Dizziness is a common presentation that accounts for about 5% of primary care visits.1 When a patient describes dizziness, it can reflect one of four conditions (Table 1).1,2 Unfortunately, patients tend to use the term dizziness loosely. In the case study described in this article, the patient presented with dizziness followed by fainting episodes, indicating presyncope rather than vertigo.
Table 1. Four categories causing a sensation of dizziness1,2
| Categories | Pathophysiology | Aetiology |
|---|
Vertigo
= spinning sensation |
Vestibular pathology |
Vestibular neuritis
Labyrinthitis
Meniere’s disease |
Presyncope
= fainting sensation |
Reduced cerebral perfusion |
Volume depletion
Neurocardiogenic syncope |
Dysequilibrium
= imbalance sensation |
Gait disorder |
Myelopathy
Peripheral neuropathy
Parkinson’s disease |
Light-headedness
= sensation of disconnection from the environment |
Psychological disorder |
Anxiety
Depression |
She had a history of hypertension, stable familial haemochromatosis, gastroesophageal reflux disease and hypothyroidism, which was treated with thyroxine but treatment was ceased due to euthyroid status. She is a lifelong non-smoker and drinks three glasses of wine each day with dinner. Her medications include lercanidipine 20 mg daily, irbesartan 150 mg daily and omeprazole 20 mg daily.
The additional information produces a list of differential diagnoses. Chronic hypertension may cause left ventricular diastolic dysfunction, leading to low cardiac output, which may lead to cardiac arrhythmias.3 Haemachromatosis can contribute to the development of cardiomyopathy.4–6 The accumulation of iron in the myocardium can lead to severe left ventricular diastolic dysfunction that ultimately leads to heart failure and cardiac arrhythmias.5,6 Similarly, over-replacement of thyroxine can lead to a hyperthyroid state, which, in turn, can lead to atrial tachyarrythmias presenting with palpitations and dizziness. On the other hand, hypothyroidism may cause hypotension and bradycardia, which also lead to dizziness. However, in this case, the patient’s euthyroid status rules out these possibilities. A history of gastroesophageal reflux raises the possibility of peptic ulcer development, which may cause anaemia or volume depletion, contributing to her dizziness.3 Lastly, the combination of a calcium channel blocker and an angiotensin receptor blocker may cause postural hypotension.
Eight months before her current presentation to the emergency department, while sitting and having lunch, she had two episodes of sudden dizziness followed by syncope lasting for 1–2 minutes. She described a prodrome of hot sensation and diaphoresis prior to loss of consciousness. She immediately presented to her GP and her antihypertensive medication was adjusted. An ECG revealed normal sinus rhythm at 80 beats per minute (Figure 1). No further investigation was done at that stage but she was advised to go to hospital if the dizziness recurred.
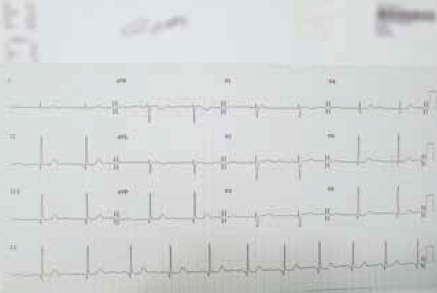
Figure 1. ECG of patient X
She had been well over the next 8 months but 18 hours before her current presentation to the emergency department, she experienced five separate but similar episodes of dizziness while lying in bed. These episodes were also followed by syncopal episodes lasting between a few seconds to 2 minutes. Again, there was no precipitant or sudden change in posture or emotion prior to the dizziness. This time she was referred to hospital for further assessment.
The additional information above confirms that the dizziness was not associated with head movement and was not postural in nature. There was no history of bleeding or volume depletion. It is worrisome that the dizziness was always followed by syncopal episodes that increased in frequency over a period of 24 hours. It is unlikely that the dizziness is due to vestibular dysfunction and is more likely to be due to a cardiac arrhythmia such as bradyarrythmia.
