Excessive daytime sleepiness (EDS) is a common presentation to general practitioners and sleep physicians. Excessive daytime sleepiness can adversely affect quality of life and also impair mood, personal relationships and functional status. Although a common presentation, EDS may be under recognised. In the 2000 Sleep Foundation Gallup Survey conducted in the United States, 20% of respondents reported that daytime sleepiness interfered with their daily activities, 8% fell asleep at work and 19% made errors at work because of sleepiness, yet 61% of the respondents reported their primary physician had never asked how well they slept.2
In a comprehensive survey, 16% of respondents reported sleeping too much (primary hypersomnia), 30% showed sleepy behaviours all day, 15% had night time awakenings followed by EDS and 2.5% experienced problems with work.3
Excessive daytime sleepiness caused by chronic sleep deprivation has been implicated in major catastrophes, including the Exxon Valdez oil spill and the space shuttle Challenger explosion.4
Sleep apnoea, chronic insomnia and parasomnias may affect cardiovascular, neurological and psychiatric status of sufferers, leading to increased morbidity and even mortality in severely afflicted patients.5
Excessive daytime sleepiness is not only a personal health issue but also a public safety concern, meaning that it is important to be able to accurately screen and identify EDS and provide proper treatment.
Common causes of EDS include sleep related breathing disorder, insufficient sleep time, circadian rhythm disorder and shiftwork, psychiatric disorders, restless leg syndrome, medication effect, narcolepsy, idiopathic hypersomnia (with or without long sleep time) and various related medical conditions.6,7 In comparison with narcolepsy, which is characterised by an abnormal propensity to fall asleep, idiopathic hypersomnia with long sleep time can be viewed as an inability to terminate sleep. Idiopathic hypersomnia without long sleep time could belong to the spectrum of narcolepsy.
Clinical evaluation
History taking
The most important step in evaluating EDS is a detailed history from the patient and their family members. Snoring, witnessed apnoea, excessive sweating, gasp arousals, nocturia and choking or coughing while asleep are suggestive of sleep related breathing disorder.
The history should include total sleep time during the week days and ‘catching up on sleep’ on weekends. The use of the snooze function on alarm clocks can be indicative of sleep inertia and insufficient sleep.
Patients who do shiftwork and those who frequently travel in different time zones (jet lag effect) experience sleepiness as a normal physiological response to the time of day. Many shiftworkers develop chronic partial sleep restriction and may experience somnolence even when they are on a daytime schedule. Consider the patient’s work schedule, including working hours per day and fixed versus rotating schedules. If they have a rotating schedule, ascertain whether the rotations are weekly or monthly, and forward versus backward.
A long commute to work can significantly shorten sleep duration and can cause chronic partial sleep deprivation. The use of tactics while driving to stay awake, such as rolling the windows down, playing loud music, snacking and even slapping oneself, are all indicative of EDS.
Restless leg syndrome can be diagnosed by the history alone. Restless leg syndrome is characterised by disagreeable leg sensations that usually occur before sleep onset, an irresistible urge to move the limbs, and partial or complete relief from discomfort upon leg movements. These symptoms can lead to significantly reduced sleep time, leading to daytime sleepiness.
Adverse effects of many medications can also result in EDS. Such medications include analgesics, antidepressants, benzodiazepines, antipsychotics and beta-blockers. In addition, common over-the-counter drugs such as antihistamines can have the same effect. The current or past use of recreational drugs, including alcohol, should be discussed. Sudden withdrawal from stimulants such as cocaine or amphetamines can also cause significant sleepiness.
Ask about sleep paralysis, cataplexy, hypnogogic hallucinations and sleep attacks (irresistible desire to sleep). In addition, the history should include asking about the irresistible need for naps throughout the day and whether the naps are refreshing or not. A diagnosis of narcolepsy should be considered in sleepy patients with a clear history of cataplexy. In patients with idiopathic hypersomnia, naps are not refreshing; whereas in narcoleptics, short naps can be effective.
