As a medical student, I remember feeling that once the diagnosis was made, uncertainty was over and our task then involved following the evidence based guideline to achieve a satisfactory clinical outcome. Arthur Frank would call this approach a restitution narrative:1 symptoms lead to diagnosis, diagnosis leads to evidence based guidelines, guidelines suggest remedies and remedies lead to the restoration of health. The restitution narrative underpins much of Western medicine, and serves us well in acute and serious disease. It also forms the basis of many of the medical stories we hear in the media. The medical sleuths on popular television programs usually struggle with the mysteries of diagnosis, rather than the complexities of management.
However, the model of categorical diagnosis being the core to management begins to break down in chronic disease, where the illness experience becomes progressively more important than the name of the disease. When treatment has been commenced and stabilised, coping becomes central to illness management and concepts like treatment adherence, lifestyle management and monitoring become central to ongoing care. Diagnosis is even less helpful when the illness has no name, as in so-called medically unexplained symptoms.2 In patients with complex chronic illness and poor mental health, which may include a history of trauma, disease classification is only a partial view of what is going on.
Sadler, a psychiatrist who has written extensively on values and psychiatric diagnosis3 believes that diagnosis has a core ethical role: that a ‘good’ diagnosis is clinically useful. He describes different types of diagnosis using the metaphor of botany and gardening. For the botanist, classification produces a taxonomy that is rigorous and reliable. For the gardener, diagnosis informs the way a garden is developed and nurtured in a specific context. Both perspectives are important to achieve a good clinical outcome.
The role of diagnosis in complex general practice presentations
In the complex and uncertain world of primary care, general practitioners often manage patients with an array of distressing physical and psychological symptoms. In attempting to make sense of these symptoms, GPs use three types of diagnosis: the medical diagnosis, the psychosocial formulation and the psychiatric diagnosis (Figure 1). Each diagnosis may be categorical, such as ‘noninsulin-dependent diabetes’ or involve more descriptive frameworks such as ‘an adult survivor of childhood sexual abuse’. These descriptions overlap and intersect, creating a picture of the illness from several different points of view. An example of this approach is shown in Table 1.
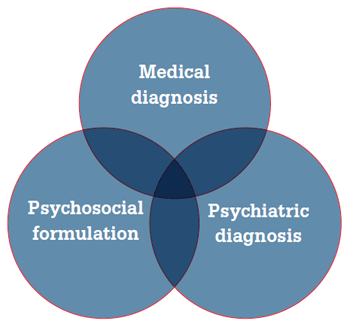
Figure 1. Types of diagnosis in general practice consultations
Table 1. The application of diagnostic frameworks to a specific patient
| This example highlights the benefits of acquiring experience in different therapeutic frameworks. Helpful frameworks are clinically useful, not just accurate |
Example
A woman, 49 years of age, is a carer for her mother and her intellectually disabled adolescent son. She emigrated with her family from India 2 years before. She presents with a depressed mood on a background of diabetes |
Possible diagnostic frameworks
- Disease classification systems (such as DSM-IV* or guidelines for the diagnosis and treatment of diabetes)
- Models learned in clinical education (such as the Black Dog Institute model of depression†)
- Psychological frameworks (such as interpersonal therapy concepts, or cognitive behavioural models)
|
Author’s formulation
- Medical diagnosis: Poorly controlled noninsulin-dependent diabetes and obesity
- Psychosocial formulation: ‘A middle aged woman who is overwhelmed with her caring responsibilities. She lives with her mother, who has early dementia, and her intellectually disabled adolescent son, as well as her three other children and her husband. Culturally, there is an expectation that she will assume full responsibility for caring and there is little support available to her from within the family. She is also isolated in her community because she has limited English and is naturally shy and anxious. At this time, she has become depressed because she is overwhelmed by the complex care needs of her family and doesn’t have resources to deal with them’
- Psychiatric diagnosis: Major depressive disorder (DSM-IV) or nonmelancholic depression (Black Dog Institute model)
|
| * American Psychiatric Association 200025 † Black Dog Institute26 |
The medical diagnosis
It is essential to diagnose or exclude serious disease in any assessment of patients in the general practice context. This type of diagnosis is what Sadler would call a ‘botanical’ one.3 Botany is a categorical science, where each plant has a unique name. Disease classification is a categorical process and is important to direct evidence based management of specific conditions.
