The Australian Government recently announced an expansion of Medicare-funded MRI services. From November 2012, general practitioners can refer children under the age of 16 years and from November 2013, patients of any age, for MRI services of a ‘select group of clinically appropriate indications’.2 Indications for GP-referred scans for children under the age of 16 years include MRI of the knee to investigate possible internal joint derangement (Table 1).3 General practitioners can already refer patients for the evaluation of possible complications of PIP breast implants and can also refer private patients for MRI scans by most services, but this usually incurs an out-of-pocket expense which may be beyond the means of many patients.
Table 1. Medicare funded indications for GP-referred MRI in children under the age of 16 years3*
- Head: unexplained seizure or headache, paranasal sinus pathology not responding to conservative therapy
- Spine: unexplained neck or back pain, including when associated with significant trauma
- Knee: internal joint derangement
- Hip: investigation of septic arthritis, slipped upper femoral epiphysis, Perthes disease
- Elbow: suspicion of significant fracture or avulsion injury, which would result in change of management
- Wrist: suspected scaphoid fracture
|
|
* From November 2012
|
How does the test work?
MRI uses a superconducting magnet and radiowaves to obtain an image with very high contrast resolution. Different soft tissues, such as muscle and tendons, can be differentiated and the intraosseous compartment can be evaluated. There are no known long term adverse effects from having an MRI scan. Intravenous contrast is generally not used but may be indicated for example, in the assessment of synovitis, bone tumours or infection.
What is the radiation dose?
MRI does not use ionising radiation, which makes it a very attractive imaging technique for investigating pain in children.
What is tested?
Simplest sequences measure alterations in water content in soft tissue structures, which allows visualisation of oedema in bone marrow and tears in menisci and ligaments. More advanced sequences allow the detection of blood products and measurement of specific chemical species.
What is the difference between 1.5T and 3T?
Tesla (T) is the measure of magnetic field strength. Signal-to-noise (SNR) is a prime determinant of image resolution and is directly proportional to field strength. In simple terms, doubling the field strength will double signal-to-noise and result in increased image quality, however there will also be increased artefact. In practical terms, there are many other factors that may impact more on image quality than field strength. Currently, 1.5T is highly accurate in the diagnosis of meniscal and cruciate ligament injuries and in postoperative joint examinations. 3T has marginally higher accuracy for the detection of cartilage lesions and improves diagnostic confidence.
What are the indications?
MRI is indicated in the investigation of acute knee pain when plain X-ray has excluded fracture, osteoarthritis and osteochondral defects and where there is clinical suspicion of internal derangement. Other uses include assessing the stability of known osteochondral injuries, suspected insufficiency or stress fracture, osteonecrosis and the assessment of competitive athletes when expeditious management is required.
How does MRI fit in with other tests? When are other tests better?
Plain X-ray and computed tomography (CT) are more accurate in diagnosing acute fracture. Ultrasound is equally accurate in the assessment of collateral ligaments, quadriceps, patellar tendons and popliteal fossa, and will generally be more accessible than MRI. Ultrasound cannot assess deeper structures, including the anterior cruciate ligament, menisci, cartilage and bone marrow.
When shouldn’t MRI be used?
MRI is not indicated routinely in the assessment of the acutely painful knee or where careful examination does not reveal signs of cruciate or collateral ligament or meniscal injury. MRI does not usually provide additional information where degenerative joint disease is evident on plain X-rays.
What information should be included on the request form?
The request form should include pertinent clinical history, examination and laboratory findings. Most MRI services have a dedicated request form that includes a screening tool for common contraindications. This needs to be completed by the referring doctor. The referral must also include the referrer’s name, date of request and provider number. It is very useful to provide a contact number for urgent or unexpected results to facilitate prompt communication between the GP and radiologist.
Are there any contraindications?
There are some absolute and some relative contraindications to MRI (Table 2). In most cases, a cardiac pacemaker or defibrillator is an absolute contraindication, although devices are now emerging which are ‘MRI safe’. Intraocular metal is another absolute contraindication, as the metal will heat and may move, resulting in structural damage. Orbital X-rays and/or CT may need to be performed before the MRI scan where intraocular or intracerebral metal is suspected. Other absolute contraindications include deep brain stimulators.
Common relative contraindications include cerebral aneurysm clips, metallic stents, cochlear implants, neurostimulators and pregnancy.
