The main goal in treating T2D is to achieve blood glucose levels as close as possible to the normal range to prevent chronic microvascular and macrovascular complications.3,4 This evidence is recognised by key national bodies, such as Diabetes Australia and the Australian Diabetes Society, which recommend a target HbA1c level of between 6.0 and 7.0%, while also acknowledging targets need to be tailored to the individual patient, especially in the elderly.4,5 Due to the progressive nature of T2D, patients require periodic intensification of blood glucose lowering therapy to continue to meet these targets and eventually most patients will require insulin to maintain target HbA1c levels.6
The aim of the Type2Care clinical audit was to encourage general practitioners to evaluate and optimise their management of T2D patients using a tailored decision support system.
Methods
The Type2Care audit follows The Royal Australian College of General Practitioners (RACGP) clinical audit criteria and involves five steps: needs assessment, audit cycle 1, review and reflection, audit cycle 2, review and reflection. It was a prospective, fixed time clinical audit, whereby GPs evaluated their own management of diabetes in 20 consecutive consenting patients with T2D, irrespective of the reason for the patient seeing the doctor. Following completion of the initial audit (cycle 1), GPs received performance feedback in the form of an individualised report for each patient they audited, which summarised their performance against Australian management guidelines and the audit standards. The GPs also received a decision support tool (Figure 1), which provided a colour-coded overview about the management of all audited patients, highlighting which patients required a review in the near future to address gaps in their diabetes management. After a period of 6 months, a further audit (cycle 2) of the same 20 patients was conducted to assess any change in practice.
Six criteria were identified as performance outcome measures for this audit (Table 1). These evaluation criteria were based on Australian diabetes management guidelines4,5 and the ideal and acceptable standards were determined by consensus from a panel of GPs as part of the audit development process.

Figure 1. Decision support tool used by GPs in the audit
Table 1. Type2Care: clinical audit evaluation criteria
| Clinical audit criteria | Ideal standard | Acceptable standard |
|---|
| 1. All patients with T2D should have a written annual cycle of care plan in their records |
100% |
85% |
| 2. All patients with T2D should have their HbA1c checked at least every 6 months |
100% |
85% |
| 3. All patients with T2D should have an HbA1c of <7% |
100% |
75% |
| 4. All patients with T2D should have their (a) waist circumference and (b) BP checked at least every 6 months |
100% |
85% |
| 5. All patients with T2D should have their (a) serum lipids and (b) microalbumin checked at least every 12 months |
100% |
85% |
| 6. All patients with T2D should meet the established goals for optimum management: |
- Waist circumference
|
100% |
60% |
- Blood pressure
|
100% |
70% |
- Total cholesterol
|
100% |
85% |
- Microalbumin
|
100% |
85% |
| The evaluation criteria and the ideal and acceptable standards were determined by a panel of GPs as part of the audit development process |
Data collection
General practitioners were recruited through advertising in medical publications, on the RACGP website, or by direct mail (from a commercially available mailing list of GPs who worked full-time in a busy practice). General practitioners were provided with quantitative questionnaires and asked to evaluate their management of T2D in 20 patients.
Statistical analyses
All data were captured in an Excel database. Only data from GPs who completed both audit cycles were included in the final analysis. Analysis included basic descriptive statistics and comparisons between cycle 1 and cycle 2 using the Wilcoxon’s signed rank test for paired observations, as normal distribution of the variables could not be assumed. Cycle 1 versus cycle 2 data recorded by each GP constituted a pair. Results were considered statistically significant when p<0.05.
The clinical audit was accredited by the RACGP and the Australian College of Rural and Remote Medicine. Written patient consent was obtained by the GP for each patient who was entered into the clinical audit.
Results
A total of 39 GPs completed the entire audit; 1541 case record forms were completed and were included in the analysis; providing data for 780 patients (cycle 1) and 761 patients (cycle 2). Nineteen patients were not available to be audited in the second cycle, due to relocation or patient death. The average age of the patients audited (at enrolment, audit cycle 1) was 64.8 years and 52.6% were male. Type 2 diabetes was diagnosed in the previous 12 months in 57 (7.3%) patients, between 1 and 5 years previously in 243 (31.2%) patients, between 5 and 10 years previously in 276 (35.4%) patients and more than 10 years previously in 204 (26.2%) patients. Seventy-nine (10.1%) patients smoked cigarettes in cycle 1 and this reduced to 72 (9.5%) in cycle 2. Less than 8% of patients in both cycles reported consuming more than two standard drinks per day; above Australian guideline levels for long term harm.4
An annual cycle of care plan had been initiated in 579 patients (74.2%) in cycle 1 and 674 patients (88.6%) in cycle two (p<0.05). Nearly all patients (>95% in both audit cycles) had been provided with advice regarding diet, exercise and general diabetes self-care. Most patients had also received care from diabetes related healthcare providers (diabetic educators, dieticians, endocrinologists, ophthalmologists, podiatrists) with the use of these resources significantly increasing in cycle 2 (Figure 2).
