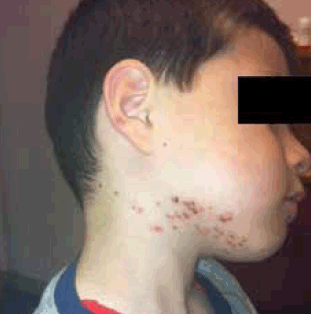
Figure 1. An erythematous maculopapular rash in a 5-year-old boy
Question 1
What differential diagnoses would you consider?
Question 2
What further history would be useful?
Answer 1
Differential diagnoses for the initial presentation would include:
- Herpes zoster infection (shingles)
- impetigo
- contact dermatitis
- insect bites
- scabies
- folliculitis.
Answer 2
It is useful to elicit a history of allergic reactions or exposure to potential allergens. Given the distribution of the rash, contact with or exposure to a plant or other allergen would assist in narrowing the differential diagnoses. Although important, the childhood immunisation status of the patient is a less contributory aspect of the history. It may be more useful to ask if he or his siblings had been recently exposed to varicella.
Further information
Medical opinion at the resort suggested the lesions were due to insect or sandfly bites and a topical corticosteroid was prescribed. A few days later, on returning home, he was reviewed and a revised diagnosis of folliculitis was made. This was treated with a course of cephalexin syrup. Gradual improvement of the lesions was noted, with decreased erythema and pruritis.
Past history revealed that the patient had experienced previous urticarial reactions of unknown sources. There was no clear history of eczema. Skin-prick testing completed by an allergist had shown strong sensitivity to peanuts and rye grass. He had asthma and episodes of croup as an infant, but was an otherwise healthy child. A complete vaccination history was documented, including varicella at the recommended age of 18 months.
On presentation to our clinic, the patient had approximately 15 dry scabbed lesions over the right side of his neck and inferior jaw, in the C3 distribution. He had mild right-sided pre-auricular lymphadenopathy. Our final diagnosis, on the basis of these findings was H. zoster infection (shingles).
Question 3
Is it reasonable to reach this diagnosis given the child had been immunised against varicella?
Question 4
Has there been a change in the incidence of shingles since the introduction of a routine scheduled varicella immunisation? Is there any difference in incidence between patients who receive one or two doses of the vaccination?
Answer 3
The case presents a clinical diagnosis of shingles, despite routine vaccination at the age recommended by the Australian National Guidelines.1 Since 2005, a single dose of a live attenuated varicella vaccine has been funded for all children aged 18 months; a catch-up dose is available for children aged between 10–14 years who have not received varicella vaccine previously and who have not had the disease.1 Detection of shingles in vaccinated children is often a diagnostic challenge, as the lesions tend to be fewer and smaller in size, and patients often present with fewer systemic symptoms.2,3 Clinicians should, therefore, consider shingles as a differential diagnosis for a rash in a child, regardless of immunisation status. The condition occurs in 20% of the population, but is rare in children aged <12 years.4 Detection of H. zoster in this age group is significant from a public health perspective, in limiting their contact with high-risk groups including immunocompromised patients, pregnant women and babies <1 month of age.4
Answer 4
Some sources suggest that following implementation of the varicella vaccination, the incidence of shingles may be higher as a result of the decreased circulation of wild-type virus, which subsequently reduces natural T-cell immunity.2,5 Overall, the reported incidence of shingles following introduction of the varicella vaccine, compared with the pre-vaccination era, varies markedly in published studies, depending on age range and population types.1,2,6 A 2-dose vaccination schedule was implemented for children in the US in 2006 following reports that a second dose is optimal to provide an immune response more like that acquired after natural infection thus increasing population immunity.2 A study using Australian data and a mathematical model projecting long-term outcomes suggests a 2-dose vaccination program would be a better long-term strategy in minimising breakthrough varicella (chickenpox), but its effect on the incidence of shingles is unlikely to be significant for 65 years.7 Routine administration of a second dose of a varicella vaccine for children is not currently a part of the National Immunisation Program schedule.1
Key points
- The differential diagnosis for a rash in children should include H. zoster infection (shingles), which can occur in children who have been immunised against varicella.
- There is currently little evidence from Australian data to determine whether a 2-dose vaccination schedule would decrease this risk, compared with a single dose schedule.
- At present, if parents wish to minimise the risk of breakthrough varicella (chicken pox), administration of a follow-up dose of varicella vaccine can be given with a minimum interval of 4 weeks between doses, but the second dose is currently not funded.
Conflict of interest: None.
Provenance and peer review: Not commissioned; externally peer reviewed.