Case study
A child, 3 years of age, presented to a district hospital emergency department with a 4 day history of loss of appetite and a 2 day history of passing, with apparent difficulty, pale, thick, pasty faeces.
Examination revealed a tired looking child, normal vital signs, moist mucous membranes, and a moderately distended abdomen with some mild left upper quadrant tenderness. Bowel sounds were of normal frequency but high pitched.
An abdominal X-ray revealed numerous irregular X-ray opaque objects (Figure 1).
The child’s mother then revealed that the child frequently ate soil. The X-ray was typical of such pica.
In soil pica, or geophagia, the majority of X-ray opaque material is found in the colon.1 Iron and potassium tablets are also X-ray opaque, but are seen on X-ray to be in the stomach, not the colon. Tuberculosis, calcified lymph nodes and enteroliths can also cause multiple abdominal opacities, but not on the scale and pancolonic distribution of geophagia. Kidney and gall bladder stones produce opacities restricted to the region of the organs concerned. Barium that has entered diverticula from previous barium studies has a different and characteristic appearance.
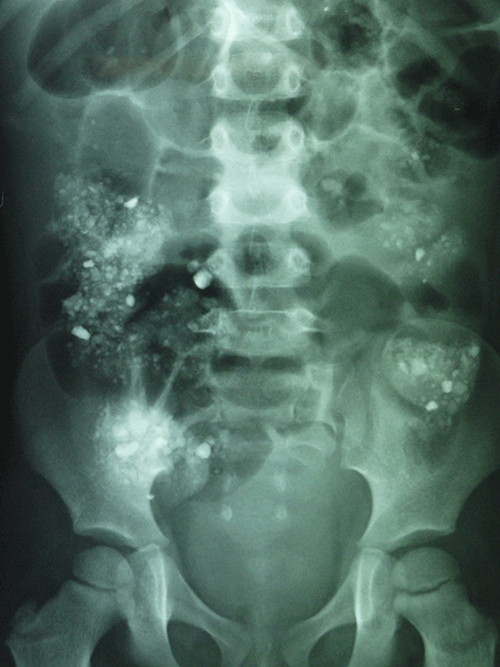
Figure 1. Abdominal X-ray displaying typical features of soil pica. The X-ray opacities are mainly in the colon
Case study continued
A full blood count revealed microcytic anaemia with a haemoglobin of 76 g/L (normal range 110–145 g/L) and a mean cell volume of 54 fL (normal range 72–87 fL). There was no family history of thalassaemia, thus the most likely cause of such a low mean cell volume was iron deficiency. The serum iron was 2 µg/L (normal range 10–100 µg/L) and the transferrin saturation was 2%, confirming severe iron deficiency. The whole blood lead ordered on the basis of soil eating was 8 µg/dL (Australian level of further investigation >10 µg/dL; suggested United States reference level for further investigation >5 µg/dL).2
Pica
Pica is the Latin name for ‘magpie’, a bird with a reputation for eating non-food items.3 It is defined as a persistent intended ingestion of non-food items4 and is often viewed as a compulsion. The Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) views pica as a disorder. However, it can be argued that pica should be seen as a symptom.5 There may be a hazy boundary when eating non-food items is culturally the norm, or when such items are consumed for traditional ‘medicinal’ purposes. In such cases, pica is clearly more a behaviour than a disorder.
There are a number of theories for the causation of pica, which range from an attempt to gain minerals such as iron, to various theories of psychological and physical comfort.6,7
In general, the most common forms of pica are soil ingestion (geophagia) and ingestion of large quantities of ice (pagophagia). Geophagia is very common in some African communities, with several studies reporting rates in excess of 50% in those sampled.8–10 Pagophagia is commonly reported in studies of pica in Caucasian populations, usually at rates over 10%.6,11 Geophagia occurs in Western populations, particularly in migrant groups living in such communities.6,12
Pica and iron
Pica in its various forms is often associated with certain medical conditions, especially iron deficiency anaemia. There are studies and numerous case reports that appear to show that the iron deficiency leads to the pica, and studies that show that geophagia may actually result in dietary iron being bound to the ingested clays, thus causing iron deficiency.13 Certainly many studies and case reports show an association of iron deficiency anaemia and pica.8,11,14,15 There are also studies that do not show such an association.
Various authors have recommended asking about pica when iron deficiency is found. It should also be enquired about when adults or children are found to have an elevated lead level.16
Pica and lead
Pica is an established risk behaviour for lead poisoning in areas where the soil is contaminated, such as in lead mining and processing communities (eg. Broken Hill, Port Pirie, Mt Isa) and in old housing with flaking, lead-based paint.17,18 Indeed the first description of cases of childhood lead poisoning involved children chewing paint in Queensland a century ago.19 In this era of do-it-yourself home renovation, people may be inadvertently liberating large amounts of old lead paint into the home environment.
The relationship between pica and lead poisoning is more complex than just the ingestion of lead contaminated soil or paint flakes. The iron deficiency associated with many cases of pica increases duodenal absorption of lead.20 This is brought about by iron deficiency stimulating an increase in the divalent cation transporter in the duodenum. This transporter absorbs Fe2+ as well as some other divalent cations such as Pb2+. Thus, in iron deficient children the mechanism for absorbing lead from the gut is increased. Further, the iron deficient child has less Fe2+ in the duodenum to compete for the divalent cation transporter with the Pb2+.
Pica and obstruction
There are occasional reports of constipation and intestinal obstruction due to geophagia.21,22 Fortunately this would seem to be a rare complication.
Key points
- The presence of pica should alert the clinician to the risk of associated iron deficiency.
- In areas where there is lead contamination, the whole blood lead level should be tested in children who exhibit pica.
- In children with elevated lead levels it is particularly important to enquire into pica as the ingestion of lead will continue until the pica ceases.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.