A 2002 United States survey indicated that most doctors (83%) choose topic areas for continuing medical education programs that constitute a significant part of their regular practice.1 While GPs develop an intuitive sense of the frequencies of the problems that they see, empirical data would be helpful to direct continuing medical education. General practitioners could use the diseases covered in new guidelines and articles from professional publications or journals as a stimulus to guide their learning, if the material matched their frequency-based learning needs. We sought to answer the following two questions:
- What conditions do GPs see most frequently and how many conditions make up 50% of all problems managed by GPs?
- How well do published guidelines and Australian Family Physician (AFP) articles reflect the most common conditions in general practice?
To achieve this, we analysed data from the Bettering the Evaluation and Care of Health (BEACH) program. BEACH is an ongoing cross-sectional survey of general practice activity in Australia, enrolling a new random sample of about 1000 GPs per year. Each GP provides details for 100 consecutive patient encounters.2
Methods
We used BEACH data collected between January 2009 to December 2010, which included 194 100 patient encounters from 1941 GPs. In most cases, we used standard problem groups reported in BEACH.3–5 However, to create more educationally consistent groups, we modified inclusions of six problem groups that fell in the top 200 most frequently managed problems. For example, the usual BEACH grouper for hypertension includes that related to pregnancy. As it is unlikely that an educational session on hypertension would cover pre-eclampsia or gestational hypertension, these encounters were removed from the ‘hypertension’ group and dealt with separately. The changes did not alter the order of the top 30 most commonly managed problems.
We created a centile table from the 200 more commonly managed problems, providing examples of some conditions that occur around landmark centiles (Table 1). Using a subjective estimation of the average number of consultations conducted by a fulltime GP (four patients per hour, with 36 hours per week in direct patient care), we calculated the average management frequency of each condition.
For each of the 10 most commonly managed conditions, we searched the National Health and Medical Research Council (NHMRC) Clinical Practice Guidelines Portal (December 2011) to determine if a relevant Australian guideline existed.6 All guidelines on the portal were eligible for inclusion if they addressed the topic, even if they were not authored for a general practice audience. Using MEDLINE, we searched for all articles published in AFP between 2005 and 2010. Two authors independently reviewed the abstracts to determine how often research and nonresearch articles had been published in AFP about each common condition. Disagreements were resolved by discussion.
Table 1. Diagnostic centile chart for the most frequently managed problems
| Diagnostic centile | Cumulative number of problems managed | Examples of problems that occur at and around this centile* and rank order of each example |
|---|
| 10th |
3 |
Immunisations/vaccination all (2), URTI (3), depression (4) |
| 25th |
9 |
Osteoarthritis (8), back complaint (9), prescription (10) |
| 50th |
34 |
bursitis-tendonitis-synovitis (33), acute otitis media (34), administrative procedure (35) |
| 75th |
102 |
drug abuse (101), mouth/tongue/lip disease (102), vertiginous syndrome (103) |
| 80th |
130 |
Overweight (129), muscle symptom NOS (130), joint symptom NOS (131) |
| 85th |
167 |
Glaucoma (166), cholecystitis/cholelithiasis (167), stroke (168) |
| * Problems highlighted in bold fell at the exact centile; NOS = not otherwise specified |
Results
The 194 100 patient consultations involved 305 738 problems managed; an average of 157.5 problems per 100 encounters. The 167 most frequently managed problems accounted for 85% of all problems managed by the GPs. At least one of these common problems was managed at 90% of all encounters. Only 1 in 10 consultations involved management of less common problems alone.
The top 30 problems accounted for almost half (48%) of all problems managed, three problems accounting for the top 10% and nine accounting for 25% of all problems managed (Table 2).
For illustrative purposes, if an average GP conducts 144 patient consultations per week (four per hour, 36 hours per week in direct patient care), they will manage: hypertension, immunisations/vaccination, upper respiratory tract infection (URTI), depression and diabetes on a daily basis; pregnancy and sleep disturbance about twice per week; menstrual problems and weakness/tiredness (0.7 per 100 encounters) on a weekly basis; psoriasis and diverticular disease (0.2 per 100 encounters) about once per month; transient cerebral ischaemia, syncope and goitres (0.1 per 100 encounters) about seven times per year.
In classifying AFP articles and guidelines, we did not perform searches for the seventh (general check-up) and tenth (prescription: all) problems in the frequency list. ‘General check-up’ could constitute any preventive activity or more formal processes such as routine paediatric screening visits or a health check carried out in accordance with The Royal Australian College of General Practitioners (RACGP) Guidelines for preventive activities in general practice (the ‘red book’).7 Due to the breadth of potential definitions for ‘general check-up’ and ‘prescription’, we did not classify articles into these categories.
Between 2005 and 2010, AFP published 218 research articles and 1270 other articles. The NHMRC Clinical Guidelines portal contained 540 guidelines in December 2011. While hypertension was the most commonly managed problem (accounting for 5.7% of all problems managed), it was under-represented in both research articles (1.8%) and nonresearch articles (0.2%) in AFP, and in the guidelines (0.6%), when compared to how often the problem was encountered. Diabetes was the only problem in the eight investigated that was over-represented in both AFP and guidelines. Depression was the topic of many research articles (7.3%), but was under-represented in guidelines (1.5%) and nonresearch articles (1.2%) (Figure 1).
We noted that there were a larger number of articles on influenza10 than on URTI.3 Similarly, cardiovascular risk was the topic of 10 articles, which we did not classify to lipids or to hypertension.
