, and the importance placed by GPs on such an activity and their motivation to review results.
While receptionists were capable of taking a reading on the iECG, in this study they were generally reluctant to do so. It is plausible that the additional research-specific explanation and receptionist time required to recruit patients and obtain informed written consent may have increased the reported reluctance, rather than solely having to ask patients to do a screen. The key reasons were difficulties with explaining the process to patients and answering their questions (despite training), a sense of inconveniencing patients, an inability to see the relevance of screening and an overall perception that this was beyond the scope of their traditional duties. Some of the key reasons identified by receptionists could be overcome with more intensive training, provided there was sufficient underlying motivation. There are recent moves to train receptionists to undertake a more clinical role, such as recognising heart attacks17 and working as medical assistants following a 12-month course.18 The findings presented here suggest that expansion of receptionists’ roles into clinical domains constitutes a paradigm shift towards a new ‘medical assistant’ receptionist workforce. In order for such a model to be viable, broader system level factors would need to be considered.
By contrast, the practice nurse workforce has played an increasingly prominent part in the primary healthcare system over the past decade. During the period 2003–2007, the number of practice nurses almost doubled to 7824 and there was a further 15% increase between 2007 and 2009 to 8914.19 A recent report found 82% of GPs had practice nursing staff, with an average of 0.4 full-time equivalent (FTE) practice nurses per FTE GP.12 The role of practice nurses in Australia has been expanding and evolving since service-based funding was introduced in 2005.20 This was explored in a recent article that identified six main roles for practice nurses and concluded that ‘nursing roles may be enhanced through progressive broadening of the scope of the patient care role’.20
Practice nurses have been accustomed to delivering a range of interventions and improving management of chronic conditions in primary care in Australia, including type 2 diabetes,21 childhood obesity prevention,22 depression and heart disease.23 Practice nurses have also been trained to conduct cervical screening24 and chronic obstructive pulmonary disease (COPD) screening.25 Practice nurses have also successfully worked with GPs to deliver opportunistic AF screening programs in general practices in the UK.26 Empowering practice nurses to conduct AF screening to prevent stroke using the iECG, as part of an inter-professional team under GP supervision, may be the optimal model for screening. This fits well within the context of fostering engagement and increasing practice nurses’ clinical capacity. To ensure sustainability, ideally practices would be funded for iECG screening, either under a new Medicare item number or an existing item (eg. 10997) related to managing patients with chronic disease under a care plan.
As many patients have poor knowledge of AF management, treatment and risks,27 one of the secondary aims of this study was educating the community about the importance of AF as a common arrhythmia and a significant cause of stroke. All but one of the patients interviewed did not have AF and, with a couple of exceptions, most were not interested in the educative process. Rather, they were relieved to have a negative iECG and did not engage further. We have no information on how the screening program could be used as a prompt to education of patients with known or unknown AF, and it would be worth exploring this further in subsequent studies.
Importantly, GPs found the iECG screening useful as a prompt to concentrate on cardiovascular health, which could facilitate further implementation research. Although stroke is highly preventable, there is a significant gap between evidence and practice in prescription of anticoagulants because of treating doctors’ reticence to prescribe warfarin, mainly because of an overestimated risk of bleeding and difficulties with use and monitoring of the drug relative to the potential reduction of stroke.5 Therefore, there is the opportunity for future research to integrate iECG AF screening with decision support for evidence-based anticoagulant use in those with known AF. Ideally, a future study would include development of decision support tools integrated with current practice software systems to inform the GP of the ECG diagnosis and provide best practice management recommendations.
Implications for general practice
- Screening for AF in general practice using an iPhone-enabled ECG device in patients ≥65 years is feasible and heralds new opportunities for reducing AF-related disease burden.
- Practice nurses are well placed to explain the process and conduct screening.
- Although enhanced screening is critical, improved medical management of detected AF will ultimately be required to prevent stroke burden.
Competing interests: AliveCor have provided free iECG covers for study purposes. None of the authors or associated institution has received any financial payment from AliveCor. Nor do they own any shares in AliveCor. Saul Benedict Freedman received investigator-initiated grants from Boehringer-Ingelheim, Bayer Pharma AG, BMS/Pfizer, Servier, Astra-Zeneca. Lis Neubeck received investigator-initiated grants from Boehringer-Ingelheim, BMS/Pfizer.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgements
The authors gratefully acknowledge the assistance of Dr Charles Ovadia, Dr Jade Robertson, Dr Andrew Krzyszton and Dr Oliver Leung. NL is funded by a National Heart Foundation Postgraduate Scholarship, DP is supported by an NHMRC fellowship and LN is funded by an NHMRC Early Career Fellowship.