Every 5 years the International Liaison Committee on Resuscitation (ILCOR) assesses the latest evidence evaluated by an international body of experts interested in resuscitation and issues updated guidelines.2 The Australian Resuscitation Council (ARC), in conjunction with the New Zealand Resuscitation Council, contributes to this process on behalf of the Pacific region. In December 2010, the latest guidelines were released in Australia for implementation in 20113 (Figure 1, 2). The key messages from the new guidelines are about recognising the importance of compressions, simplifying drug regimens and emphasising the importance of postresuscitation care.
Importance of compressions
Continuous compressions allow a build-up of pressure in the aorta, which in turn maintains flow to both the myocardium and the brain. Whenever there is a break in compressions to allow ventilation or to perform some other manoeuvre, the pressure within the aorta drops. Guidelines have attempted to reflect this by reducing or eliminating as much as possible any gaps in compression. Over the years, compression to ventilation ratios have changed from five compressions to one ventilation, to 30 compressions to two ventilations. In the new ARC basic life support guidelines, the value of providing ventilation at all is considered discretionary.4
The guidelines support starting compressions on any person who is not responsive and not breathing normally.4 The description 'not breathing normally' means that, even if the person still has agonal respiratory effort, compressions should be started quickly. The rescuer then should consider two ventilations for every 30 compressions, if they are willing and able. This change in policy from ventilation first recognises that compression only cardiopulmonary resuscitation (CPR) is significantly better than no CPR.4 Some authors recommend advising bystanders and first responders to use compression only CPR in the first instance on the basis that this will increase the percentage of patients receiving CPR.5 In one South Australian study, under half of the patients in cardiac arrest received CPR, which represents a significant missed opportunity.6

Figure 1. Australian Resuscitation Council basic life support algorithm
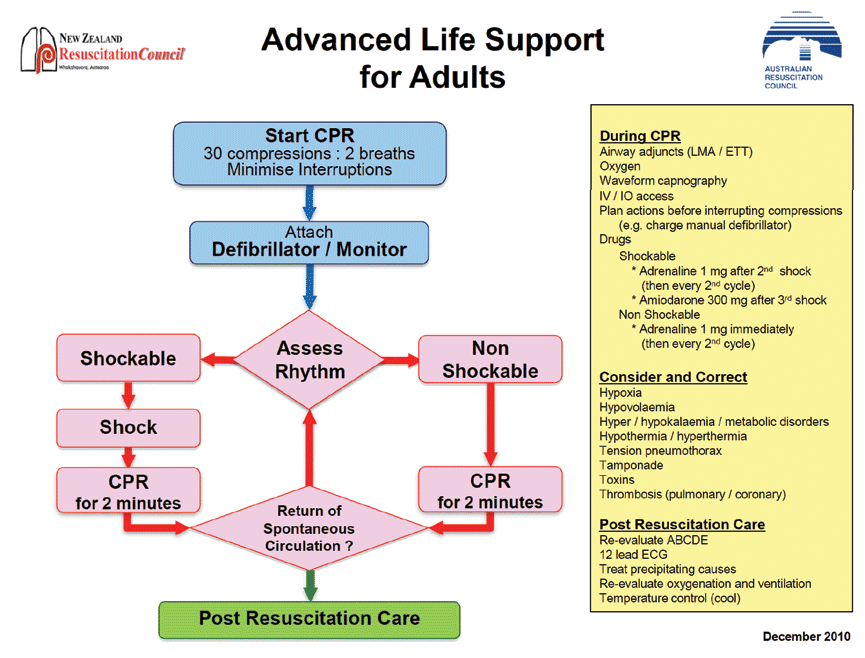
Figure 2. Australian Resuscitation Council advanced life support for adults algorithm
Importantly, in the basic life support guidelines all reference to checking a pulse has been dropped on the basis that patients who are not responsive and not breathing normally are highly likely to be in arrest and will not be harmed by compressions if these are commenced unnecessarily.4
The new advanced life support guidelines also support continuous CPR, with a change to the recommendations surrounding charging and discharging a manual defibrillator. The new recommended procedure when using a manual defibrillator with pads for contact is to charge the defibrillator while compressions continue and only stop compressions when it is fully charged and ready to defibrillate.7 Once the defibrillation has occurred, compressions should be commenced straight away with no pause to assess the outcome of the shock.
