The respiratory tract is a primary interface of our bodies with the outside world. It comes into contact with 14 000 litres of air during a 40 hour working week and physical activity can increase ventilation 12-fold.1 The quality of the air we breathe therefore has major implications for the health of the respiratory tract. Although approximately 25% of our time is spent in the workplace, this environment is more likely to be the cause of exposure-related respiratory problems because, generally, air quality will be poorer at work than in the domestic environment.2
Air contaminants may be dusts, gases, vapours or fumes. Any part of the respiratory tract can be adversely affected by poor air quality, from the nose to the alveoli. The site affected within the respiratory tract depends on the integrity of defense mechanisms and the properties of the air contaminants (Figure 1). Other determinants include individual susceptibility and the intensity and duration of the exposure.
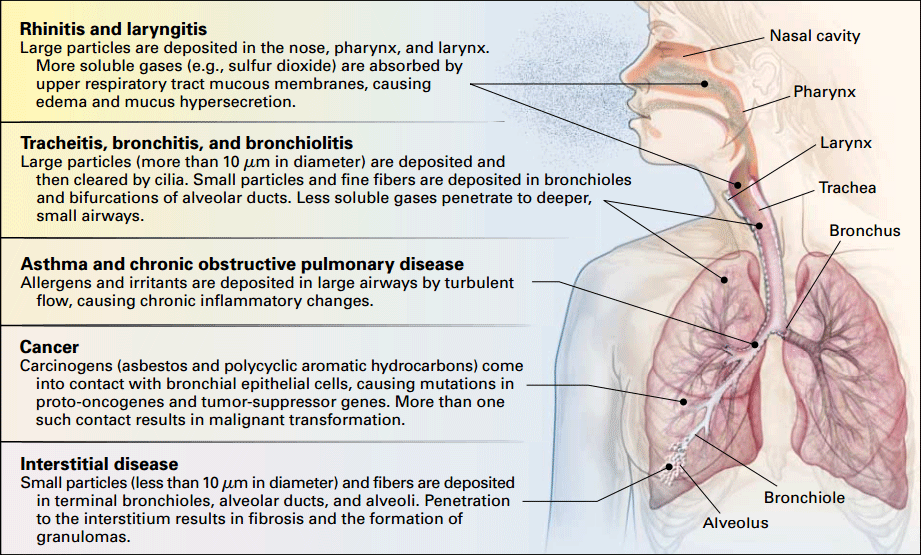
Figure 1. Categories of occupational respiratory disease, their anatomical locations within the respiratory system, examples of common causative substances and their pathophysiologic effects
Reproduced with permission. Beckett WS. Occupational respiratory diseases. N Engl J Med 2000;342:406–13
Inhalation of a strong irritant, such as that caused by an industrial accident, may injure the respiratory tract causing acute symptoms of shortness of breath, cough and chest tightness, potentially requiring emergency medical care. The extent of injury will depend on the type and dose of exposure and may lead to prolonged symptoms due to the development of irritant induced lung disease.2 Usually there will be a clear history of high level exposure at the time of onset of symptoms.
There is however, often a period of latency between the actual exposure and the development of disease. This period may vary from hours to decades. Conditions with long latencies include pneumoconiosis, chronic obstructive pulmonary disease (COPD) and pulmonary malignancies. The latency from the time of asbestos exposure to the development of mesothelioma is approximately 20–40 years.3 Allergic lung diseases, such as sensitiser induced occupational asthma and hypersensitivity pneumonitis, have widely variable periods of latency, from days to years between first exposure and the development of exposure-related symptoms.2 A classification of occupational and exposure-related lung disease is listed in Table 1.