Table 2. Contraindications for MRI (absolute and relative)
- Cardiac pacemaker*
- Deep brain stimulators
- Intraocular metal
- Cerebral aneurysm clips
- Recent stents
- Cochlear implants
- Neurostimulators and implantable pumps
- Early pregnancy
|
|
* Some devices may be MRI compatible with cardiac technologist/cardiologist assistance
|
The department performing the MRI scan is responsible for the safety of patients undergoing MRI examinations and will use both a screening questionnaire and verbal interview to screen patients. It is helpful for referring clinicians to indicate any potential contraindications, as the assessment of implant safety can take some time if older operative records need to be obtained.
Is MRI safe in pregnancy?
There are no known adverse effects of MRI on the human fetus, however, MRI does increase tissue temperature, particularly with increasing field strength. Risk is believed to be greater in the first trimester when organ development is progressing at a fastest rate. Balance of risk to the fetus and benefit to the mother will generally be in favour of avoiding MRI for investigation of knee pain during pregnancy.
What about MRI in claustrophobic patients and children?
Most children over the age of 6 years will tolerate MRI well. Under the age of 6 years, children respond differently to the noise and physical constraints of the magnet and most will require some sedation under the supervision of an anaesthetist. This will often necessitate admission to a hospital.
Infants up to the age of 9 months generally do not require sedation but need to be immobilised in a special ‘bean bag’ or similar device.
Claustrophobic adults may be helped by premedication with oral anxiolytics in consultation with the MRI service, but many will require deeper sedation and this is most safely performed with the assistance of an anaesthetist. Not all MRI providers will support this level of service and GPs may need to locate a suitable service provider. More recently, manufacturers of MRI equipment have built magnets with larger apertures or ‘bores’, generally 90 cm in diameter, which can accommodate claustrophobic patients and overweight/obese patients.
What do the results mean?
MRI can reveal cartilage lesions, osteophytes and meniscal lesions in asymptomatic patients with no signs of joint disease.4 MRI findings need to be correlated with the patient’s history and clinical findings.
What should I tell my patients?
Typically the imaging time will be between 15 and 30 minutes, but patients should allow approximately 1 hour to complete the pre-examination preparation, including the safety questionnaire and interview. Patients need to remove ferrous material (eg. belts) and clothing below the waist (excluding underwear) and will be given a gown to wear. The scanner is noisy (generally reaching levels of just under 100 dB), so patients are given protective headphones through which their favourite music or radio station can be transmitted during the scan. Patients can converse with the scanning technologist at all times.
There may be an out-of-pocket cost, which may need to be paid on the day of the scan.
Case study
A man, 39 years of age, presents with right knee pain after playing soccer in the backyard with his children. The next morning he woke up with worsening pain and swelling of the right knee. He presented for medical review, as he could not attend his work as an electrician. The pain was worse when twisting and he had intermittent locking. Other relevant history included that as a teenager and young adult he had played football and ‘hurt his knee’ a few times without any significant injury.
On examination, there was right knee swelling consistent with a joint effusion and medial joint line tenderness. He was unable to fully extend the knee. An X-ray showed no acute fracture. Management started with RICE. The pain and functional impairment continued at review so an MRI was ordered (Figure 1).
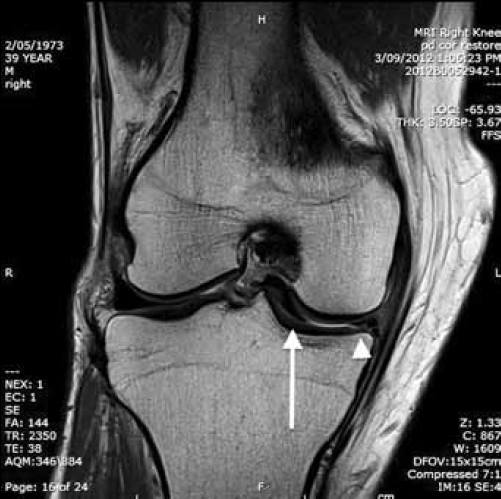
Figure 1. MRI of the patient's right knee
The T2 coronal image shown demonstrates a bucket-handle tear of the the medial meniscus with a small residual meniscal fragment in normal position (arrowhead) and a large loose fragment adjacent to the intercondylar notch (long arrow). The patient was referred for an orthopaedic surgical opinion given the ongoing symptoms, functional impairment and correlation with MRI findings.
Conflict of interest: none declared