Physical examination
The physical examination of a patient should include measurement of body mass index and neck circumference. Examine the oral cavity for tongue size and note the presence of a narrow arched palate, tonsillar hypertrophy, retrognathia, micrognathia and crowded oral pharynx. Nasal septum deviation, allergies, swollen turbinates and nasal polyps are risk factors for sleep related breathing disorder. The Mallampati classification is very helpful in evaluating airway size.8 It has been shown that a high Mallampati score and nasal obstruction are risk factors for obstructive sleep apnoea (Figure 1).9,10
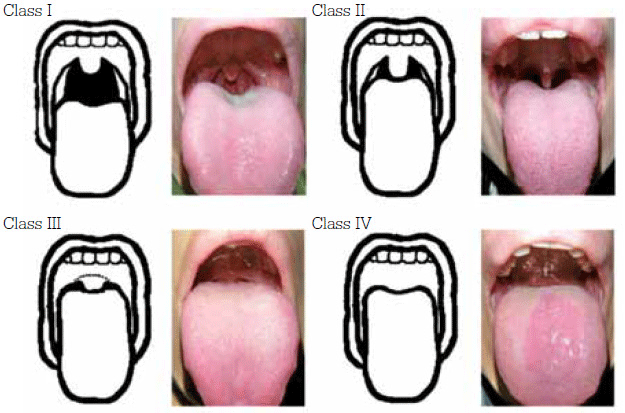
Figure 1. Mallampati classification of upper airway
Adapted from Huang H, et al. BMC Gastroenterology 2011, 11:12 doi:10.1186/1471- 230X-11-12, under the terms of the creative commons attribution license
Measures of sleepiness
It is very hard to quantify sleepiness, either subjectively or objectively, however some methods have been developed to attempt to determine the severity of a patient’s sleepiness. Another limiting factor is the fact that sleepiness is not well defined. It is difficult to differentiate chronic fatigue from excessive sleepiness. There are some subjective and objective assessments of propensity to fall asleep or ability to stay awake.
Subjective
Epworth Sleepiness Scale
First described by Johns in 1991, the Epworth Sleepiness Scale (ESS) is one of the most frequently used tools to assess sleepiness.11 The questionnaire describes eight situations:
- sitting and reading
- watching television
- sitting inactive in a public place
- as a passenger in a car riding for an hour without a break
- lying down to rest in the afternoon when circumstances permit
- sitting and talking with someone
- sitting quietly after lunch without alcohol
- being in a car while stopped for a few minutes in traffic.
The patient will score each situation on a scale of 0–3 (0 = would never doze; 1 = slight chance of dozing; 2 = moderate chance of dozing and 3 = high chance of dozing). A total score of 11 or more is suggestive of EDS.
Being subjective, this instrument has a wide margin of error and patients’ motivation should be considered when analysing the results: for example, is the patient trying to get their driver’s licence reinstated?
While the ESS may not correlate well with objective measurements, it is still widely used and has proven to be an effective screening tool.11
Note that ESS results do not always accurately reflect severity of the underlying condition and should be followed up with objective tests.12
Stanford Sleepiness Scale
While the Epworth Sleepiness Scale measures overall propensity to fall asleep during various mundane activities, the Stanford Sleepiness Scale measures the current state of sleepiness. It consists of the following seven statements:
- Feeling active, vital, alert or wide awake
- Functioning at high levels, but not at peaks; able to concentrate
- Awake, but relaxed; responsive but not fully alert
- Somewhat foggy, let down
- Foggy; losing interest in remaining awake; slowed down
- Sleepy, woozy, fighting sleep; prefer to lie down
- No longer fighting sleep, sleep onset soon; having dream-like thoughts.13
The patient chooses the statement that most accurately describes their current state of sleepiness. The advantage of the Stanford Sleepiness Scale is that it can be administered multiple times during the day; however the disadvantage is that it cannot differentiate between acute sleep deprivation and an underlying sleep disorder.
Karolinska Sleepiness Scale
Another instrument, which is very similar to the Stanford Sleepiness Scale, is the Karolinska Sleepiness Scale. This questionnaire requires the patient to choose one statement that best describes his or her current state of alertness. The detrimental states of alertness are classified as: extremely alert, very alert, alert, rather alert, neither alert nor sleepy, some signs of sleepiness, sleepy/no effort to stay awake, very sleepy/great effort to keep awake/fighting sleep.14
Karolinska and Stanford sleepiness scales are measures of state (immediate) sleepiness. They are probably less useful when administered while the patient is at the clinic; a measure would be more useful if it reflected sleepiness while driving or probed a more general ‘trait’, like degree of sleepiness.
Sleep diary
A patient’s sleep diary can give insight into the cause of the patient’s sleepiness. The patient is asked to maintain this log for 2 weeks, recording bedtime, wake time, number of arousals, time it takes to return to sleep after an arousal, the use of a sleep aid, and any other relevant symptoms. It is particularly helpful for identifying sleep fragmentation, insufficient sleep time, circadian rhythm sleep disorder and insomnia.
Objective measures of sleepiness
Polysomnogram
A polysomnogram (PSG) is performed to rule out obstructive sleep apnoea as the cause of sleepiness. The PSG typically includes an electroencephalogram (EEG), electro-oculogram, electromyogram, electrocardiogram, respiratory channels and oxygen saturation. An Apnoea-Hypopnea Index (AHI) of more than 15 per hour of sleep is diagnostic for a sleep related breathing disorder. Although not indicated for restless leg syndrome, the PSG can help identify periodic limb movements as a cause of sleep disruption. A PSG is also done a night before a Multiple Sleep Latency Test to ensure the patient achieved an adequate amount of sleep.
