Question 1
What is the diagnosis?
Question 2
What is the differential diagnosis of pelvic pain in early pregnancy?
Question 3
What are the risk factors for this diagnosis?
Question 4
What diagnostic tools are helpful in assessing this presentation?
Question 5
What is the management of this condition?
Answer 1
The diagnosis is heterotopic pregnancy (both intrauterine and extrauterine pregnancies). This patient has a triplet heterotopic pregnancy.
Answer 2
Pelvic pain is a common presentation in early pregnancy. The differential diagnosis includes pregnancy related and nonpregnancy related pathology. Miscarriage, ectopic pregnancy, ovarian torsion, ruptured ovarian cyst/corpus luteum, pelvic inflammatory disease, red degeneration of fibroid, heterotopic pregnancy, gastrointestinal tract pathology and urinary tract pathology should all be considered.
Answer 3
Heterotopic pregnancy is rare in spontaneous conceptions, with an incidence of 1:30 000.1 However, the incidence is up to 1:100 in pregnancies conceived by assisted reproductive technologies (ART).2Other risk factors include previous ectopic pregnancy, smoking, endometriosis, pelvic inflammatory disease and previous tubal surgery.3
Answer 4
Heterotopic pregnancy is often a diagnostic dilemma, and is usually only diagnosed after tubal rupture.3,4 Clinical signs and symptoms are often unhelpful in making a diagnosis, and the presence of an intrauterine gestation can be falsely reassuring. Diagnosis is made using transvaginal ultrasound, or retrospectively at laparoscopy or laparotomy.
Answer 5
Treatment of a heterotopic pregnancy is primarily surgical, although expectant and medical management has been described.3,4 Medical management involves ultrasound guided transvaginal injection of hyperosmolar glucose or potassium chloride into the extrauterine gestational sac.5 Surgical treatment is either laparotomy (advised in cases of shock) or laparoscopy.
Discussion
Heterotopic pregnancy presents a diagnostic and management problem.
Transvaginal ultrasound was invaluable in revealing the diagnosis in this case, however, ultrasound may reveal only an intrauterine pregnancy without any abnormal features.6 Other ultrasound findings in heterotopic pregnancy include an intrauterine pregnancy in conjunction with an adnexal mass, free fluid in the pelvis and, rarely, a fetal heartbeat outside the uterus.6
In Samantha's case, a laparoscopy and left salpingectomy (Figure 1) with minimal handling of the uterus was performed. She subsequently had an elective caesarian section at 38 weeks gestation, with both twins born alive and well.
Although rare, heterotopic pregnancy should be considered in all cases of abdominal pain in pregnancy, particularly in women who have conceived using ART. Every woman who conceives using ART should have both adnexae carefully examined using transvaginal ultrasound in the first trimester.2
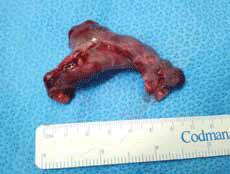
Figure 1. Left fallopian tube and ectopic products of conception
Conflict of interest: none declared