Case study
A man, 77 years of age, presented with haematemesis, abdominal pain and increasing limb weakness. He also had a skin rash on his chest and face. On further questioning, he revealed that the rash had been present for 5 years and had previously been diagnosed as eczema. It had been treated for a time with topical steroids, but had responded poorly.
Clinical examination showed proximal muscle weakness and skin changes including erythematous violaceous plaques in the periorbital region associated with oedema of the eyelids and periorbital tissue (Figure 1), confluent violaceous erythema of upper chest, neck and back with evidence of poikilodermatous skin changes (Figure 2, 3) and periungual telangiectasia (Figure 4). Poikilodermatous skin changes include hyperpigmentation, telangiectasia and atrophy resulting in a mottled appearance. Skin biopsy showed mild atrophy of the epidermis with vacuolar changes in the basal keratinocyte layer and a perivascular lymphoid infiltrate in dermis. Creatinine kinase was increased at 947 U/L (normal range 38–174 U/L). Gastroscopy revealed a stage IV gastric adenocarcinoma.
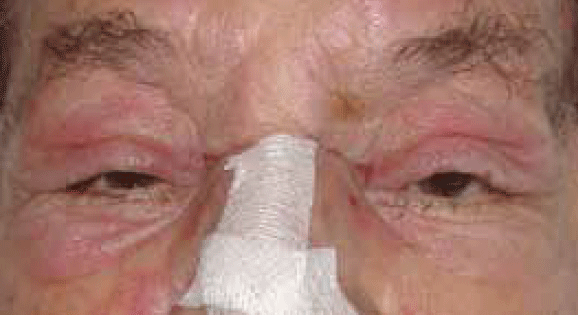
Figure 1. The patient's periorbital rash
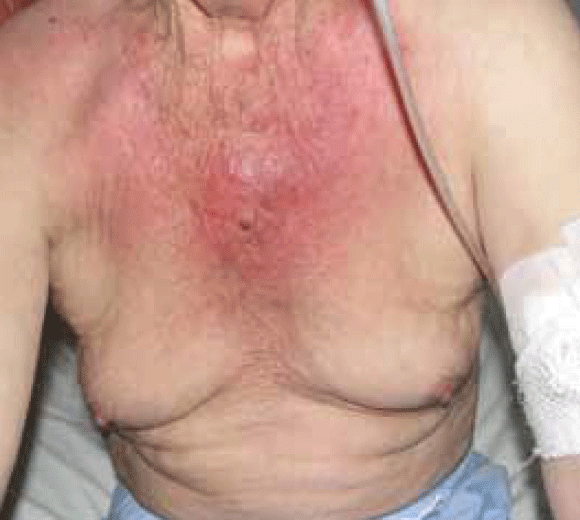
Figure 2. Rash seen on the patient's trunk
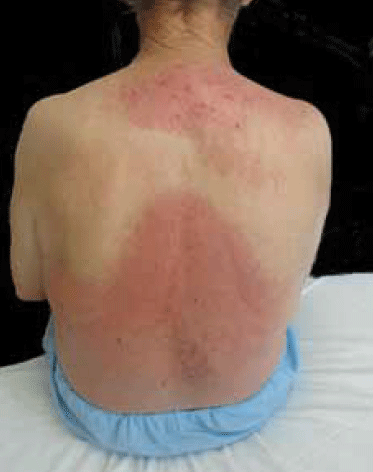
Figure 3. Rash seen on the patient's back
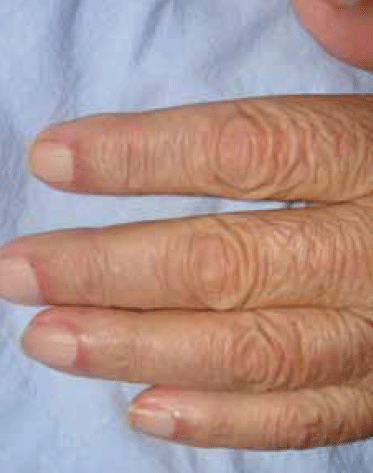
Figure 4. Periungual telangiectasia
Question 1
What is the most likely diagnosis of the patient’s skin rash?
Question 2
What are the typical skin findings in this disease?
Question 3
Is there any relationship between this disorder and the diagnosis of a gastric tumour in this patient?
Question 4
What are the treatment options for this condition?
Answer 1
The patient has the hallmark cutaneous manifestations of dermatomyositis combined with muscle weakness. The likely diagnosis is classic dermatomyositis. This is a form of idiopathic inflammatory myopathies (IIM), which is a heterogeneous group of genetically determined autoimmune disorders that predominately target the skeletal musculature and/or skin.
Answer 2
Several distinct rashes occur in dermatomyositis. These are outlined in Table 1.1–3 Importantly, the V and shawl signs can be can be confused with other photodermatoses or sunburn. To help discriminate between these two causes it is important to enquire if there is any seasonal pattern and about any exposure to potential photosensitisers. On physical examination, careful attention should be paid to the distribution of the lesions and whether there is sparing of photoprotected areas, eg. postauricular and submental areas, nasolabial folds, above the upper eyelid and covered areas of the trunk and upper arms.
Table 1. Cutaneous signs of dermatomyositis1–3
| Sign | Clinical features |
|---|
| Psoriasiform changes in scalp |
Scaly erythematous plaques in the scalp |
| Heliotrope rash |
Violaceous upper eyelid eruption often associated with periorbital edema (Figure 1) |
| Erythroderma |
Scaling and erythema of more than 90% of the surface area of the skin |
| Shawl sign and V sign |
Erythematous plaque affecting the posterior neck and shoulders (shawl sign) and/or the anterior neck and chest (V sign) |
| Flagellate erythema |
Violaceous streaks on the trunk |
| Gottron’s sign |
Scaly and erythematous dermatitis on the dorsum of the hand over the metacarpophalangeal and interphalangeal joints |
| Mechanic’s hands |
Roughening and fissuring of the skin on the palm and radial surface of the fingers |
| Periungual abnormalities |
Abnormal capillary nailbed loops (alternating areas of dilatation and dropout and periungual erythema) |
| Calcinosis cutis |
Whitish skin nodules with stony consistency |
Answer 3
This was confirmed in population based studies in Sweden4 and elsewhere.5 The close relationship is thought to be a paraneoplastic process involving a link between oncogenesis and autoimmunity.6
Answer 4
If the dermatomyositis is associated with malignancy, the best treatment is to treat the tumour directly, with resolution of dermatomyositis in most cases. Treatment for dermatomyositis is outlined in Table 2.
For skin disease, hydroxychloroquine and chloroquine have been beneficial in small, open-label case studies7 and methotrexate8 and mycophenolate mofetil have been reported to be useful. Rituximab has also been used for skin disease, but the results are mixed.9 Intravenous immune globulin has been shown to have benefit in treating muscle disease as well as clearing skin lesions in the patients in whom it was used.10
Table 2. Treatment of dermatomyositis6–9
| Muscle involvement |
Systemic corticosteroids (0.5–1.0 mg/kg body weight
per day) ± immunosuppressive agents |
| Cutaneous involvement |
First line therapy
- Explain to the patient that they are photosensitive and should avoid sun exposure and use sun protective measures, including broad spectrum sunscreens
- Topical corticosteroids and topical tacrolimus
Second line therapy
- Hydroxychloroquine
- Methotrexate
- Mycophenolate mofetil
- Other immunosuppressive agents
|
Conflict of interest: none declared.