This is a significant departure from past practice and has been recommended in light of evidence about the safety of compression when using the newer biphasic external defibrillators with conformal, adhesive, pregelled electrodes. However, care should still be taken to prevent defibrillation while performing compressions until further research evidence is available, particularly when using older model defibrillators.8 Using the technique outlined in the new guidelines,7 it is possible to assess a rhythm and deliver a shock with a break in compressions of only about 8 seconds. Unfortunately, this technique cannot be used with semiautomatic defibrillators, which are more commonly available in a general practice and public areas, because they require a static period in which to identify a shockable rhythm (ventricular fibrillation or ventricular tachycardia) and then charge.
Simplifying drug regimens in cardiac Arrest
The trend in drug therapy for cardiac arrest is toward simplification of the process and treating the patient on a standard protocol. We are now effectively down to two drugs – adrenaline and amiodarone – in addition to electricity and oxygen.
The new ARC advanced life support guidelines recommend that 1 mg of adrenaline be given intravenously every second cycle of CPR.7 As CPR is delivered for 2 minutes every cycle, this means that adrenaline is given every four-and-a-bit minutes (compared to every 3 minutes in the previous guidelines). In patients with a shockable rythmn (ventricular fibrillation and pulseless ventricular tachycardia), the first action would be to defibrillate as soon as possible followed by 2 minutes of CPR and the second defibrillation, after which adrenaline should be started and repeated every second cycle. In a pulseless electrical activity arrest or asystolic arrest the adrenaline should be started as soon as possible and again repeated every second cycle. The dose of adrenaline should be given with a significant fluid push (100 mL) behind it.
Amiodarone is the only other drug used in a routine cardiac arrest and 300 mg is given to patients in a shockable rhythm (ventricular fibrillation and pulseless ventricular tachycardia) after the third defibrillation. In normal practice, there is no need for any repeat doses as this dose is thought to provide an adequate anti-arrhythmic effect.9 Atropine, which used to be recommended for asystole, is no longer part of the cardiac arrest algorithm – although it is still used to treat bradycardia in a nonarrested patient.
Postresuscitation care
The third key message from the new ARC advanced life support guidelines is the importance of appropriate postresuscitation care.9 Postresuscitation, consider the following three areas early:
- Attention to detail. This involves addressing contributing factors to the arrest, eg. by normalising electrolytes and blood glucose
- Removal of the underlying cause of the cardiac arrest with either angioplasty or, in remote areas, by thrombolysis. Systems now exist for rapid access to angioplasty in most large centres with thrombolysis being supported in those areas where a patient cannot be transported to an angioplasty suite within 60–90 minutes
- Cooling of the postresuscitation patient, aiming for a period of mild hypothermia for 24 hours following return of circulation for most patients. Hypothermia can be achieved with a large volume of cold saline or more specialised cooling devices. Preliminary studies in both Australia and Europe have shown a survival benefit from cooling and this has now become the standard of care.10 Trials of commencing this cooling in the prehospital phase are under way in Victoria, with Western Australia and South Australia due to join the trial in early 2012.11
Outcomes and prevention
Return of circulation rates in the order of 25% for all witnessed out-of-hospital cardiac arrests, and 45% if the patient was in ventricular fibrillation (VF) or ventricular tachycardia (VT), are becoming the expected standard.10 An overall hospital discharge rate for out-of-hospital cardiac arrest of 7.6% has been reported.10 Of course the best results from cardiac arrests are when the arrest has been averted by early detection and early intervention.12 The National Safety and Quality Council has identified the recognition and response to the deteriorating patient as one of its key initiatives in improving quality and safety. As standardised systems of early recognition and response become widespread throughout the health system it should be hoped that fewer patients go on to suffer a cardiac arrest.
Summary
The latest ARC guidelines on basic and advanced life support emphasise the importance of early recognition of deterioration for patients already within the system, early defibrillation and early chest compressions with a simplification of drug treatment and appropriate postresuscitation care.
None of the new developments are particularly surprising, as they represent the continuation of trends that have been developing over recent years.
Conflict of interest: none declared