Hyperhidrosis is a deeply distressing condition for patients: it causes physical discomfort and social awkwardness, negatively impacts on daily activities, impairs performance and productivity of work, and results in higher rates of depression and reduced levels of confidence.2 Despite this, a recent survey demonstrated that only one-third of patients with hyperhidrosis seek help from their general practitioner.2
Bromhidrosis is defined as offensive body odour. As this conveys strong non-verbal signals,3 it can cause significant social embarrassment, especially if the patient has selective anosmia – the inability to perceive odour.3 Bromhidrosis is due to biotransformation of odourless natural secretions into volatile odorous molecules4 and is closely linked with excessive sweating. In the axilla, Corynebacterium in the resident microflora are thought to be important in this biotransformation.
Sudiferous (sweat) glands are divided into eccrine glands, found all over the body, and apocrine glands found in the axilla, breast and groin region. While bacterial metabolism of apocrine sweat usually causes the malodour, eccrine sweating can also become offensive after ingestion of certain foods, such as garlic and alcohol.
Assessment and diagnosis of hyperhidrosis
Hyperhidrosis can be generalised or focal. Generalised hyperhidrosis affects the entire body and may be idiopathic or secondary to an underlying metabolic disorder or systemic disease. A number of conditions that have been associated with generalised hyperhidrosis are listed in Table 1. Most of these conditions can be identified on history and examination. Patients most likely to require further investigation are those who are older, or those with severe hyperhidrosis of recent onset. Investigations that may be helpful are listed in Table 2.
Conversely, focal hyperhidrosis involves specific sites of the body, most commonly the axilla, palms and soles. Focal hyperhidrosis occurs in otherwise healthy patients commonly before the age of 25 years,5 and roughly two-thirds of patients report a positive family history.1 The most common cause of focal hyperhidrosis is primary idiopathic hyperhidrosis; causes are outlined in Table 3. It is important to note that primary hyperhidrosis ceases when sleeping, in contrast to night sweats, which can indicate a serious underlying disorder.
A distinction between generalised and focal hyperhidrosis should be made at the initial assessment. The medical history should be concentrated on:
- location of sweating: general or specific area, unilateral or symmetrical areas
- duration of presentation
- family history of focal hyperhidrosis
- age of onset
- concurrent medical illnesses
- triggers of sweating including anxiety, chewing, eating, temperature.
A diagnosis of idiopathic focal hyperhidrosis can be made on history if the patient is noted to have excessive visible sweating for at least 6 months and two of the following:
- bilateral symmetrical sweating
- impairment of daily activities
- at least one episode per week
- onset before 25 years of age
- positive family history
- focal sweating that ceases during sleep.
If there is no obvious underlying cause on history and examination, and the presentation is characteristic for primary focal hyperhidrosis, then further investigations are not required.
Table 1. Causes of generalised hyperhidrosis
- Endocrine diseases
- menopause*
- hyperthyroidism*
- diabetes**
- hypoglycaemia**
- pheochromocytoma***
- hyperpituitarism***
- carcinoid syndrome***
- Medications*
- propranolol
- tricyclic antidepressants
- cholinesterase inhibitors
- selective serotonin reuptake inhibitors
- opioids
- Febrile infective illness**
- malaria
- tuberculosis
- endocarditis
- HIV (seropositive patients)
- Congestive heart failure**
- Neurological disorders**
- Parkinson disease
- peripheral neuropathies
- brain lesions (eg. malformation of corpus callosum)
- Malignancy***
|
* Uncommon
** Very uncommon
*** Rare |
Table 2. Investigations that may be considered for late onset, recent onset or very severe hyperhidrosis
- Blood tests
- full blood count
- electrolytes and renal function tests
- liver function tests
- thyroid function tests
- HIV serology
- fasting blood glucose level
- Testing for specific infectious diseases as suggested by the history (eg. tuberculosis)
- 24 hour urinary catecholamines
|
Table 3. Causes of focal hyperhidrosis
- Primary idiopathic hyperhidrosis
- Gustatory sweating (sweating after eating or seeing food that produces strong salivation. Chewing can also stimulate sweating)
- Neurological causes
- spinal injuries
- neuropathies
|
Assessment and diagnosis of bromhidrosis
While Staphylococcus, Micrococcus, Corynebacterium and Propionibacterium can be commonly isolated from the resident microflora in people affected by bromhidrosis, bacterial swabs are unlikely to be useful in guiding management.
Triethylaminuria is a rare inborn error of metabolism leading to a distinctive fishy odour.6 Genetic testing is available in Australia, and the condition can be corrected by dietary modification.
Management of hyperhydrosis
Conservative treatment measures have usually been tried and failed by the time the patient consults their GP. There are a number of surgical and non-surgical treatments for focal hyperhidrosis. Management of generalised hyperhidrosis, on the other hand, involves addressing the underlying cause.
Topical therapies for focal hyperhidrosis
Aluminium compounds
While most standard supermarket antiperspirants contain aluminium chloride, higher potency agents may contain aluminium chlorohydrate. Aluminium chloride hexhydrate is significantly more effective again, and should be the first line of therapy. Antiperspirants containing aluminium chloride hexhydrate are sold in pharmacies; a prescription is not required. All of these agents have a common mechanism of action that involves the mechanical obstruction of the eccrine gland duct, which in turn leads to atrophy of the eccrine acini.7
Aluminium chloride hexhydrate is used in a concentration of 20% for axillary hyperhidrosis, while 25% for palmar and plantar hyperhidrosis is usually needed to achieve euhydrosis.8,9 However, a concentration of 10% can be used initially to avoid side effects, including localised skin irritation and a burning sensation. Topical therapy should be applied once daily, usually at night when the skin is dry, for optimal results. The concentration can be increased up to 35%, as tolerated, if there is no response, although patients can rarely tolerate side effects at this strength in the axilla. Associated skin irritation can be controlled with 1% hydrocortisone.