Table 1. Classification of occupational and exposure associated lung disease13
| Disease category | Representative causative agent |
|---|
Upper respiratory tract
- Nonspecific irritation
- Rhinitis – allergic and nonallergic
- Upper airway dysfunction (vocal cord dysfunction, work associated irritable larynx syndrome)
|
- Irritant gases, fumes, dust
- House dust mite, pollens, animals
- Irritants, strong scents, emotional factors
|
Airway disorders
- Occupational asthma
- sensitiser induced asthma/reactive airways dysfunction syndrome
- irritant induced asthma
- Work exacerbated asthma
- Chronic bronchitis/COPD
- Bronchiolitis
|
- Diisocyanates, wood dust, flour, animals
- Irritant gases, smoke
- Irritants, fumes, exertion, cold air, emotion
- Irritants, mineral dust, coal, fumes
- Diacetyl (‘popcorn worker’s lung’)
|
Acute inhalational injuries
- Toxic pneumonitis
- Metal fume fever
- Smoke inhalation
|
- Inhalational accident
- Metal oxides
- Combustion products
|
| Hypersensitivity pneumonitis |
Bacteria, fungi, animal proteins |
| Infectious disorders |
Bacteria (eg. legionella), tuberculosis, viruses |
| Pneumoconioses |
Asbestos, silica, beryllium, coal |
Malignancies
- Sinonasal cancer
- Lung cancer
- Mesothelioma
|
- Wood dust
- Asbestos, radon
- Asbestos
|
Nonspecific building related illness
(‘Sick building syndrome’) |
Volatile organic compounds, fungal endotoxin, inadequate air circulation |
| Adapted from Fishman AP, editor. Fishman’s Pulmonary Diseases and Disorders. 4th edn. New York: McGraw Hill, 2008 |
Upper respiratory tract conditions
Exposures that typically affect the upper respiratory tract tend to be large particle dusts (>10 µm in diameter) and highly water soluble gases such as ammonia and chlorine.1 Exposure of the upper respiratory tract to airborne irritants will cause nonspecific symptoms such as cough, nasal irritation and congestion. These unpleasant symptoms will encourage individuals to remove themselves from the exposure thereby providing protection.
Rhinitis
Rhinitis may be allergic or nonallergic.4 Symptoms include sneezing, rhinorrhoea, nasal obstruction and itching of the nose, eyes and palate. If symptoms are due to an allergic mechanism (IgE mediated) there is generally a temporal association with exposure to the allergen. Sneezing occurs immediately, such as when emptying a vacuum cleaner bag or on entering a room with a cat, then nasal discharge followed by nasal obstruction over a few hours. Domestic exposures associated with perennial allergic rhinitis include house dust mite and pets. Occupational allergic rhinitis is defined as rhinitis directly attributable to a specific substance encountered in the work environment caused by IgE mediated sensitisation.5 Occupational exposures associated with allergic rhinitis include animal allergens (research laboratory workers, veterinarians), grain and flour dust (bakers, flour mill workers) and plant allergens (gardeners, farmers).
There is a clear association between occupational allergic rhinitis and asthma, therefore all workers with work related rhinitis should be assessed for the presence of asthma.6 The diagnosis of occupational allergic rhinitis should be considered a sentinel workplace health event and alert the employer that further control is required.5
Irritant rhinitis may be difficult to clinically differentiate from allergic rhinitis. In the office environment irritants may be in the form of volatile organic compounds from new paint, office furniture and cleaning products or emitted from malfunctioning appliances such as photocopiers. In the industrial setting, irritant exposures are likely to be more obvious such as welding fumes or wood dust.
Vocal cord dysfunction
Dysfunctional behaviour of the larynx is an important and underappreciated cause of recurrent respiratory symptoms and may be triggered by exposure to respiratory irritants and strong odours, such as perfumes. Unfortunately, there is a lack of consensus regarding the terminology and diagnostic features of this condition. Vocal cord dysfunction (VCD) is probably the most well known form of nonorganic laryngeal dysfunction, especially to respiratory physicians. Often VCD may masquerade with symptoms suggestive of asthma; it may also co-exist with asthma. Symptoms are due to inappropriate vocal cord motion causing partial airway obstruction, especially during inspiration.7 Typical symptoms of VCD are recurrent episodes of dyspnoea, sensation of inspiratory limitation, throat tightness and cough. Frequently, episodes have a rapid onset and resolution.8 Work-associated irritable larynx syndrome describes recurrent laryngeal symptoms associated with a specific workplace trigger.8
Occupational asthma
Occupational asthma is the development of new onset asthma (or the recurrence of asthma) due to an exposure specific to a workplace.9 Occupational asthma is the most common occupational lung disease in developed countries. It is estimated that 15% of all adult onset asthma is due to workplace factors; contributing substantially to the burden of asthma in the general community.10
For further information, refer to a review previously published in the January/February 2010 issue of Australian Family Physician.11
Hypersensitivity pneumonitis
Hypersensitivity pneumonitis (HP, or extrinsic allergic alveolitis) is a complex syndrome caused by an immunological reaction to an inhaled agent.2 Acute HP may present with fevers, chills, malaise, cough and shortness of breath; mimicking an infective process. Symptoms of acute HP generally subside within hours or a few days of removal from the exposure. Chronic HP may present with features of pulmonary fibrosis such as dyspnoea. Identification of this condition requires a high level of suspicion and a careful exposure history. Some industries and exposure associated with HP include:4
- farming (‘farmer’s lung’, ‘mushroom worker’s lung’)
- bird or poultry handling (‘bird breeder/fancier’s lung’)
- water-related contamination (‘humidifier lung’)
- grain processing (wheat weevil disease)
- plastics industry workers
- textile workers.