In cycle 1, height and weight measurements were available in the records of 674 (86.4%) patients. Waist circumference had been measured at some point in 425 patients (54.5%) and in the past 6 months in 353 patients (46.4%). In cycle 2 the recording of height, weight and waist circumference measurements increased significantly (p<0.05) with height and weight available for 698 patients (91.7%) and waist circumferences available for 510 patients (67.0%) with 397 (52.2%) having had this measurement recently taken.
Table 2 summarises the proportions of patients with data recorded and the mean values for measures of blood glucose, blood lipids, blood pressure (BP) and microalbumin. With the exception of microalbumin, all other clinical measurements of interest were available in the records of most patients. HbA1c was recorded in almost all patients (97% and 98% in cycles 1 and 2 respectively); however, this was not a recent measurement as only 80% of patients had their HbA1c measured within the past 6 months for either audit cycle. The assessment of microalbumin increased significantly between audit cycles (p<0.05). The mean recorded values for these clinical measures differed only slightly between the audit cycles.
Most patients were taking medications to manage their diabetes. Oral hypoglycaemic agents (OHAs) were prescribed more frequently than insulin preparations with 77.9% and 79.5% of patients taking OHAs and 13.8% and 14.8% on insulin therapy in audit cycles 1 and 2 respectively. The most commonly used OHAs were metformin and gliclazide, and insulin glargine was the most frequently used insulin therapy, prescribed in half of patients receiving insulin. Between audit cycles there were no significant changes in the proportions of patients being prescribed the different classes of diabetes medications.
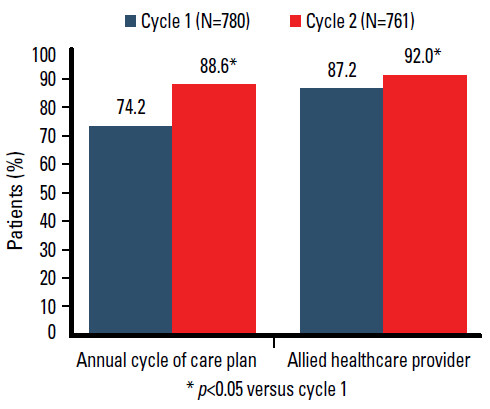
Figure 2. Changes in use of annual cycle of care plans and allied healthcare professionals between audit cycles
Table 2. Recording of clinical measures and mean values in cycle 1 and cycle 2 of the Type2Care audit
| | Audit cycle 1 | Audit cycle 2 |
|---|
| | N | % | Mean | N | % | Mean |
|---|
| Blood glucose |
735 |
94.2 |
7.2 mmol/L |
732 |
96.2 |
7.1 mmol/L |
| HbA1c |
757 |
97.1 |
6.9% |
747 |
98.2 |
6.9% |
| Total cholesterol |
772 |
99.0 |
4.3 mmol/L |
748 |
98.3 |
4.2 mmol/L |
| LDL-C |
772 |
99.0 |
2.1 mmol/L |
748 |
98.3 |
2.1 mmol/L |
| HDL-C |
772 |
99.0 |
1.2 mmol/L |
748 |
98.3 |
1.2 mmol/L |
| Triglycerides |
772 |
99.0 |
1.7 mmol/L |
748 |
98.3 |
1.7 mmol/L |
| Systolic BP |
775 |
99.4 |
132 mmHg |
752 |
98.8 |
131 mmHg |
| Diastolic BP |
775 |
99.4 |
75 mmHg |
752 |
98.8 |
74 mmHg |
| Urinary microalbuminuria: |
612 |
78.5 |
|
665 |
87.4* |
|
| – spot collection |
|
|
30.9 mg/L |
|
|
30.6 mg/L |
| – albumin/creatinine ratio |
|
|
4.8 mg/mmol |
|
|
2.9 mg/mmol |
| * p<0.05 vs cycle 1 results |
GP performance vs standards
The mean GP performance for each of the audit criteria is shown in Figure 3. Performance in the first audit cycle was lower than expected, achieving the acceptable standard in only three domains: criterion 3 (at least 75% of patients having a HbA1c ≤7.0%), criterion 4b (at least 85% having their BP checked every 6 months) and criterion 5a (at least 85% having their serum lipids measured annually).