Iontophoresis
Iontophoresis is a specialised treatment only available in some states. It utilises a delivery system for small polar molecules into the skin (Figure 1). Figure 2 and Figure 3 provide a visual comparison for the effectiveness of this therapy. The most effective chemical for hyperhidrosis is glycopyrrolate. Tap water is much less effective, although there are iontophoresis devices available for home use.10

Figure 1. An iontophoresis machine
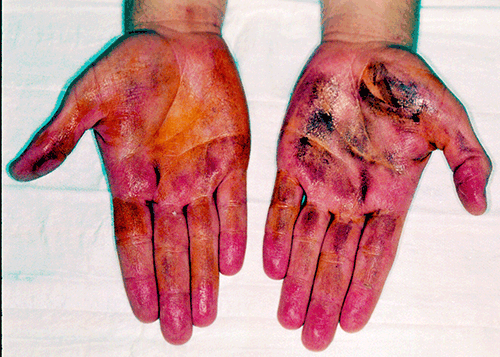
Figure 2. The starch-iodine test. Iodine is applied to a dry area of skin and starch is sprinkled on top. The iodine, starch and sweat react to form the dark sediment. The left palm has not yet been treated with iontophoresis
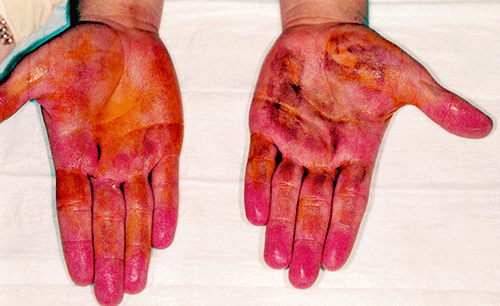
Figure 3. Starch-iodine test after a patient has had iontophoresis to the left palm 7 days earlier. The image demonstrates a reduction in perspiration
Botulinum toxin A
Botulinum toxin A is a highly effective treatment for focal hyperhidrosis. The main mechanism of action is the inhibition of acetylcholine release from the sympathetic nerves that innervate the eccrine sweat glands.11 Medicare subsidises the use of botulinum toxin A for severe primary axillary hyperhidrosis in patients aged 12 years or more who have failed or are intolerant to topical aluminium chloride hexahydrate after 1–2 months of treatment, when administered by a dermatologist, neurologist or paediatrician. The dose for intradermal injections depend on the area, eg. 50–100 U for the axilla. The treatment is highly effective for non-Medicare subsidised use on the palms and soles, although pain during injections can be a limiting factor to its use.
Systemic therapy
There is long term data on the safety and efficacy of anticholinergic use in focal hyperhidrosis. Propantheline bromide and oxybutynin are the most common anticholinergics used. Both are highly effective and relatively cheap. Selective serotonin reuptake inhibitor (SSRI) induced hyperhidrosis also responds well to oxybutynin. Glycopyrrolate is another effective alternative, but expense is a limiting factor for many patients.
The dosage required to control hyperhidrosis invariably results in generalised anticholinergic effects, including dry mouth and eyes, urinary retention and headaches.
Oxybutynin can be prescribed initially at a low dose of 2.5 mg/day and increased progressively up to 10 mg/day until an improvement is seen. This regimen results in fewer side effects.12
The role of surgery
Surgery is reserved for those refractory to medical therapy and in whom the hyperhidrosis is having a significant impact on their activities of daily living. Local excision of the axillary vault may reduce excessive sweating in the axilla. The results, however, can be cosmetically unappealing and scarring can result in functional impairment. Removal of axillary sweat glands using tumescent liposuction has also been shown to be a safe method of reducing axillary hyperhidrosis.13 The cost of this procedure may be a limiting factor for some patients, particularly as there is a risk of relapse of hyperhidrosis.13
Endoscopic thoracic sympathectomy is the last resort for the treatment of palmar, axillary and craniofacial hyperhidrosis. It works by interrupting the fibres of the sympathetic ganglia. While effective, it has many limitations including the $5000+ cost, which can make this unobtainable for many patients. Risks include Horner syndrome, pneumothorax, and compensatory hyperhidrosis, the latter occurring in 67% of patients who have had endoscopic thoracic sympathectomy.14
Management of bromhidrosis
Regular washing and axillary hair removal are helpful. Fragrant antiperspirants are first line treatment in the management of body odour. These reduce the volume of sweating and are also antibacterial. Some deodorants contain specific antimicrobial metal ions or antimicrobial ceramics, including zeolite antimicrobial ceramics and calcium phosphate antimicrobial ceramics that specifically inhibit axillary bacteria.3
Fragrances mask the offensive smell. Some people may develop allergic contact dermatitis to fragrance, although this is uncommon.
Summary
Both hyperhidrosis and bromhidrosis are common and potentially distressing conditions. Sensitive management and appropriate referral may help minimise the impact on the patient’s quality of life at both a social and functional level.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.