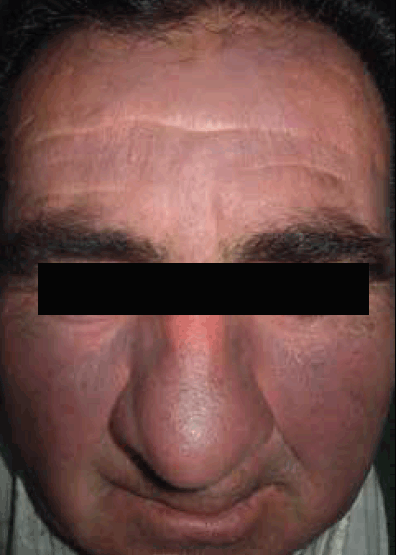
Figure 1. Blue-grey hyperpigmentation on sun-exposed skin of the face
Question 1
What is the most likely diagnosis?
Question 2
What is the differential diagnosis?
Question 3
What skin related adverse effects could occur with amiodarone?
Question 4
What are the treatment options for this case presentation?
Answer 1
The most likely diagnosis is blue-grey discolouration secondary to amiodarone intake. Amiodarone can cause a diffuse blue-grey discolouration affecting the face and, less commonly, other sun exposed areas. Skin folds are spared, as they are less likely to be exposed to the sun. This side effect is relatively uncommon in patients taking amiodarone (1–2% of patients).1
Unlike other causes of blue-grey discolouration, amiodarone related hyperpigmentation does not occur in the oral mucosa, the lunulae of the nails, the hair, or the eyes. Importantly, discolouration can manifest after several months or years of amiodarone intake. The risk factors associated with blue-grey amiodarone related hyperpigmentation are young age, higher daily and total dosages of the drug, duration of treatment, rate of amiodarone metabolism and frequency and intensity of sun exposure.
Answer 2
Differential diagnoses include other medications, adrenal insufficiency, iron and copper storage disorders, heavy metal exposure, and cutaneous metastases of melanoma presenting as generalised melanosis (may appear blue due to the Tyndall effect when melanin pigment is located deep in the dermis).2–7
A careful history of systemic and topical drugs, contact with metals on skin or mucous membranes, or exposure to industrial fumes containing metals4 should be sought. Discolouration due to silver ingested in an alternative medicine preparation has been reported.6 Amiodarone related hyperpigmentation is usually a clinical diagnosis, but if the diagnosis is in doubt, biopsy for histology may be helpful as different metals can be distinguished microscopically by their unique deposition patterns.5
Answer 3
In addition to the possible rare side effect of blue-grey discolouration of sun-exposed areas, amiodarone can cause photosensitivity in more than half of patients.8 Severity of photosensitivity varies widely, from an increased propensity to suntan in the summer months, to sun intolerance on sun-exposed areas with burning sensation, erythema and swelling on exposure. Reduction of amiodarone dosage and photoprotective cream may be useful measures for alleviating symptoms. However, photosensitivity improves with time.
Answer 4
While discolouration due to amiodarone intake is a benign condition, patients are usually concerned with aesthetic appearance. A reduction in dose may be helpful, but in most cases, patients have ceased amiodarone with fading of the discolouration after several months.9 However, there have been some reports of persistence of the discolouration, despite cessation of the drug.9 Q-switched laser therapy has been shown to be an effective treatment for discolouration due to amiodarone.10 Importantly, cardiology review is required before cessation of amiodarone occurs.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.