The psychosocial formulation
While every patient brings their own psychosocial context to the consultation, not every patient is psychologically ‘unwell’. A psychosocial formulation is a way of understanding and describing why this patient in this context is unwell at this time.
Sadler compares this type of understanding to gardening. The goal of a gardener is to grow a garden, not just describe it. They must assess the context, the relationship of each plant to other plants, and a garden’s purpose, function and aesthetics. They bring to this undertaking mastery of certain skills, experience in different types and schools of gardening and knowledge of their local environment.
Similarly, each GP brings to each consultation cultural understanding, local knowledge, familiarity with patients and their families and various models and methods they have acquired throughout their professional lives. There is never enough time for a GP to acquire the breadth of potentially useful ideas and theoretical frameworks they could apply in practice: they must do the best they can with what they have. Their approaches are always influenced by the time in which they trained and in which they work, their own personality and personal preferences, their values and beliefs and the opportunities they have had to learn along the way. The psychosocial formulation will reflect the differences between practitioners: individual health professionals will ‘formulate’ a patient’s issues in different ways (Table 1).
The psychiatric diagnosis
The psychiatric diagnosis utilises both ‘botany’ and ‘gardening’. Some psychiatric disorders, such as schizophrenia, clearly fit within a disease or ‘botanical’ model, but many psychiatric disorders are not so clear cut. For instance, there is some controversy around the distinction between depression and normal sadness,4,5 with some writers accusing the medical profession of ‘medicalising misery’ by trying to turn sadness into a disease.6
There is also some controversy around the relationship psychiatric disorders have with the self. Kraus7 suggests that psychiatric disorders are not ‘real’ in the same way that a broken leg is real, because they are based, to a large extent, on the subjective experience of the sufferer. One does not ‘have’ schizophrenia in the same way one ‘has’ a somatic disease, because it is always also ‘a kind of being’.7 In response to these issues, modern psychiatry has evolved to describe a psychiatric disorder by using both a categorical diagnosis (such as depression) and a formulation describing the context around the disease (Table 1).
Comorbidities and 'blended' diagnoses
Medical and psychiatric diagnoses
Medical and psychiatric disorders often coexist, but the relationship between them differs. In some cases, the two conditions may be unrelated. In others, a patient may suffer one disorder as a consequence of the other: treatment of psychosis with atypical antipsychotics may lead to weight gain and then type 2 diabetes. Sometimes the nature of the relationship remains unclear, such as the relationship between depression and Parkinson disease, or anxiety and asthma.
Medical disorders and psychosocial formulations
Medical disorders and psychosocial dysfunction commonly interact. Medical disorders can bring disability, financial cost, disfigurement and other forms of psychosocial stress. Any of these stresses can overload a person’s capacity to cope, and destabilise a previously functional system: what David Clarke calls ‘demoralisation syndrome’.8–10 Illness can also precipitate existential crises, with patients facing their own mortality or grieving for their losses.11
On the other hand, patients managing a life of poverty, or abuse, or other forms of chronic trauma, face a higher incidence of medical illness. The aetiology is not always clear. Lifestyle issues, such as poor nutrition, poor access to health services or physical neglect are associated with increased rates of chronic disease12 but patients with long term psychosocial stress, such as those with a history of childhood trauma, also experience higher rates of medically unexplained symptoms and disability.13–15
Psychiatric disorders and psychosocial formulations
Patients with psychiatric disorders also experience significant losses, which affect their psychosocial health and function. The social cost of the stigma surrounding mental illness, along with reduced inability to work and chronic stress within relationships, can lead to ongoing psychosocial trauma.16 Psychosocial issues can also affect the likelihood of acquiring a psychiatric disorder and accessing appropriate care. Poverty significantly reduces access to psychiatric and psychological treatment, as does geographic isolation and barriers due to language, literacy or intellectual capacity.12 Certain patient groups, such as carers, veterans, refugees and victims of interpersonal violence have an increased risk of developing psychiatric disorders.17–20 Patients may also manifest patterns of relating that are unhelpful and damaging, stemming, for example, from a lifetime of abuse and trauma.
