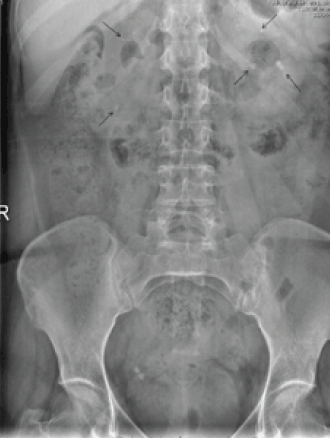
Figure 1. Abdominal X-ray in which multiple and bilateral calcium foci are observed in both renal units
Question 1
What is the diagnosis?
Question 2
What are the common causes?
Question 3
What investigations would you perform?
Question 4
How would you treat this condition?
Answer 1
Because of the presence of recurrent renal colic and the plain radiography images, the diagnosis in this patient was nephrocalcinosis, a condition with ultrasound, radiographic or computed tomography (CT) evidence of multiple calcium deposits in the renal parenchyma, most commonly in the renal medulla.1,2 Nephrocalcinosis can be classified as intratubular or interstitial. Interstitial subepithelial deposits contain calcium phosphate that erodes the renal papilla and produces a pre-lithiasic lesion (also called type I) corresponding with Randall plaque. The excessive super-saturation that is associated with necrosis of the tubular epithelial cells produce crystallisation and crystal deposits in the terminal portion of the collecting ducts (also called type II).2,3 The development of interstitial nephrocalcinosis depends on calcium deposits and anions, such as oxalate and phosphate, in the interstitial tissue. These conditions are caused by local factors, such as pH levels and the presence or absence of inhibitors and anions. Intratubular nephrocalcinosis represents only a small percentage of interstitial nephrocalcinosis and requires a thorough histopathological analysis to determine the cause.1
Answer 2
The presence of nephrocalcinosis and calcium phosphate nephrolithiasis is often associated with urine abnormalities.4,5 The most common underlying pathologies include distal renal tubular acidosis (characterised by the inability to acidify the urine in the distal tubule, in combination with hypokalaemia, hypocitraturia and decreased levels of urinary ammonium), primary hyperparathyroidism, idiopathic hypercalciuria (characterised by the presence of hypercalciuria, normocalcaemia, normophosphataemia and the absence of disturbances in bone metabolism),6 medullary sponge kidney (which causes a malformation of the distal collecting tubules and can lead to the development of hypokalaemia, lithiasis, nephrocalcinosis, an elevated urinary pH and occasionally renal tubular acidosis),7 analgesic nephropathy and papillary necrosis.7–14 Less common causes include hyperoxaluria and other tubulopathies.1
Answer 3
A plain X-ray or ultrasound can be suggestive of the diagnosis, with the gold standard imaging test being a CT scan because it can clearly distinguish nephrolithiasis from nephrocalcinosis. A complete biochemical profile is also required, including serum calcium, phosphorus, alkaline phosphatase, intact parathyroid hormone (iPTH) and vitamin D. A urinalysis was also requested in this case to determine the patient’s 24-hour calcium excretion, urinary creatinine, calcium/creatinine ratio and pH. In the presenting patient, the results yielded a serum level of calcium of 3.46 mmol/L (normal 2.14–2.54), phosphorus of 0.67 mmol/L (normal 0.81–1.62), alkaline phosphatase of 82 U/L (normal 40–130), iPTH of 26.56 pmol/L (normal 1.57–6.82) and vitamin D of 24.4 nmol/L (normal 37.3–49.8). The urinalysis revealed a pH of 5.5, 24-hour urine calcium of 12.45 mmol (normal <6.24), creatinine of 6.24 mmol and calcium/creatinine ratio of 1.99. The patient also had decreased tubular reabsorption of phosphates of 72% (normal >80). In addition to the patient’s increased iPTH and hypovitaminosis D, the presence of hypercalcaemia, hypophosphataemia and hypercalciuria, an increased calcium/creatinine ratio in the urine and decreased tubular reabsorption of phosphates suggested primary hyperparathyroidism as the primary diagnosis. Parathyroid scintigraphy with technetium confirmed an anomalous uptake and an increased retention of tracer in the lower left parathyroid gland, consistent with parathyroid adenoma. Bone densitometry revealed osteoporosis in the lumbar spine (T-score –3.5) and hip osteopenia (T-score –1.8). The bone resorption marker beta-CrossLaps (beta-CTx) was also elevated at 0.516 ng/mL (normal 0.157–0.440).
Answer 4
In 2002, the National Institutes of Health recommended surgical treatment in patients younger than 50 years of age (or in patients who cannot be monitored) who develop serum calcium levels greater than 2.86 mmol/L, osteoporosis and 24-hour calcium excretion levels greater than 9.6 mmol.8,9 Parathyroidectomy is considered to be the only curative treatment for primary hyperparathyroidism and can be performed with a minimally invasive endoscopic treatment or by open exploration of all four glands; the last is considered to be the gold standard.8 As this patient declined surgical treatment, medical therapy was started with cinacalcet (30 mg twice daily) and denosumab (60 mg every 6 months). Excellent control of the calcaemia was achieved 1 month after treatment, with the level dropping to 2.66 mmol/L. The patient also had decreased levels of beta-CTx (0.041 ng/mL) and iPTH (24.31 pmol/L). Cinacalcet is a calcimimetic that increases the sensitivity of calcium receptors and decreases the iPTH levels.11,14 The treatment was tolerated well by the patient and controlled the disease,14 which suggests that chemical parathyroidectomy may be an attractive option. The use of other antiresorptive agents, such as denosumab (a human monoclonal antibody), inhibits the receptor activator of the nuclear factor-kB ligand (RANKL), thereby improving bone mineral density and decreasing resorption markers.15,16
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.