On examination her blood pressure was 155/85 mmHg when lying down and 175/90mmHg when standing, and heart rate was 73 beats per minute. Her temperature was 36.3°C, oxygen saturation was 97% at room air and her random blood sugar was 6.2 mmol/L. Her Glasgow coma scale was 15/15 and she was alert and orientated. Cardiovascular examination revealed dual heart sounds with ejection systolic murmur at the aortic region radiating to the carotids. Jugular venous pressure was not elevated and there was no pedal oedema or calf tenderness. Lung auscultation was clear and respiratory rate was 20 respirations per minute. Abdominal and neurological examinations were normal. A blood test showed haemoglobin 143 g/L, white cell count 9.7 x 109/L, sodium 137 mmol/L, potassium 4.2 mmol/L, magnesium 0.8 mmol/L, free T4 12.5 pmol/L, thyroid stimulating hormone 0.16 mU/L, iron 24 umol/L, transferrin 26 umol/L, transferrin saturation 46% and ferritin 38 µg/L.
Blood pressure was slightly elevated but there was no postural decrease on standing, which suggests safe dosage of the antihypertensive combination and excludes volume depletion. Her heart rate was within normal limits and glucose level was normal, which excludes hypoglycaemia. Her oxygen saturation was maintained in room air, which makes a diagnosis of pulmonary embolism unlikely. Neurological examination was normal, excluding a neurological disorder. The ejection systolic murmur may account for aortic stenosis and requires further investigation with echocardiography. The blood tests are reassuring.
The patient was admitted for cardiac monitoring. A similar episode recurred the next morning, coinciding with 14 seconds of ventricular standstill on telemetry (Figure 2). An echocardiogram showed normal left ventricular size, hyperdynamic systolic function, an ejection fraction of 75% and normal valvular structure. A carotid ultrasound showed no haemodynamically significant carotid artery disease.
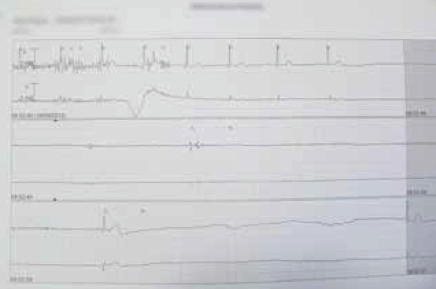
Figure 2. Telemetry of patient X
On the basis of the telemetry result, the patient’s prodrome of dizziness and syncopal episode is due to an arrhythmia. The normal echocardiogram excludes structural heart disease. The ejection systolic murmur heard in the examination may represent systolic flow murmur.
The patient received a dual-chamber pacemaker with a lower rate limit of 50 beats per minute.
Discussion
Patients often describe presyncope as a feeling of fainting or dizziness. It is caused by global cerebral hypoperfusion and is usually associated with compensatory activation of the sympathetic nervous system, which manifests as symptoms of diaphoresis and tachycardia.2 Presyncope episode is often followed by syncope, a transient loss of consciousness followed by complete and spontaneous recovery.7 This phenomenon was seen in the case above.
There are multiple causes of presyncope/syncope, which can affect people of any age. In general, it can be classified into three broad categories: neurally mediated syncope, orthostatic hypotension and cardiac syncope8 (Table 2). Rarer causes include syncope secondary to neurological, metabolic and psychogenic disorder.
Table 2. Etiology of presyncope/syncope8
| Neurally mediated syncope |
Vasovagal syncope |
Provoked by
- pain
- fear, emotion
- venesection
|
| Situational syncope |
Provoked by
- coughing
- micturition
- defaecation
|
| Orthostatic hypotension |
Primary autonomic failure |
Lewy body disease
Multiple system atrophy |
| Secondary autonomic failure |
Diabetes
HIV neuropathy |
| Postprandial hypotension |
|
| Drug-induced |
Anti-hypertensives, diuretics, antidepressants |
| Volume loss |
|
| Cardiac syncope |
Arrhythmias |
Sinus node dysfunction
Atrioventricular dysfunction
Supraventricular tachycardia
Ventricular tachycardias
Atrial fibrillation |
| Structural cardiac disease |
Valvular heart disease
Ischaemic heart disease
Cardiomyopathy
Pericardial disease |
Generally, the three categories of presyncope/syncope are associated with three different age groups. Neurally mediated syncope, such as vasovagal or situational syncope, often affect children and young adults.9 A study by Kang et al in children aged 3–18 years showed that syncope may be related to prolonged standing (30%), movement (13%) or a change in body position (9%).9 It may also be situational (ie. provoked by micturition, defecating or coughing).9 Syncope in this age group is usually considered low risk.