Trauma and biopsychosocial suffering
This area includes diagnoses and descriptors such as somatisation disorder, functional disorders and medically unexplained symptoms, which represent an attempt at ‘botanical’ classification. It also includes doctor-centred classification systems, such as ‘heartsink patients’, which focus on our own discomfort rather than a patient’s symptoms. The confusion of terminology and concepts reflects our lack of a clear diagnostic framework. ‘There is no modernist clinical category for “living a life of overwhelming trouble and suffering”.’1 Table 2 provides an example of using different diagnostic frameworks.
This is a frustrating area for doctors, patients, carers and families. Without a name, GPs struggle to find a direction for their therapeutic effort and patients find it difficult to make sense of their illnesses: they can’t find others with a similar experience and may describe how friends, relatives and even health professionals discount their suffering.21–23 As Broyard writes, ‘nobody wants an anonymous illness’.24
This is the point at which who the person is becomes more important than what the person has. The challenge for doctors and patients is to live with the uncertainty and cope with the suffering. Arthur Frank describes this as the ‘chaos narrative’: a story of suffering that does not lend itself to restitution. These patients can make GPs feel very uncomfortable: their troubles are ‘too complex in both medical and social terms for fixing’.1
In this circumstance, it can be tempting to focus on a psychiatric disorder model to define their illness: with a diagnosis such as depression we can reinstate the restitution narrative and we know what it is we are trying to do. As Frank would say, ‘it is very tempting to try to drag the patient out of their own story to make ourselves feel comfortable and effective’.1
Table 2. Whose diagnosis is it anyway?
| In every consultation there are multiple possible perspectives. In complex encounters it can be helpful to look at the interaction with the patient from these different points of view and using different diagnostic frameworks |
Example
A patient with a past history of childhood sexual abuse and subsequent difficulties in establishing and maintaining positive relationships |
The doctor’s diagnosis
This is the diagnosis that we hold in our heads, and that guides our clinical reasoning reason and therapeutic effort. If we understand the symptoms to be part of borderline personality disorder (BPD) it may lead us to recognise our patient’s fears of abandonment and help us manage boundaries effectively |
The patient’s diagnosis
Patients will have their own understanding of why they are unwell that at this time and it may be helpful to draw upon this understanding in the consulting room. For example, we may work with a narrative diagnosis with our patients describing how their childhood trauma has affected their ability to make and maintain healthy relationships. This helps the doctor and the patient to examine patterns in relationships that are destructive, without the stigma associated with the BPD label |
The diagnosis for other health professionals
Some labels carry professional stigma, which can prejudice future care. Borderline personality disorder is one such example. We don’t necessarily share this diagnosis with other health professionals, perhaps describing our patient as ‘a victim of childhood sexual abuse with ongoing relationship issues and associated depression’ |
The diagnosis for third parties
The effect of diagnosis can be fraught when we are dealing with insurance companies or employers. Being sensitive to the ethical consequences of an uncertain diagnosis in this setting means we may delay assigning a diagnostic ‘label’ until we are sure that it is appropriate, necessary or helpful |
Conclusion
A single view of health and illness has substantial limitations, especially with respect to mental disorders. ‘Mental disorders, after all, are conditions that disturb a person’s unique self – a self that is at once biological, storied, encultured, social-political and existential. This inevitability of our knowledge being only partial is a theme that shadows all attempt at classification’.3
In a way, a consultation is a mixed methods study with a cohort of one. Like any mixed methods study, there will always be challenges synthesising data from different sources and different perspectives. However having the flexibility to consider different points of view enables us to use our knowledge of botany and our skills as gardeners to reduce suffering. Ultimately, our job is not only to accurately classify disease; it is also to provide clinical benefit for our patients. To do so we need to expand our repertoire of diagnostic frameworks beyond mere botanical classification.
Conflict of interest: none declared.