Table 2. The 30 most frequently managed problems
| Rank | Problem type | Percent of problems
(n=305 738) | Rate per 100 encounters
(n=194 100) | Rank | Problem type | Percent of problems
(n=305 738) | Rate per 100 encounters
(n=194 100) |
|---|
| 1 |
Hypertension |
5.7 |
9.0 |
16 |
Test results |
1.2 |
1.8 |
| 2 |
Immunisation/ vaccination: all |
4.2 |
6.7 |
17 |
Urinary tract infection |
1.1 |
1.8 |
| 3 |
Acute upper respiratory tract infection |
3.3 |
5.1 |
18 |
Dermatitis, contact/allergic |
1.0 |
1.6 |
| 4 |
Depression |
2.9 |
4.6 |
19 |
Pregnancy |
1.0 |
1.5 |
| 5 |
Diabetes: non-gestational |
2.3 |
3.7 |
20 |
Sleep disturbance |
1.0 |
1.5 |
| 6 |
Lipid disorders |
2.1 |
3.4 |
21 |
Sinusitis acute/chronic |
0.9 |
1.4 |
| 7 |
General check-up |
1.9 |
3.0 |
22 |
Gastroenteritis |
0.8 |
1.3 |
| 8 |
Osteoarthritis |
1.7 |
2.7 |
23 |
Vitamin/nutritional deficiency |
0.8 |
1.3 |
| 9 |
Back complaint |
1.7 |
2.6 |
24 |
Malignant neoplasm of skin |
0.8 |
1.3 |
| 10 |
Prescription |
1.6 |
2.5 |
25 |
Abnormal test results |
0.8 |
1.2 |
| 11 |
Oesophagus disease |
1.6 |
2.4 |
26 |
Atrial fibrillation/flutter |
0.8 |
1.2 |
| 12 |
Female genital check-up |
1.5 |
2.4 |
27 |
Oral contraception |
0.8 |
1.2 |
| 13 |
Acute bronchitis/ bronchiolitis |
1.5 |
2.3 |
28 |
Solar keratosis/sunburn |
0.8 |
1.2 |
| 14 |
Asthma |
1.3 |
2.1 |
29 |
Ischaemic heart disease |
0.7 |
1.1 |
| 15 |
Anxiety |
1.2 |
2.0 |
30 |
Viral disease, not otherwise specified |
0.7 |
1.1 |
| |
Cumulative total top 15 |
34.6% |
– |
Cumulative total top 30 |
47.8% |
– |
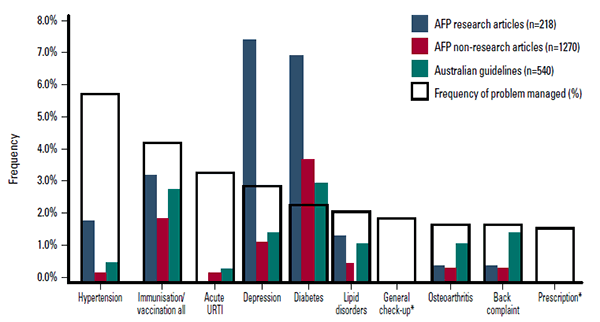
Figure 1. Distribution of common problems managed compared with distribution of publications and guidelines
* No search conducted – see results section
Discussion
A GP must have good working knowledge of 167 problems to cover 85% of the conditions they will see most frequently. Our results suggest that 78% of general practice consultations would require management of only one or more of these 167 problems and another 12% of consultations would require knowledge of one or more rarer problems in addition. One in 10 consultations would deal purely with one of the thousands of rarer conditions.
Of the 10 most common presentations, only diabetes was consistently over-represented in guidelines and AFP research and nonresearch articles. Guidelines for the management of hypertension, the problem most commonly managed in general practice in Australia, were notably infrequent. Four of the six under-represented areas relate to the National Health Priority Areas of arthritis and musculoskeletal conditions and cardiovascular health.
We limited our examination to a single Australian publication, which has a high readership and is targeted to general practice readers, but did not examine research published in other Australian journals (such as the Medical Journal of Australia), or international journals. We also recognise that publication in AFP may not reflect the research submitted to AFP or be a reliable proxy for research being done in a particular area. Another limitation of our study is that we examined the frequency of management of each condition, not burden of disease. Furthermore, we did not attempt to classify AFP articles into ‘general check-up’ and ‘prescription’ categories, as the breadth of potential definitions limited the utility of doing this. This decision did not impact on the results of categorisation of other problems. However, by not categorising ‘general check-up’, the RACGP ‘red book’7 was not counted as a guideline in this category.
The breadth of general practice consultations has been described internationally. Despite different health systems, the range and frequency of problems managed in primary care is similar between the United Kingdom, the US and Australia.8 We are not aware of other research examining clinical guidelines and research publications compared with frequency of problem management, though the disparity between research funding and burden of disease has been documented.9,10
We had expected that the distribution of publications and guidelines would more closely approximate the distribution of consultation frequency, particularly for the most common conditions of hypertension, immunisation and URTI. The existence of a well-publicised, gold-standard guideline may explain why some topics, such as hypertension, have relatively few published guidelines. However, this does not explain why topics are under-represented in AFP research articles. It may be that published research tends to focus on emerging areas, with fewer knowledge gaps existing in more common problems. This would explain why influenza and absolute cardiovascular risk were popular research article topics.
Learning about all diseases is not possible. More than 11 000 conditions are currently described11 with approximately five new diseases being described each week.12 This research will help GPs, general practice registrars and medical students plan their professional development and learning. It will also aid their teachers and medical educators in planning programs and curricula; employing different strategies for the common diagnoses than they do for the rarities. This research has only taken into account problem management frequency in general practice. Future research on this topic should examine serious, but less common conditions, and diseases with a high burden of illness.
Competing interests: None.
Ethics approval: Committees of the University of Sydney and the Australian Institute of Health and Welfare.
Provenance and peer review: Not commissioned; externally peer reviewed.