In middle-aged people (40–70 years), 10–20% of syncopal episodes have a cardiac aetiology.10 Adult athletes often experience exercise-induced syncope, which may be associated with underlying structural heart disease (ie. hypertrophic obstructive cardiomyopathy and Wolff-Parkinson-White syndrome).11 Often, a family history of sudden death is an important clue. In adults who have multimorbidities and risk factors, the incidence of coronary atherosclerosis is high. As this is a modifiable disease requiring secondary prevention, careful investigation and early intervention are vital. People in this age group (40–70 years) are also at risk of syncope related to arrhythmias.12 Initial investigation should include 12-lead ECG, 24-hour Holter monitoring or 7-day event loop recorder.12 Electrolyte imbalance may predispose to arrhythmias and, therefore, routine blood tests to measure levels of electrolytes and magnesium are important. If these investigations are negative, an electrophysiological study may be considered.12 If an underlying structural heart disease is suspected, transthoracic echocardiography should be considered. If a cardiac ischaemic event is suspected, troponin and cardiac stress test should be requested. Misdiagnosing cardiac syncope can be fatal and in this age group it is usually considered high risk and further investigation is warranted until all differential diagnoses have been explored.
In elderly people (>70 years), syncope is often associated with orthostatic hypotension secondary to autonomic failure, volume loss or medications. Age-related physiological changes, such as blunting of baroreflex sensitivity, reduced intravascular blood volume, greater susceptibility to infection, reduced myocardial elasticity and increased afterload, play a significant part in syncope in this age group.13 Medication review is crucial especially for medications that reduce blood pressure (eg. antihypertensive drugs, anti-parkinsonian drugs), affect cardiac output (eg. beta blockers, antiarrhythmics), prolong QT interval (eg. tricyclic antidepressants, amiodarone), cause drowsiness (ie. sedatives, cocaine) or affect electrolytes (ie. diuretics).14 Syncope in this age group requires careful assessment of their medication, comorbidities and fluid status.
Neurological disorders that cause syncope include seizures, migraine, transient ischaemic attacks and stroke.11 Electroencephalography should be requested if seizures are suspected.11 A computed tomography (CT) scan of the head is useful to rule out acute intracranial haemorrhage; however, routine head scans are not recommended for patients with low suspicion of neurological disease as diagnostic yield is low.11 In transient ischaemic attacks or stroke, syncope often results from disturbances in vertebrobasilar circulation presenting as vertigo and nystagmus.11 In such cases, magnetic resonance imaging (MRI) of the head is superior to imaging of the posterior circulation.11 Metabolic causes include hypoxia, hypo-/hyperglycaemia, anaemia and dehydration.11 This can be easily assessed by clinical examination and baseline blood tests. Intoxication with alcohol or illicit drug use is common in the younger age group. Lastly, psychogenic disorders should be considered when other aetiologies have been excluded. Social psychiatric histories are important in such cases and referral to a psychiatrist may be helpful.
The severity of syncope ranges from benign to fatal and distinguishing between different aetiologies can be challenging, as described above. Evaluation of patients presenting with syncope is outlined in Figure 3. Quinn et al have devised a syncope risk-stratification tool known as the San Francisco Syncope Rule.15 This tool is used to classify patients as high risk for fatality if they have any element of ‘CHESS’: congestive cardiac failure, haematocrit <30%, electrocardiogram abnormality, shortness of breath or systolic blood pressure <90 mmHg.15 A validation study in 2006 showed a 98% sensitivity and 56% specificity for predicting serious outcome.15 This risk-stratification tool together with with the red-flags described in Table 3 can be used to help general practitioners to ascertain safety discharge.