Mean GP performance in the second audit surpassed the acceptable standards in six of the 11 domains. Compared to cycle 1, in cycle 2 there were statically significant improvements in four domains – annual cycle of care plans, checking of urinary microalbuminuria, meeting established goals for waist circumference and meeting established goals for urinary microalbuminuria.
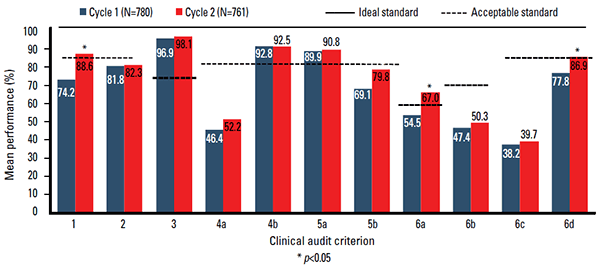
Figure 3. Mean GP performance vs standards
Discussion
Delivery of care to T2D patients was significantly improved during the Type2Care clinical audit. The use of management guidelines, decision support tools and patient registers in the treatment of T2D can lead to improved patient outcomes. These findings are supported by previous studies that have shown that diabetes related patient outcomes were improved by interventions such as initiation of multidisciplinary care,7 provision of integrated support programs and guidelines8 and use of diabetes registers.9 Our findings indicate that GPs could improve clinical outcomes by reviewing their current management processes and embedding existing tools, such as patient registers and care plans, into routine clinical practice for all patients with T2D.
The main goal in management of T2D is to achieve blood glucose levels close to accepted Australian Diabetes Society guideline targets to prevent complications.4,5 The pre-audit standard of care with respect to glycaemic control was excellent as reflected by the very high proportion of patients with HbA1c levels at target. This result could be due to a selection bias, in that the audit may have attracted GPs with a strong interest in diabetes and hence management practices among these GPs may not be representative of the wider GP practice. The level of glycaemic control may also reflect advances in pharmacotherapy, such as the availability of basal insulin, which enables easier use of insulin for patients when diabetes progresses and oral agents alone are no longer adequate.10
While this audit intimated that all patients with T2D should have an HbA1c <7.0%, it should be emphasised that the target HbA1c needs to be individualised, where appropriate.5 Extra care needs to be taken when establishing HbA1c targets in the elderly and those with increased risk of cardiovascular disease.
The management of patient weight and lifestyle should be improved. Although the proportion of patients who had their waist circumference measured in the past 6 months showed minor improvement during the audit, the recording and education around this key metric occurred in just over half of the audited patients. Clinical trials have demonstrated that more intensive control of HbA1c is associated with increased weight gain,5 thus GPs initiating more intensive therapy to lower HbA1c should also ensure that healthy lifestyle factors such as weight loss/weight maintenance are also addressed.
Patients in this audit were just above targets for BP and serum cholesterol levels. There were slight improvements observed in these parameters during the audit process. With the increased use of annual cycle of care plans, there is potential for further clinical improvements on these measures.
The main limitation of this study is that GPs were self-selected. This may have contributed to the small number of GPs completing the audit and inadvertently led to a recruitment bias as the GP group may have had an especially strong interest in the management of diabetes. There was a high dropout rate of GPs between audit cycles 1 and 2. This rate is consistent with other published Australian GP clinical audits11,12 and may reflect the time pressures on GPs. Combined, these factors indicate that the findings of this audit may not be representative of the wider GP workforce.
Conclusion
The provision of the Type2Care clinical audit and associated decision support tools and disease registers improved the delivery of care to T2D patients. This is reflected in the increased use of annual cycle of care plans, improvements in monitoring key clinical parameters and increased utilisation of allied healthcare professionals to support patient management. Although significant changes in clinical parameters would not be expected over such as short time frame, some positive changes were observed. Our results demonstrate the usefulness of audits in improving GP management of chronic diseases.
Implications for general practice
- The use of clinically based decision support tools and diabetes registers can improve the delivery of care and corresponding clinical outcomes in patients with T2D.
- A narrow focus on reaching individualised HbA1c targets does not ensure optimal care. Lifestyle and comorbid conditions need closer focus.
Competing interests: Scius Solutions received payments from Sanofi Australia Pty Ltd to develop, manage and analyse this audit and for the writing of this manuscript. Scius Solutions provides communication services and has developed educational presentations for a number of pharmaceutical companies. John Barlow has received payments from several pharmaceutical companies for consultancy.
Ethics approval: BellBerry Human Research Ethics Committee, Ashford, SA.
Provenance and peer review: Not commissioned; externally peer reviewed.