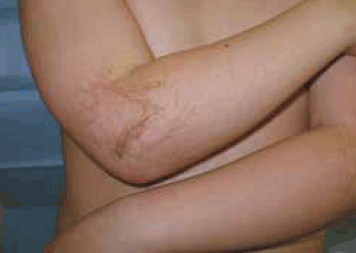
Figure 1. Bilateral hairy elbows
Question 1
What is a primary nevoid hypertrichosis?
Question 2
Do you need to perform any tests to diagnose it?
Question 3
What is an appropriate therapeutic approach to this condition?
Answer 1
Nevoid hypertrichosis is a localised type of hypertrichosis characterised by its low incidence. It is defined by the growth of hair on a localised area of the body surface at birth or during the first years of life. It usually involves an isolated region but, occasionally, several areas may be involved.1
Nevoid hypertricoses can be subdivided into primary or secondary. HC, or hairy elbows syndrome (Table 1), is included in the first group. It was first described by Beighton2 in 1970. This circumscribed hypertrichosis clinically presents with a significant amount of lanuginous, thin hair on skin otherwise normal in texture and morphology. The distribution is symmetrical and bilateral on the extensor surfaces of the distal third of the arms and proximal forearms. These hairs progressively become longer and more pigmented.
This condition frequently arises in early childhood (1–3 years) and reaches its greatest severity at the age of 4–5 years.3 The inheritance pattern is variable. There have been reports of autosomal dominant and recessive cases, as well as sporadic ones.
Table 1. Primary nevoid hypertrichosis
- Hairy elbow syndrome
- Eyebrow hypertrichosis
- Hypertrichosis of the auricle
- Hairy polythelia
- Posterior cervical hypertrichosis
- Anterior cervical hypertrichosis
- Eyelashes hypertrichosis
- Nose edge hypertrichosis
- Hairy palms and soles malformation
|
Answer 2
As far as the hairy elbows syndrome is concerned, two types of patients may be considered. On the one hand, there are sporadic cases that do not present with any radiological, morphological or hormonal changes. On the other hand, some cases of HC form part of a more complex syndrome. Several anomalies and disorders have been reported in the literature, such as short stature (usually restricted to cases of patients with Weill-Marchesani syndrome), facial or limb deformities, developmental disorders, bone disorders and ocular and neurological abnormalities. Therefore, the need to perform a workup to rule out an associated disorder will be determined by the findings of a properly conducted medical history. Awareness of this condition is important in avoiding unnecessary tests.
A skin biopsy of the affected area does not usually provide any significant data. A trichogram may show a normal proportion of hair in all three phases of their cycle, or else increased hair in the anagen phase, which would explain their length (eg. 90% anagen , 9% telogen, 1% catagen).
Answer 3
It is important to emphasise to parents the benign nature of HC, so that expenditure on expensive and useless treatments can be avoided. Depigmentation or shaving of the area may be initially recommended. More definitive therapies, such as laser hair removal, should be delayed until adolescence for those rare cases that have not spontaneously regressed by then.4 Additionally, the psychosocial needs of the child should be considered.
The actual prevalence of HC, as well as its strength of association with other disorders, remains unknown. This may be the result of misdiagnosis or miscommunication in sporadic cases such as the one reported.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.