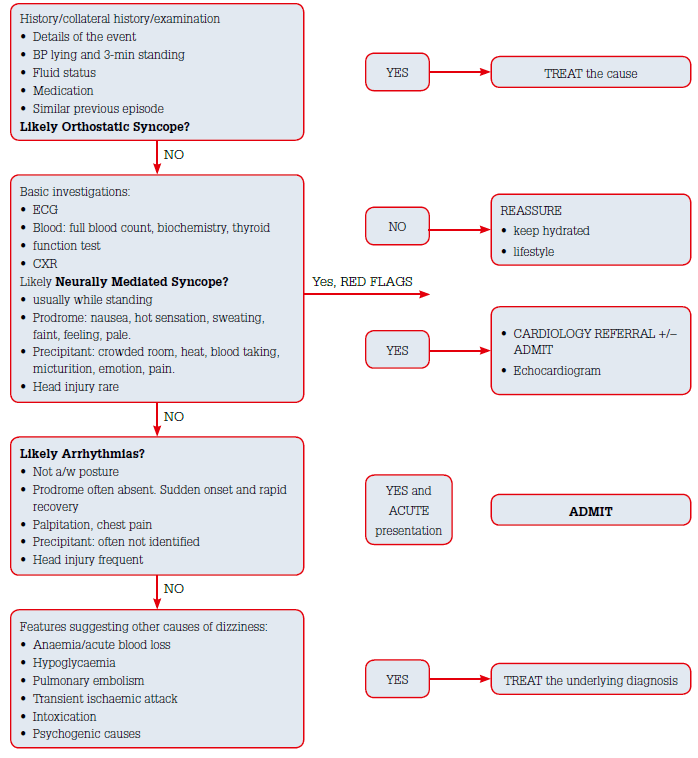
Figure 3: Evaluation of patients with pre-syncope/syncope in GP practice16
Table 3. Cardiac red flags 8,11
| Symptoms |
Chest pain |
Coronary artery disease |
| Worsening shortness of breath on exertion |
Heart failure |
| Palpitation or ‘skipped beats’ |
Arrhythmias |
| Signs |
Fluid overload |
Heart failure |
| Murmurs |
Valvular heart disease |
| Carotid bruits |
Carotid artery stenosis |
| Past history |
Ventricular arrhythmias, coronary vascular disease |
| Family history |
Sudden death |
| ECG findings |
Ischemic changes |
ST and T wave ischaemic changes |
| Prolonged QTc |
QTc >500 msec |
| Atrial fibrillation |
New atrial fibrillation |
| Persistent sinus bradycardia/tachycardia |
HR <40 or >120 |
| Non-sustained ventricular tachycardia |
4 or more VT beat |
| Brugada pattern |
J-point ST elevation V1–V3 and right bundle branch block |
| Wolf-Parkinson-White syndrome or supraventricular tachycardia |
Short PR interval and delta wave |
| Atrioventricular block |
Prolonged PR interval and bundle branch block |
| Right ventricular dysplasia |
Right bundle branch block with QRS >110 ms in V1, an epsilon wave in V1–V2 and T-wave inversion in right precordial leads |
Conclusion
Dizziness is a common clinical presentation. The biggest challenge for doctors is to formulate a diagnosis and to be able to identify patients with high-risk features that will require further investigation and urgent management to avoid fatality. Careful history taking and physical examination are pivotal in this case.
Competing interest: None.
Provenance and peer review: Commissioned; externally peer reviewed.
Acknowledgements
I wish to acknowledge the help provided by Dr Karam Kostner MD, PhD, FRACP, Consultant Cardiologist and Lipidologist at Mater Hospital for his assistance in the completion of this article.