Multiple Sleep Latency Test
A Multiple Sleep Latency Test (MSLT) is primarily indicated for evaluation of narcolepsy and idiopathic hypersomnia. The MSLT assesses the patient’s propensity to fall asleep. The test consists of five 20 minute nap opportunities. An overnight PSG, performed the night before, is required to ensure the patient attained adequate sleep. The first nap is 1.5–3 hours after the PSG, with each subsequent nap taken 2 hours apart. Sleep latency is calculated by averaging the time from lights out to sleep onset during each nap period. In addition, the occurrence of rapid eye movement (REM) sleep during the 20 minute nap period (sleep onset REM period, or SOREMP) should also be noted. Sleep latency greater than 11 minutes is considered normal. Sleep latency of less than 8 minutes can be seen in patients with idiopathic hypersomnia. However, a mean sleep latency of less than 8 minutes with the presence of two or more SOREMPS is highly indicative of narcolepsy. The trends for sleep propensity appear to be identical in narcoleptic patients with or without cataplexy.15,16
Objective measures of wakefulness
Maintenance of Wakefulness Test
Whereas the MSLT tests the propensity to fall asleep, the Maintenance of Wakefulness Test (MWT) assesses the ability of an individual to stay awake. It is often done to verify the effectiveness of therapy in which sleepiness can be a significant public health risk, such as in the airline and trucking industries. The MWT protocol consists of four 40 minute nap periods, conducted 2 hours apart. Performing a PSG a night before the test is not required. The patient sits in a semi-reclined position in a dim, quiet room and is asked to stay awake; a mean sleep latency of less than 8 minutes is considered abnormal. An MWT value between 8 and 40 minutes is inconclusive and is of uncertain significance.13,15–17
The 'steer clear' reaction time
In this test a two lane street is shown on the computer screen. The patient is asked to press a button to avoid obstacles that appear randomly in either lane during the 30 minute test period. Instead of measuring reaction time, the number of ‘hits’ are counted and presented as a percentage of all obstacles encountered.18
Pupillometry
The size of one’s pupil is controlled by inputs from the parasympathetic and sympathetic nervous systems. In a state of drowsiness the parasympathetic tone predominates, resulting in miosis, while in a state of arousal there is increased sympathetic tone. A well-rested person is able to maintain a stable pupil size without much oscillation in 15 minutes of total darkness. Pupil size and stability are inversely related to the degree of sleepiness. Presently, pupillometry is not used widely in clinical practice. Being a portable, brief and objective measure, this test should not be undervalued and further research is necessary to determine the role of pupillometry in the assessment of sleepiness of various origins.18,19 Other ocular based measures of sleepiness such as those measuring eyelid drooping are being applied mostly in research settings.
Oxford Sleep Resistance Test
The Oxford Sleep Resistance Test can be used as a surrogate for the MWT. Behavioural elements are used in lieu of an EEG to determine sleep onset. The subject is asked to respond to a flash of light lasting 1 second, which lights up every 3 seconds. Sleep onset is defined as the failure to respond to the light for seven consecutive illuminations.18,20 The test is performed in four 40 minute sessions held 2 hours apart.
Summary
Excessive sleepiness is a common condition that has a significant public safety risk. Insufficient sleep and chronic sleep deprivation secondary to sleep related breathing disorder are the two most common causes of hypersomnia.
People with tight shiftwork schedules, intentional chronic sleep restriction, witnessed sleep apnoea or self reported nonrefreshing sleep with subjective daytime sleepiness may be patients who are at an increased risk of motor vehicle accidents and work related injuries, as well as significant cardiovascular diseases and mood disorders. Patients suspected to have this increased risk should be carefully evaluated by general practitioners and then, if deemed needed, referred for further assessment.
Subjective measures to assess sleepiness are good for screening. However, they should not replace a detailed history and physical examination. Some screening tools can be used for sleepy patients in primary care, such as the sleep diary; the Epworth, Karolinska and Stanford Sleepiness scales; and the Oxford Sleep Resistance Test. The Oxford Sleep Resistance Test, for instance, can be used as a surrogate for the MWT, which will reduce the burden on overloaded sleep laboratories.
It often becomes mandatory to conduct evaluation in a sleep laboratory (eg. using PSG, MSLT and MWT) to obtain an accurate diagnosis and appropriate therapeutic intervention.
Conflict of interest: none declared.