Case study
A young male, 6 years of age, who had previously been well, presented with his parents to the paediatric walk-in clinic.
The child was fully vaccinated, had no drug allergies and no family history of alopecia or autoimmune disease.
His parents described a 3 year history of a patch of right-sided temporal hair loss, which had not changed over time.
Treatment with topical corticosteroids (fluticasone propionate once per day for three months) was prescribed by the pediatrician, who reviewed the patient once per month.
As there was no significant improvement after 3 months, the patient was then referred to the dermatology department.
At the initial visit, he was noted to have a circumscribed 3 x 5 cm triangular plaque of alopecia on the right temporal area of the scalp (Figure 1a and 1b). There were no signs of inflammation, scaly or broken hairs, or tapering hair. His
eyelashes, eyebrows and nails were all noted to be normal.
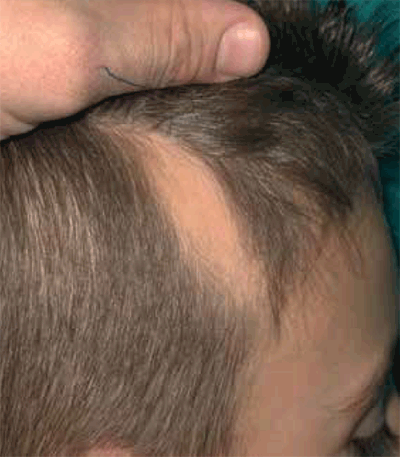
Figure 1a. Macroscopic view of area of alopecia

Figure 1b. Trichoscopic view of area of alopecia
Question 1
What is the most likely diagnosis?
Question 2
What is the aetiology of this condition?
Question 3
What is the differential diagnosis?
Question 4
How can this condition be treated?
Answer 1
The most likely diagnosis is temporal triangular alopecia (TTA), which is a circumscribed, non-cicatricial (non-scarring), non-inflammatory patch of hair loss, confined to the frontotemporal region.1 It is also referred to as congenital triangular alopecia, although in one series only 36.5% of cases were diagnosed at birth, 55.8% between the ages of 2–9 years, and 3.8% in adulthood.2 The presence in a child of a non-scarring, permanent and asymptomatic patch of alopecia in the frontotemporal area with vellus hairs surrounded by a normal terminal hair area, is highly suspicious for TTA, and may negate the need for a diagnostic biopsy.
The formal diagnostic criteria for TTA are:3,4
- a triangular or lancet-shaped patch of alopecia involving the frontotemporal scalp
- persistence without significant hair regrowth for 6 months and trichoscopic findings of:
- normal follicular openings with vellus hairs surrounded by a normal terminal hair area
- absence of broken hairs, regrowing (tapering) hairs, black dots, yellow dots and orifice loss.
If there is any doubt in recognising TTA, a dermatology referral should be considered.
Answer 2
The cause of TTA is still unknown.5 However, because familial cases were reported previously, it has been argued that TTA may be transmitted as a paradominant trait, which would be expressed only when postzygotic loss of the corresponding wild-type allele occurred in a early developmental stage.5
Answer 3
The differential diagnosis6,7 of focal alopetic lesions similar to TTA and their key points of differentiation are:
- alopecia areata – broken hairs, tapering hairs, black dots or yellow dots
- trichotillomania and traction alopecia – broken hairs and different sizes of hair
- aplasia cutis congenital – complete lack of skin appendages, including hair follicles and a translucent appearance on the skin of the scalp.
Answer 4
No active treatment is probably the best option for this benign condition.
Currently, the only curative treatment is surgery.7 Complete removal of the bald patch can be considered, but the closing of a surgical wound 3–4 cm in diameter on the scalp may require the use of flap or tissue expanders.
Treatment by follicular unit hair transplantation has acheived a satisfactory cosmetic result in at least two cases, as described by Bargman8 in 1984 and Jimenez-Acosta9 in 2009.
As TTA shares the clinical features of vellus hair and hair follicle miniaturisation with androgenetic alopecia, some are considering treatment with topical minoxidil. There is, however, no evidence of treatment efficacy at this time.10
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.