Exacerbation of lung disease due to exposures
Workplace and environmental exposures may exacerbate pre-existing respiratory disease. Asthma is a common condition that is influenced by environmental exposures. It has been estimated that work exposures worsen asthma control in 21% of adults with asthma.12 Factors include irritants, exercise, cold or dry environments and emotional stress. The identification and management of these factors will assist in achieving asthma control. All patients with asthma should be questioned regarding symptom triggers and their domestic and work environments.
The presence of chronic respiratory diseases such as COPD, pulmonary fibrosis and bronchiectasis is likely to result in impairment of the respiratory tract defence mechanisms and therefore increased susceptibility to the effects of adverse exposures. The benefits of work to general health are becoming better appreciated and measures should be in place to allow people with chronic respiratory conditions to maintain an active work life without exposures exacerbating their lung disease. This will often involve good communication with an employer regarding a worker’s needs.
Assessment and management of exposure related respiratory conditions
To identify whether a respiratory problem may be due to an exposure, clinicians need to have a high index of suspicion and take an occupational and environmental history (Table 2, 3). If a patient presents with new onset respiratory symptoms it is useful to ask about recent changes in their environment, such as whether they have a new pet at home or if they have commenced a new job. It is also useful to ask whether symptoms improve when away from an exposure. Symptoms of recent onset occupational asthma may improve over a weekend but are more likely to improve over a week or when on holidays. Longstanding or severe occupational asthma may not improve until many months after removal of the cause, if at all.
Table 2. When when to consider workplace exposure as a cause of shortness of breath
| New onset respiratory symptoms, eg. persistent cough, shortness of breath or wheeze |
| New diagnosis of a respiratory condition with known occupational or environmental causes, eg. hypersensitivity pneumonitis or mesothelioma |
Assessment of an individual with increased susceptibility to the effects of exposure, eg:
- atopy, increases the risk of some allergic lung diseases such as sensitiser induced occupational asthma
- pre-existing respiratory conditions such as asthma or COPD that may impair defences to exposures
|
| Worsening of a previously stable respiratory condition, eg. exacerbations of asthma or COPD |
| Presentation with temporal association of symptoms with exposure, eg. improvement of symptoms when away from the workplace |
| Working in a high risk environment, eg. bakery, animal facility, farm, chemical industry, mining |
| Presentation with any form of chronic lung disease, as nearly all respiratory conditions may be caused by exposures |
| Outbreak of similar symptoms or disease in a group with shared exposure, eg. Legionnaire disease, ‘popcorn worker’s lung’ (bronchiolitis obliterans secondary to microwave popcorn butter flavouring, diacetyl) |
Investigation of patients with respiratory problems should include spirometry and a chest X-ray, which is available to most general practitioners. These preliminary tests will not rule out many conditions and more specialised investigations such as bronchial provocation testing or a chest computed tomography (CT) scan may be necessary. Referral to a respiratory physician will assist in the performance of appropriate further investigations and establishing a diagnosis. If the condition is work related, then involvement of a respiratory or occupational physician is needed to consider factors such as the effect of the causative exposure on other workers, how to control the exposure at the workplace and appropriate use of personal protective equipment. The role of pre-employment screening is controversial and therefore an experienced clinician should supervise these assessments.
Table 3. Taking an occupational and environmental history13
General health history
- Does the patient think symptoms/problem is related to any specific exposure?
- When was the onset of symptoms and how are symptoms related to exposures?
- Has the patient missed time from work due to symptoms and why?
- Prior respiratory problems
- Medications
- Smoking history
|
Current or most relevant employment
- Job/process
- Type of industry and specific work
- Name of employer
- Years employed
|
Exposure information
- General description of job processes and hygiene of workplace
- Materials used
- Ventilation/exhaust systems
- Use of respiratory protection
- Are other workers affected?
|
Environmental nonoccupational factors
- Smoking history
- Pets
- Hobbies
|
Specific workplace exposures
- Fumes/dusts
- Gases
- Metals
- Solvents
- Infectious agents
- Organic dusts: cotton, wood
- Physical factors: exertion, cold, heat
- Emotional factors: stress
|
Past employment
- List jobs in chronological order
- Job title
- Exposures
- Military service
|
| Adapted from Fishman AP, editor. Fishman’s Pulmonary Diseases and Disorders. 4th edn. New York: McGraw Hill, 2008 |
Summary
Nearly all respiratory diseases can be caused or exacerbated by environmental exposures. The identification and control of relevant exposures has the potential to improve clinical outcomes and protect others from the development of respiratory disease. Clinicians should regularly take an occupational and environmental history to identify possible exposures associated with breathing problems.
Conflict of interest: none declared.
Acknowledgement
Thanks to Professor Michael Abramson for reviewing this article.