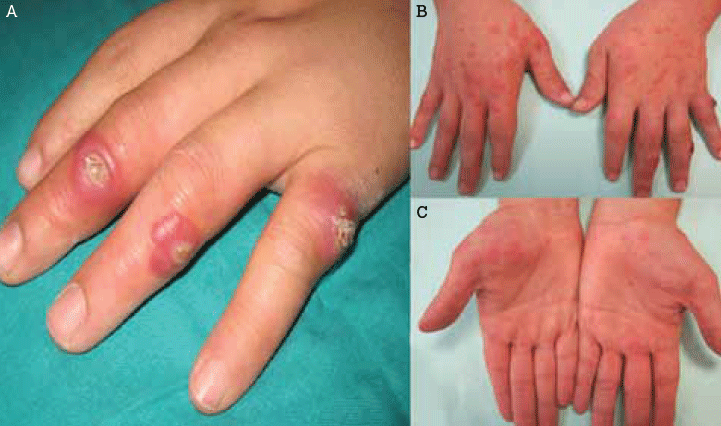
Figure 1. Finger nodules on presentation A) and 1 week later B) and C)
Question 1
What is the most likely diagnosis?
Question 2
What is the aetiology of this condition?
Question 3
What population is at risk for this condition?
Question 4
What would be the most frequent complications expected in this clinical picture?
Question 5
What would be the appropriate management of this condition?
Answer 1
The most likely diagnosis is orf nodule, also known as ecthyma contagiosum, and erythema multiforme secondary to this infection. Most important differential diagnoses include Milker nodule.
Answer 2
Orf nodules are caused by a parapox virus subgroup of the poxvirus family. It is generally transmitted by direct contact with an infected sheep (‘scabby mouth’). Milker nodules have a similar appearance and are caused by another parapox virus found in cattle. The clinical images of the nodules are the first key to diagnosis, then the epidemiological context (sheep or cattle exposure) can separate the two conditions. In this case, further specific questioning elicited the history of exposure to sheep.
Answer 3
Orf is an occupational disease among sheep farmers, veterinarians and abattoir workers.1–3 Patients usually do not present for medical care because they know the cause of the nodules and their self limiting nature. In contrast, there is a rural population without regular contact with livestock who may have contact with an infected sheep. They may not know of the infection and lesions and may be more likely to seek medical care, as in this case. It was only after diagnosis that the patient recalled and recognised the relevance of contact with sheep.
Answer 4
Severe systemic complications are uncommon. Fever, superinfection, erysipelas and lymphadenitis are the most frequent complications. Erythema multiforme, a hypersensitivity reaction in this case to the parapox virus, is a complication that may lead to seeking medical attention.1,4–6 Immunocompromised patients can develop very large and atypical orf lesions that do not always regress spontaneously and may recur.6,7
Answer 5
Orf is a self limiting disease that generally resolves after about 3–4 weeks. This is in contrast to Milker nodule, which usually resolves in 5–6 weeks.8 Although severe systemic complications of orf are uncommon, the lesions may be alarming. Once the diagnosis is made, the key is to explain the self limiting nature of the lesion and to reassure the patient. If initially an accurate diagnosis is not made, patient concern may increase as the lesions will not have improved after the prescribed treatment (frequently an antibiotic).2
In the case of an immunocompromised patient, lesions may have a chronic evolution. It is then necessary to consider an active treatment with cryotherapy,9 surgical excision,10 interferon,11 topical idoxuridine12 or imiquimod cream.13
Conflict of interest: none declared.